Abstract
Purpose of Review
The goal of this review is to introduce surgical decision-making pearls for reverse shoulder arthroplasty and describe optimization of surgical exposure for reverse shoulder arthroplasty.
Recent Findings
While the technology of reverse shoulder replacement and the associated prosthetic options have expanded, the principles involved in successfully exposing the humerus and glenoid in arthroplasty remain the same.
Summary
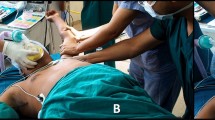
Reverse shoulder replacement should be considered in arthroplasty situations with rotator cuff disease, deformity, bone loss, and instability as part of the diagnosis. Optimal exposure in reverse shoulder arthroplasty can be obtained by (1) releasing deltoid adhesions, (2) removal of humeral osteophytes, (3) generous humeral head cuts, (4) thorough humeral and glenoid capsular release and (5) optimal glenoid retractor placement. Neuromuscular paralysis can also aid glenoid exposure.


Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Grammont P, Troiulloud P, Laffay J, Deries X. Study and development of a new shoulder prosthesis. Rheumatologie. 1987;39:407–18.
Flatow EL, Harrison AK. A history of Reverse Total shoulder arthroplasty. Clin Orthop Relat Res. 2011;469(9):2432–9.
Schairer WW, Nwachukwu BU, Lyman S, Craig EV, Gulotta LV. National utilization of reverse total shoulder arthroplasty in the United States. J Shoulder Elb Surg. 2015;24(1):91–7.
Lung TS, Cruickshank D, Grant HJ, Rainbow MJ, Bryant TJ, Bicknell RT. Factors contributing to glenoid baseplate micromotion in reverse shoulder arthroplasty : a biomechanical study. J Shoulder Elb Surg. 2019;28(4):648–53.
Wiater JM, Jr JEM, Budge MD, Koueiter DM, Marcantonio D, Wiater BP. Clinical and radiographic results of cementless reverse total shoulder arthroplasty : a comparative study with 2 to 5 years of follow-up. J Shoulder Elb Surg. 2014;23(8):1208–14.
Peers S, Moravek JE Jr, Budge MD, Newton MD, Kurdziel MD, Baker KC, et al. Wear rates of highly cross-linked polyethylene humeral liners subjected to alternating cycles of glenohumeral flexion and abduction. J Shoulder Elb Surg. 2015;24(1):143–9.
Carpenter SR, Urits I, Murthi AM. Porous metals and alternate bearing surfaces in shoulder arthroplasty. Curr Rev Musculoskelet Med. 2016;9:59–66.
•Werner BS, Chaoui J, Walch G. The influence of humeral neck shaft angle and glenoid lateralization on range of motion in reverse shoulder arthroplasty. J Shoulder Elb Surg. 2017;26(10):1726–31 This computer simulation study demonstrates the effect of a lower humeral neck-shaft angle and lateralized glenoid component on lowering the rate of impingement following RTSA, with implications for subsequent prosthetic design.
Werner BC, Dines JS, Dines DM, Werner BC. Platform systems in shoulder arthroplasty. Curr Rev Musculoskelet Med. 2016;9:49–53.
Grosel TW, Darren BS, Joel RP, Scharschmidt TJ, Barlow JD Oncologic reconstruction of the proximal humerus with a reverse total shoulder arthroplasty megaprosthesis. J Surg Oncol 2018;118(6):867–872. https://doi.org/10.1002/jso.25061.
•Gagliano JR, Helms SM, Colbath GP, Przestrzelski BT, Hawkins RJ, Desjardins JD. BASIC SCIENCE A comparison of onlay versus inlay glenoid component loosening in total shoulder arthroplasty. J Shoulder Elb Surg. 2017;26(7):1113–20 This cadaveric biomechanical study compares inlay and onlay glenoid components in TSA, suggesting that onlay-style implants may be prone to loosening secondary to edge-loading.
Collin P, Liu X, Denard PJ, Gain S, Nowak A, Lädermann A. Standard versus bony increased-offset reverse shoulder arthroplasty : a retrospective comparative cohort study. J Shoulder Elb Surg. 2018;27(1):59–64.
Werthel J et al. Lateralization in reverse shoulder arthroplasty : a descriptive analysis of different implants in current practice. Int Orthop 2019;43(10):2349–2360. https://doi.org/10.1007/s00264-019-04365-3.
••Ivaldo N, Mangano T, Caione G, Rossoni M, Ligas A. Customized tantalum-augmented reverse shoulder arthroplasty for glenoid bone defect and excessive medialization : description of the technique. Musculoskelet Surg. 2016;100(s1):13–8 This study describes a novel technique using custom porous tantalum glenoid components to create a lateralized RTSA prosthesis in the setting of tumor reconstruction, with implications both for implant biomechanics as well as biomaterials.
Nashikkar PS, Scholes CJ, Haber MD. Role of intraoperative navigation in the fixation of the glenoid component in reverse total shoulder arthroplasty : a clinical case-control study. J Shoulder Elb Surg. 2019;28(9):1685–91. https://doi.org/10.1016/j.jse.2019.03.013.
Venne G, Rasquinha BJ, Pichora D, Ellis RE, Bicknell R. Comparing conventional and computer-assisted surgery baseplate and screw placement in reverse shoulder arthroplasty. J Shoulder Elb Surg. 2015;24(7):1112–9.
Verborgt O, De Smedt T, Vanhees M, Clockaerts S, Parizel PM, Van Glabbeek F. Accuracy of placement of the glenoid component in reversed shoulder arthroplasty with and without navigation. J Shoulder Elb Surg. 2011;20(1):21–6.
Levy JC, Everding NG, Frankle MA, Keppler LJ. Accuracy of patient-specific guided glenoid baseplate positioning for reverse shoulder arthroplasty. J Shoulder Elb Surg. 2014;23(10):1563–7.
Walch G, Badet R, Boulahia A. Morphologic Study of the Glenoid in Primary Glenohumeral Osteoarthritis. J Arthroplast. 1999;14(6):756–60.
Nové-josserand L, Clavert P. Glenoid exposure in total shoulder arthroplasty. Orthop Traumatol Surg Res. 2018;104(1):S129–35.
Berhouet J, et al. Preoperative planning for accurate glenoid component positioning in reverse shoulder arthroplasty. Orthop Traumatol Surg Res. 2017;103(3):407–13.
Goutallier D, Postel JM, Bernageau J, Lavau L, Voisin MC. Fatty muscle degeneration in cuff ruptures. Pre- and postoperative evaluation by CT scan. Clin Orthop Relat Res. 1994;304:78–83.
Neer Cuff-Tear. 1983; J Bone Joint Surg Am. 1983;65(9):1232–1244.
Mulieri P, Dunning P, Klein S, Pupello D, Reverse FM. Shoulder arthroplasty for the treatment of irreparable rotator cuff tear without Glenohumeral arthritis. J Bone Joint Surg Am. 2010;92(15):2544–56. https://doi.org/10.2106/JBJS.I.00912.
Kontakis G, Tosounidis T, Galanakis I. Prosthetic replacement for proximal humeral fractures. Preoperative planning for accurate glenoid component positioning in reverse shoulder arthroplasty. Orthop Traumatol Surg Res. 2017;103(3):407–13. https://doi.org/10.1016/j.otsr.2016.12.019.
Boileau P, Chuinard C, Bicknell R, Frcs C, Walch G. Reverse total shoulder arthroplasty after failed rotator cuff surgery. J Shoulder Elb Surg. 2009;18:600–6.
Hansen ML, Routman H. The biomechanics of current reverse shoulder replacement options. Annals of Joint. 2019;4:1–7.
Berliner JL, Regalado-magdos A, Ma CB, Feeley BT. Biomechanics of reverse total shoulder arthroplasty. J Shoulder Elb Surg. 2015;24(1):150–60.
••Ferle M, Pastor M, Hagenah J, Hurschler C, Smith T. Effect of the humeral neck-shaft angle and glenosphere lateralization on stability of reverse shoulder arthroplasty : a cadaveric study. J Shoulder Elb Surg. 2019;28(5):966–73 This computer-aided biomechanical study builds on earlier data suggesting the benefits of a lower humeral neck-shaft angle and lateralized glenoid component, demonstrating that glenosphere lateralization is associated with increased stability in RTSA. Interestingly, external rotation range was not significant affected.
Berhouet J, Garaud P, Favard L. Evaluation of the role of glenosphere design and humeral component retroversion in avoiding scapular notching during reverse shoulder arthroplasty. J Shoulder Elb Surg. 2014;23(2):151–8.
Werthel J, et al. Acromial fractures in Reverse shoulder arthroplasty : A clinical and radiographic analysis. Journal of Shoulder and Elbow Arthroplasty. 2018;2:1–9.
Boileau P, Watkinson D, Hatzidakis AM, Hovorka I. Neer Award 2005 : The Grammont reverse shoulder prosthesis : Results in cuff tear arthritis , fracture sequelae , and revision arthroplasty. J Shoulder Elb Surg. 2006;15:527–40.
Birmingham P, Sperling JW, Craig E, Care P. Glenoid exposure in shoulder arthroplasty. Techniques in Shoulder and Elbow Surgery. 2010;11(3):92–6.
Nové-josserand L. Instructional lecture : Shoulder & Elbow Exposing the glenoid in shoulder arthroplasty. EFORT Open Rev. 2019;4(6):248–53. https://doi.org/10.1302/2058-5241.4.180057.
Gadea F, Bouju Y, Berhouet J. Deltopectoral approach for shoulder arthroplasty : anatomic basis. Int Orthop. 2015;39(2):215–25. https://doi.org/10.1007/s00264-014-2654-x.
Williams GR Jr. Top ten tips for glenoid exposure in shoulder arthroplasty. Semin Arthroplast. 2017;28(3):124–7.
Nagda SH et al. Peripheral nerve function during shoulder arthroplasty using intraoperative nerve monitoring. J Shoulder Elb Surg. 2007;16(3Suppl):S2–S8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Harshvardhan Chawla and Seth Gamradt declare that they have no conflict of interest. Seth Gamradt receives consultancy fees from Zimmer Biomet Holdings, Inc. and Arthrex, Inc. outside of the submitted work.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Reverse Shoulder Arthroplasty
Rights and permissions
About this article
Cite this article
Chawla, H., Gamradt, S. Reverse Total Shoulder Arthroplasty: Technique, Decision-Making and Exposure Tips. Curr Rev Musculoskelet Med 13, 180–185 (2020). https://doi.org/10.1007/s12178-020-09613-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12178-020-09613-3