Abstract
Background
The global rise in obesity prevalence among children and adolescents has been linked to modifiable lifestyle factors, including lack of physical activity. However, no known meta-analysis has been conducted on the effects of exercise intervention on body composition and cardiometabolic risk factors in overweight and obese adolescents.
Objectives
The aim of this study was to (1) estimate whether exercise intervention meaningfully improves body composition and cardiometabolic risk factors in overweight and obese adolescents; and (2) discuss the implications of the findings in terms of primary healthcare provision and public health policy, using New Zealand as an exemplar context.
Data Sources
Electronic databases (PubMed, Web of Science, SPORTDiscus, Google Scholar) from inception to May 2015. The reference lists of eligible articles and relevant reviews were also checked.
Study Selection
Inclusion criteria were (1) randomized controlled trial; (2) structured exercise intervention, alone or combined with any other kind of intervention; (3) control group received no structured exercise or behavioural modification designed to increase physical activity; (4) participants overweight or obese (body mass index [BMI] ≥85th percentile); and (5) participants aged between 10 and 19 years.
Appraisal and Synthesis Methods
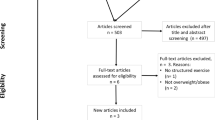
Initially, 1667 articles were identified. After evaluation of study characteristics, quality and validity, data from 13 articles (15 trials) involving 556 participants (176 male, 193 female, 187 unknown) were extracted for meta-analysis. Meta-analyses were completed on five body composition parameters and ten cardiometabolic parameters. Effect sizes (ESs) were calculated as mean differences, as well as standardized mean differences in order to determine effect magnitude.
Results
Exercise intervention reduced BMI (mean 2.0 kg/m2, 95 % CI 1.5–2.5; ES moderate), body weight (mean 3.7 kg, 95 % CI 1.7–5.8; ES small), body fat percentage (3.1 %, 95 % CI 2.2–4.1; ES small), waist circumference (3.0 cm, 95 % CI 1.3–4.8; ES small), but the increase (improvement) in lean mass was trivial (mean 1.6 kg, 95 % CI 0.5–2.6). The response to an oral glucose tolerance test following exercise intervention was for a decrease in the area under the curve for insulin (mean 162 μU/μl, 95 % CI 93–231; ES large) and blood glucose (mean 39 mg/dl, 95 % CI 9.4–69; ES moderate). Improvements in the homeostatic model assessment were also noted (mean 1.0, 95 % CI 0.7–1.4; ES moderate) and systolic blood pressure (mean 7.1 mmHg, 95 % CI 3.5–10.7; ES moderate). The effects of exercise on total cholesterol, low-density lipoprotein cholesterol, high-density lipoprotein cholesterol, fasting insulin and fasting blood glucose were inconclusive.
Limitations
Most of the included trials were short term (6–36 weeks) and 13 had methodological limitations. Additionally, the meta-analyses for some of the secondary outcomes had a small number of participants or substantial statistical heterogeneity.
Conclusions
The current evidence suggests that exercise intervention in overweight and obese adolescents improves body composition, particularly by lowering body fat. The limited available evidence further indicates that exercise intervention may improve some cardiometabolic risk factors.





Similar content being viewed by others
References
Malhotra A, Noakes T, Phinney S. It is time to bust the myth of physical inactivity and obesity: you cannot outrun a bad diet. Br J Sports Med. 2015;49(15):967–8.
Triggle CR. Exercise ‘not key to obesity fight’. 2015. http://www.bbc.com/news/health/32417699. Accessed 14 May 2015.
Royal Society for Public Health. Mixed messages surrounding diet and exercise risk confusing the public. 2015. https://www.rsph.org.uk/en/about-us/latest-news/index.cfm/pid/ADAA562D-5FBA-4082-A4E5F076A16EA3AB. Accessed 14 May 2015.
OECD. OECD Obesity Update 2014. http://www.oecd.org/health/obesity-update.htm. Accessed 15 Apr 2016.
Olshansky SJ, Passaro DJ, Hershow RC, et al. A potential decline in life expectancy in the United States in the 21st century. N Engl J Med. 2005;352(11):1138–45.
Meeuwsen S, Horgan GW, Elia M. The relationship between BMI and percent body fat, measured by bioelectrical impedance, in a large adult sample is curvilinear and influenced by age and sex. Clin Nutr. 2010;29(5):560–6.
World Health Organization. Plan of action of the Commission on Ending Childhood Obesity. 2014. http://www.who.int/dietphysicalactivity/end-childhood-obesity/action-plan/en/. Accessed 26 May 2014.
Hammond RA, Levine R. The economic impact of obesity in the United States. Diabetes Metab Syndr Obes. 2010;3:285–95.
Brettschneider C, Leicht H, Bickel H, et al. Relative impact of multimorbid chronic conditions on health-related quality of life: results from the Multicare Cohort Study. PLoS One. 2013;8(6):e66742.
Lal A, Moodie M, Ashton T, et al. Health care and lost productivity costs of overweight and obesity in New Zealand. Aust N Z J Public Health. 2012;36(6):550–6.
Faigenbaum AD, Myer GD. Exercise deficit disorder in youth: play now or pay later. Curr Sports Med Rep. 2012;11(4):196–200.
Lieberman D. The story of the human body: evolution, health, and disease. 1st ed. London: Pantheon; 2013.
Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA Statement. Open Med. 2009;3(3):e123–30.
Centers for Disease Control and Prevention. Basics about childhood obesity. 2015. http://www.cdc.gov/obesity/childhood/basics.html. Accessed 12 May 2015.
Higgins J, Green S, Cochrane Collaboration, editors. Cochrane handbook for systematic reviews of interventions. Chichester: Wiley; 2008.
Crowther M, Lim W, Crowther MA. Systematic review and meta-analysis methodology. Blood. 2010;116(17):3140–6.
Cohen J. A power primer. Psychol Bull. 1992;112(1):155–9.
Borenstein M, Hedges LV, Higgins JPT. A basic introduction to fixed-effect and random-effects models for meta-analysis. Res Syn Meth. 2010;1(2):97–111.
Hopkins WG. A spreadsheet for deriving a confidence interval, mechanistic inference and clinical inference from a p value. Sport Sci. 2007;11:16–20.
Hopkins WG, Marshall SW, Batterham AM, et al. Progressive statistics for studies in sports medicine and exercise science. Med Sci Sports Exerc. 2009;41(1):3–13.
Higgins JP, Thompson SG, Deeks JJ, et al. Measuring inconsistency in meta-analyses. BMJ. 2003;327(7414):557–60.
Ryan R. Cochrane Consumers and Communication Review Group: meta-analysis. http://cccrg.cochrane.org. Accessed 17 May 2015.
Davis JN, Kelly LA, Lane CJ, et al. Randomized control trial to improve adiposity and insulin resistance in overweight Latino adolescents. Obesity (Silver Spring). 2009;17(8):1542–8.
Davis JN, Tung A, Chak SS, et al. Aerobic and strength training reduces adiposity in overweight Latina adolescents. Med Sci Sports Exerc. 2009;41(7):1494–503.
Balagopal P, George D, Patton N, et al. Lifestyle-only intervention attenuates the inflammatory state associated with obesity: a randomized controlled study in adolescents. J Pediatr. 2005;146(3):342–8.
Ben Ounis O, Elloumi M, Zouhal H, et al. Effect of individualized exercise training combined with diet restriction on inflammatory markers and IGF-1/IGFBP-3 in obese children. Ann Nutr Met. 2010;56(4):260–6.
Kim ES, Im JA, Kim KC, et al. Improved insulin sensitivity and adiponectin level after exercise training in obese Korean youth. Obesity (Silver Spring). 2007;15(12):3023–30.
Lee KJ, Shin YA, Lee KY, et al. Aerobic exercise training-induced decrease in plasma visfatin and insulin resistance in obese female adolescents. Int J Sport Nutr Exerc Metab. 2010;20(4):275–81.
Melnyk BM, Small L, Morrison-Beedy D, et al. The COPE Healthy Lifestyles TEEN program: feasibility, preliminary efficacy, & lessons learned from an after school group intervention with overweight adolescents. J Pediatr Health Care. 2007;21(5):315–22.
Meyer AA, Kundt G, Lenschow U, et al. Improvement of early vascular changes and cardiovascular risk factors in obese children after a six-month exercise program. J Am Coll Cardiol. 2006;48(9):1865–70.
Rocchini AP, Katch V, Schork A, et al. Insulin and blood pressure during weight loss in obese adolescents. Hypertension. 1987;10(3):267–73.
Sun MX, Huang XQ, Yan Y, et al. One-hour after-school exercise ameliorates central adiposity and lipids in overweight Chinese adolescents: a randomized controlled trial. Chin Med J (Engl). 2011;124(3):323–9.
Toulabi T, Khosh Niyat Nikoo M, Amini F, et al. The influence of a behavior modification interventional program on body mass index in obese adolescents. J Formos Med Assoc. 2012;111(3):153–9.
Tsang TW, Kohn M, Chow CM, et al. A randomised placebo-exercise controlled trial of Kung Fu training for improvements in body composition in overweight/obese adolescents: the “Martial Fitness” study. J Sports Sci Med. 2009;8(1):97–106.
Wong PC, Chia MY, Tsou IY, et al. Effects of a 12-week exercise training programme on aerobic fitness, body composition, blood lipids and C-reactive protein in adolescents with obesity. Ann Acad Med Singapore. 2008;37(4):286–93.
Kong AS, Sussman AL, Yahne C, et al. School-based health center intervention improves body mass index in overweight and obese adolescents. J Obes. 2013;2013:575016.
de Mello MT, de Piano A, Carnier J, et al. Long-term effects of aerobic plus resistance training on the metabolic syndrome and adiponectinemia in obese adolescents. J Clin Hypertens (Greenwich). 2011;13(5):343–50.
Nowicka P, Hoglund P, Pietrobelli A, et al. Family weight school treatment: 1-year results in obese adolescents. Int J Pediatr Obes. 2008;3(3):141–7.
DeBar LL, Stevens VJ, Perrin N, et al. A primary care-based, multicomponent lifestyle intervention for overweight adolescent females. Pediatrics. 2012;129(3):e611–20.
Johnston CA, Tyler C, Fullerton G, et al. Effects of a school-based weight maintenance program for Mexican-American children: results at 2 years. Obesity (Silver Spring). 2010;18(3):542–7.
Johnston CA, Tyler C, McFarlin BK, et al. Weight loss in overweight Mexican American children: a randomized, controlled trial. Pediatrics. 2007;120(6):e1450–7.
Neumark-Sztainer D, Story M, Hannan PJ, et al. New Moves: a school-based obesity prevention program for adolescent girls. Prev Med. 2003;37(1):41–51.
Savoye M, Shaw M, Dziura J, et al. Effects of a weight management program on body composition and metabolic parameters in overweight children: a randomized controlled trial. JAMA. 2007;297(24):2697–704.
Ben Ounis O, Elloumi M, Ben Chiekh I, et al. Effects of two-month physical-endurance and diet-restriction programmes on lipid profiles and insulin resistance in obese adolescent boys. Diabetes Metab. 2008;34(6 Pt 1):595–600.
Davis JN, Gyllenhammer LE, Vanni AA, et al. Startup circuit training program reduces metabolic risk in Latino adolescents. Med Sci Sports Exerc. 2011;43(11):2195–203.
Buchan DS, Ollis S, Thomas NE, et al. Physical activity interventions: effects of duration and intensity. Scand J Med Sci Sports. 2011;21(6):e341–50.
Roberts CK, Lee MM, Katiraie M, et al. Strength fitness and body weight status on markers of cardiometabolic health. Med Sci Sports Exerc. 2015;47(6):1211–8.
Ho M, Garnett SP, Baur LA, et al. Impact of dietary and exercise interventions on weight change and metabolic outcomes in obese children and adolescents: a systematic review and meta-analysis of randomized trials. JAMA Pediatr. 2013;167(8):759–68.
Stoner L, Cornwall J. Did the American Medical Association make the correct decision classifying obesity as a disease? Australas Med J. 2014;7(11):462–4.
World Health Organization. The World Health report 2002. Geneva: World Health Organization; 2002.
Riley M, Bluhm B. High blood pressure in children and adolescents. Am Fam Physician. 2012;85(7):693–700.
Law MR, Morris JK, Wald NJ. Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies. BMJ. 2009;338:b1665.
Dias KA, Green DJ, Ingul CB, et al. Exercise and vascular function in child obesity: a meta-analysis. Pediatrics. 2015;136(3):e648–59.
Korner A, Wiegand S, Hungele A, et al. Longitudinal multicenter analysis on the course of glucose metabolism in obese children. Int J Obes (Lond). 2013;37(7):931–6.
Alanazi A. Metformin treatment for obesity in children and adolescents: a meta-analysis and review of literature. Pharmacologia. 2013;4(8):511–8.
Janssen I, Leblanc AG. Systematic review of the health benefits of physical activity and fitness in school-aged children and youth. Int J Behav Nutr Phys Act. 2010;7:40.
Kahn BB, Flier JS. Obesity and insulin resistance. J Clin Invest. 2000;106(4):473–81.
Lambrick DM, Stoner L, Faulkner J, et al. Preventive medicine needs to begin with our children. Int J Prev Med. 2014;5(1):129–31.
Schonfeld-Warden N, Warden CH. Pediatric obesity. An overview of etiology and treatment. Pediatr Clin North Am. 1997;44(2):339–61.
Rosenbaum M, Leibel RL, Hirsch J. Obesity. N Engl J Med. 1997;337(6):396–407.
World Health Organization. Global nutrition targets 2025: childhood overweight policy brief (WHO/NMH/NHD/14.6). Geneva: World Health Organisation; 2014.
LeMura LM, Maziekas MT. Factors that alter body fat, body mass, and fat-free mass in pediatric obesity. Med Sci Sports Exerc. 2002;34:487–96.
Peterson MD, Saltarelli WA, Visich PS, et al. Strength capacity and cardiometabolic risk clustering in adolescents. Pediatrics. 2014;133(4):e896–903.
Lobelo F, Stoutenberg M, Hutber A. The Exercise is Medicine global health initiative: a 2014 update. Br J Sports Med. 2014;48(22):1627–33.
Sallis RE. Exercise is medicine and physicians need to prescribe it! Br J Sports Med. 2009;43(1):3–4.
Coombes JS, Law J, Lancashire B, et al. “Exercise is Medicine”: curbing the burden of chronic disease and physical inactivity. Asia Pac J Public Health. 2015;27(2):NP600–5.
Exercise is Medicine Network: Pediatrics. http://www.exerciseismedicine.org/support_page.php?p=87. Accessed 21 May 2015.
Hainer V, Toplak H, Stich V. Fat or fit: what is more important? Diabetes Care. 2009;32(Suppl 2):S392–7.
Moschonis G, Mougios V, Papandreou C, et al. “Leaner and less fit” children have a better cardiometabolic profile than their “heavier and more fit” peers: the Healthy Growth Study. Nutr Metab Cardiovasc Dis. 2013;23(11):1058–65.
Stoner L, Lambrick DM, Faulkner J. We’re not ready to encourage children to be “lean” rather than “fit”. Nutr Metab Cardiovasc Dis. 2014;24(1):e6–7.
Castro N, Faulkner J, Skidmore P, et al. Pre-adolescent cardio-metabolic associations and correlates: PACMAC methodology and study protocol. BMJ Open. 2014;4(9):e005815.
Rush E, McLennan S, Obolonkin V, et al. Beyond the randomised controlled trial and BMI: evaluation of effectiveness of through-school nutrition and physical activity programmes. Public Health Nutr. 2015;18(9):1578–81.
Cornwall J, Stoner L. School-based health interventions should be assessed with measures of fitness and fatness: comment on ‘Beyond the randomised controlled trial and BMI: evaluation of effectiveness of through-school nutrition and physical activity programmes’. Public Health Nutr. 2015;18(11):2094.
Young Y, Abdolhosseini P, Brown F, et al. Reliability of oscillometric central blood pressure and wave reflection readings: effects of posture and fasting. J Hypertens. 2015;33(8):1588–93.
Parikh P, Mochari H, Mosca L. Clinical utility of a fingerstick technology to identify individuals with abnormal blood lipids and high-sensitivity C-reactive protein levels. Am J Health Promot. 2009;23(4):279–82.
Barrett SC, Huffman FG, Johnson P. Validation of finger-prick testing of fasting blood glucose, total cholesterol, and HbA1c in adolescents. J Near-Patient Test Tech. 2011;10(2):51–8.
Ministry of Health. Healthy Families NZ. 2015. http://www.health.govt.nz/our-work/preventative-health-wellness/healthy-families-nz. Accessed 6 Jun 2015.
Healthy Together Victoria. 2015. http://www.healthytogether.vic.gov.au/. Accessed 6 Jun 2015.
Galea S, Riddle M, Kaplan GA. Causal thinking and complex system approaches in epidemiology. Int J Epidemiol. 2010;39(1):97–106.
Bayon V, Leger D, Gomez-Merino D, et al. Sleep debt and obesity. Ann Med. 2014;46(5):264–72.
Lucassen EA, Rother KI, Cizza G. Interacting epidemics? Sleep curtailment, insulin resistance, and obesity. Ann N Y Acad Sci. 2012;1264:110–34.
Lambiase MJ, Gabriel KP, Kuller LH, et al. Temporal relationships between physical activity and sleep in older women. Med Sci Sports Exerc. 2013;45(12):2362–8.
Martinez-Gomez D, Veiga OL, Gomez-Martinez S, et al. Behavioural correlates of active commuting to school in Spanish adolescents: the AFINOS (Physical Activity as a Preventive Measure Against Overweight, Obesity, Infections, Allergies, and Cardiovascular Disease Risk Factors in Adolescents) study. Public Health Nutr. 2011;14(10):1779–86.
Tricket E, Beehler S, Deutsch C, et al. Advancing the science of community-level interventions. Fram Health Matters. 2011;101(8):1410–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No sources of funding were used to assist in the preparation of this article.
Conflict of interest
Lee Stoner, David Rowlands, Ariel Morrison, Daniel Credeur, Michael Hamlin, Kim Gaffney, Danielle Lambrick and Anna Matheson declare that they have no conflicts of interest relevant to the content of this review.
Rights and permissions
About this article
Cite this article
Stoner, L., Rowlands, D., Morrison, A. et al. Efficacy of Exercise Intervention for Weight Loss in Overweight and Obese Adolescents: Meta-Analysis and Implications. Sports Med 46, 1737–1751 (2016). https://doi.org/10.1007/s40279-016-0537-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-016-0537-6