Abstract
Background
Very few clinical trials have investigated the effect of topical acne treatment on scarring.
Objectives
Our objective was to evaluate the efficacy of adapalene 0.3%/benzoyl peroxide 2.5% gel (A0.3/BPO2.5) in atrophic acne scar formation in patients with acne.
Methods
In this multicenter, randomized, investigator-blinded, vehicle-controlled study, subjects with moderate or severe facial acne (Investigator’s Global Assessment [IGA] score 3 or 4; ≥ 25 inflammatory lesions; ten or more atrophic acne scars) applied A0.3/BPO2.5 or vehicle daily per half face for 24 weeks. Subjects with acne requiring systemic treatment were excluded. Assessments included investigator atrophic acne scar count, Scar Global Assessment (SGA), acne lesion count, IGA, skin roughness and skin texture, subject self-assessment of clinical acne-related scars and satisfaction questionnaire, tolerability, and safety.
Results
Included subjects (n = 67) had mainly moderate acne (92.5% IGA 3); mean scores at baseline were approximately 40 acne lesions and 12 scars per half face. By week 24, the change from baseline in total scar count was − 15.5% for A0.3/BPO2.5 versus + 14.4% for vehicle (approximately 30% difference), with a mean of 9.5 scars versus 13.3 per half face, respectively (p < 0.0001). For SGA at week 24, a total of 32.9% with A0.3/BPO2.5 versus 16.4% with vehicle (p < 0.01) were clear/almost clear. Inflammatory acne lesions decreased by 86.7% for A0.3/BPO2.5 versus 57.9% for vehicle (p < 0.0001), and 64.2 versus 19.4% of subjects, respectively, were IGA clear/almost clear (p < 0.0001) at week 24. Treatment-related AEs were reported by 20.9% for A0.3/BPO2.5 versus 9% for vehicle side, most commonly skin irritation (14.9 vs. 6%, respectively).
Conclusions
Topical A0.3/BPO2.5 prevented and reduced atrophic scar formation. Scar count increased with vehicle (+ 14.4%) but decreased with A0.3/BPO2.5 (− 15.5%) over 24 weeks.
Trial registry
ClinicalTrials.gov identifier NCT02735421.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Very few clinical trials have investigated the effect of topical acne treatment on atrophic acne scars. |
Adapalene 0.3%/benzoyl peroxide 2.5% gel (A0.3/BPO2.5) is effective in the treatment of moderate to severe acne vulgaris and, by treating acne lesions, prevents the formation of scars. |
A0.3/BPO2.5 prevented the formation of scars and reduced the number of existing scars after 24 weeks of treatment. |
Further studies are now warranted, especially in subjects with severe acne, to confirm these promising results and evaluate the best treatment regimen to further reduce atrophic acne scars. |
1 Introduction
Facial scarring is frequent in patients with acne, especially if acne is not treated early and effectively [1, 2]. Atrophic scars, involving loss of tissue, are the most frequently occurring scars. In a recent study of 1942 subjects with acne, 43% had acne scarring and, although the prevalence of acne scars increases with acne severity, even those with mild acne were at risk of scarring [3]. Almost all scars (99%) originate from papules and pustules (inflammatory lesions) and post-inflammatory lesions [4]. As acne scars generally arise from inflammatory acne lesions that are not effectively treated [2], effective treatment can prevent the risk of future scars.
A variety of topical therapies exist for the treatment of mild to moderate acne vulgaris [5, 6]. Topical retinoids target multiple aspects of acne pathophysiology (e.g., normalizing infundibular hyperkeratinization and reducing inflammation) and have a unique class action in reducing the formation of acne precursor lesions (microcomedones) and limiting the development of new lesions [5, 7]. Adapalene is a synthetic retinoid that has anticomedogenic, keratolytic, anti-inflammatory, and immunoregulatory effects. Multiple randomized controlled trials [8,9,10,11] have demonstrated the efficacy and safety of adapalene (0.1 and 0.3% gel).
Given the multi-factorial pathogenesis of acne, combination therapy with agents with complementary mechanisms can simplify therapy [12]. Adapalene 0.1%/benzoyl peroxide 2.5% fixed-dose combination gel (A0.1/BPO2.5 gel; Epiduo® Gel; Galderma Laboratories, TX, USA) combines a retinoid with BPO, which exhibits potent and rapid bactericidal effect on Cutibacterium (formerly Propionibacterium [13]) acnes [14]. A0.1/BPO2.5 gel is recommended as first-line therapy in all but the most severe cases of inflammatory and/or comedonal acne vulgaris [12]. Adapalene 0.3%/BPO 2.5% gel (A0.3/BPO2.5; Epiduo® Forte Gel; Galderma Laboratories) was developed to address greater acne severity levels [15, 16]. Furthermore, the fixed-combination A/BPO gels provide optimal percutaneous absorption of the active compounds compared with free combinations, and in vitro assays have indicated the higher concentration of adapalene (0.3%) in A0.3/BPO2.5 results in the highest absorption [17].
Atrophic scar treatment strategies can be categorized into two broad groups: prevention and correction. A wide range of interventions (e.g., laser resurfacing, dermabrasion) for the latter are available, but they may not be suitable or affordable for all patients [18]. Furthermore, a recent Cochrane review concluded that quality evidence to support the first-line use of any invasive procedure in the treatment of acne scars was lacking, and whether any short-term benefit would translate to long-term effects is unclear [19].
Despite the well-documented efficacy of topical retinoid treatments for primary lesions of acne, information on the efficacy of these treatments in mitigating acne scars is sparse. An exploratory study demonstrated that adapalene 0.3% gel improved skin texture and the appearance of atrophic acne scars according to investigator and subject global assessment over 24 weeks, which may have been related to enhanced collagen production [20]. Additionally, in a previous split-face randomized controlled trial over a 24-week period, A0.1/BPO2.5 gel (containing 0.1% adapalene) was shown to reduce the risk of atrophic scar formation in moderate facial acne and improve the overall appearance of global scarring grade [21].
The objective of this study was to evaluate whether using a higher concentration of retinoid in A0.3/BPO2.5 would also demonstrate efficacy in atrophic acne scars, specifically in subjects with moderate and severe acne.
2 Methods
2.1 Study Design
This was a 24-week randomized, investigator-blinded, vehicle-controlled, intra-individual comparison (right half face vs. left half face) study (ClinicalTrials.gov identifier NCT02735421) conducted at five centers in Canada and one in France. Following a screening visit, study visits were planned at baseline and weeks 1, 4, 8, 12, 16, 20, and 24.
At the end of the study, based on satisfactory investigator-assessed efficacy (on scars and acne lesions), subjects could be treated with once-daily A0.3/BPO2.5 on the whole face for up to 24 additional weeks with two additional visits at weeks 36 and 48 (results not shown).
2.2 Subjects
Male or female subjects aged 16–35 years with Fitzpatrick skin phototype I–IV and a clinical diagnosis of moderate or severe acne vulgaris on the face were enrolled. Eligible subjects had an Investigator Global Assessment (IGA) score of 3 or 4 on both sides; ≥ 25 inflammatory lesions (papules and pustules) with ten or more on each side (excluding the nose); up to two acne nodules ≥ 1 cm for whole face; ten or more atrophic acne scars > 2 mm (for whole face excluding the nose); with an approximately symmetric number of inflammatory and non-inflammatory lesions, and atrophic acne scars on the whole face. Subjects with acne conglobata, acne fulminans, secondary acne, nodulocystic acne, or acne requiring systemic treatment were excluded. Wash-out periods for topical treatments were 2 weeks for corticosteroids, antibiotics, benzoyl peroxide, azelaic acid, hydroxy acids, and other anti-inflammatory drugs and 4 weeks for topical retinoids. The wash-out periods for systemic treatments were 1 month for corticosteroids or antibiotics, 3 months for spironolactone/drospirenone or immunomodulators, and 6 months for oral retinoids or cyproterone acetate/chlormadinone acetate.
2.3 Study Treatment
Subjects were randomized to apply A0.3/BPO2.5 on half their face and vehicle gel on the other half in the evening for 24 weeks. Subjects were instructed to apply two pea-sized amounts per half face and record the applications on a tablet to ensure compliance with the protocol. Subjects were also provided with skin care products to be used on both sides of the face daily: foam wash (Cetaphil® DermaControl™ Oil Control Foam Wash [Galderma Laboratories], morning and evening) and moisturizer (Cetaphil® DermaControl™ Oil Control Moisturizer SPF 30 [Galderma Laboratories], every morning).
2.4 Efficacy Endpoints
The primary efficacy endpoint was atrophic acne scar count per half face at week 24.
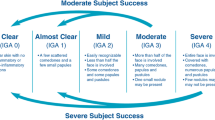
Secondary efficacy endpoints included atrophic acne scar count per half face at each visit (baseline and weeks 1, 4, 8, 12, 16, 20, and 24). Scar Global Assessment (SGA) by investigator on a scale from 0 (clear; no visible scars from acne) to 4 (severe; more than 75% of the half face affected) was performed at each visit. Acne lesion count (non-inflammatory lesions, inflammatory lesions) and IGA of acne severity from 0 (clear; clear skin with no lesions) to 4 (severe; entire face covered with comedones and numerous papules and pustules) were performed per half face at each visit. At baseline and weeks 12 and 24, the investigator assessed skin roughness on a 5-point scale from 0 (none; very smooth) to 4 (severe; very rough) and skin texture change on a 7-point scale from 0 (worse) to 6 (91–100% complete improvement).
2.5 Patient-Reported Outcomes
Subjects completed a Self-assessment of Clinical Acne-Related Scars (SCARS) questionnaire (on a scale from 0 to 10) at baseline and weeks 12 and 24 and a subject satisfaction questionnaire at week 24.
2.6 Safety Endpoints
Adverse events (AEs) were recorded at each study visit. Local tolerability (signs and symptoms of erythema, scaling, dryness, and/or stinging/burning) was assessed on a scale from 0 (none) to 3 (severe).
2.7 Sample Size Calculation
Based on results from a previous intra-individual trial designed as a right–left comparison of A0.1/BPO2.5 gel versus vehicle, a sample size of 50 evaluable subjects was necessary to ensure 80% power to detect superiority of A0.3/BPO2.5 over vehicle. Assuming 20% of subjects would be excluded from the analysis at week 24, a total of 60 enrolled subjects were required.
2.8 Randomization and Blinding
Prior to the start of the study, a randomization list was generated by the statistician, and unique kit numbers were allocated to eligible subjects. The RANUNI routine of the Statistical Analysis System (SAS Institute Inc., Cary, NC, USA) was utilized for kit number generation to randomly assign the active treatment or vehicle to the right or left side of the subject’s face. The study design was considered investigator-blind since the topical trial products were packaged in identical tubes and dispensed by a third party and neither the product dispenser nor the investigator had access to the unblinded randomization list.
2.9 Statistical Methods
For the primary efficacy endpoint, the mean difference between each half face (randomly allocated to vehicle or A0.3/BPO2.5) for total atrophic acne scar count at week 24 was analyzed with the Wilcoxon rank signed test to address the hypothesis of equality on the intent-to-treat population (ITT; all randomized subjects). Per protocol (PP) analysis (all ITT subjects who met all major protocol criteria) was also performed to assess the robustness of the results obtained. Similarly, secondary efficacy endpoints were analyzed on these populations. Safety and local tolerance were recorded on the all patients treated (APT) population. The Statistical Analysis System version 9.3 was used for all analyses, and all tests were two-sided with significance at the 0.05 level.
3 Results
3.1 Demographic and Clinical Characteristics
In total, 54 (80.6%) of the 67 subjects randomized completed the study between May 2016 and November 2017. Reasons for premature discontinuation were subject request (9%), lost to follow-up (4.5%), AE (3%), pregnancy (1.5%), and other (1.5%). The PP population comprised 51 subjects.
Two-thirds of subjects were female (65.7%), mean age was 21.5 years, and mean duration of acne was 6.8 years (Table 1). Most subjects were phototype II (47.8%) or III (34.3%). Most subjects had mild (62.7%) or moderate (29.9%) scars, and subjects had an average of 12 scars per side. The majority had moderate acne (92.5%) and a mean of 40 acne lesions (18 inflammatory lesions, 22 non-inflammatory lesions) per side. Most subjects (79.1%) had a skin roughness assessment of somewhat smooth or slightly rough.
3.2 Efficacy
At 24 weeks, a difference of 3.8 scars per half face was observed for A0.3/BPO2.5 compared with vehicle (mean 9.5 [range 0–27] vs. 13.3 [0–36] total scar count, ITT population; p < 0.0001) (Fig. 1a). These efficacy results were confirmed by PP analysis with a difference of 4.3 scars at week 24 (mean total scar count 9.6 [range 0–27] A0.3/BPO2.5 vs. 13.9 [0–36] vehicle; p < 0.0001). Scar reduction (percentage change from baseline in total atrophic scar count) with A0.3/BPO2.5 was observed over time, with statistical significance compared with vehicle at week 1 and all study visits (Fig. 1b). The percentage change in total atrophic scar count at 24 weeks was a decrease of 15.5% for A0.3/BPO2.5 compared with an increase of 14.4% for vehicle, i.e., a difference of approximately 30% (Fig. 1b). A 16.5% difference in SGA clear/almost clear was observed between the A0.3/BPO2.5 and vehicle at 24 weeks (32.9 vs. 16.4%; p < 0.01) (Fig. 1c).
Effect on scars demonstrated by a total atrophic scar count at week 24, b mean percentage change from baseline of total atrophic scar count by visit (ITT; N = 67), and c percentage of subjects with Scar Global Assessment clear/almost clear by visit (ITT; N = 67). A0.3/BPO2.5 adapalene 0.3%/benzoyl peroxide 2.5% gel, ITT intention to treat, LOCF last observation carried forward, PP per protocol
Reductions in acne lesions were observed in both groups, with significant superiority for A0.3/BPO2.5 by week 1 and all subsequent study visits (all p < 0.005) (Fig. 2). Between baseline and week 24, the percentage reduction in acne lesion counts was greater for the A0.3/BPO2.5 side than for the vehicle side, with differences of 22.4% (− 73.3 vs. − 50.9% vehicle), 28.8% (− 86.7 vs. − 57.9% vehicle), and 18.1% (− 59.5 vs. − 41.4% vehicle) for total, inflammatory, and non-inflammatory lesions, respectively (Fig. 2).
Global improvement of acne was observed in both groups, but significantly more subjects were IGA clear/almost clear with A0.3/BPO2.5 than with vehicle at all study visits and as early as week 1 (all p < 0.0001) (Fig. 3). After 24 weeks, 45% more subjects were clear/almost clear with A0.3/BPO2.5 than with vehicle (64.2 vs. 19.4%, respectively).
At the week 24 visit, 46.0% A0.3/BPO2.5 versus 28.6% vehicle side had no or minimal roughness. Improvement in skin texture was observed for 81.0% of subjects with A0.3/BPO2.5 versus 36.6% with vehicle; a marked or better improvement in skin texture was reported for 31.8 versus 14.3%, respectively.
Representative photographs illustrating two subjects at baseline, week 12 and week 24 are shown in Fig. 4.
Representative photographs of two subjects who applied adapalene 0.3%/benzoyl peroxide 2.5% gel on the right side of their face and vehicle on the left side. a An 18-year-old subject with Scar Global Assessment (SGA) scores of mild on both sides at baseline (scar count: eight scars A0.3/BPO2.5 vs. five vehicle) and, at week 24, mild SGA on the A0.3/BPO2.5 side (11 scars) and moderate SGA on the vehicle side (16 scars). b A 16-year-old subject with moderate SGA on both sides at baseline (scar count: 32 scars on each side) and moderate SGA on both sides at week 24 (27 scars A0.3/BPO2.5 side vs. 29 scars vehicle side)
3.3 Patient-Reported Outcomes
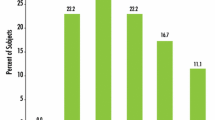
According to the subject SCAR questionnaire, the median severity (0–10 scale) of indents or holes was 4.0 for A0.3/BPO2.5 and 3.6 for the vehicle side at baseline compared with 1.6 versus 2.9, respectively, after 24 weeks (p < 0.0001). Regarding the number of visible indents or holes, the percentage reporting at least some (i.e., some/quite a lot/many) at baseline was 62.5% for A0.3/BPO2.5 versus 66.7% for vehicle compared with 34.5 versus 60.4%, respectively, at week 24 (p < 0.0001) (Fig. 5a). At week 24, the percentage reporting that the indent or holes were moderately visible or very visible was 24.1% for A0.3/BPO2.5 versus 51.8% for vehicle (p = 0.0013) (Fig. 5b).
According to the subject satisfaction questionnaire at week 24, a total of 90.1% indicated they were satisfied to very satisfied with A0.3/BPO2.5 versus 59.0% for vehicle, and 59.0 versus 32.8% were very satisfied, respectively (p < 0.0001). Similarly, 86.8% of subjects were satisfied to very satisfied with the time that A0.3/BPO2.5 took to work versus 50.9% for vehicle (p < 0.0001).
3.4 Safety
No serious or severe AEs were reported. Treatment-related AEs were reported for 25.4% of subjects, with 20.9% specifically on the A0.3/BPO2.5 side compared with 9.0% on the vehicle side (Table 2). The most common treatment-related AEs were skin irritation (14.9% A0.3/BPO2.5 vs. 6.0% vehicle) and pain of skin (3.0% A0.3/BPO2.5 vs. 1.5% vehicle). Two subjects had treatment-related AEs on the A0.3/BPO2.5 side that led to study discontinuation, one subject with moderate pain of skin on both sides of the face and one subject with mild skin irritation.
Concerning local tolerance, slightly more stinging/burning was observed with A0.3/BPO2.5 than vehicle, especially during the first week of treatment, with a mean score of 0.9 A0.3/BPO2.5 versus 0.3 vehicle; the mean scores had decreased to 0.5 versus 0.2, respectively, by week 4 (Fig. 6). Similarly, mild scaling, dryness, and erythema were observed with A0.3/BPO2.5 at week 1, with mean scores of 1.2, 1.0, and 0.9, respectively, compared with 0.5, 0.4, and 0.6, respectively, for vehicle.
At week 24, a total of 44.3% of subjects indicated they were not bothered at all by side effects: A0.3/BPO2.5 versus 77.0% with vehicle (p < 0.0001).
4 Discussion
In these subjects with mainly moderate acne and an average of 12 scars per half face at baseline, the decrease in scar count with A0.3/BPO2.5 was significantly superior to vehicle at all study visits. By week 24, the mean decrease was approximately two acne scars per half face for A0.3/BPO2.5 compared with an increase with vehicle (approximately two acne scars), i.e., there would be a difference of around eight scars if the whole face were to be treated. The difference in percentage change from baseline to week 24 in total atrophic scar count was approximately 30% (− 15.5% A0.3/BPO2.5 vs. + 14.4% vehicle). In a previous study with a lower concentration of retinoid, scar counts remained stable after 6 months of treatment with A0.1/BPO2.5 but increased by approximately 25% with vehicle (mean scar count 11.58 vs. 13.55, respectively, per half face at 24 weeks; p = 0.036) [21]. With the higher adapalene concentration of 0.3% in this study with A0.3/BPO2.5, the scar count was reduced over 24 weeks of treatment rather than remaining stable with the lower concentration of adapalene. Interestingly, the increase in scar count with vehicle over this 24-week study (+ 14.4%) was lower than the increase with vehicle in that previous study (+ 25%) [21], which may have been due to providing a skin care regimen (foam wash and moisturizer) to improve the skin barrier; the vehicle combined with the skin care regimen may have had an effect on inflammatory lesions and contributed to an improvement in skin texture and roughness. A vehicle effect may occur in dermatological studies because there is no strict placebo.
Global scar improvement, as measured by SGA, was also superior with A0.3/BPO2.5 compared with vehicle, with 32.9% A0.3/BPO2.5 versus 16.4% vehicle clear/almost clear at week 24. The patient-reported outcome (PRO) results very closely resembled the SGA (investigator) results since, at week 24, the percentage of patients indicating they saw very few indents or holes was 31.0% on the A0.3/BPO2.5 side versus 15.5% on the vehicle side. Admittedly, improvement in skin roughness and skin texture are not validated scales, but the results after 24 weeks of treatment further corroborate the SGA results.
Atrophic acne scars form continuously and can be permanent or transient [4]. A hypothesis for the higher reduction in scars with the higher concentration of retinoid (A0.3/BPO2.5 vs. A0.1/BPO2.5 in the previous study) may be an increase in the speed of regression of transient scars and/or treatment (or improvement) of pre-existing permanent scars, by remodeling of the dermal matrix with a higher concentration of retinoid. Loss of dermal matrix via degradation of collagen, induced by inflammation, is a contributing factor in atrophic acne scars [22]. Gene array expression profiling comparing lesional and non-lesional skin in patients with acne indicated a prominent role of inflammation and matrix remodeling, including matrix metalloproteinases, inflammatory cytokines, and antimicrobial peptides in acne lesions [23, 24]. Furthermore, treatment with topical tretinoin has been shown to stimulate the production of procollagen in photodamaged skin [25, 26]. As both photodamaged skin and atrophic acne scars are associated with loss of dermal matrix, A0.3/BPO2.5 may exert a beneficial effect on pre-existing atrophic scars. A phase II pilot study in 20 subjects with a history of acne and moderate to severe acne scars receiving adapalene 0.3% for 24 weeks (once daily for 4 weeks then twice daily for 20 weeks) provided evidence for the improvement of atrophic scars with adapalene 0.3% [20]. Immunohistochemical analysis showed increased staining for procollagen-1 and collagen-3, supporting a remodeling effect of adapalene 0.3% gel, which was shown to improve skin texture and the appearance of atrophic acne scars, with a significant improvement in global scar grades [20].
The effect on occurrence of new scars probably reflected the high efficacy of A0.3/BPO2.5 compared with vehicle on the reduction of inflammatory acne lesions, with improvement as early as week 1 and continuing to week 24. The median percentage reduction in inflammatory lesion counts by week 12 (73.3% A0.3/BPO2.5 vs. 41.2% vehicle) was very similar to the mean percentage change at week 12 (68.7% A0.3/BPO2.5 vs. 39.2% vehicle) observed in the pivotal phase III study [15]. Similarly, the percentage IGA clear/almost clear at week 12 (31.4% A0.3/BPO2.5 vs. 11.9% vehicle; p < 0.0001) was very similar to the results of the pivotal phase III study (33.7 vs. 11.0% vehicle, respectively; p < 0.001) [15]. By continuing up to 24 weeks in our study, the percentage of subjects with clear/almost clear skin continued to increase and doubled between week 12 and week 24 on the A0.3/BPO2.5 side (64.2 vs. 19.4% vehicle side at week 24).
The phase III study was 12 weeks long (as is the case for most randomized controlled trials with acne medication designed to be approved by regulatory authorities). However, in our study, the progressive incremental increase in efficacy and effect on scars observed with A0.3/BPO2.5 over 24 weeks highlights the importance of a longer duration of treatment. In fact, 3 months may be sufficient to observe resolution of the primary acne lesions, but the remodeling processes occur slowly, and 6 months may be required to induce significant stimulation of the dermal fibroblasts and collagen and clinically observe an effect on scars [20].
Mild irritation of facial skin is expected with topical retinoids, but most side effects resolve within 2–3 weeks of continued use of retinoids; moisturizers and pH-balanced, non-soap cleansers can be used to improve both efficacy and tolerability [12, 27]. It is also important to educate patients about irritation, manage expectations, and improve adherence to treatment [28]. Modulating treatment regimens during the first 4 weeks has been shown to improve local tolerability without impacting the overall efficacy outcome of A/BPO after 12 weeks and may improve treatment adherence during the first weeks of therapy [29]. In our study, subjects reported more treatment-related AEs on the A0.3/BPO2.5 side than on the vehicle side, and the rates observed in this 24-week study were higher than in the 12-week phase III study [15]. However, most of the AEs were mild in severity, and it is possible that, as the subjects were carefully comparing both sides of their face in this split-face study, they may have been more aware of any AEs. As expected, during the first month (especially the first week), irritation was reported on the A0.3/BPO2.5 side. However, at week 24, a total of 44.3% of subjects with A0.3/BPO2.5 (77.0% with vehicle) indicated they were not bothered at all by side effects, and only two subjects discontinued because of related AEs. Finally, most subjects (90.1%) were overall satisfied to very satisfied with the A0.3/BPO2.5 treatment versus 59.0% for vehicle, including 59.0 versus 32.8% very satisfied, respectively.
Limitations of this study are the split-face design and the inability to completely rule out some systemic contamination of A0.3/BPO2.5 from one side of the face to the other after 24 weeks of treatment, or from subjects inadvertently transferring gel by rubbing their face during the day. Despite this possibility, differences between the active and vehicle sides were consistently observed, with investigator assessments and PROs demonstrating a continuous reduction in both acne lesions and acne scars over the 24-week study.
Further studies are now warranted, especially in subjects with severe acne, to confirm these promising results and evaluate the best treatment regimen to further reduce atrophic acne scars.
5 Conclusions
Topical A0.3/BPO2.5 is efficacious in reducing acne over 24 weeks, with consequential mitigation of acne scarring, by preventing and reducing the number of acne scars.
References
Layton AM, Henderson CA, Cunliffe WJ. A clinical evaluation of acne scarring and its incidence. Clin Exp Dermatol. 1994;19(4):303–8.
Layton AM, Seukeran D, Cunliffe WJ. Scarred for life? Dermatology. 1997;195(Suppl 1):15–21 (discussion 38–40).
Tan J, Kang S, Leyden J. Prevalence and risk factors of acne scarring among patients consulting dermatologists in the Unites States. J Drugs Dermatol. 2017;16(2):97–102.
Tan J, Bourdès V, Bissonnette R, et al. Prospective study of pathogenesis of atrophic acne scars and role of macular erythema. J Drugs Dermatol. 2017;16(6):566–72.
Thiboutot DM, Dréno B, Abanmi A, et al. Practical management of acne for clinicians: an international consensus from the global alliance to improve outcomes in Acne. J Am Acad Dermatol. 2018;78(2S1):S1–23.
Leyden J, Stein-Gold L, Weiss J. Why topical retinoids are mainstay of therapy for acne. Dermatol Ther (Heidelb). 2017;7(3):293–304.
Thielitz A, Helmdach M, Ropke EM, Gollnick H. Lipid analysis of follicular casts from cyanoacrylate strips as a new method for studying therapeutic effects of antiacne agents. Br J Dermatol. 2001;145:19–27.
Thiboutot D, Pariser DM, Egan N, et al. Adapalene gel 0.3% for the treatment of acne vulgaris: a multicenter, randomized, double-blind, controlled, phase III trial. J Am Acad Dermatol. 2006;54:242–50.
Pariser DM, Thiboutot DM, Clark SD, et al. The efficacy and safety of adapalene gel 0.3% in the treatment of acne vulgaris: a randomized, multicenter, investigator blinded, controlled comparison study versus adapalene gel 0.1% and vehicle. Cutis. 2005;76:145–51.
Weiss JS, Thiboutot DM, Hwa J, et al. Long-term safety and efficacy study of adapalene gel 0.3%. J Drugs Dermatol. 2008;7:s24–8.
Thielitz A, Sidou F, Gollnick H. Control of microcomedone formation throughout a maintenance treatment with adapalene gel, 0.1%. J Eur Acad Dermatol Venereol. 2007;21:747–53.
Gollnick HP, Bettoli V, Lambert J, et al. A consensus-based practical and daily guide for the treatment of acne patients. J Eur Acad Dermatol Venereol. 2016;30(9):1480–90.
Scholz CF, Kilian M. The natural history of cutaneous propionibacteria, and reclassification of selected species within the genus Propionibacterium to the proposed novel genera Acidipropionibacterium gen. nov., Cutibacterium gen. nov. and Pseudopropionibacterium gen. nov. Int J Syst Evol Microbiol. 2016;66(11):4422–32.
Gollnick H, Cunliffe W, Berson D, et al. Management of acne: a report from a global alliance to improve outcomes in acne. J Am Acad Dermatol. 2003;49:S1–37.
Stein Gold L, Weiss J, Rueda MJ, et al. Moderate and severe inflammatory acne vulgaris effectively treated with single-agent therapy by a new fixed-dose combination adapalene 0.3%/benzoyl peroxide 2.5% gel: a randomized, double-blind, parallel-group, controlled study. Am J Clin Dermatol. 2016;17(3):293–303.
Weiss J, Stein Gold L, Leoni M, et al. Customized single-agent therapy management of severe inflammatory acne: a randomized, double-blind, parallel-group, controlled study of a new treatment—adapalene 0.3%-benzoyl peroxide 2.5% gel. J Drugs Dermatol. 2015;14(12):1427–35.
Osman-Ponchet H, Sevin K, Gaborit A, et al. Fixed-combination gels of adapalene and benzoyl peroxide provide optimal percutaneous absorption compared to monad formulations of these compounds: results from two in vitro studies. Dermatol Ther (Heidelb). 2017;7(1):123–31.
Goodman GJ. Treatment of acne scarring. Int J Dermatol. 2011;50(10):1179–94 (Review).
Abdel Hay R, Shalaby K, Zaher H, et al. Interventions for acne scars. Cochrane Database Syst Rev. 2016;4:CD011946.
Loss M, Leung S, Chien A et al. Adapalene 0.3% gel shows efficacy for the treatment of atrophic acne scars. Dermatol Ther (Heidelb). 2018. https://doi.org/10.1007/s13555-018-0231-8.
Dreno B, Tan J, Rivier M, et al. Adapalene 0.1%/benzoyl peroxide 2.5% gel reduces the risk of atrophic scar formation in moderate inflammatory acne: a split-face randomized controlled trial. J Eur Acad Dermatol Venereol. 2017;31(4):737–42.
Kang S, Cho S, Chung JH, et al. Inflammation and extracellular matrix degradation mediated by activated transcription factors nuclear factor-kappaB and activator protein-1 in inflammatory acne lesions in vivo. Am J Pathol. 2005;166(6):1691–9.
Trivedi NR, Gilliland KL, Zhao W, et al. Gene array expression profiling in acne lesions reveals marked upregulation of genes involved in inflammation and matrix remodeling. J Investig Dermatol. 2006;126(5):1071–9.
Uchida G, Yoshimura K, Kitano Y, et al. Tretinoin reverses upregulation of matrix metalloproteinase-13 in human keloid derived fibroblasts. J Exp Dermatol. 2003;12(Suppl 2):35–42.
Griffiths CE, Russman AN, Majmudar G, et al. Restoration of collagen formation in photodamaged human skin by tretinoin (retinoic acid). N Engl J Med. 1993;329(8):530–5.
Kang S, Voorhees JJ. Photoaging therapy with topical tretinoin: an evidence-based analysis. J Am Acad Dermatol. 1998;39(2 Pt 3):S55–61 (Review).
Bouloc A, Roo E, Imko-Walczuk B, et al. A skincare combined with combination of adapalene and benzoyl peroxide provides a significant adjunctive efficacy and local tolerance benefit in adult women with mild acne. J Eur Acad Dermatol Venereol. 2017;31(10):1727–31.
Myhill T, Coulson W, Nixon P, et al. Use of supplementary patient education material increases treatment adherence and satisfaction among acne patients receiving adapalene 0.1%/benzoyl peroxide 2.5% gel in primary care clinics: a multicenter, randomized, controlled clinical study. Dermatol Ther (Heidelb). 2017;7(4):515–24.
Tan J, Bissonnette R, Gratton D et al. The safety and efficacy of four different fixed combination regimens of adapalene 0.1%/benzoyl peroxide 2.5% gel in the treatment of acne vulgaris: results from a randomized controlled study. Eur J Dermatol. 2018 (in press).
Acknowledgements
Medical writing support in the preparation of this publication, in accordance with good publication practice (GPP3), was provided by Helen Simpson, PhD, of Galderma R&D. The authors are responsible for all content and editorial decisions and received no honoraria related to the development of this publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was funded by Galderma R&D/Nestle Skin Health. Open access was funded by Galderma R&D/Nestle Skin Health.
Conflict of interest
The investigators (JT, RB, AGH, BB, CL, BD) received financial support for conducting the study. Dr. B. Dréno has been an investigator and/or consultant for Bioderma, Galderma, Pierre Fabre, and La Roche Posay. Dr. R. Bissonnette has been an investigator, consultant, advisory board member, and speaker for BioPharmX, Cipher, Dermira, Galderma, GSK-Stiefel, Valeant, and Xenon and is a shareholder of Innovaderm Research. Dr. A. Gagné-Henley has been an investigator, consultant, advisory board member, and/or speaker for Abbvie, Celgene, Dignity, Galderma, Janssen, Leo pharma, Novartis, Sanofi, Valeant, and Xenon. Dr. B. Barankin has been a consultant and speaker for Galderma. Dr. C. Lynde has been a consultant, advisory board member, and speaker for Bayer, Galderma, GSK, and Valeant. Dr. J. Tan has been an investigator, consultant, advisory board member, and speaker, and has provided expert testimony, for Galderma. Mr N. Kerrouche is an employee of Galderma R&D.
Ethical approval
This study was conducted in accordance with the principles of the Declaration of Helsinki and in compliance with the International Conference on Harmonization-Good Clinical Practice and local regulatory requirements. The study was reviewed and approved by the appropriate Independent Ethics Committees, and written informed consent was obtained from all subjects prior to study initiation. Additional informed consent was obtained from all individual participants whose photographs are included in this article.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Dréno, B., Bissonnette, R., Gagné-Henley, A. et al. Prevention and Reduction of Atrophic Acne Scars with Adapalene 0.3%/Benzoyl Peroxide 2.5% Gel in Subjects with Moderate or Severe Facial Acne: Results of a 6-Month Randomized, Vehicle-Controlled Trial Using Intra-Individual Comparison. Am J Clin Dermatol 19, 275–286 (2018). https://doi.org/10.1007/s40257-018-0352-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40257-018-0352-y