Abstract
Background
Acceptance and commitment therapy has shown to be effective in chronic pain rehabilitation, and acceptance has been shown to be a key process of change. The influence of treatment dose on acceptance is not clear, and in particular, the effectiveness of a non-intensive treatment (<20 h) in a tertiary pain clinic is required.
Purpose
The purpose of the study was to assess the effectiveness of a low-intensity, acceptance and commitment therapy (ACT) group program for chronic pain. The study sought to compare, at both groups and individual patient levels, changes in acceptance with changes observed in previous ACT studies.
Methods
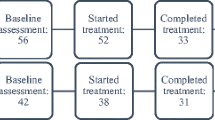
Seventy-one individuals with chronic pain commenced a 9-week ACT-based group program at an outpatient chronic pain service. In addition to acceptance, outcomes included the following: pain catastrophizing, depression, anxiety, quality of life, and pain-related anxiety. To compare the current findings with previous research, effect sizes from seven studies were aggregated using the random-effects model to calculate benchmarks. Reliable change indices (RCIs) were applied to assess change on an individual patient-level.
Results
The ACT intervention achieved a statistically significant increase in acceptance and medium effect size (d = 0.54) at a group level. Change in acceptance was of a similar magnitude to that found in previous ACT studies that examined interventions with similar treatment hours (<20 h). Results across other outcome measures demonstrated small to medium effect sizes (d = 0.01 to 0.48, mean = 0.26). Reliable improvement in acceptance occurred in approximately one-third (37.2, 90 % CI) of patients. Approximately three-quarters (74.3, 90 % CI) demonstrated reliable change in at least one of the outcome measures.
Conclusions
The low-intensity, group-based ACT intervention was effective at a group level and showed a similar magnitude of change in acceptance to previous ACT studies employing low-intensity interventions. Three-quarters of patients reported reliable change on at least one outcome measure.
Similar content being viewed by others
References
Vowles KE, Wetherell JL, Sorrell JT. Targeting acceptance, mindfulness, and values-based action in chronic pain: findings of two preliminary trials of an outpatient group-based intervention. Cogn Behav Pract. 2009;16(1):49–58.
Wetherell JL, Afari N, Rutledge T, Sorrell JT, Stoddard JA, Petkus AJ, et al. A randomized, controlled trial of acceptance and commitment therapy and cognitive-behavioral therapy for chronic pain. Pain. 2011;152(9):2098–107.
American Psychological Association Division 12 Society of Clinical Psychology. 2012. Psychological treatments. http://www.div12.org/PsychologicalTreatments/treatments.html. Accessed 23 Sep 2014.
McCracken LM, Gutiérrez-Martínez O. Processes of change in psychological flexibility in an interdisciplinary group-based treatment for chronic pain based on acceptance and commitment therapy. Behav Res Ther. 2011;49(4):267–74.
McCracken LM, Vowles KE, Eccleston C. Acceptance-based treatment for persons with complex, long standing chronic pain: a preliminary analysis of treatment outcome in comparison to a waiting phase. Behav Res Ther. 2005;43(10):1335–46.
McCracken LM, Jones R. Treatment for chronic pain for adults in the seventh and eighth decades of life: a preliminary study of acceptance and commitment therapy (ACT). Pain Med. 2012;13(7):860–7.
Flor H, Turk C. Chronic pain: an integrated biobehavioral approach. Seattle: IASP Press; 2011.
McCracken LM, Morley S. The psychological flexibility model: a basis for integration and progress in psychological approaches to chronic pain management. J Pain. 2014;15(3):221–34.
McCracken LM, Sato A, Taylor GJ. A trial of a brief group-based form of acceptance and commitment therapy (ACT) for chronic pain in general practice: pilot outcome and process results. J Pain. 2013;14(11):1398–406.
Reneman MF, Dijkstra A, Geertzen JH, Dijkstra PU. Psychometric properties of chronic pain acceptance questionnaires: a systematic review. Eur J Pain. 2010;14(5):457–65.
Fish RA, McGuire B, Hogan M, Morrison TG, Stewart I. Validation of the Chronic Pain Acceptance Questionnaire (CPAQ) in an Internet sample and development and preliminary validation of the CPAQ-8. Pain. 2010;149(3):435–43.
Fish RA, Hogan MJ, Morrison TG, Stewart I, McGuire BE. Willing and able: a closer look at pain willingness and activity engagement on the Chronic Pain Acceptance Questionnaire (CPAQ-8). J Pain. 2013;14(3):233–45.
Baranoff J, Hanrahan SJ, Kapur D, Connor JP. Validation of the chronic pain acceptance questionnaire-8 in an Australian pain clinic sample. Int J Behav Med. 2014;21(1):177–85.
Rovner GS, Årestedt K, Gerdle B, Börsbo B, McCracken LM. Psychometric properties of the 8-item Chronic Pain Acceptance Questionnaire (CPAQ-8) in a Swedish chronic pain cohort. J Rehabil Med. 2014;46(1):73–80.
Rosenstiel AK, Keefe FJ. The use of coping strategies in chronic low back pain patients: relationship to patient characteristics and current adjustment. Pain. 1983;17(1):33–44.
Robinson ME, Riley JL, Myers CD, Sadler IJ, Kvaal SA, Geisser ME, et al. The Coping Strategies Questionnaire: a large sample, item level factor analysis. Clin J Pain. 1997;13(1):43–9.
Hirsh AT, George SZ, Riley JL, Robinson ME. An evaluation of the measurement of pain catastrophizing by the coping strategies questionnaire. Eur J Pain. 2007;11(1):75–81.
Stewart MW, Harvey ST, Evans IM. Coping and catastrophizing in chronic pain: a psychometric analysis and comparison of two measures. J Clin Psychol. 2001;57(1):131–8.
McCracken LM, Vowles KE, Eccleston C. Acceptance of chronic pain: component analysis and a revised assessment method. Pain. 2004;107(1):159–66.
Rodero B, García-Campayo J, Casanueva B, del Hoyo YL, Serrano-Blanco A. Luciano, JV Research Validation of the Spanish version of the Chronic Pain Acceptance Questionnaire (CPAQ) for the assessment of acceptance in fibromyalgia. Health Qual Life Outcome. 2010;8:37–46.
Zigmond AS, Snaith RP. The hospital anxiety and depression scale. Acta Psychiatr Scand. 1983;67(6):361–70.
Snaith RP. The hospital anxiety and depression scale. Health Qual Life Outcomes. 2003;1(1):29–32.
Herrmann C. International experiences with the Hospital Anxiety and Depression Scale-a review of validation data and clinical results. J Psychosom Res. 1997;42(1):17–41.
Gandek B, Sinclair SJ, Kosinski M, Ware Jr JE. Psychometric evaluation of the SF-36 health survey in Medicare managed care. Health Care Financ Rev. 2004;25(4):5–25.
Hopman WM, Berger C, Joseph L, Towheed T, van den Kerkhof E, Anastassiades T, et al. Stability of normative data for the SF-36: Results of a three-year prospective study in middle-aged Canadians. Can J Public Health. 2004;95(5):387–91.
Calsyn DA, Saxon AJ, Bush KR, Howell DN, Baer JS, Sloan KL, et al. The Addiction Severity Index medical and psychiatric composite scores measure similar domains as the SF-36 in substance-dependent veterans: concurrent and discriminant validity. Drug Alcohol Depend. 2004;76(2):165–71.
Ware Jr JE, Kosinski M, Keller SD. SF-36 Physical and Mental Health Summary Scales: A User’s Manual. Boston: The Health Institute, New England Medical Center; 1994.
McCracken LM, Dhingra L. A short version of the Pain Anxiety Symptoms Scale (PASS--20): Preliminary development and validity. Pain Res Manag. 2002;7(1):45–50.
McCracken LM, Zayfert C, Gross RT. The Pain Anxiety Symptoms Scale (PASS): A multimodal measure of pain-specific anxiety symptoms. Behav Ther. 1993;1:183–4.
Coons MJ, Hadjistavropoulos HD, Asmundson GJ. Factor structure and psychometric properties of the Pain Anxiety Symptoms Scale‐20 in a community physiotherapy clinic sample. Eur J Pain. 2004;8(6):511–6.
Thompson M, McCracken LM. Acceptance and related processes in adjustment to chronic pain. Curr Pain Headache Rep. 2011;15(2):144–51.
Cohen J. A power primer. Psychol Bull. 1992;112(1):155–9.
Hedges LV, Olkin I. Statistical methods for meta-analysis. Orlando: Academic; 1985.
Rosenthal R. Meta-analytic methods for social research. Newbury Park: Sage; 1993.
Borenstein M, Hedges LV, Higgins JP, Rothstein HR. Introduction to meta-analysis. Chichester: Wiley; 2011.
Higgins J, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327(7414):557–60.
Orwin RG. A fail-safe N for effect size in meta-analysis. J Educ Stat. 1983;8(2):157–9.
Jacobson NS, Truax P. Clinical significance: a statistical approach to defining meaningful change in psychotherapy research. J Consult Clin Psychol. 1991;59(1):12–9.
Han X, Geffen S, Browning M, Kenardy J, Geffen G. Outcome evaluation of a multidisciplinary pain management programme comparing group with individual change measures. Clinical Psychologist. 2011;15(3):133–8.
Vowles KE, McCracken LM. Acceptance and values-based action in chronic pain: a study of treatment effectiveness and process. J Consult Clin Psychol. 2008;76(3):397–407.
Vowles KE, McCracken LM, Eccleston C. Processes of change in treatment for chronic pain: the contributions of pain, acceptance, and catastrophizing. Eur J Pain. 2007;11(7):779–87.
Acknowledgments
Jason Connor is supported by an Australian National Health and Medical Research Council (NH&MRC) Career Development Fellowship (APP1031909). The authors would like to thank the patients of the Royal Adelaide Hospital (RAH) Pain Management Unit, who attended the sessions and completed the questionnaires. Thanks are also extended to the staff at the RAH Pain Management Unit and Psychology Department for their support of this project.
Contributors
Anne Burke provided clinical management of the pain program. The statistical analysis was conducted by Dr John Baranoff, under the guidance of Dr Jason Connor. An initial draft of the manuscript was written by Dr John Baranoff. All authors contributed to and approved the final draft.
Ethical Standards
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study.
Conflict of Interest
The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Baranoff, J.A., Hanrahan, S.J., Burke, A.L.J. et al. Changes in Acceptance in a Low-Intensity, Group-Based Acceptance and Commitment Therapy (ACT) Chronic Pain Intervention. Int.J. Behav. Med. 23, 30–38 (2016). https://doi.org/10.1007/s12529-015-9496-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12529-015-9496-9