Abstract
Objectives
Healthcare staff can be prone to high levels of stress and research investigating mindfulness-based courses for this population is showing promise. Given the demands of healthcare work, shortened mindfulness courses may be more appropriate. The aim of the study was to evaluate the utility of a workplace-adapted mindfulness course (MBOE) in a hospital setting, including research on workplace-specific outcomes beyond stress reduction and data relating to home practice with a mobile app.
Method
The effects of assignment to a workplace-adapted, 6-week mindfulness course or a waitlist control condition on dispositional mindfulness, perceived stress and fulfilment of basic psychological needs at work were examined in a sample of 65 hospital staff.
Results
Compared with waitlist, staff taking the course showed significant increases in mindfulness and psychological need fulfilment and reductions in perceived stress. Mean levels of perceived stress reduced from a high level to within published norms. Reductions in stress and increases in mindfulness, autonomy and competence remained stable at follow-up. Increased mindfulness mediated improvements in need fulfilment and reductions in stress. Attendance and use of a mobile app for home practice were associated with positive outcomes. Social factors (relatedness) associated with the delivery and outcome of the course were also explored.
Conclusions
The results indicate that a workplace-adapted, short-format mindfulness course can achieve positive results in line with mindfulness courses for other contexts. Questions were raised regarding which distinct elements may improve outcomes, e.g. home practice and dispositional mindfulness vs. learning environment on more general improvements.
Similar content being viewed by others
High-quality patient care and a well-functioning service are key concerns across the National Health Service (NHS). NHS staff may be particularly prone to stress given their role often requiring long work hours and the provision of medical and emotional care and support to patients and their families (Botha et al. 2015). Staff well-being can be an antecedent to patient experience of care (Maben et al. 2012) and high work stress can have a negative impact on healthcare costs, illness and work-related attrition (Wolever et al. 2012).
Mindfulness-based courses, including Mindfulness-Based Cognitive Therapy (MBCT; Segal et al. 2002), have produced sustained reductions in perceived stress (1–3 months; Carmody and Baer 2008; Carmody et al. 2009; Epel et al. 2009; Fjorback et al. 2011). Further, it has been found that higher levels of dispositional mindfulness lead to improved well-being including depressive symptoms (Kiken et al. 2017) and that larger amounts of home meditation practice tend to increase dispositional mindfulness and decrease unhealthy behaviours and low mood including perceived stress, well-being, depression and anxiety (Carmody and Baer 2008; Crane et al. 2014; Greeson 2009).
Research on mindfulness-based courses in workplace contexts is growing including successful findings for stress, anxiety, depression, distress and emotional exhaustion in healthcare professionals (Burton et al. 2017; Galantino et al. 2005; Martín-Asuero and García-Banda 2010; Morgan et al. 2015; Shapiro et al. 1998). One qualitative review also showed perceived benefits to compassion to the self and others and enhanced presence when relating to others (Morgan et al. 2015). A combination of course facets have been proposed as the components leading to successful results: mindfulness meditation, education and social support through group-based learning (Shapiro et al. 1998). Dispositional mindfulness in itself also appears important with one study finding that higher levels moderated relaxation and hassles experienced by nurses during time off (Marzuq and Drach-Zahavy 2012).
Research suggests that mindfulness-based courses are particularly helpful for reducing stress in healthcare workers, regardless of technique, dosage and class length (Burton et al. 2017). One study exploring the barriers and facilitators to participation in a mindfulness course offered to healthcare professionals found that courses were viewed as generally acceptable and positive feedback tended to depend on motivation and positive predisposition (Banerjee et al. 2017). Participants struggled with longer practices however and the authors suggest tailoring a mindfulness course to meet time demands. A healthcare setting may necessitate shorter formats because of the issue of potential absence due to workplace pressures, a negative consequence that healthcare workers may be more prone to due to the high-volume workload and critical scheduling of patient care (Shapiro et al. 2005). The delivery of shorter format courses not only offers potential advantages to the individual attendee but also to the organisation as it puts less strain on resources (Foureur et al. 2013; Jamieson and Tuckey 2017).
Reduced dose alternatives to the 8-week format of Mindfulness-Based Stress Reduction (MBSR; Kabat-Zinn 1990) and MBCT have received attention but studies involving healthcare workers are few (Foureur et al. 2013; Irving et al. 2009; Jamieson and Tuckey 2017). Two studies have shown improvements in depression, stress, anxiety and burnout when examining a modified, shortened MBSR course supplied to healthcare workers (Fortney et al. 2013; Manotas et al. 2014). While these results show promise, a review of empirical workplace mindfulness studies (Jamieson and Tuckey 2017) raised concerns that a lack of integrity of some courses could lead to them being ineffective. The authors highlight the importance of adapting courses with “careful consideration and sensitivity to the needs of both employees and organizations” and note that researchers should attempt to use organisationally relevant outcome measures.
One such measure may be self-determination, for which a theoretical link with mindfulness has been proposed, contingent on the “fuller” sense of awareness about oneself that mindfulness can bring (Ryan and Brown 2003). In self-determination theory, it is posited that such awareness allows the individual to focus on behaving in a way that more accurately satisfies their underlying needs, values and goals (Deci and Ryan 1980). Crucially, the literature points to automatic behaviour limiting our ability to consider actions that are congruent with our needs and values (Ryan et al. 1997). Thus, by inhibiting automatic behaviour through the noticing of it, the awareness that is learned with mindfulness meditation “facilitates attention to prompts arising from basic needs, making one more likely to regulate behavior in a way that fulfills such needs”, while also creating the conditions to be able to “rediscover and choose values that may be truer for us” (Brown and Ryan 2003; Shapiro et al. 2006).
Self-determination has been measured according to satisfaction of basic psychological needs, comprised of autonomy (possessing a sense of agency, volition or authorship over one’s actions), competence (feeling able to act) and relatedness (feeling a sense of belonging and connection to others) (Deci and Ryan 2000). Insofar as the value of such an approach to self-regulation in the workplace, there is evidence that self-determined goals elicit more effort and persistence, even in the face of challenges (Bono and Judge 2003; Sheldon and Elliot 1999). Self-determination is outlined in one review on workplace mindfulness as a promising avenue for inquiry as a secondary process through which increased mindfulness skills may improve performance and resilience and promote organisational commitment (Glomb et al. 2011). Supporting theoretical work, perceived fulfilment of basic psychological needs has been linked to measures of mindfulness (Brown and Ryan 2003), shown to mediate the relationship between mindfulness and well-being (Chang et al. 2015) and predict positive work outcomes (Ilardi et al. 1993), hormonal and emotional responses to performance-related stress (Quested et al. 2011) and general well-being (Patrick et al. 2007).
The aim of the study was to evaluate a workplace-adapted, short-format mindfulness course, Mindfulness-Based Organisational Education (MBOE; Leonard 2016). The hypotheses were as follows: following the course, fulfilment of basic psychological needs and dispositional mindfulness would increase and perceived stress would decrease, compared with those who did not attend; a higher level of attendance would be associated with better outcomes at post-course; a larger amount of practice outside of class (home practice) would be associated with better outcomes at post-course; the change in mindfulness would mediate changes in perceived stress and work-based psychological needs.
Method
Participants
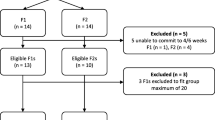
Several courses of MBOE were delivered by the company “Mindfulness Connected” over two 6-week periods to employees of the Royal Orthopaedic Hospital (ROH) in Birmingham. The study was open to anyone who wanted to participate, whether or not they held a clinical role at the hospital. Participants were able to sign up to one of the two course periods so that they either completed an initial course or a proceeding one depending on their availability, later participants thus becoming a waitlist control comparison group. Using G*Power software (Erdfelder et al. 1996), the required sample size for a repeated measure design with 95% power using a conservative effect size of 0.25 (f) (Cohen 1992) was 54 (27 per group) and for a large effect size of 0.40 (f), 24 (12 per group). Accounting for attrition, the aim was to recruit a sample of 70 participants.
Procedure
The study was supported by the trust board, the hospital chair and the research department. Participants were informed about the course by Human Resources (HR) staff and their managers via word-of-mouth and email. There was no pressure to participate; participants were informed that the course was free to attend and may help to improve stress levels. To manage class sizes, each cohort was split into three so that the same session was run three times in 1 day with different class groups over a six-week period.
Although the study design included a waitlist control group, selection was not randomised but rather was designed to include staff from different services within the same classes. The reasons for this were twofold: critical numbers of staff were not removed from any one service at any one time and, by placing staff with different organisational perspectives together in the same classes, there was an intention to stimulate understanding in the group activities that formed a key part of the curriculum. Selection and scheduling required coordination between researchers, the course trainer and senior staff across the institution.
The study was optional; employees could attend the course without completing questionnaires. When participants signed up to one of the mindfulness courses, they then opted into the research element if they chose to. Secure links to online information and questionnaires were sent via email. Participants were asked to read the study information, give consent and then supply answers to questionnaires measuring perceived stress, dispositional mindfulness and perceived fulfilment of basic psychological needs at work.
Course Overview
See Table 1 for a detailed MBOE course outline. The course differs from therapeutic mindfulness courses in that it is reduced in length from 8 to 6 weeks; classes are reduced from 2 hours to 1 hour; daily guided meditations are reduced from 40 minutes to 10 minutes; content is contextualised for the workplace and is delivered cabaret style so that groups of people sit around the tables facing the teacher (rather than in a circle). Instructions and explanations are provided through discussion and via presentation slides to help participants understand the practices they are being asked to do and why they are being asked to do the different practices. See Leonard 2016 for more information about the background of the course. The course was designed and delivered by a teacher with over 5 years of experience delivering short-format mindfulness-based courses.
The “Mindfulness Connected” app was created by the study team (it was made available for iOS (v 8+) and Android (v 4.1+) platforms [on Google play]) and contained seven distinct meditation exercises, each accompanied by information and instruction. Six exercises were audio recordings (shown in Fig. 1) to be followed by the user daily, depending on each week of the course. These were week one “One-minute Reset” (started in week one but also to be used throughout the course), week two “Body Scan”, week three “Posture and Breath”, week four “Stretching and Sitting”, week five “Mindfulness of Feelings” and week six “Mind Wandering”. A seventh meditation exercise named Sync With Your Breath (SWYB) was included for use at participants’ discretion. SWYB (Fig. 2) takes a gesture-based approach of meditating with the breath, a central feature of many forms of meditation (Nash and Newberg 2013).
The app was provided to course participants as the delivery mechanism for the home practice exercises. The course leader encouraged participants to download the app to their mobile devices and to use it to do regular practice outside of the classroom; however, it was explained that doing so was not a pre-requisite for receiving training.
Measures
Participants completed the measures online before the course and immediately following the course. Participants who took part in the initial course (i.e. the active group) were also asked to complete the questionnaires 1 month after they had completed the course. Control participants were unable to complete follow-up questions as their courses had already begun at this stage. Perceived fulfilment of basic psychological needs was measured using the Basic Psychological Needs at Work Scale, based on Self-Determination Theory (BPNWS; Deci and Ryan 2000). The BPNWS consists of 12 items with a total range of 12–72, comprising the three subscales of autonomy, competence and relatedness to others. The scale measures the degree to which one feels fulfilled of each of the three factors within their work environment. These psychological needs have been found to be important for healthy functioning in various areas of living (e.g. Patrick et al. 2007), including in the workplace (Ryan et al. 2010). The BPNWS has been validated for use in multiple workplace samples (Brien et al. 2012). Cronbach’s α in this study was 0.92. For the subscales comprising the BPNWS, the values of Cronbach’s α were as follows: autonomy, 0.87, competence, 0.83, relatedness, 0.90.
Perceived stress was measured using the Perceived Stress Scale (PSS; Cohen et al. 1983). The PSS consists of ten items with scores ranging from 0 to 40 and is a widely used and validated scale which asks the individual how much they perceived events as uncontrollable and overwhelming during the previous month. Cronbach’s α in this study was 0.88.
Dispositional mindfulness was measured using the Five-Facet Mindfulness Questionnaire short form (FFMQ-SF; Baer et al. 2006). The FFMQ-SF consists of 24 items with a total range of 24–120 and is widely used as a measure of dispositional mindfulness. The FFMQ-SF includes questions relating to five factors of mindfulness: observing, non-reactivity, describing, non-judging and acting with awareness. Dispositional mindfulness measured using the FFMQ has been found to increase following mindfulness courses (e.g. Baer et al. 2012; Carmody and Baer 2008). Cronbach’s α in this study was 0.88. For the subscales comprising the FFMQ-SF, values of Cronbach’s α were as follows: awareness, 0.89, describing, 0.85, observing, 0.86, non-judgement, 0.70, non-reactivity, 0.72.
Home practice was assessed by examining the use of the app during the course or the follow-up period. We included two measures of home practice based on data from the app in our analysis, a dichotomous variable of those who used the app vs. those who did not use the app, and a continuous variable sampling only those who used the app measuring the number of distinct occasions of use (recorded each time they opened the app and performed a home practice exercise). Attendance was measured retrospectively by asking participants at post-course how many classes out of the six they had attended.
Data Analysis
Global scores of mindfulness (FFMQ-SF) and psychological needs at work (BPNWS) were analysed. Mixed factorial repeated measures ANOVAs were conducted to examine whether participation in the mindfulness course incurred any changes in perceived stress, psychological needs and mindfulness from baseline to post-course compared with control group participants. Correlations were conducted to explore whether class attendance and home practice improved the change in outcomes from pre to post, including subscales of the FFMQ-SF and BPNWS, especially as this has not been explored previously. Intention-to-treat analysis was conducted to explore the potential of the course at follow-up, given that control scores were unavailable at this point. To examine whether mindfulness mediated change in outcomes, an estimation of the indirect effect of the mediator on the outcome variable/s was examined using the Process tool (Hayes 2012).
Results
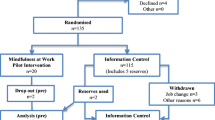
While men and women of differing job titles, including clinical and non-clinical positions, signed up to the courses, the sociodemographic data were unavailable due to study anonymity. See Fig. 2 for a flowchart outlining participant progression through the study. Forty participants who signed up to the initial course and 36 participants who signed up to the second course completed pre-course measures, respectively, thereby becoming the study ‘active’ and ‘waitlist control’ groups (one participant in the active group and one participant in the control group completed the post-course questions having not completed them at pre-course so these data were omitted).
Six control participants did not complete post-course questions so their data were removed for proceeding statistical analysis leaving 35 active participants and 30 controls with complete (pre and post) data sets. Thirty-one active participants completed the questionnaires once more 1 month after their course had finished (controls were unable to complete follow-up measures because they had already begun their course).
Thirty-three of the active participants answered the attendance item at post-course. The mean number of classes attended was 4.76 (range 1–6, SD = 1.20). Only active participants were given access to the app during the study, of whom 18 installed it to their mobile devices and used it on at least one occasion over the course and follow-up periods. The mean number of occasions that participants used the app was 14.00 during the course (n = 18, range 1–46, SD = 14.23) and 3.75 during the follow-up period (n = 8, range 1–7, SD = 2.32).
Basic Psychological Needs at Work
See Table 2 for the mean scores and effect sizes by group. The mean baseline BPNWS score for the total sample was 52.82 out of a possible 72 (SD = 10.42). At post-course, the BPNWS score increased for active participants and remained stable for control participants.
To test the hypothesis that completing the mindfulness course would result in greater post-course scores for perceived fulfilment of psychological needs at work, a mixed factorial repeated measures ANOVA was conducted with the within-subjects variable of time (baseline vs. post-course scores) and between-subjects variable of group allocation (active n = 35 vs. control n = 30). This analysis was conducted for participants completing both baseline and post-course questionnaires. Consistent with the hypothesis, there was a significant interaction of time × group allocation, F(1, 63) = 7.21, p = 0.009, η2 = 0.10, see Fig. 3.
Post-hoc comparisons examining needs at work over time were significant for active participants, F(1, 63) = 9.44, p < 0.005, η2 = 0.13 (mean difference 4.89) but not for control participants, F(1, 63) = 0.67, p > 0.05, η2 = 0.01 (mean difference − 1.40). The difference in scores between groups at baseline, F(1, 63) = 0.45, p > 0.05 and post-course was not significant, F(1, 63) = 2.67, p > 0.05.
Attendance (n = 33) did not correlate, p > 0.05, with post-course change in psychological needs fulfilment, except moderately with post-course change in relatedness scores, r = 0.355, p = 0.043.
Similar to attendance, engaging in home practice (being an app user or not, n = 35, 18 users) correlated moderately with relatedness for post-course change, r = 0.369, p = 0.029. However, being an app user did not correlate with post-course change for autonomy, competence or overall psychological needs, p > 0.05. For participants who used the app during the course (n = 18), no correlations were found between the number of occasions that they used it and outcomes for basic psychological needs.
Perceived Stress
The mean baseline Perceived Stress Scale (PSS) score for the total sample was 18.55 (SD = 6.19, higher than published population norms (between 11.9 and 14.7, Cohen and Williamson 1988). The active and control groups were similar in their stress scores before the course began, t(74) = 0.18, p = 0.86, see Table 2. Post-course, the mean PSS score of the active sample was within the threshold of published norms for perceived stress.
A mixed factorial repeated measures ANOVA was conducted with the within-subjects variable of time (baseline vs. post-course scores) and between-subjects variable of group allocation (active n = 35 vs. control n = 30). Again, this analysis was conducted only using participant data where both baseline and post-course questionnaires were completed. Consistent with the hypothesis, there was a significant interaction of time × group allocation, F(1, 63) = 14.12, p < 0.001, η2 = 0.18 (see Fig. 4). The mean baseline score for actives (n = 35) was 18.49 (SD = 6.29, range 8–31), and their mean post-course score was 14.43 (SD = 5.80, range 3–30). The effect size (d) of the change in active participants is 0.67. The mean baseline score for controls (n = 30) was 19.20 (SD = 6.32, range 4–29), and their mean post-course score was 19.87 (SD = 6.57, range 4–32).
Post-hoc comparisons examining stress over time were significant for active participants, F(1, 63) = 22.56, p < 0.001, η2 = 0.26 (mean difference − 4.06) but not for control participants, F(1, 63) = 0.52, p > 0.05, η2 = 0.01(mean difference − 0.67). The difference in scores between groups at post-course was statistically significant, F(1, 63) = 12.57, p = 0.001, η2 = 0.17.
For post-course change in stress, being an app user was moderately correlated, r = − 0.396, p = 0.018, although attendance was just outside of significant correlation at the 95% confidence interval level, r = − 0.335, p = 0.057. For participants who used the app during the course (n = 18), no correlations were found between the number of occasions that they used it and perceived stress outcomes.
Dispositional Mindfulness
The mean baseline FFMQ-SF score for the sample was 76.13 out of a possible 120 (SD = 11.37). Post-course, the mindfulness score increased for active participants and remained stable for control participants, see Table 2. The statistical effect size (d) of the change was 0.52 for actives indicating a moderate change in mindfulness post-course.
A mixed factorial repeated measures ANOVA was conducted with the within-subjects variable of time (baseline vs. post-course scores) and between-subjects variable of group allocation; again, this analysis was conducted only using data from completers of both baseline and post-course questionnaires (actives n = 35 vs. control n = 30). Consistent with the hypothesis, there was a significant interaction of time × group allocation, F(1, 63) = 6.78, p = 0.012, η2 = 0.097 (see Fig. 5). The mean baseline FFMQ-SF score was 74.94 (SD = 11.74, range 51–100) for actives and 77.53 (SD = 12.03, range 59–108) for controls. The post-course mean FFMQ-SF score was 80.23 (SD = 9.97, range 65–112) for active participants and 77.50 (SD = 13.36, range 55–107) for controls. The effect size (d) was 0.49 for actives indicating a moderate change in mindfulness post-course.
Post-hoc comparisons examining mindfulness over time were significant for active participants, F(1, 63) = 14.50, p < 0.001, η2 = 0.19 (mean difference 5.29), but not for control participants, F(1, 63) = 0, p > 0.05, η2 = 0.00 (mean difference − 0.03). The difference in scores between groups at baseline, F(1, 63) = 0.77, p > 0.05, and post-course was not statistically significant, F(1, 63) = 0.89, p > 0.05.
Attendance (n = 33) was not correlated with pre-post change for mindfulness, p > 0.05. Several correlations were revealed between those who used the app and change in mindfulness. Using the app during the course (n = 35, 18 users) correlated strongly with post-course change in overall mindfulness, r = 0.506, p = 0.002, and with post-course change in subscales of awareness, r = 0.432, p = 0.010, observing, r = 0.342, p = 0.044, non-judging, r = 0.369, p = 0.029, and non-reactivity, r = 0.372, p = 0.028. For participants who used the app during the course (n = 18), the number of occasions that they used it correlated strongly with change in observing, r = 0.639, p = 0.004, and moderately with change in awareness, r = 0.497, p = 0.036.
Active Participants at 1-Month Follow-Up
Thirty-one active participants completed questionnaires at follow-up, 1 month after their course had finished, see Table 2 for the outcome scores. To explore whether the scores had changed significantly since the course finished or had remained stable, t tests were conducted using the post-course and follow-up scores for the active participants who completed both sets of questions (n = 31). Although there was a trend for perceived psychological needs fulfilment reducing overall, t(30) = 1.97, p = 0.059, this appears to be specifically owing to a reduction in the relatedness subscale score, t(30) = 2.58, p < 0.05, moving back towards pre-course baseline. In contrast, increases in both the autonomy subscale, t(30) = 1.07, p > 0.05, and the competence subscale, t(30) = 1.23, p > 0.05, remained stable at follow-up. Stress scores remained stable, t(30) = − 1.03, p > 0.05, as did mindfulness, t(30) = − 1.73, p = 0.09.
Class attendance (n = 29) did not correlate at all with any of the follow-up change measures (calculated by subtracting follow-up scores from baseline scores). Using the app during the follow-up period (n = 31, 8 users) was moderately correlated with change in observing, r = 0.503, p = 0.004, and moderately correlated with change in non-reactivity, r = 0.376, p = 0.037, overall mindfulness, r = 0.473, p = 0.007, stress, r = − 0.465, p = 0.008, autonomy, r = 0.376, p = 0.037, relatedness, r = 0.425, p = 0.017, and overall psychological needs, r = 0.446, p = 0.012. Due to low sample size limitations for follow-up app users, no within-group correlation analyses looking at number of occasions of use were performed.
Relatedness
Given that the increase in relatedness was not maintained at follow-up, a further correlation analysis was performed to explore the relationship between relatedness and other outcome measures. A Pearson correlation on data from active participants (n = 35) showing post-course change in relatedness was strongly correlated with post-course change in describing, r = 0.534, p = 0.00, and moderately correlated with post-course change in overall mindfulness, r = 0.446, p = 0.007, and non-reactivity, r = 0.364, p = 0.031.
Intention-to-Treat Analysis
Owing to the control scores missing at follow-up, the post-course scores were taken forward to analyse the difference between groups over time, had control scores remained stable from post-course to 1-month follow-up (n = 31 active participants and n = 30 control participants). Repeated measures ANOVAs showed that there was a time by group interaction for psychological needs at work, F(2, 58) = 5.10, p < 0.01, η2 = 0.08, a time by group interaction for perceived stress, F(2, 58) = 9.43, p < 0.001, η2 = 0.14, and a time by group interaction for mindfulness, F(2, 58) = 8.52, p < 0.001, η2 = 0.13.
Dispositional Mindfulness as a Mediator
A mediation analysis was conducted (Hayes 2012) to explore whether the post-course change in dispositional mindfulness mediated the post-course changes in fulfilment of workplace psychological needs and perceived stress (n = 65). Examining perceived stress as an outcome, the post-course change in dispositional mindfulness (FFMQ-SF) mediated the post-course change in stress (PSS), dependent on group allocation, [R2 = 0.10]. This represents a large effect, standardised b for indirect effect, see Fig. 6. Despite the presence of a significant indirect effect (b = − 2.20, 95% CIs [− 4.06 to − 0.66]), change in mindfulness appears to only be a partial mediator of the effect of group on change in stress as the direct effect (b = − 2.53, p = 0.013) remains significant and is stronger than the indirect effect.
Examining workplace psychological needs as an outcome, the post-course change in dispositional mindfulness (FFMQ-SF) mediated the post-course change in psychological needs (BPNWS), dependent on group allocation, [R2 = 0.10]. Again, this represents a large effect, standardised b for indirect effect, see Fig. 7. The pre to post-course change in dispositional mindfulness mediated the effect of group on change in workplace psychological needs. The mediation model reveals a significant indirect effect (b = 2.53, 95% CIs [0.57–6.16]) and an insignificant direct effect (b = 3.76, p > 0.1).
Discussion
This study examined the potential of a short-format, workplace-adapted mindfulness course delivered to hospital staff, including a control comparison group with a 1-month follow-up. The aim of this study was to evaluate a workplace-adapted mindfulness course for perceived stress and psychological needs in a sample of UK hospital employees. The hypotheses were supported: basic psychological needs at work and mindfulness scores increased and perceived stress scores decreased compared with participants who did not attend the course. It is encouraging that the change in perceived stress decreases from a high level to a level within published norms (Cohen and Williamson 1988). Our findings support studies showing that participation in a mindfulness course increases dispositional mindfulness, produces a desirable effect on stress and well-being (Greeson 2009; Kiken et al. 2017) and improves rates of stress in healthcare workers (Manotas et al. 2014). Alongside field-comparable results using established mindfulness research tools (PSS and FFMQ), a positive result at course completion for the Basic Psychological Needs at Work Scale (BPNWS) and stable improvements at follow-up for the autonomy and competence subscales were found. This suggests the utility of a mindfulness course in achieving work-related outcomes in addition to stress reduction. The finding is potentially an important step in examining courses aimed at producing sustained benefits for staff, something which may also benefit patient care in healthcare settings (Maben et al. 2012).
Class attendance had a positive relationship with post-course scores for stress, relatedness and non-reactivity. However, attendance bore no relationship with dispositional mindfulness nor basic needs fulfilment. This contradicts previous findings suggesting that course dosage and length do not impact on stress (Burton et al. 2017), but that improvements were found in needs fulfilment regardless of dosage and length is important, especially given the potential time constraints of healthcare workers, and warrants further investigation. As previous qualitative findings recommended (Banerjee et al. 2017), the reduced time requirements and tailoring of MBOE classes to the workplace were likely helpful in being able to deliver it in a busy environment. That the employer was willing to supply this course and to help with a study is one potential reason that the course and study completion rates seem so promising.
Engagement with home practice (via the Mindfulness Connected app) was associated with positive outcomes for perceived stress, fulfilment of basic psychological needs at work and mindfulness. The reduction in stress and increase in dispositional mindfulness at post-course and follow-up were associated with the amount of app usage during and after the course so may be extended if app use is continued. At post-course, relatedness was associated with attendance and app use, again suggesting the potential of app usage for this population. Given that mindfulness-based interventions for healthcare workers can be difficult to maintain because of the time and commitment needed, (e.g. Foureur et al. 2013), it may be a useful route to enhance access and convenience to continued practice in this population. However, only 35% (18/51) participants downloaded the app. It would be interesting to examine this with longer follow-up and to conduct qualitative research to investigate the barriers and facilitators to use given the potential for further benefits.
The relatedness subscale of the BPNWS was of particular interest given previous qualitative work suggesting improvements following mindfulness courses (Morgan et al. 2015) and because of its social orientation, the course format and social factors involved in the work-line of the participants. It was the only aspect of basic needs fulfilment not maintained at follow-up, prompting additional exploration. As previously suggested (Shapiro et al. 1998), it is likely that this sort of course is successful because of different features: mindfulness exercises, education and social support through class-based learning. Relatedness may be an organisationally relevant benefit to attending a course such as MBOE, developed through engaging in a cohort-based environment and associated in turn with other beneficial outcomes. This may be particularly important in this population given the current literature stating that social support is important in reducing burnout (Albar Marín and Garcia-Ramirez 2005; Botha et al. 2015) and that staff well-being is a precursor to patient care (Maben et al. 2012). Proceeding research would benefit from the use of a more complete measure of relatedness and other social factors. Further, it may be interesting to investigate whether positive social effects could be extended and maintained beyond the classroom environment.
Mindfulness mediated the improvement in psychological needs fulfilment, consistent with work linking self-determination and mindfulness (Brown and Ryan 2003; Chang et al. 2015; Glomb et al. 2011). Contradicting our hypothesis, mindfulness only partially mediated the reduction in perceived stress, suggesting that other mediators were acting in concert to produce a reduction in stress. Of course, one limitation of mediation is that we cannot be sure of the directionality and given that recent findings vary (see Burton et al. 2017 for a review), it would be beneficial to repeat this analysis in the future.
Limitations and Future Research
The current study has limitations. First, classes were attended based on self-referral and five participants did not complete post-course questionnaires so the final sample is likely to be more motivated. However, given that this is likely to be reflected in real-world use and a control comparison was investigated, the findings reflect what might be reasonably found should a similar course be rolled-out in a similar population.
Second, due to study anonymity and a reduction in participant load, sociodemographic data were not collected. While, anecdotally, a mixture of male and female participants took part from a range of occupation types, analyses exploring potential differences in gender, age or job type are unavailable. In the future, it would be helpful to collect this data to allow for an exploration of sociodemographic factors which may impact on and inform results.
Third, 1-month follow-up data were unavailable for the waitlist control group due to the date of their courses beginning before the follow-up time. While intent-to-treat analysis was conducted, it would be beneficial to follow up the control group to explore any sustained benefits.
It is unclear to what extent the distinct elements of a course such as MBOE, classroom learning and home practice improve specific outcomes. One interpretation of our results might suggest that the overall learning environment is important for improvement and that home practice is key to the development of dispositional mindfulness. It would be interesting in the future to compare with an active control group, to elucidate specific elements which may be helpful such as whether it is social support from a group or mindfulness elements which are effective. The mode of delivery examined here could be an acceptable and effective way to improve well-being for healthcare workers, appropriate to the demands of a high-pressure workplace such as a hospital. Clearly, our results need expansion, but we suggest they could provide a precursor to further research. A broader understanding in this area might be useful for those looking to design and implement mindfulness-based programmes for high-pressured workplaces.
References
Albar Marín, M., & Garcia-Ramirez, M. (2005). Social support and emotional exhaustion among hospital nursing staff. The European Journal of Psychiatry, 19(2), 96–106.
Baer, R. A., Smith, G. T., Hopkins, J., Krietemeyer, J., & Toney, L. (2006). Using self-report assessment methods to explore facets of mindfulness. Assessment, 13(1), 27–45. https://doi.org/10.1177/1073191105283504.
Baer, R. A., Carmody, J., & Hunsinger, M. (2012). Weekly change in mindfulness and perceived stress in a mindfulness-based stress reduction program. Journal of Clinical Psychology, 68(7), 755–765. https://doi.org/10.1002/jclp.21865.
Banerjee, M., Cavanagh, K., & Strauss, C. (2017). A qualitative study with healthcare staff exploring the facilitators and barriers to engaging in a self-help mindfulness-based intervention. Mindfulness, 8(6), 1653–1664. https://doi.org/10.1007/s12671-017-0740-z.
Bono, J. E., & Judge, T. A. (2003). Self-concordance at work: toward understanding the motivational effects of transformational leaders. Academy of Management Journal, 46(5), 554–571.
Botha, E., Gwin, T., & Purpora, C. (2015). The effectiveness of mindfulness based programs in reducing stress experienced by nurses in adult hospital settings: a systematic review of quantitative evidence protocol. JBI Database of Systematic Reviews and Implementation Reports, 13(10), 21–29.
Brien, M., Forest, J., Mageau, G. A., Boudrias, J. S., Desrumaux, P., Brunet, L., et al. (2012). The basic psychological needs at work scale: measurement invariance between Canada and France. Applied Psychology: Health and Well-Being, 4(2), 167–187.
Brown, K. W., & Ryan, R. M. (2003). The benefits of being present: mindfulness and its role in psychological well-being. Journal of Personality and Social Psychology, 84(4), 822–848. https://doi.org/10.1037/0022-3514.84.4.822.
Burton, A., Burgess, C., Dean, S., Koutsopoulou, G. Z., & Hugh-Jones, S. (2017). How effective are mindfulness-based interventions for reducing stress among healthcare professionals? A systematic review and meta-analysis. Stress and Health, 33(1), 3–13.
Carmody, J., & Baer, R. A. (2008). Relationships between mindfulness practice and levels of mindfulness, medical and psychological symptoms and well-being in a mindfulness-based stress reduction program. Journal of Behavioural Medicine, 31(1), 23–33.
Carmody, J., Baer, R. A., Lykins E, L. B., & Olendzki, N. (2009). An empirical study of the mechanisms of mindfulness in a mindfulness-based stress reduction program. Journal of Clinical Psychology, 65(6), 613–626. https://doi.org/10.1002/jclp.20579.
Chang, J.-H., Huang, C.-L., & Lin, Y.-C. (2015). Mindfulness, basic psychological needs fulfillment, and well-being. Journal of Happiness Studies, 16(5), 1149–1162.
Cohen. (1992). A power primer. Psychological Bulletin, 112(1), 155–159. https://doi.org/10.1037/0033-2909.112.1.155.
Cohen, S., & Williamson, G. (1988). Perceived stress in a probability sample of the United States. In S. Spacapan, & S. Oskamp (Eds.), The social psychology of health (pp. 31–67). Newbury Park: Sage.
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A global measure of perceived stress. Journal of Health and Social Behavior, 24(4), 385–396.
Crane, C., Crane, R. S., Eames, C., Fennell, M. J., Silverton, S., Williams, J. M. G., et al. (2014). The effects of amount of home meditation practice in mindfulness based cognitive therapy on hazard of relapse to depression in the staying well after depression trial. Behaviour Research and Therapy, 63, 17–24.
Deci, E. L., & Ryan, R. M. (1980). Self-determination theory: When mind mediates behavior. The Journal of Mind and Behavior, 1(1), 33–43
Deci, E. L., & Ryan, R. M. (2000). The “what” and “why” of goal pursuits: human needs and the self-determination of behavior. Psychological Inquiry, 11(4), 227–268.
Epel, E., Daubenmier, J., Moskowitz, J. T., Folkman, S., & Blackburn, E. (2009). Can meditation slow rate of cellular aging? Cognitive stress, mindfulness, and telomeres. Annals of the New York Academy of Sciences, 1172(1), 34–53. https://doi.org/10.1111/j.1749-6632.2009.04414.x.
Erdfelder, E., Faul, F., & Buchner, A. (1996). GPOWER: a general power analysis program. Behavior Research Methods, Instruments, & Computers, 28(1), 1–11.
Fjorback, L., Arendt, M., Ørnbøl, E., Fink, P., & Walach, H. (2011). Mindfulness-based stress reduction and mindfulness-based cognitive therapy—a systematic review of randomized controlled trials. Acta Psychiatrica Scandinavica, 124(2), 102–119.
Fortney, L., Luchterhand, C., Zakletskaia, L., Zgierska, A., & Rakel, D. (2013). Abbreviated mindfulness intervention for job satisfaction, quality of life, and compassion in primary care clinicians: a pilot study. The Annals of Family Medicine, 11(5), 412–420.
Foureur, M., Besley, K., Burton, G., Yu, N., & Crisp, J. (2013). Enhancing the resilience of nurses and midwives: pilot of a mindfulness-based program for increased health, sense of coherence and decreased depression, anxiety and stress. Contemporary Nurse, 45(1), 114–125.
Galantino, M. L., Baime, M., Maguire, M., Szapary, P. O., & Farrar, J. T. (2005). Association of psychological and physiological measures of stress in health-care professionals during an 8-week mindfulness meditation program: mindfulness in practice. Stress and Health: Journal of the International Society for the Investigation of Stress, 21(4), 255–261.
Glomb, T. M., Duffy, M. K., Bono, J. E., & Yang, T. (2011). Mindfulness at work. Research in Personnel and Human Resources Management, 30, 115.
Greeson, J. M. (2009). Mindfulness research update: 2008. Complementary Health Practice Review, 14(1), 10–18. https://doi.org/10.1177/1533210108329862.
Hayes, A. F. (2012). PROCESS: a versatile computational tool for observed variable mediation, moderation, and conditional process modeling.
Ilardi, B. C., Leone, D., Kasser, T., & Ryan, R. M. (1993). Employee and supervisor ratings of motivation: main effects and discrepancies associated with job satisfaction and adjustment in a factory setting1. Journal of Applied Social Psychology, 23(21), 1789–1805.
Irving, J. A., Dobkin, P. L., & Park, J. (2009). Cultivating mindfulness in health care professionals: a review of empirical studies of mindfulness-based stress reduction (MBSR). Complementary Therapies in Clinical Practice, 15(2), 61–66.
Jamieson, S. D., & Tuckey, M. R. (2017). Mindfulness interventions in the workplace: a critique of the current state of the literature. Journal of Occupational Health Psychology, 22(2), 180–193.
Kabat-Zinn, J. (1990). Full catastrophe living: the program of the stress reduction clinic at the University of Massachusetts Medical Center. New York: Delta.
Kiken, L. G., Lundberg, K. B., & Fredrickson, B. L. (2017). Being present and enjoying it: dispositional mindfulness and savoring the moment are distinct, interactive predictors of positive emotions and psychological health. Mindfulness, 8(5), 1280–1290. https://doi.org/10.1007/s12671-017-0704-3.
Leonard, M. (2016). Making mindfulness meditation accessible and meaningful. In M. A. Chapman-Clarke (Ed.), Mindfulness in the workplace: an evidence-based approach to improving wellbeing and maximizing performance (pp. 247–266). London: Kogan Page Publishers.
Maben, J., Peccei, R., Adams, M., Robert, G., Richardson, A., Murrells, T., et al. (2012). Exploring the relationship between patients’ experiences of care and the influence of staff motivation, affect and wellbeing. Final report. Southampton: NIHR service delivery and organization programme.
Manotas, M., Segura, C., Eraso, M., Oggins, J., & McGovern, K. (2014). Association of brief mindfulness training with reductions in perceived stress and distress in Colombian health care professionals. International Journal of Stress Management, 21(2), 207–225.
Martín-Asuero, A., & García-Banda, G. (2010). The mindfulness-based stress reduction program (MBSR) reduces stress-related psychological distress in healthcare professionals. The Spanish Journal of Psychology, 13(2), 897–905.
Marzuq, N., & Drach-Zahavy, A. (2012). Recovery during a short period of respite: the interactive roles of mindfulness and respite experiences. Work & Stress, 26(2), 175–194.
Morgan, P., Simpson, J., & Smith, A. (2015). Health care workers’ experiences of mindfulness training: a qualitative review. Mindfulness (N Y), 6(4), 744–758.
Nash, J. D., & Newberg, A. (2013). Toward a unifying taxonomy and definition for meditation. Frontiers in Psychology, 4, 806.
Patrick, H., Knee, C. R., Canevello, A., & Lonsbary, C. (2007). The role of need fulfillment in relationship functioning and well-being: a self-determination theory perspective. Journal of Personality and Social Psychology, 92(3), 434–457.
Quested, E., Bosch, J. A., Burns, V. E., Cumming, J., Ntoumanis, N., & Duda, J. L. (2011). Basic psychological need satisfaction, stress-related appraisals, and dancers’ cortisol and anxiety responses. Journal of Sport and Exercise Psychology, 33(6), 828–846.
Ryan, R. M., & Brown, K. W. (2003). Why we don’t need self-esteem: on fundamental needs, contingent love, and mindfulness. Psychological Inquiry, 14(1), 71–76.
Ryan, R. M., Kuhl, J., & Deci, E. L. (1997). Nature and autonomy: an organizational view of social and neurobiological aspects of self-regulation in behavior and development. Development and Psychopathology, 9(4), 701–728.
Ryan, R. M., Bernstein, J. H., & Brown, K. W. (2010). Weekends, work, and well-being: psychological need satisfactions and day of the week effects on mood, vitality, and physical symptoms. Journal of Social and Clinical Psychology, 29(1), 95–122.
Segal, Z. V., Williams, J. M. G., & Teasdale, J. D. (2002). Mindfulness-based cognitive therapy for depression: a new approach to preventing relapse. New York: Guilford Press.
Shapiro, S. L., Schwartz, G. E., & Bonner, G. (1998). Effects of mindfulness-based stress reduction on medical and premedical students. Journal of Behavioral Medicine, 21(6), 581–599.
Shapiro, S. L., Astin, J. A., Bishop, S. R., & Cordova, M. (2005). Mindfulness-based stress reduction for health care professionals: results from a randomized trial. International Journal of Stress Management, 12(2), 164–176.
Shapiro, S. L., Carlson, L. E., Astin, J. A., & Freedman, B. (2006). Mechanisms of mindfulness. Journal of Clinical Psychology., 62(3), 373–386,
Sheldon, K. M., & Elliot, A. J. (1999). Goal striving, need satisfaction, and longitudinal well-being: the self-concordance model. Journal of Personality and Social Psychology, 76(3), 482–497.
Wolever, R. Q., Bobinet, K. J., McCabe, K., Mackenzie, E. R., Fekete, E., Kusnick, C. A., et al. (2012). Effective and viable mind-body stress reduction in the workplace: a randomized controlled trial. Journal of Occupational Health Psychology, 17(2), 246–258. https://doi.org/10.1037/a0027278.
Acknowledgements
The study team would like to thank Mark Leonard of Mindfulness Connected Limited for providing insight and a description of the MBOE course. CJ would like to thank Robin Leonard of Mindfulness Connected Limited for co-designing the Mindfulness Connected app. To ensure the scheduled delivery of the course, we enjoyed the full approval and ongoing support of the hospital trust board and executives, from the chairman Dame Yve Buckland and chief executive to line-managers and service leads.
Funding
This work was sponsored by the Royal Orthopaedic Hospital Foundation Trust (ROHFT) and funded by ROHFT Charitable Funds and the Engineering and Physical Sciences Research Council (EPSRC) grant EP/G03723X/1 (Centre for Doctoral Training in Media and Arts Technology). The write-up of this paper for publication was unpaid.
Author information
Authors and Affiliations
Contributions
AK, CJ and CB conceived the study. AK, CJ and CB designed the study and secured funding. AK and CJ conducted the analysis and drafted the manuscript with input from AH. All authors approved the final manuscript.
Adele Krusche and Christopher Jack contributed equally to this paper and are joint first authors.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Informed Consent
Consent was taken online by each study participant before beginning the baseline questionnaires.
Ethics Statement
This study was approved by the NHS Research Ethics Committee, reference 16/HRA/2783.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
OpenAccess This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Krusche, A., Jack, C.D., Blunt, C. et al. Mindfulness-Based Organisational Education: an Evaluation of a Mindfulness Course Delivered to Employees at the Royal Orthopaedic Hospital. Mindfulness 11, 362–373 (2020). https://doi.org/10.1007/s12671-019-01121-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-019-01121-x