Abstract
Purpose of Review
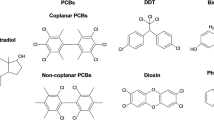
In modern society, we are exposed to a wide variety of manufactured chemical compounds, called “endocrine-disrupting chemicals” (EDCs). EDCs interact with hormone receptors and have a detrimental effect on reproduction, a complex and hormonally regulated process. Two widely prevalent groups of EDCs are bisphenols and phthalates. This review aims to evaluate and summarize current research on EDCs and their proposed relationship with increased rates of pregnancy loss.
Recent Findings
Most research focuses on one of many bisphenols, bisphenol A or BPA. Studies of BPA in animals have shown a causative effect on pregnancy loss even at low concentrations, likely through disruption of hormone receptor expression in the uterine lining that impedes implantation. Human studies have correlated levels of BPA exposure with pregnancy loss and suggest a role for synergistic effect of BPAs with other EDCs. Phthalate studies include multiple different metabolites that have variably been associated with pregnancy loss. The mechanism of phthalate effect on pregnancy loss appears to be through disruption of timing of implantation or cell apoptosis. In humans, a trend has been suggested between high levels of phthalate exposure and increased pregnancy loss.
Summary
Recent research supports an association between EDCs in the environment and pregnancy loss, particularly for BPAs, but the effect in humans is less well developed and studies appreciably limited. Further research is needed not only on the effect of these individual compounds on pregnancy loss but on which populations may be at greatest risk.
Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Carson R. Silent Spring. Boston: Houghton Mifflin; 1962.
Lutts RH. Chemical fallout: Rachel Carson’s silent spring, radioactive fallout, and the environmental movement. Environ Rev ER. 1985;9:211–25.
ACOG Committee Opinion No. 575. Exposure to toxic environmental agents. Obstet Gynecol. 2013;122:931–5.
Birnbaum LS. State of the Science of Endocrine Disruptors. Environ Health Perspect [Internet]. 2013 [cited 2018 Dec 29];121. Available from: https://ehp.niehs.nih.gov/doi/10.1289/ehp.1306695. Accessed 29 Dec 2018.
Norwitz ER, Schust DJ, Fisher SJ. Implantation and the survival of early pregnancy. N Engl J Med. 2001;345:1400–8.
Daya S, Stephenson MD. Frequency of factors associated with habitual abortion in 197 couples. Fertil Steril. 1996;66:24–9.
Santangeli S, Maradonna F, Olivotto I, Piccinetti CC, Gioacchini G, Carnevali O. Effects of BPA on female reproductive function: the involvement of epigenetic mechanism. Gen Comp Endocrinol. 2017;245:122–6.
Cabaton NJ, Wadia PR, Rubin BS, Zalko D, Schaeberle CM, Askenase MH, et al. Perinatal exposure to environmentally relevant levels of bisphenol a decreases fertility and fecundity in CD-1 mice. Environ Health Perspect. 2011;119:547–52.
Meruvu S, Zhang J, Bedi YS, Choudhury M. Mono-(2-ethylhexyl) phthalate induces apoptosis through miR-16 in human first trimester placental cell line HTR-8/SVneo. Toxicol in Vitro. 2016;31:35–42.
Vogel SA. The Politics of plastics: the making and unmaking of bisphenol A “safety.”. Am J Public Health. 2009;99:S559–66.
Calafat AM, Ye X, Wong LY, Reidy JA, Needham LL. Exposure of the U.S. population to bisphenol A and 4-tertiary-octylphenol: 2003–2004. Environ Health Perspect. 2008;116:39–44.
Ikezuki Y, Tsutsumi O, Takai Y, Kamei Y, Taketani Y. Determination of bisphenol A concentrations in human biological fluids reveals significant early prenatal exposure. Hum Reprod Oxf Engl. 2002;17:2839–41.
Cao X-L, Zhang J, Goodyer CG, Hayward S, Cooke GM, Curran IHA. Bisphenol A in human placental and fetal liver tissues collected from Greater Montreal area (Quebec) during 1998-2008. Chemosphere. 2012;89:505–11.
Blair RM, Fang H, Branham WS, Hass BS, Dial SL, Moland CL, et al. The estrogen receptor relative binding affinities of 188 natural and xenochemicals: structural diversity of ligands. Toxicol Sci Off J Soc Toxicol. 2000;54:138–53.
Silva E, Rajapakse N, Kortenkamp A. Something from “nothing”--eight weak estrogenic chemicals combined at concentrations below NOECs produce significant mixture effects. Environ Sci Technol. 2002;36:1751–6.
Welshons WV, Nagel SC, Vom Saal FS. Large effects from small exposures. III. Endocrine mechanisms mediating effects of bisphenol A at levels of human exposure. Endocrinology. 2006;147:S56–69.
Wozniak AL, Bulayeva NN, Watson CS. Xenoestrogens at picomolar to nanomolar concentrations trigger membrane estrogen receptor-alpha-mediated Ca2+ fluxes and prolactin release in GH3/B6 pituitary tumor cells. Environ Health Perspect. 2005;113:431–9.
Varayoud J, Ramos JG, Bosquiazzo VL, Muñoz-de-Toro M, Luque EH. Developmental exposure to bisphenol A impairs the uterine response to ovarian steroids in the adult. Endocrinology. 2008;149:5848–60.
Varayoud J, Ramos JG, Bosquiazzo VL, Lower M, Muñoz-de-Toro M, Luque EH. Neonatal exposure to bisphenol A alters rat uterine implantation-associated gene expression and reduces the number of implantation sites. Endocrinology. 2011;152:1101–11.
Berger RG, Hancock T, de Catanzaro D. Influence of oral and subcutaneous bisphenol-A on intrauterine implantation of fertilized ova in inseminated female mice. Reprod Toxicol. 2007;23:138–44.
• Tran DN, Jung E-M, Ahn C, Lee J-H, Yoo Y-M, Jeung E-B. Effects of bisphenol A and 4-tert-octylphenol on embryo implantation failure in mouse. Int J Environ Res Public Health. 2018;15:1614 A recent study that investigates the mechanism of proposed BPA effect on implantation failure.
Liliana R, Slawomir G, Tomasz J, Joanna W, Andrzej P. The effects of bisphenol A (BPA) on sympathetic nerve fibers in the uterine wall of the domestic pig. Reprod Toxicol. 2019;84:39–48. https://doi.org/10.1016/j.reprotox.2018.12.004.
Aldad TS, Rahmani N, Leranth C, Taylor HS. Bisphenol-A (BPA) exposure alters endometrial progesterone receptor expression in the non-human primate. Fertil Steril. 2011;96:175–9.
Borman ED, Foster WG, Greenacre MKE, Muir CC, de Catanzaro D. Stress lowers the threshold dose at which bisphenol A disrupts blastocyst implantation, in conjunction with decreased uterine closure and e-cadherin. Chem Biol Interact. 2015;237:87–95.
• Pollack AZ, Mumford SL, Krall JR, Carmichael AE, Sjaarda LA, Perkins NJ, et al. Exposure to bisphenol A, chlorophenols, benzophenones, and parabens in relation to reproductive hormones in healthy women: a chemical mixture approach. Environ Int. 2018;120:137–44 A recent study suggesting synergistic effects of environmental toxins on reproduction.
Buck Louis GM, Smarr MM, Patel CJ. The exposome research paradigm: an opportunity to understand the environmental basis for human health and disease. Curr Environ Health Rep. 2017;4:89–98.
Hunt PA, Koehler KE, Susiarjo M, Hodges CA, Ilagan A, Voigt RC, et al. Bisphenol A exposure causes meiotic aneuploidy in the female mouse. Curr Biol. 2003;13:546–53.
Campen KA, Kucharczyk KM, Bogin B, Ehrlich JM, Combelles CMH. Spindle abnormalities and chromosome misalignment in bovine oocytes after exposure to low doses of bisphenol A or bisphenol S. Hum Reprod. 2018;33:895–904.
Lathi RB, Liebert CA, Brookfield KF, Taylor JA, vom Saal FS, Fujimoto VY, et al. Conjugated bisphenol A in maternal serum in relation to miscarriage risk. Fertil Steril. 2014;102:123–8.
Shen Y, Zheng Y, Jiang J, Liu Y, Luo X, Shen Z, et al. Higher urinary bisphenol A concentration is associated with unexplained recurrent miscarriage risk: evidence from a case-control study in eastern China. PLoS One. 2015;10:e0127886.
Chen X, Chen M, Xu B, Tang R, Han X, Qin Y, et al. Parental phenols exposure and spontaneous abortion in Chinese population residing in the middle and lower reaches of the Yangtze River. Chemosphere. 2013;93:217–22.
Ehrlich S, Williams PL, Missmer SA, Flaws JA, Ye X, Calafat AM, et al. Urinary bisphenol A concentrations and early reproductive health outcomes among women undergoing IVF. Hum Reprod. 2012;27:3583–92.
Mínguez-Alarcón L, Gaskins AJ, Chiu Y-H, Williams PL, Ehrlich S, Chavarro JE, et al. Urinary bisphenol a concentrations and association with in vitro fertilization outcomes among women from a fertility clinic. Hum Reprod Oxf Engl. 2015;30:2120–8.
Chin HB, Jukic AM, Wilcox AJ, Weinberg CR, Ferguson KK, Calafat AM, et al. Association of urinary concentrations of phthalate metabolites and bisphenol A with early pregnancy endpoints. Environ Res. 2019;168:254–60.
Mu D, Gao F, Fan Z, Shen H, Peng H, Hu J. Levels of phthalate metabolites in urine of pregnant women and risk of clinical pregnancy loss. Environ Sci Technol. 2015;49:10651–7.
Lovekamp-Swan T, Davis BJ. Mechanisms of phthalate ester toxicity in the female reproductive system. Environ Health Perspect. 2003;111:139–45.
Melnick AP, Pereira N, Murphy EM, Rosenwaks Z, Spandorfer SD. How low is too low? Cycle day 28 estradiol levels and pregnancy outcomes. Fertil Steril. 2016;105:905–909.e1.
Tomita I, Nakamura Y, Yagi Y, Tutikawa K. Fetotoxic effects of mono-2-ethylhexyl phthalate (MEHP) in mice. Environ Health Perspect. 1986;65:249–54.
Ema M, Miyawaki E, Kawashima K. Effects of dibutyl phthalate on reproductive function in pregnant and pseudopregnant rats. Reprod Toxicol Elmsford N. 2000;14:13–9.
Mankidy R, Wiseman S, Ma H, Giesy JP. Biological impact of phthalates. Toxicol Lett. 2013;217:50–8.
Erkekoglu P, Rachidi W, Yuzugullu OG, Giray B, Favier A, Ozturk M, et al. Evaluation of cytotoxicity and oxidative DNA damaging effects of di(2-ethylhexyl)-phthalate (DEHP) and mono(2-ethylhexyl)-phthalate (MEHP) on MA-10 Leydig cells and protection by selenium. Toxicol Appl Pharmacol. 2010;248:52–62.
Tetz LM, Cheng AA, Korte CS, Giese RW, Wang P, Harris C, et al. Mono-2-Ethylhexyl phthalate induces oxidative stress responses in human placental cells in vitro. Toxicol Appl Pharmacol. 2013;268:47–54.
Ferguson KK, Cantonwine DE, Rivera-González LO, Loch-Caruso R, Mukherjee B, Anzalota Del Toro LV, et al. Urinary phthalate metabolite associations with biomarkers of inflammation and oxidative stress across pregnancy in Puerto Rico. Environ Sci Technol. 2014;48:7018–25.
Gunnar T, Jönsson Bo AG, Lindh Christian H, Kold JT, Hjollund Niels H, Anne V, et al. Association between pregnancy loss and urinary phthalate levels around the time of conception. Environ Health Perspect. 2012;120:458–63.
Jukic AM, Calafat AM, McConnaughey DR, Longnecker MP, Hoppin JA, Weinberg CR, et al. Urinary concentrations of phthalate metabolites and bisphenol A and associations with follicular-phase length, luteal-phase length, fecundability, and early pregnancy loss. Environ Health Perspect. 2016;124:321–8.
•• Messerlian C, Wylie BJ, Minguez-Alarcon L, Williams PL, Ford JB, Souter IC, et al. Urinary concentrations of phthalate metabolites in relation to pregnancy loss among women conceiving with medically assisted reproduction. Epidemiol Camb Mass. 2016;27:879–88 A recent human study supporting the association between phthalates and pregnancy loss.
Hauser R, Gaskins AJ, Souter I, Smith KW, Dodge LE, Ehrlich S, et al. Urinary phthalate metabolite concentrations and reproductive outcomes among women undergoing in vitro fertilization: results from the EARTH Study. Environ Health Perspect. 2016;124:831–9.
Sun Q, Cornelis MC, Townsend MK, Tobias DK, Eliassen AH, Franke AA, et al. Association of urinary concentrations of bisphenol A and phthalate metabolites with risk of type 2 diabetes: a prospective investigation in the Nurses’ Health Study (NHS) and NHSII cohorts. Environ Health Perspect. 2014;122:616–23.
Townsend MK, Franke AA, Li X, Hu FB, Eliassen AH. Within-person reproducibility of urinary bisphenol A and phthalate metabolites over a 1 to 3 year period among women in the Nurses’ Health Studies: a prospective cohort study. Environ Health. 2013;12:80.
Braun JM, Smith KW, Williams PL, Calafat AM, Berry K, Ehrlich S, et al. Variability of urinary phthalate metabolite and bisphenol A concentrations before and during pregnancy. Environ Health Perspect. 2012;120:739–45.
Nir SM. Perfect Nails, Poisoned Workers. N Y Times [Internet]. 2015 May 8 [cited 2019 Jan 6]; Available from: https://www.nytimes.com/interactive/2019/admin/100000003667286.embedded.html?. Accessed 6 Jan 2019.
Zota AR, Shamasunder B. The environmental injustice of beauty: framing chemical exposures from beauty products as a health disparities concern. Am J Obstet Gynecol. 2017;217:418.e1–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Molly Siegel, Sacha Krieg, and Lora Shahine declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Environmental Exposures and Pregnancy Outcomes
Rights and permissions
About this article
Cite this article
Siegel, M., Krieg, S. & Shahine, L. Endocrine Disruptors and Pregnancy Loss. Curr Obstet Gynecol Rep 8, 39–45 (2019). https://doi.org/10.1007/s13669-019-0258-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13669-019-0258-6