Abstract
Introduction
Glycemic control in participants with insulin-treated diabetes remains challenging. We assessed safety and efficacy of new flash glucose-sensing technology to replace self-monitoring of blood glucose (SMBG).
Methods
This open-label randomized controlled study (ClinicalTrials.gov, NCT02082184) enrolled adults with type 2 diabetes on intensive insulin therapy from 26 European diabetes centers. Following 2 weeks of blinded sensor wear, 2:1 (intervention/control) randomization (centrally, using biased-coin minimization dependant on study center and insulin administration) was to control (SMBG) or intervention (glucose-sensing technology). Participants and investigators were not masked to group allocation. Primary outcome was difference in HbA1c at 6 months in the full analysis set. Prespecified secondary outcomes included time in hypoglycemia, effect of age, and patient satisfaction.
Results
Participants (n = 224) were randomized (149 intervention, 75 controls). At 6 months, there was no difference in the change in HbA1c between intervention and controls: −3.1 ± 0.75 mmol/mol, [−0.29 ± 0.07% (mean ± SE)] and −3.4 ± 1.04 mmol/mol (−0.31 ± 0.09%) respectively; p = 0.8222. A difference was detected in participants aged <65 years [−5.7 ± 0.96 mmol/mol (−0.53 ± 0.09%) and −2.2 ± 1.31 mmol/mol (−0.20 ± 0.12%), respectively; p = 0.0301]. Time in hypoglycemia <3.9 mmol/L (70 mg/dL) reduced by 0.47 ± 0.13 h/day [mean ± SE (p = 0.0006)], and <3.1 mmol/L (55 mg/dL) reduced by 0.22 ± 0.07 h/day (p = 0.0014) for intervention participants compared with controls; reductions of 43% and 53%, respectively. SMBG frequency, similar at baseline, decreased in intervention participants from 3.8 ± 1.4 tests/day (mean ± SD) to 0.3 ± 0.7, remaining unchanged in controls. Treatment satisfaction was higher in intervention compared with controls (DTSQ 13.1 ± 0.50 (mean ± SE) and 9.0 ± 0.72, respectively; p < 0.0001). No serious adverse events or severe hypoglycemic events were reported related to sensor data use. Forty-two serious events [16 (10.7%) intervention participants, 12 (16.0%) controls] were not device-related. Six intervention participants reported nine adverse events for sensor-wear reactions (two severe, six moderate, one mild).
Conclusion
Flash glucose-sensing technology use in type 2 diabetes with intensive insulin therapy results in no difference in HbA1c change and reduced hypoglycemia, thus offering a safe, effective replacement for SMBG.
Trial registration
ClinicalTrials.gov identifier: NCT02082184.
Funding
Abbott Diabetes Care.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The number of people with diabetes is increasing globally with 90% having type 2 diabetes, a fifth of whom are on insulin treatment. A significant proportion of adults with insulin-treated type 2 diabetes are less than 65 years of age and frequently have poor glycemic control [1, 2]. Improving glycemia reduces the risk of diabetes complications and is a key management objective [3]. However, intensification of insulin therapy increases the risk of hypoglycemia [4] which is associated with adverse clinical outcome [5], impacts on quality of life [6], and increases treatment costs secondary to hospital admissions, ambulance call-outs, and clinic attendance [7]. Glycated hemoglobin (HbA1c), the gold standard for assessment of glycemic control, is unable to reflect hypoglycemic risk or indicate glucose variability, which recent reports suggest are associated with inferior clinical outcome [8, 9]. Detection of hypoglycemia or glucose variability can be difficult with self-monitoring of blood glucose which is usually the main method used for self-management and adjusting insulin therapy. For participants on intensive insulin therapy, four or more blood glucose tests are required daily to safely and effectively adjust insulin doses. This is not always achieved because of the pain and inconvenience associated with this method of glucose testing [10, 11]. A tool that can support a more comprehensive assessment of glycemia is continuous glucose monitoring; however, current devices are costly, require repeated calibration, and are constantly attached to the patient, all key factors preventing widespread use. There is a need for a new method of glucose monitoring that is affordable and provides clear, comprehensive glucose data with minimal patient inconvenience.
We used a novel sensor-based flash glucose monitoring system (FreeStyle Libre™; Abbott Diabetes Care, Witney, UK). The small, single-use, factory-calibrated, on-body sensor utilizes wired enzyme technology (osmium mediator and glucose oxidase enzyme co-immobilized on an electrochemical sensor) to continuously monitor interstitial glucose levels. The sensor is worn on the back of the arm for up to 14 days and automatically stores glucose data every 15 min. A real-time glucose level may be obtained as often as every minute by scanning the sensor with the reader. A glucose trend arrow (indicating rate and direction of change in glucose levels) and a graphical trace of glucose values for the previous 8-h period are also displayed on the screen. Data are transferred by radio frequency identification (RFID) from the sensor to the reader memory which stores historical sensor data for 90 days. This data can be uploaded using the device software to generate summary glucose reports (including an ambulatory glucose profile) for review by the patient at home or in clinic with their healthcare professional (HCP) [12].
The aim of our study was to assess the role of this new category of glucose-sensing technology on glycemic control in individuals with type 2 diabetes using intensive insulin therapy or continuous subcutaneous insulin infusion (CSII).
Methods
Study Design and Participants
We conducted this 6-month, prospective, open-label, non-masked, two-arm randomized controlled study at 26 European diabetes centers, eight in France, ten in Germany, and eight in the UK (Supplementary Material p. 1).
We enrolled participants aged 18 years or older with type 2 diabetes treated with insulin for at least 6 months and on their current regimen (prandial only or prandial and basal intensive insulin therapy or CSII therapy) for 3 months or more, an HbA1c level 58–108 mmol/mol (7.5–12.0%), self-reported regular blood glucose testing (more than 10/week for at least 2 months prior to study entry), and were considered by the investigator to be technically capable of using the flash sensor-based glucose monitoring system. At each study center, any potentially eligible patient from the general diabetes population was invited to participate in the study.
Participants were not included if they had any other insulin regimen to that described above; a total daily dose of insulin ≥1.75 units/kg on study entry; had severe hypoglycemia (requiring third-party assistance) [13], diabetic ketoacidosis, or hyperosmolar-hyperglycemic state in the preceding 6 months; known allergy to medical-grade adhesives; used continuous glucose monitoring within the previous 4 months; were pregnant or planning pregnancy; were receiving steroid therapy for any condition; or were considered by the investigator to be unsuitable to participate.
Approval was given by the appropriate competent authorities in each country. All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964, as revised in 2013. Informed consent was obtained from all patients for participation in the study.
Randomization and Masking
Participants were centrally randomized in a 2:1 ratio to sensor-based flash glucose monitoring (intervention group) or to self-monitoring of blood glucose (control group) by an interactive web response system (IWRS) using biased-coin minimization, with study center and insulin administration as prognostic factors. The intention of a 2:1 randomization ratio was to ensure a sufficient number of participants in the intervention arm to complete an additional 6-month, open-access study phase. Participants, investigators, and study staff were not masked to group allocation.
Procedures
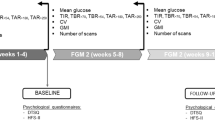
Following consent, screening, and enrollment, all participants wore a system locked into masked mode for the 14-day baseline period and were asked to scan their sensor every 8 h. Sensor glucose measurements were blinded (not visible) to participants and investigators during this phase. Glucose management was supported by continuation of their current regimen for blood glucose monitoring using the strip-port built into the reader and compatible test strips (Abbott Diabetes Care, Witney, Oxon, UK). Participants were asked to record blood glucose levels in a glucose diary and to log other events (e.g., severe hypoglycemia) in an event diary. Participants with sensor data for at least 50% of the blinded wear or at least 650 individual sensor readings (only two subjects did not meet this criterion and withdrew) were centrally randomized to intervention or control group.
For the 6-month treatment phase (post-randomization), the sensor-based glucose monitoring system was unblinded for intervention participants to continuously use sensor glucose data for self-management, including insulin dose decisions, in accordance with the product labelling. No training was provided to these participants for interpretation of glucose sensor data. Their historical data was uploaded at subsequent study visits and glucose reports were generated for review by the HCP with the participant, using the device software [12].
Control participants self-managed their glucose levels utilizing a standard blood glucose device (Abbott Diabetes Care, Witney, UK) and a glucose diary for the duration of the study, wearing a blinded sensor again for the last 2 weeks of the study.
Between randomization and day 194, intervention and control participants had two visits. At these visits, participants' glucose control was reviewed with an HCP and the effects of diet/lifestyle on glucose trends and insulin dose modifications were discussed. There was no preset algorithm for insulin adjustments mandated by the protocol in order to reflect “real-world”. However, common principles were applied that included avoidance of hypoglycemia, optimization of fasting glucose levels, and reduction of postprandial glucose excursions. Intervention participants had a safety visit (day 45) as the device was not on-market when the study commenced.
HbA1c was measured in all participants at baseline, 3 and 6 months with analysis by a central laboratory (ICON Laboratories, Dublin, Ireland).
All participants completed quality of life and patient-reported outcome questionnaires [14,15,16] prior to other study activities on day 1 and on day 194.
Outcomes
The primary outcome was the difference in HbA1c between intervention and control groups at 6 months. Prespecified secondary endpoints were subgroup analyses by age (less than and 65 years or older), sensor-derived glycemic measures from baseline to days 194–208, frequency of glucose finger-sticks and sensor scans per day during the study period, system utilization for days 15–208 (defined as the percentage of data collected, assuming continuous device wear), and change in total daily dose of insulin, body mass index (BMI), weight, and participant questionnaire responses. Sensor-derived glycemic measures comprised number and duration of hypoglycemic events (<3.9 mmol/L [70 mg/dL], and <3.1 mmol/L [55 mg/dL]); time in range (3.9–10.0 mmol/L [70–180 mg/dL]), number and duration of hyperglycemic events (>10.0 mmol/L [180 mg/dL], and >13.3 mmol/L [240 mg/dL]), mean glucose, and glucose variability measures [17,18,19]). An event was defined as at least two consecutive readings, at 15-min intervals, outside the predefined glucose range (the end of an episode was one reading at or inside the predefined range).
Secondary endpoints reported in the clinical study report and not here, include change in HbA1c from baseline to day 105, proportion of participants with reduction in HbA1c of ≥5.5 mmol/mol (0.5%) from baseline, or achieving HbA1c ≤ 58 mmol/mol (7.5%), post-prandial hyperglycemia, blood pressure, lipid levels, HCP questionnaire responses, emergency room visits, hospital admissions, additional clinic time, lancet use and non-insulin medication use.
Results for the user questionnaire (intervention participants only) were assessed at 6 months. Patient-reported outcome and quality of life (QoL) measures were assessed using validated questionnaires: Diabetes Distress Scale (DDS) [14], Diabetes Quality of Life (DQoL) [15], and Diabetes Treatment Satisfaction (DTSQs and DTSQc) [16].
Safety endpoints incorporated all adverse events including severe hypoglycemia (requiring third-party assistance) [13], hypoglycemic events [20], sensor insertion or sensor wear-related symptoms, diabetic ketoacidosis or hyperosmolar hyperglycemic state episodes, and cardiac events.
Statistical Analysis
This study was powered at 90% to detect a difference of 3.8 mmol/mol (0.35%) in HbA1c between the intervention and control group at 6 months with a 5% significance level as per guidance of the Food and Drug Administration [21] and assuming SD for the change of 0.65 [22]. The intervention group was double the size of the control group resulting in a sample size of 210 participants allowing for a dropout rate of 20% post-randomization. Missing values for the primary endpoint were imputed using the last observation carried forward (LOCF) approach. For the sensor data derived secondary endpoints, if less than 72 h of sensor results were available from the final 14-day sensor wear (days 194–208), the last 72 h of available recorded results were used. Analysis of covariance was used to adjust for chance imbalances in baseline measurements between the treatment groups [23], adjusted means were then used to compare differences between the groups for the 6-month endpoints.
Glycemic control and variability results, BMI/weight, and total daily dose of insulin were compared between treatment groups using analysis of covariance of the differences between post-baseline and baseline values with study center and baseline measurement as covariates.
Changes in questionnaire responses were considered using analysis of covariance on baseline values and study center to compare scores from intervention with control group participants.
Confidence intervals were calculated for the group least-square mean of each measure and the difference between group least-square means.
Results presented here are for the full analysis set, which included all randomized participants since there were no pregnancies.
Data analysis was performed by a contract research organization (ICON PLC; Dublin, Ireland, managed by Abbott Diabetes Care) and by Abbott Diabetes Care. We used SAS version 9.2 or higher for all analyses.
The trial is registered with ClinicalTrials.gov (NCT02082184).
Role of the Funding Source
The sponsor designed the study protocol in collaboration with the principal investigator in each country and provided all study materials. The sponsor was involved in collecting data and reporting results, but was not involved in the authors’ interpretation or text writing. The sponsor also gave approval to submit for publication. The corresponding author had full access to all the data in the study and, together with all authors, had final responsibility for the decision to submit for publication.
Results
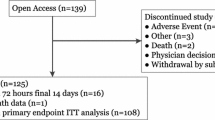
We recruited 302 participants between March 13 and October 15, 2014; 224 were randomized (149 intervention, 75 controls) after completing the baseline phase (Fig. 1). Prior to randomization 78 participants discontinued, the primary reason for this was failure to meet screening HbA1c criterion. Participants’ baseline characteristics are summarized in Table 1, the full analysis set included 224 randomized participants, and there were no significant differences between groups.
There was no difference in HbA1c change at 6 months between intervention and control groups [−3.1 ± 0.75 mmol/mol (adjusted mean ± SE), (−0.29 ± 0.07%) and −3.4 ± 1.04, (−0.31 ± 0.09%), respectively; p = 0.8222]. A similar drop in HbA1c was detected in both groups comparing study end to baseline values.
In participants younger than 65 years, a prespecified subgroup, the drop in HbA1c was more pronounced in the intervention group compared with controls [−5.7 ± 0.96 mmol/mol, (adjusted mean ± SE) (−0.53 ± 0.09%) and −2.2 ± 1.31 mmol/mol (−0.20 ± 0.12%), respectively; p = 0.0301 (Supplementary Material p. 2)]. A significant interaction between treatment group and age was observed for change in HbA1c (p = 0.0017).
In participants aged 65 years or more, the drop in HbA1c was more pronounced for the controls compared to the intervention group [−5.4 ± 1.45 mmol/mol (−0.49 ± 0.13%)] and [−0.6 ± 1.09 mmol/mol (−0.05 ± 0.10%), respectively, p = 0.0081 (Supplementary Material p. 3)].
Significant reductions in all sensor measures of time spent in hypoglycemia, number of events, and area under the curve were observed for intervention participants compared with control (Table 2, Fig. 2, and Supplementary Material pp. 4–7).
Time in hypoglycemia [<3.9 mmol/L (70 mg/dL)] reduced by 43% (−0.47 ± 0.13 h/day; mean ± SE) for intervention participants compared with control (p = 0.0006).
Time in hypoglycemia [<3.1 mmol/L (55 mg/dL)] reduced by 53% (−0.22 ± 0.068 h/day) for intervention participants compared with control (p = 0.0014).
Time in hypoglycemia [<2.5 mmol/L (45 mg/dL)] reduced by 64% (−0.14 ± 0.04 h/day) for intervention participants compared with control (p = 0.0013).
Nocturnal hypoglycemia [<3.9 mmol/L (70mg/dL), 23.00–06.00 h] reduced by 54% (−0.29 ± 0.08 h per 7 h) for intervention participants compared with control (p = 0.0001).
Daytime hypoglycemia [<3.9 mmol/L (<70 mg/dL), 06.00–23.00 h] reduced by 31% (−0.16 ± 0.08 h per 17 h) for intervention participants compared with control (p = 0.0374).
The frequency of events with glucose <3.9 mmol/L (70 mg/dL) reduced by 28% (−0.16 ± 0.065 per day mean ± SE) for intervention participants compared with controls (p = 0.0164). Events <3.1 mmol/L (55 mg/dL) reduced by 44% (−0.12 ± 0.037) for intervention participants compared with controls (p = 0.0017). Frequency of events <2.5 mmol/L (45 mg/dL) reduced by 49% (−0.06 ± 0.02) for intervention participants compared with controls (p = 0.0098).
A between-group difference for area under the curve of 51% (−7.80 ± 2.20 h/day × mg/dL mean ± SE) for sensor glucose level <3.9 mmol/L (70 mg/dL) was observed for intervention versus control participants (p = 0.0005). For sensor glucose levels <3.1 mmol/L (55 mg/dL), area under the curve reduced by 60% (−2.51 ± 0.76 h/day × mg/dL) for intervention participants compared with controls (p = 0.0012). Area under the curve was also significantly reduced by 67% (−0.70 ± 0.22 h/day × mg/dL) at glucose levels <2.5 mmol/L (45 mg/dL) for intervention compared with control participants (p = 0.0015).
For the prespecified subgroup aged less than 65 years, time in hypoglycemia [<3.9 mmol/L (70 mg/dL)] reduced by 35% for intervention participants compared to control (−0.37 ± 0.168 h/day, p = 0.0279) with 40% reduction in area under the curve (p = 0.0305) and no difference in the number of events. A trend towards reduced time and events for hypoglycemia at other thresholds was observed (Supplementary Material p. 2).
For participants 65 years or more, time in hypoglycemia (<3.9 mmol/L [70 mg/dL]) reduced by 56% for intervention participants compared to control (−0.60 ± 0.220, p = 0.0083) with 71% reduction in area under the curve (p = 0.0061). No difference was detected in number of events (p = 0.0513). Reduced time, events, and area under the curve for hypoglycemia at other thresholds was observed (Supplementary Material p. 3).
There was no difference in time in range (3.9–10.0 mmol/L (70–180 mg/dL)] between intervention and control participants [p = 0.7925, (Table 2)].
There was no difference in time in hyperglycemia [>10.0 mmol/L (180 mg/dL) and >13.3 mmol/L (240 mg/dL)] between the two groups (Table 2).
A number of glucose variability measures were explored and an improvement for intervention participants was observed (Table 2 and Supplementary Material pp. 8–9).
Glucose variability measured as coefficient of variation (CV) reduced by 2.26 ± 0.71% mean ± SE for intervention participants compared with controls (p = 0.0017). LBGI reduced by 0.3 ± 0.11 mean ± SE for intervention participants compared with controls (p = 0.0029). CONGA was reduced for intervention compared with controls by 3 ± 1.3 mg/dL mean ± SE at 2 h time interval (p = 0.0385), by 5 ± 2.2 at 4 h (p = 0.0133), and by 8 ± 3.0 at 6 h (p = 0.0046).
Self-monitoring blood glucose frequency for intervention participants fell from 3.8 ± 1.4 tests/day mean ± SD (3.8 tests/day median) at baseline to 0.5 ± 1.1 (0.1 median) from the first unblinded sensor wear with full access to sensor glucose data (day 15–31), reducing further to 0.4 ± 1.0 tests/day (0.0 median) by study end (day 208). The overall blood glucose monitoring rate over 6 months was 0.3 ± 0.7, median 0.1 (Fig. 3).
During the treatment phase (day 15 onwards) average sensor-scanning frequency was 8.3 ± 4.4 (mean ± SD) times/day (median 6.8), i.e., double the frequency of blood glucose testing (Fig. 3). There was no significant difference in the number of scans performed by those <65 years and ≥65 years of age [8.1 ± 4.6 (median 6.8) and 8.5 ± 4.1 (median 6.9), respectively, p = 0.6627].
There was no correlation between frequency of sensor scanning and reduced time in hypoglycemia or change to HbA1c. Device use for the intervention group (n = 138) was 88.7 ± 9.2% (defined as the percentage of data collected, assuming continuous device wear for 6 months).
Self-monitoring of blood glucose frequency for control participants was 3.9 ± 1.5 test/day (median 3.9) at baseline and this rate was maintained until study end [3.8 ± 1.9 (median 3.9), Fig. 3]. Control group participants <65 years performed less blood glucose monitoring tests (2.78 ± 1.08 test/day) than those ≥65 years (3.46 ± 0.94), p = 0.0247.
At baseline, 95% of participants used an insulin pen device or syringe for intensive insulin therapy, with the remainder (5%) on CSII (Table 1); 78% used analogue insulin, seven participants from each group (n = 14) utilized human insulin, and 35 participants used both human and analogue insulin (intervention n = 22, control n = 13).
There was no difference detected in total daily dose of insulin, basal, or bolus insulin doses between the two groups. None of the changes in insulin were correlated with the treatment effect on HbA1c or time in hypoglycemia (<3.9 mmol/L [70 mg/dL]).
There was no difference in total daily dose of insulin by study end for intervention participants (from 87.6 ± 44.0 (mean ± SD) to 85.2 ± 39.7 units) compared with controls (from 90.1 ± 40.6 to 87.8 ± 41.5), −0.4 ± 3.75 units mean ± SE (p = 0.9059). Basal insulin was similar for intervention and control participants (−2.3 ± 1.96 units mean ± SE, p = 0.2498). Bolus insulin was similar for intervention and control participants (1.4 ± 2.53 units mean ± SE, p = 0.5856). Similarly, for participants above or below 65 years, there was no difference detected in the total daily dose of insulin (0.7 ± 4.86, p = 0.8871; and −3.3 ± 5.40, p = 0.5403, respectively).
There were no changes in body weight (p = 0.2496) or BMI (p = 0.2668) from baseline for either group.
Total treatment satisfaction score for DTSQ (status versus change) was significantly improved for intervention group participants (13.1 ± 0.50, mean ± SE) compared with controls (9.0 ± 0.72), p < 0.0001. Satisfaction with treatment results using DQoL demonstrated significant improvement for the intervention group (−0.2 ± 0.04, mean ± SE) versus the control group (0.0 ± 0.06), p = 0.0259, for this element of the questionnaire. There were no other significant differences observed in other aspects of DTSQ and DQoL or for the DDS scales (Fig. 4, Supplementary Material p. 10).
Scores from DTSQ (a) and DQoL (b) questionnaires. Error bars show 95% CIs. DTSQ treatment satisfaction scores range from −18 to 18; high scores indicate much more satisfied, convenient, flexible, or likely to recommend treatment now. DTSQ perceived frequency scores range from −3 to 3; high scores indicate much more time now. DQoL scores range from 1 to 5; high scores indicate dissatisfaction, frequent impact, or frequent worry. DQoL Diabetes Quality of Life Questionnaire, DTSQ Diabetes Treatment Satisfaction Questionnaire
User questionnaire results showed intervention participants agreed with positive aspects of the device including use, comfort, and utilization of sensor glucose information (Supplementary Material p. 11).
The system was used for 6 months by intervention participants and worn (blinded) for 4 weeks by control participants (n = 224). In total, serious adverse or adverse events (n = 515) were experienced by 114 (76.5%) intervention and 47 (62.7%) control participants.
There were no serious adverse events related to the device or study procedure. Forty-two serious events were experienced by 16 (10.7%) intervention and 12 (16.0%) control participants.
Four hypoglycemia serious adverse events were experienced by four participants (three intervention and one control) and 57 hypoglycemia adverse events by 10 (7%) intervention and seven (9%) control participants.
None of the severe hypoglycemic episodes [13] or hypoglycemic adverse events were associated with the device.
Three participants (one intervention, two controls) experienced an adverse event leading to withdrawal from the study; none were associated with the device.
Six (4.0%) intervention participants reported nine device-related adverse events (two severe, six moderate, and one mild). These were sensor-adhesive reactions, primarily treated with topical preparations. All were resolved at study exit.
There were no reported events of diabetic ketoacidosis or hyperosmolar hyperglycemic state. Seven cardiac events were reported for four (2.7%) intervention and three (4.0%) control participants (none were considered to be related to study procedures or the device).
Anticipated symptoms refer to those typically expected using a sensor device and equate to symptoms normally experienced with blood glucose finger-stick testing, e.g., pain, bleeding, bruising. There were 158 anticipated sensor insertion site symptoms observed for 41 (27.5%) intervention and 9 (12.0%) control participants. These symptoms were primarily (63%) due to the sensor adhesive (erythema, itching, and rash) and resolved without medical intervention. Adverse events and anticipated symptoms associated with the insertion of the sensor and sensor wear are summarized in Table 3 and Supplementary Material p. 12.
Discussion
This European study is the first to investigate the use of flash sensor-based glucose technology as a replacement for standard self-monitoring of blood glucose in individuals with type 2 diabetes treated with intensive insulin therapy. Whilst the primary endpoint was not achieved (no difference in HbA1c change between the groups at 6 months), the secondary endpoints demonstrate a number of interesting findings for further consideration including use of the technology is associated with reduced time in hypoglycemia, particularly nocturnal; treatment satisfaction improved across two questionnaire methodologies; HbA1c improvement combined with reduced hypoglycemia measures were observed in the <65 years subgroup; and the safety data confirms that flash glucose monitoring technology is an effective and safe replacement for blood glucose monitoring.
There is a paucity of data on continuous glucose monitoring (CGM) use in type 2 diabetes and, to our knowledge, no recent randomised, controlled studies in this population using intensive insulin therapy. Available data for CGM use in those using oral glucose-lowering medication or basal insulin with higher baseline HbA1c values indicate they are more likely to show benefit with a reduction in this clinical marker [24–26]. However, hypoglycaemia was not an endpoint in these studies, and exposure to hypoglycaemic risk is much less in treatment regimens excluding prandial insulin. Reductions in hypoglycaemic markers generally require de-escalation of glucose-lowering therapy [27] with less stringent glucose targets [28]. In the intervention group, HbA1c level improved with significantly reduced exposure to hypoglycaemia.
Reductions in hypoglycemia in the intervention group were present across all age groups, particularly significant in those aged above 65 years, and over 24 h of the day, with benefit particularly pronounced during nighttime. Reduced nocturnal hypoglycemia likely resulted through learning from historical nighttime sensor glucose data leading to adjustments in pre-bedtime snacks or overnight basal insulin doses. Improved daytime hypoglycemia was likely achieved through a combination of on-demand access to real-time sensor glucose results with trend arrows, enabling preventative action and informing behavior modification, alongside HCP review of glucose reports with the participant, to alter the balance of insulins. Smaller, daily adjustments to insulin doses or proportions may not be apparent in the total insulin dose [29]. Given the association of hypoglycemia with adverse clinical outcome, including enhanced risk of cardiovascular events, increased hospital admissions, and reduced survival [5, 7], these results for multiple hypoglycemia-related secondary endpoints highlight the effectiveness and safety of this technology and its potential for improving glycemic control. Detection of hypoglycemia, especially nocturnal, can be difficult with intermittent glucose monitoring even when it is performed frequently.
Once intervention participants were able to see sensor glucose readings, their blood glucose testing frequency fell to around 1 test every 3 days, with 57% of participants testing less than once every 10 days. High device utility rate (89%) [22] with average sensor scanning eight times daily replaced blood glucose testing and shows confident use of the technology to access current and historic sensor glucose data. In contrast, although the control group remained concordant with regular blood glucose testing throughout the study (averaging 3–4 tests daily), they did not benefit from a reduction in hypoglycemia.
In addition to benefiting from less time in hypoglycemia compared with the control group, intervention participants showed improvement in glucose variability [30] and LBGI, a specific risk marker for hypoglycemia [31]. These findings can be partially explained by the documented association between hypoglycemia and glucose variability [30, 31]. The reduction in hypoglycemic exposure in the intervention group may offer additional clinical benefits [8, 9].
A significant improvement in HbA1c was detected in those younger than 65 years. Although the reasons for this finding are not entirely clear we hypothesize that the convenience associated with sensor glucose readings, compared with blood glucose testing, prompted more frequent testing. This supports a recent study reporting younger participants as being “too busy” for finger-stick testing [32]. HbA1c level was unchanged for intervention participants ≥65 years. Again the reasons for this are not entirely clear, and we hypothesize that the benefit for older intervention participants of being able to visualize actual or potential hypoglycemic risk prompted a more cautious approach to therapy adjustments for this vulnerable group, prioritizing hypoglycemia reduction over a more indiscriminate approach to glucose control. The overall impact of these two approaches to care was no effect on HbA1c.
These findings may have future clinical implications as past studies show worse glycemic control in younger participants with type 2 diabetes [3, 4] and this new sensor-based technology may be helpful for these participants. However, no adjustments were made for multiple testing by subgroup and future work is required to confirm this observation.
Participants in the intervention group had improved quality of life and satisfaction with their treatment compared with control. The visual presentation of the historical glucose profile and ease of testing with flash glucose monitoring, avoidance of blood glucose testing, and reduced concerns about hypoglycemia probably contributed to improved quality of life and satisfaction with treatment. A recent study investigating insulin-treated participants on continuous glucose monitoring has shown, similar to our study, improved quality of life measures, attributed to various factors including reduced fear of hypoglycemia, greater confidence, and perceived control over diabetes [33].
Our study results support those of a recent randomized control trial comparing use of this technology with blood glucose testing in adults with well-controlled type 1 diabetes, which also demonstrated superior reduction in hypoglycemia without deterioration of HbA1c and improved treatment satisfaction [34]. Limitations of this work include the absence of a treatment algorithm for modifying insulin therapy. Our aim was to test the new technology in “real-world settings” according to local practices in different centers. Having restrictive protocols for treatment changes would have made general applicability of our data uncertain. Our inclusion of only adults with intensive insulin therapy performing regular glucose testing means future studies to assess the effectiveness of this novel glucose-sensing technology in younger, less concordant, individuals with type 2 diabetes are needed. Had there been an insulin treatment algorithm and inclusion of participants with less regular blood glucose testing, the similar decline in HbA1c observed in both groups during the short period of this study may have been different. Common to glucose technology studies, our intervention was non-masked to subjects as sensor wear was experienced by all with assessment and some treatment decisions based on the same sensor glucose values [35]. No adjustment was made for multiple testing of secondary endpoints. Many of the endpoints, particularly those derived from sensor glucose values, are highly inter-related and should not be considered in isolation.
Conclusion
In summary, use of sensor glucose readings resulted in similar drop in HbA1c compared with standard methods of blood glucose testing. When compared with self-monitored blood glucose testing there were no safety concerns and use of this new technology was associated with highly significant reductions in hypoglycemic measures across all age groups, decreased glucose variability, and improved quality of life and treatment measures. Collectively these results demonstrate that flash glucose-sensing technology is safe and effective when used in place of standard self-monitoring of blood glucose for glycemic management of type 2 diabetes treated by intensive insulin therapy.
References
Chiu C-J, Wray LA. Factors predicting glycemic control in middle-aged and older adults with type 2 diabetes. Prev Chronic Dis. 2010;7(1):A08.
Nichols GA, Hillier TA, Javor K, Brown JB. Predictors of glycemic control in insulin-using adults with type 2 diabetes. Diabetes Care. 2000;23(3):273–7.
Holman RR, Paul SK, Bethel MA, et al. 10-year follow up of intensive glucose control in type 2 diabetes. N Eng J Med. 2008;359:577–89.
UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). UK Prospective Diabetes Study (UKPDS) Group. Lancet. 1998;352:837–53.
Bonds DE, Miller ME, Bergenstal RM, et al. The association between symptomatic, severe hypoglycaemia and mortality in type 2 diabetes: retrospective epidemiological analysis of the ACCORD study. BMJ. 2010;340:b4909.
Alvarez-Guisasola F, Yin DD, Nocea G, Qui Y, Mavros P. Association of hypoglycemic symptoms with patients’ rating of their health-related quality of life state: a cross sectional study. Health Qual Life Outcomes. 2010;8:86.
Amiel SA, Dixon T, Mann R, Jameson K. Hypoglycemia in type 2 diabetes. Diabet Med. 2008;25:245–54.
Lin CC, Li CI, Yang SY, et al. Variation of fasting plasma glucose: a predictor of mortality in patients with type 2 diabetes. Am J Med. 2012;125(416):e9–18.
Schisano B, Tripathi G, McGee K, McTernan PG, Ceriello A. Glucose oscillations, more than constant high glucose, induce activation and a metabolic memory in human endothelial cells. Diabetologia. 2011;54:1219–26.
Ong WM, Chua SS, Ng CJ. Barriers and facilitators to self-monitoring of blood glucose in people with type 2 diabetes using insulin: a qualitative study. Patient Prefer Adherence. 2014;8:237–46.
Hortensius J, Kars MC, Wierenga WS, Kleefstra N, Bilo HJ, van der Bijl JJ. Perspectives of patients with type1 or insulin treated type 2 diabetes on self-monitoring of blood glucose: a qualitative study. BMC Public Health. 2012;12:167–77.
Abbott Diabetes Care. FreeStyle Libre Software. http://www.FreeStyleLibre.com. Accessed 11 April 2016.
ADA. Defining and reporting hypoglycemia in diabetes: a report from the American Diabetes Association Workgroup on Hypoglycemia. Diabet Care. 2005;28:1245–9.
Polonsky WH, Fisher L, Earles J, et al. Assessing psychosocial distress in diabetes: development of the diabetes distress scale. Diabet Care. 2005;28:626–31.
The DCCT. Research group reliability and validity of a diabetes quality-of-life measure for the diabetes and complications trial (DCCT). Diabet Care. 1988;11:725–32.
Bradley C. Diabetes treatment satisfaction questionnaire. In: Bradley C, editor. Handbook of psychology and diabetes. Chur: Harwood Academic; 1994.
Kovatchev BP, Clarke WL, Breton M, Brayman K, McCall A. Quantifying temporal glucose variability in diabetes via continuous glucose monitoring: mathematical methods and clinical application. Diabetes Technol Ther. 2005;7:849–62.
McDonnell CM, Donath SM, Vidmar SI, Werther GA, Cameron FJ. A novel approach to continuous glucose analysis utilizing glycemic variation. Diabetes Technol Ther. 2005;7(2):253–63.
Clarke W, Kovatchev B. Statistical tools to analyze continuous glucose monitor data. Diabetes Technol Ther. 2009;11(S1):S45–54.
Abbott Diabetes Care. Randomised controlled study to evaluate the impact of novel glucose sensing technology on HbA1c in type 2 diabetes (REPLACE) ADC-CI-APO 12018. Data on file. 2015.
Food and Drug Administration. Guidance for industry diabetes mellitus: developing drugs and therapeutic biologics for treatment and prevention 2008; page 23 http://www.fda.gov/downloads/Drugs/…/Guidances/ucm071624.pdfm. Accessed 15 Dec 2016.
The Juvenile Diabetes Research Foundation Continuous Glucose Monitoring Study Group. Continuous glucose monitoring and intensive treatment of type 1 diabetes. N Engl J Med. 2008;359:1464–76.
Vickers AJ, Altman DG. Statistics notes: analysing controlled trials with baseline and follow up measurements. BMJ 2001;10(323, 7321):1123–4.
Ehrhardt NM, Chellappa M, Walker SM, Fonda SJ, Vigersky RA. The effect of real-time continuous glucose monitoring on glycaemic control in patients with type 2 diabetes. J Diabet Sci Technol. 2011;5(3):668–75.
Vigersky RA, Fonda SJ, Chellappa M, Walker SM, Ehrhardt NM. Sort and long term effect of real-time continuous glucose monitoring in patients with type 2 diabetes. Diabet Care. 2012;35:32–8.
Fonda SJ, Salkind SJ, Walker SM, Chellappa M, Ehrhardt N, Vigersky RA. Heterogeneity of responses to real-time continuous glucose monitoring (RT_CGM) in patients with type 2 diabetes and its implications for application. Diabet Care. 2013;36:786–92.
McCoy RG, Kasia MS, Lipska J, et al. Intensive treatment and severe hypoglycemia among adults with type 2 diabetes. JAMA Intern Med. 2016;176(7):969–78.
American Diabetes Association Standards of Medical Care in. Diabetes. Diabete, Care. 2016;39:1.
Battelino T, Conget I, Olsen B, et al, for the SWITCH Study Group. The use and efficacy of continuous glucose monitoring in type 1 diabetes treated with insulin pump therapy: a randomised controlled trial. Diabetologia 2012;55:3155–62.
Kovatchev BP, Cox DJ, Farhy LS, Straume M, Gonder-Frederick L, Clarke WL. Episodes of severe hypoglycemia in type 1 diabetes are preceded and followed within 48 hours by measurable disturbances in blood glucose. J Clin Endocrinol Metab. 2000;85:4287–92.
Qu Y, Jacober SJ, Zhang Q, Wolka LL, Hans DeVries J. Rate of hypoglycemia in insulin-treated patients with type 2 diabetes can be predicted from glycemic variability data. Diabetes Technol Ther. 2012;14(11):1008–12.
Ward JEF, Stetson BA, Mokshagundam SPL. Patient perspectives on self-monitoring of blood glucose: perceived recommendations, behaviours and barriers in a clinic sample of adults with type 2 diabetes. J Diabetes Metab Disord. 2015;14(43):1–7.
Polonsky WH, Hassler D. What are the quality of life-related benefits and losses associated with real-time continuous glucose monitoring? A survey of current users. Diabetes Technol Ther. 2013;15:295–301.
Bolinder J, Antuna R, Geelhoed-Duijvestijn P, Kroeger J, Weitgasser R. Novel glucose-sensing technology and hypoglycaemia in type 1 diabetes: a multicentre, non-masked, randomised controlled trial. Lancet. 2016. doi:10.1016/S0140-6736(16)31535-5.
Maahs DM, Buckingham B, Castle J, et al. Outcome measures for artificial pancreas clinical trials: a consensus report. Diabet Care. 2016;39:1175–9.
Acknowledgements
Sponsorship for this study, provision of study devices, all study materials, and article processing charges were funded by Abbott Diabetes Care, Witney, UK. All authors had full access to all of the data in this study and take complete responsibility for the integrity of the data and accuracy of the data analysis.
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published. TH wrote the first draft of the manuscript and together with all the co-authors worked collaboratively to write, discuss, and review this manuscript which was revised and edited by RA. All named authors collectively took the decision to submit it for publication.
The authors thank the participants for their involvement in the study, are grateful to those who contributed to the collection of data at the REPLACE study sites (Supplementary Material p. 13) and to Zoe Welsh (Abbott Diabetes Care) for statistical support.
Disclosures
Thomas Haak reports personal fees from Abbott Diabetes Care outside the submitted work. Gerry Rayman reports personal fees from Abbott Diabetes Care outside the submitted work. Hélène Hanaire reports personal fees from Abbott Diabetes Care and Medtronic, and grants from Johnson and Johnson outside the submitted work. Ramzi Ajjan reports other funding from Abbott Diabetes Care during the conduct of the study and personal fees from Abbott Diabetes Care outside the submitted work. Norbert Hermanns reports grants and personal fees from Abbott Diabetes Care Germany, grants from Dexcom, grants and personal fees from Berlin-Chemie, grants from Ypsomed, personal fees and non-financial support from Novo Nordisk, and grants from Lilly International, outside the submitted work. Jean-Pierre Riveline reports grants outside the submitted work.
Compliance with Ethics Guidelines
Approval was given by the appropriate competent authorities in each country. All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964, as revised in 2013. Informed consent was obtained from all patients for being included in the study.
Data Availability
The datasets during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to http://www.medengine.com/Redeem/8A47F0602144B45F.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Haak, T., Hanaire, H., Ajjan, R. et al. Flash Glucose-Sensing Technology as a Replacement for Blood Glucose Monitoring for the Management of Insulin-Treated Type 2 Diabetes: a Multicenter, Open-Label Randomized Controlled Trial. Diabetes Ther 8, 55–73 (2017). https://doi.org/10.1007/s13300-016-0223-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13300-016-0223-6