Abstract
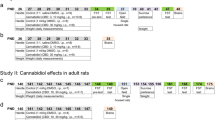
Currently available antidepressants have a substantial time lag to induce therapeutic response and a relatively low efficacy. The development of drugs that addresses these limitations is critical to improving public health. Cannabidiol (CBD), a non-psychotomimetic component of Cannabis sativa, is a promising compound since it shows large-spectrum therapeutic potential in preclinical models and humans. However, its antidepressant properties have not been completely investigated. Therefore, the aims of this study were to investigate in male rodents (i) whether CBD could induce rapid and sustained antidepressant-like effects after a single administration and (ii) whether such effects could be related to changes in synaptic proteins/function. Results showed that a single dose of CBD dose-dependently induced antidepressant-like effect (7–30 mg/kg) in Swiss mice submitted to the forced swim test (FST), 30 min (acute) or 7 days (sustained) following treatment. Similar effects were observed in the Flinders Sensitive and Flinders Resistant Line (FSL/FRL) rats and the learned helplessness (LH) paradigm using Wistar rats. The acute antidepressant effects (30 min) were associated with increased expression of synaptophysin and PSD95 in the medial prefrontal cortex (mPFC) and elevated BDNF levels in both mPFC and hippocampus (HPC). CBD also increased spine density in the mPFC after 30 min, but not 7 days later. Intracerebroventricular injection of the TrkB antagonist, K252a (0.05 nmol/μL), or the mTOR inhibitor, rapamycin (1 nmol/μL), abolished the behavioral effects of CBD. These results indicate that CBD induces fast and sustained antidepressant-like effect in distinct animal models relevant for depression. These effects may be related to rapid changes in synaptic plasticity in the mPFC through activation of the BDNF-TrkB signaling pathway. The data support a promising therapeutic profile for CBD as a new fast-acting antidepressant drug.





Similar content being viewed by others
References
Vigo D, Thornicroft G, Atun R (2018) Estimating the true global burden of mental illness. Lancet Psychiatry 3:171–178
World Health Organization (WHO) (2017) Depression. website http://www.who.int/mediacentre/factsheets/fs369/en/.
Cleare A, Pariante CM, Young AH, Anderson IM, Christmas D, Cowen PJ, Dickens C, Ferrier IN et al (2015) Evidence-based guidelines for treating depressive disorders with antidepressants: a revision of the 2008 British Association for Psychopharmacology guidelines. J Psychopharmacol 29(5):459–525
Bauer M, Severus E, Köhler S, Whybrow PC, Angst J, Möller H (2015) World federation of societies of biological psychiatry (WFSBP) guidelines for biological treatment of unipolar depressive disorders in primary care. World J Biol Psychiatry 16:76–95
Shelton RC, Osuntokun O, Heinloth AN, Corya SA (2010) Therapeutic options for treatment-resistant depression. CNS Drugs 24(2):131–161. https://doi.org/10.2165/11530280-000000000-00000
Dodd S, Mitchell PB, Bauer M, Yatham L, Allan H, Kennedy SH et al (2017) Monitoring for antidepressant-associated adverse events in the treatment of patients with major depressive disorder: an international consensus statement. World J Biol Psychiatry 6:1–19
Ho SC, Jacob SA, Tangiisuran B (2017) Barriers and facilitators of adherence to antidepressants among outpatients with major depressive disorder: a qualitative study. PLoS One 12(6):e0179290. https://doi.org/10.1371/journal.pone.0179290. eCollection 2017
Agid Y, Buzsáki G, Diamond DM, Frackowiak R, Giedd J, Girault J et al (2007) How can drug discovery for psychiatric disorders be improved? Nat Rev Drug Discov 6:189–201. https://doi.org/10.1038/nrd2217
Duman RS, Heninger GR, Nestler EJ (1997) A molecular and cellular theory of depression. Arch Gen Psychiatry 54(7):597–606
Zarate CA Jr, Niciu MJ (2015) Ketamine for depression: evidence, challenges and promise. World Psychiatry 14(3):348–350. doi: https://doi.org/10.1002/wps.20269.
Ghosal S, Hare BD, Duman RS (2017) Prefrontal cortex GABAergic deficits and circuit dysfunction in the pathophysiology and treatment of chronic stress and depression. Curr Opin Behav Sci 14:1–8. https://doi.org/10.1016/j.cobeha.2016.09.012
Harmer CJ, Duman RS, Cowen PJ (2017) How do antidepressants work? New perspectives for refining future treatment approaches. Lancet Psychiatry 366:1–10. https://doi.org/10.1016/S2215-0366(17)30015-9
Castrén E, Rantamäki T (2010) The role of BDNF and its receptors in depression and antidepressant drug action: reactivation of developmental plasticity. Dev Neurobiol 70(5):289–297. https://doi.org/10.1002/dneu.20758
Yu H, Chen ZY (2011) The role of BDNF in depression on the basis of its location in the neural circuitry. Acta Pharmacol Sin 32:3–11. https://doi.org/10.1038/aps.2010.184
Castrén E (2004) Neurotrophic effects of antidepressant drugs. Curr Opin Pharmacol 4:58–64. https://doi.org/10.1016/j.coph.2003.10.004
Pandey GN, Ren X, Rizavi HS, Conley RR, Roberts RC, Dwivedi Y (2008) Brain-derived neurotrophic factor and tyrosine kinase B receptor signalling in post-mortem brain of teenage suicide victims. Int J Neuropsychopharmacol 11(8):1047–1061. https://doi.org/10.1017/S1461145708009000
Autry AE, Monteggia LM (2012) Brain-derived neurotrophic factor and neuropsychiatric disorders. Pharmacol Rev 64(2):238–258. https://doi.org/10.1124/pr.111.005108
Park H, Poo M (2013) Neurotrophin regulation of neural circuit development and function. Nat Rev Neurosci 14(1):7–23. https://doi.org/10.1038/nrn3379
Ardalan M, Wegener G, Polsinelli B, Madsen TM, Nyengaard JR (2016) Neurovascular plasticity of the hippocampus one week after a single dose of ketamine in genetic rat model of depression. Hippocampus 26(11):1414–1423. https://doi.org/10.1002/hipo.22617
Ardalan M, Rafati AH, Nyengaard JR, Wegener G (2017a) Rapid antidepressant effect of ketamine correlates with astroglial plasticity in the hippocampus. Br J Pharmacol 174(6):483–492. https://doi.org/10.1111/bph.13714
Ardalan M, Wegener G, Rafati AH, Nyengaard JR (2017b) S-Ketamine rapidly reverses synaptic and vascular deficits of hippocampus in genetic animal model of depression. Int J Neuropsychopharmacol 20(3):247–256. https://doi.org/10.1093/ijnp/pyw098
Bjorkholm C, Monteggia LM (2016) BDNF e a key transducer of antidepressant effects. Neuropharmacology 102:72–79. https://doi.org/10.1016/j.neuropharm.2015.10.034
Jiang Y, Wang Y, Sun X, Lian B, Sun H, Wang G, du Z, Li Q et al (2017) Short- and long-term antidepressant effects of ketamine in a rat chronic unpredictable stress model. Brain Behav 7(8):e00749. https://doi.org/10.1002/brb3.749
Campos AC, Fogaça MV, Scarante FF, Joca SRL, Sales AJ, Gomes FV, Sonego AB, Rodrigues NS, Galve-Roperh I, Guimarães FS (2017) Plastic and neuroprotective mechanisms involved in the therapeutic effects of cannabidiol in psychiatric disorders. Front Pharmacol 23;8:269. doi: https://doi.org/10.3389/fphar.2017.00269.
Zanelati T, Biojone C, Moreira F, Guimarães FS, Joca S (2010) Antidepressant-like effects of cannabidiol in mice: possible involvement of 5-HT 1A receptors. Br J Pharmacol 159:122–128. https://doi.org/10.1111/j.1476-5381.2009.00521.x
El-alfy AT, Ivey K, Robinson K, Ahmed S, Radwan M, Slade D et al (2010) Antidepressant-like effect of Δ 9-tetrahydrocannabinol and other cannabinoids isolated from Cannabis sativa L. Pharmacol Biochem Behav 95:434–442. https://doi.org/10.1016/j.pbb.2010.03.004
Réus GZ, Stringari RB, Ribeiro KF, Luft T, Abelaira HM, Fries GR, Aguiar BW, Kapczinski F et al (2011) Administration of cannabidiol and imipramine induces antidepressant-like effects in the forced swimming test and increases brain-derived neurotrophic factor levels in the rat amygdala. Acta Neuropsychiatrica 23:241–248. https://doi.org/10.1111/j.1601-5215.2011.00579.x
Linge R, Jiménez-Sánches L, Campa L, Pilar-Cuéllar F, Vidal R, Pazos A et al (2016) Cannabidiol induces rapid-acting antidepressant-like effects and enhances cortical 5-HT/glutamate neurotransmission: role of 5-HT 1A receptors. Neuropharmacology 103:16–26. https://doi.org/10.1016/j.neuropharm.2015.12.017
Sartim AG, Guimarães FS, Joca SRL (2016) Antidepressant-like effect of cannabidiol injection into the ventral medial prefrontal cortex—possible involvement of 5-HT1A and CB1 receptors. Behav Brain Res 303:218–227. https://doi.org/10.1016/j.bbr.2016.01.033
Schiavon A, Bonato J, Milani H, Guimarães F, Maria R, Weffort De Oliveira R (2016) Influence of single and repeated cannabidiol administration on emotional behavior and markers of cell proliferation and neurogenesis in non-stressed mice. Prog Neuro-Psychopharmacol Biol Psychiatry 64:27–34. https://doi.org/10.1016/j.pnpbp.2015.06.017
Esposito G, Scuderi C, Valenza M, Togna GI, Latina V, De Filippis D, Cipriano M, Carratù MR et al (2011) Cannabidiol reduces Aβ-induced neuroinflammation and promotes hippocampal neurogenesis through PPARγ involvement. PLoS One 6(12):e28668. https://doi.org/10.1371/journal.pone.0028668
Russo EB, Burnett A, Hall B, Parker KK (2005) Agonistic properties of cannabidiol at 5-HT1a receptors. Neurochem Res 30(8):1037–1043
Bisogno T, Hanus L, De Petrocellis L, Tchilibon S, Ponde DE, Brandi I et al (2001) Molecular targets for cannabidiol and its synthetic analogues: effect on vanilloid VR1 receptors and on the cellular uptake and enzymatic hydrolysis of anandamide. Br J Pharmacol 134(4):845–852
Leweke F, Piomelli D, Muhi D, Gerth C, Hoyer C, Klosterkötter J et al (2012) Cannabidiol enhances anandamide signaling and alleviates psychotic symptoms of schizophrenia. Transl Psychiatry 20(2):e94. https://doi.org/10.1038/tp.2012.15
Giacoppo S, Pollastro F, Grassi G, Bramanti P, Mazzon E (2017) Target regulation of PI3K/Akt/mTOR pathway by cannabidiol in treatment of experimental multiple sclerosis. Fitoterapia 116:77–84. https://doi.org/10.1016/j.fitote.2016.11.010
Mori MA, Meyer E, Soares LM, Milani H, Guimarães FS, de Oliveira RM (2017) Cannabidiol reduces neuroinfammation and promotes neuroplasticity and functional recovery after brain ischemia. Prog. Neuropsychopharmacol. Biol Psychiatry 3(75):94–105. https://doi.org/10.1016/j.pnpbp.2016.11.005
Casarotto PC, de Bortoli VC, Corrêa FM, Resstel LB, Zangrossi H Jr (2010) Panicolytic-like effect of BDNF in the rat dorsal periaqueductal grey matter: the role of 5-HT and GABA. Int J Neuropsychopharmacol 13(5):573–582. https://doi.org/10.1017/S146114570999112X
Liebenberg N, Joca S, Wegener G (2015) Nitric oxide involvement in the antidepressant-like effect of ketamine in the Flinders sensitive line rat model of depression. Acta Neuropsychiatr 27(2):90–96. https://doi.org/10.1017/neu.2014.39
Li N, Lee B, Liu RJ, Banasr M, Dwyer JM, Iwata M, Li XY, Aghajanian G et al (2010) mTOR-dependent synapse formation underlies the rapid antidepressant effects of NMDA antagonists. Science 329(5994):959–964. https://doi.org/10.1126/science.1190287
Porsolt RD, Bertin A, Jalfre M (1977) Behavioral despair in mice: a primary screening test for antidepressants. Arch Int Pharmacodyn Ther 229(2):327–336
Paxinos G, Franklin KBJ (2001) The mouse brain in stereotaxic coordinates. 2. San Diego: Academic Press. https://doi.org/10.1111/j.1469-7580.2004.00264.x.
Joca SR, Zanelati T, Guimarães FS (2006) Post-stress facilitation of serotonergic, but not noradrenergic, neurotransmission in the dorsal hippocampus prevents learned helplessness development in rats. Brain Res 1087(1):67–74
Maier SF, Seligman ME (2016) Learned helplessness at fifty: insights from neuroscience. Psychol Rev 123(4):349–367. https://doi.org/10.1037/rev0000033
Overstreet DH, Wegener G (2013) The flinders sensitive line rat model of depression—25 years and still producing. Pharmacol Rev 65(1):143–155. https://doi.org/10.1124/pr.111.005397
Pereira VS, Romano A, Wegener G, Joca SR (2015) Antidepressant-like effects induced by NMDA receptor blockade and NO synthesis inhibition in the ventral medial prefrontal cortex of rats exposed to the forced swim test. Psychopharmacology 232(13):2263–2273. https://doi.org/10.1007/s00213-014-3853-2
Campos AC, Ortega Z, Palazuelos J, Fogaça MV, Aguiar DC, Díaz-Alonso J, Ortega-Gutiérrez S, Vázquez-Villa H et al (2013) The anxiolytic effect of cannabidiol on chronically stressed mice depends on hippocampal neurogenesis: involvement of the endocannabinoid system. Int J Neuropsychopharmacol 16(6):1407–1419. https://doi.org/10.1017/S1461145712001502
Shoval G, Shbiro L, Hershkovitz L, Hazut N, Zalsman G, Mechoulam R, Weller A (2016) Prohedonic effect of cannabidiol in a rat model of depression. Neuropsychobiology 73(2):123–129. https://doi.org/10.1159/000443890
Liu RJ, Lee FS, Li XY, Bambico F, Duman RS, Aghajanian GK (2012) Brain-derived neurotrophic factor Val66Met allele impairs basal and ketamine-stimulated synaptogenesis in prefrontal cortex. Biol Psychiatry 71(11):996–1005. https://doi.org/10.1016/j.biopsych.2011.09.030
Liu RJ, Duman C, Kato T, Hare B, Lopresto D, Bang E et al (2017) GLYX-13 produces rapid antidepressant responses with key synaptic and behavioral effects distinct from ketamine. Neuropharmacology 42:1231–1242. https://doi.org/10.1038/npp.2016.202
Ampuero E, Rubio FJ, Falcon R, Sandoval M, Diaz-Veliz G, Gonzalez RE, Earle N, Dagnino-Subiabre A et al (2010) Chronic fluoxetine treatment induces structural plasticity and selective changes in glutamate receptor subunits in the rat cerebral cortex. Neuroscience 169(1):98–108. https://doi.org/10.1016/j.neuroscience.2010.04.035
O’Leary OF, Wu X, Castren E (2009) Chronic fluoxetine treatment increases expression of synaptic proteins in the hippocampus of the ovariectomized rat: role of BDNF signalling. Psychoneuroendocrinology 34(3):367–381. https://doi.org/10.1016/j.psyneuen.2008.09.015
Li N, Liu RJ, Dwyer JM, Banasr M, Lee B, Son H, Li XY, Aghajanian G et al (2011) Glutamate N-methyl-D-aspartate receptor antagonists rapidly reverse behavioral and synaptic deficits caused by chronic stress exposure. Biol Psychiatry 69(8):754–761. https://doi.org/10.1016/j.biopsych.2010.12.015
Feyissa AM, Chandran A, Stockmeier CA, Karolewicz B (2009) Reduced levels of NR2A and NR2B subunits of NMDA receptor and PSD-95 in the prefrontalcortex in major depression. Prog Neuro-Psychopharmacol Biol Psychiatry 33(1):70–75. https://doi.org/10.1016/j.pnpbp.2008.10.005
Ramaker MJ, Dulawa SC (2017) Identifying fast-onset antidepressants using rodent models. Mol Psychiatry 22(5):656–665. https://doi.org/10.1038/mp.2017.36
Kowianski P, Lietzau G, Czuba E, Waskow M, Steliga A, Morys J (2018) BDNF: a key factor with multipotent impact on brain signaling and synaptic plasticity. Cell Mol Neurobiol 38(3):579–593. https://doi.org/10.1007/s10571-017-0510-4
Taniguchi N, Shinoda Y, Takei N, Nawa H, Ogura A, Tominaga-Yoshino K (2006) Possible involvement of BDNF release in long-lasting synapse formation induced by repetitive PKA activation. Neurosci Lett. 2;406(1–2):38–42.
Ghosal S, Bang E, Yue W, Hare BD, Lepack AE, Girgenti MJ, Duman RS (2018) Activity-dependent brain-derived neurotrophic factor release is required for the rapid antidepressant actions of scopolamine. Biol Psychiatry 1 83(1):29–37. https://doi.org/10.1016/j.biopsych.2017.06.017
Garcia LS, Comim CM, Valvassori SS, Réus GZ, Barbosa LM, Andreazza AC, Stertz L, Fries GR et al (2008) Acute administration of ketamine induces antidepressant-like effects in the forced swimming test and increases BDNF levels in the rat hippocampus. Prog Neuro-Psychopharmacol Biol Psychiatry 1 32(1):140–144
Autry AE, Adachi M, Nosyreva E, Na ES, Los MF, Cheng PF, Kavalali ET, Monteggia LM (2011) NMDA receptor blockade at rest triggers rapid behavioural antidepressant responses. Nature 15; 475(7354):91–95. doi: https://doi.org/10.1038/nature10130.
Jiang DG, Jin SL, Li GY, Li QQ, Li ZR, Ma HX, Zhuo CJ, Jiang RH et al (2016) Serotonin regulates brain-derived neurotrophic factor expression in select brain regions during acute psychological stress. Neural Regen Res 11(9):1471–1479
Yoshimura Y, Ishikawa C, Kasegai H, Masuda T, Yoshikawa M, Shiga T (2017) Roles of 5-HT1A receptor in the expression of AMPA receptor and BDNF in developing mouse cortical neurons. Neurosci Res 115:13–20. https://doi.org/10.1016/j.neures.2016.09.008
Wu YC, Hill RA, Klug M, van den Buuse M (2012) Sex-specific and region-specific changes in BDNF-TrkB signaling in the hippocampus of 5-HT1A receptor and BDNF single and double mutant mice. Brain Res 3(1452):10–17. https://doi.org/10.1016/j.brainres.2012.03.011
Fogaça MV, Campos AC, Coelho LD, Duman RS, Guimarães FS (2018) The anxiolytic effects of cannabidiol in chronically stressed mice are mediated by the endocannabinoid system: role of neurogenesis and dendritic remodeling. Neuropharmacology 3(135):22–33. https://doi.org/10.1016/j.neuropharm.2018.03.001
Diniz CRAF, Casarotto PC, Resstel L, Joca SRL (2018) Beyond good and evil: a putative continuum-sorting hypothesis for the functional role of proBDNF/BDNF-propeptide/mBDNF in antidepressant treatment. Neurosci Biobehav Rev 4(90):70–83. https://doi.org/10.1016/j.neubiorev.2018.04.001
Acknowledgments
The authors acknowledge Flávia Fiacadori Salata and Per Fuglsang Mikkelsen for their helpful technical assistance.
Funding and Disclosure
This work was supported by research grants from the Research Foundation of the State of São Paulo (FAPESP, A.J.S., grant number 2015/01955-0;2012/17626-7); the National Council of Science and Technology, Brazil (CNPq) and National Institute of Science and Translational Medicine (CNPq, 465458/2014-9); the Coordination for the Improvement of Higher Education Personnel (CAPES); and Aarhus University Research Foundation (AU-UDEAS initiative: eMOOD). Gregers Wegener reported having received lecture/consultancy fees from H. Lundbeck A/S, Servier SA, Astra Zeneca AB, Eli Lilly A/S, Sun Pharma Pty Ltd., Pfizer Inc., Shire A/S, HB Pharma A/S, Arla Foods A.m.b.A., Alkermes Inc., and Mundipharma International Ltd.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(DOCX 30 kb)
Rights and permissions
About this article
Cite this article
Sales, A.J., Fogaça, M.V., Sartim, A.G. et al. Cannabidiol Induces Rapid and Sustained Antidepressant-Like Effects Through Increased BDNF Signaling and Synaptogenesis in the Prefrontal Cortex. Mol Neurobiol 56, 1070–1081 (2019). https://doi.org/10.1007/s12035-018-1143-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-1143-4