Abstract
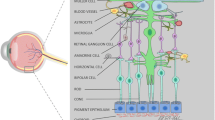
Müller cells are pivotal in sustaining retinal ganglion cells, and an intact energy metabolism is essential for upholding Müller cell functions. The present study aimed to investigate the impact of lactate on Müller cell survival and function. Primary mice Müller cells and human Müller cell lines (MIO-M1) were treated with or without lactate (10 or 20 mM) for 2 and 24 hours. Simultaneously, Müller cells were incubated with or without 6 mM of glucose. L-lactate exposure increased Müller cell survival independently of the presence of glucose. This effect was abolished by the addition of the monocarboxylate inhibitor 4-cinnamic acid to the treatment media, whereas survival continued to increase in response to addition of D-lactate during glucose restriction. ATP levels decreased over time in MIO-M1 cells and remained stable over time in primary Müller cells. Lactate was preferably metabolized in MIO-M1 cells compared to glucose, and 10 mM of L-Lactate exposure prevented complete glycogen depletion in MIO-M1 cells. Glutamate uptake increased after 2 hours and decreased after 24 hours in glucose-restricted Müller cells compared to cells with glucose supplement. The addition of 10 mM of lactate to the treatment media increased glutamate uptake in glucose supplemented and restricted cells. In conclusion, lactate is a key component in maintaining Müller cell survival and function. Hence, lactate administration may be of great future interest, ultimately leading to novel therapies to rescue retinal ganglion cells.








Similar content being viewed by others
References
Goodwin ML, Harris JE, Hernández A, Gladden LB (2007) Blood lactate measurements and analysis during exercise: a guide for clinicians. J Diabetes Sci Technol 1:558–569
Mosienko V, Teschemacher AG, Kasparov S (2015) Is L-lactate a novel signaling molecule in the brain? J Cereb Blood Flow Metab 35:1069–1075. https://doi.org/10.1038/jcbfm.2015.77
Schurr A, Payne RS (2007) Lactate, not pyruvate, is neuronal aerobic glycolysis end product: an in vitro electrophysiological study. Neuroscience 147:613–619. https://doi.org/10.1016/j.neuroscience.2007.05.002
Schurr A (2014) Cerebral glycolysis: a century of persistent misunderstanding and misconception. Front Neurosci 8:360. https://doi.org/10.3389/fnins.2014.00360
Schurr A, Gozal E (2015) Glycolysis at 75: is it time to tweak the first elucidated metabolic pathway in history? Front Neurosci 9:170. https://doi.org/10.3389/fnins.2015.00170
Ros J, Pecinska N, Alessandri B, Landolt H, Fillenz M (2001) Lactate reduces glutamate-induced neurotoxicity in rat cortex. J Neurosci Res 66:790–794
Cureton EL, Kwan RO, Dozier KC, Sadjadi J, Pal JD, Victorino GP (2010) A different view of lactate in trauma patients: protecting the injured brain. J Surg Res 159:468–473. https://doi.org/10.1016/j.jss.2009.04.020
Rice AC, Zsoldos R, Chen T, Wilson MS, Alessandri B, Hamm RJ et al (2002) Lactate administration attenuates cognitive deficits following traumatic brain injury. Brain Res 928:156–159
Suzuki A, Stern SA, Bozdagi O, Huntley GW, Walker RH, Magistretti PJ, Alberini CM (2011) Astrocyte-neuron lactate transport is required for long-term memory formation. Cell 144:810–823. https://doi.org/10.1016/j.cell.2011.02.018
Magistretti PJ, Allaman I (2018) Lactate in the brain: from metabolic end-product to signalling molecule. Nat Rev Neurosci 19:235–249. https://doi.org/10.1038/nrn.2018.19
Taher M, Leen WG, Wevers RA, Willemsen MA (2016) Lactate and its many faces. Eur J Paediatr Neurol 20:3–10. https://doi.org/10.1016/j.ejpn.2015.09.008
Dienel GA (2012) Brain lactate metabolism: the discoveries and the controversies. J Cereb Blood Flow Metab 32:1107–1138. https://doi.org/10.1038/jcbfm.2011.175
Adler AJ, Southwick RE (1992) Distribution of glucose and lactate in the interphotoreceptor matrix. Ophthalmic Res 24:243–252
Wang L, Törnquist P, Bill A (1997) Glucose metabolism in pig outer retina in light and darkness. Acta Physiol Scand 160:75–81. https://doi.org/10.1046/j.1365-201X.1997.00030.x.
Almasieh M, Wilson AM, Morquette B, Cueva Vargas JL, Di Polo A (2012) The molecular basis of retinal ganglion cell death in glaucoma. Prog Retin Eye Res 31:152–181. https://doi.org/10.1016/j.preteyeres.2011.11.002
Rodrigues EB, Urias MG, Penha FM, Badaró E, Novais E, Meirelles R, Farah ME (2015) Diabetes induces changes in neuroretina before retinal vessels: a spectral-domain optical coherence tomography study. Int J Retina Vitreous 1:4. https://doi.org/10.1186/s40942-015-0001-z
Sohn EH, van Dijk HW, Jiao C, Kok PHB, Jeong W, Demirkaya N et al (2016) Retinal neurodegeneration may precede microvascular changes characteristic of diabetic retinopathy in diabetes mellitus. PNAS 113:E2655–E2664. https://doi.org/10.1073/pnas.1522014113
Kawasaki A, Otori Y, Barnstable C (2000) Müller cell protection of rat retinal ganglion cells from glutamate and nitric oxide neurotoxicity. Invest Ophthalmol Vis Sci 41:3444–3450
Skytt DM, Toft-Kehler AK, Brændstrup CT, Cejvanovic S, Gurubaran IS, Bergersen LH, Kolko M (2016) Glia-neuron interactions in the retina can be studied in cocultures of Müller cells and retinal ganglion cells. Biomed Res Int 2016:1–10. https://doi.org/10.1155/2016/1087647.
Schultz R, Krug M, Precht M, Wohl SG, Witte OW, Schmeer C (2018) Frataxin overexpression in Müller cells protects retinal ganglion cells in a mouse model of ischemia/reperfusion injury in vivo. Sci Rep 8:4846. https://doi.org/10.1038/s41598-018-22887-5
Bringmann A, Iandiev I, Pannicke T, Wurm A, Hollborn M, Wiedemann P, Osborne NN, Reichenbach A (2009) Cellular signaling and factors involved in Müller cell gliosis: neuroprotective and detrimental effects. Prog Retin Eye Res 28:423–451. https://doi.org/10.1016/j.preteyeres.2009.07.001
Bringmann A, Grosche A, Pannicke T, Reichenbach A (2013) GABA and glutamate uptake and metabolism in retinal glial (Müller) cells. Front Endocrinol (Lausanne) 4:48. https://doi.org/10.3389/fendo.2013.00048
Bringmann A, Pannicke T, Grosche J, Francke M, Wiedemann P, Skatchkov S et al (2006) Müller cells in the healthy and diseased retina. Prog Retin Eye Res 25:397–424. https://doi.org/10.1016/j.preteyeres.2006.05.003
Bringmann A, Pannicke T, Biedermann B, Francke M, Iandiev I, Grosche J, Wiedemann P, Albrecht J et al (2009) Role of retinal glial cells in neurotransmitter uptake and metabolism. Neurochem Int 54:143–160. https://doi.org/10.1016/j.neuint.2008.10.014
Bringmann A, Wiedemann P (2012) Müller glial cells in retinal disease. Ophthalmologica 227:1–19. https://doi.org/10.1159/000328979.
Winkler BS, Arnold MJ, Brassell MA, Puro DG (2000) Energy metabolism in human retinal Müller. Cell 41:3183–3190
Winkler BS, Starnes CA, Sauer MW, Firouzgan Z, Chen S-C (2004) Cultured retinal neuronal cells and Müller cells both show net production of lactate. Neurochem Int 45:311–320. https://doi.org/10.1016/j.neuint.2003.08.017
Toft-Kehler AK, Skytt DM, Svare A, Lefevere E, Van Hove I, Moons L et al (2017) Mitochondrial function in Müller cells—does it matter? Mitochondrion 36:43–51. https://doi.org/10.1016/j.mito.2017.02.002
Lindsay KJ, Du J, Sloat SR, Contreras L, Linton JD, Turner SJ et al (2014) Pyruvate kinase and aspartate-glutamate carrier distributions reveal key metabolic links between neurons and glia in retina. Proc Natl Acad Sci U S A 111:15579–15584. https://doi.org/10.1073/pnas.1412441111
Poitry-Yamate CL, Poitry S, Tsacopoulos M (1995) Lactate released by Müller glial cells is metabolized by photoreceptors from mammalian retina. J Neurosci 15:5179–5191
Winkler BS, Sauer MW, Starnes CA (2003) Modulation of the Pasteur effect in retinal cells: implications for understanding compensatory metabolic mechanisms. Exp Eye Res 76:715–723
Toft-Kehler AK, Gurubaran IS, Desler C, Rasmussen LJ, Skytt DM, Kolko M (2016) Oxidative stress-induced dysfunction of Müller cells during starvation. Invest Ophthalmol Vis Sci 57:2721–2728. https://doi.org/10.1167/iovs.16-19275
Vohra R, Gurubaran IS, Henriksen U, Bergersen LH, Rasmussen LJ, Desler C, Skytt DM, Kolko M (2017) Disturbed mitochondrial function restricts glutamate uptake in the human Müller glia cell line, MIO-M1. Mitochondrion 36:52–59. https://doi.org/10.1016/j.mito.2017.02.003.
Flammer J, Orgül S, Costa VP, Orzalesi N, Krieglstein GK, Serra LM, Renard JP, Stefánsson E (2002) The impact of ocular blood flow in glaucoma. Prog Retin Eye Res 21:359–393. https://doi.org/10.1016/S1350-9462(02)00008-3
Abegão Pinto L, Willekens K, Van Keer K, Shibesh A, Molenberghs G, Vandewalle E et al (2016) Ocular blood flow in glaucoma—the Leuven Eye Study. Acta Ophthalmol 94:592–598. https://doi.org/10.1111/aos.12962
Shiga Y, Kunikata H, Aizawa N, Kiyota N, Maiya Y, Yokoyama Y, Omodaka K, Takahashi H et al (2016) Optic nerve head blood flow, as measured by laser speckle flowgraphy, is significantly reduced in preperimetric glaucoma. Curr Eye Res 41:1447–1453. https://doi.org/10.3109/02713683.2015.1127974
Limb GA, Salt TE, Munro PMG, Moss SE, Khaw PT (2002) In vitro characterization of a spontaneously immortalized human Müller cell line (MIO-M1). Invest Ophthalmol Vis Sci 43:864–869
Aldana BI, Zhang Y, Lihme MF, Bak LK, Nielsen JE, Holst B, Hyttel P, Freude KK et al (2017) Characterization of energy and neurotransmitter metabolism in cortical glutamatergic neurons derived from human induced pluripotent stem cells: a novel approach to study metabolism in human neurons. Neurochem Int 106:48–61. https://doi.org/10.1016/j.neuint.2017.02.010
Toft-Kehler AK, Skytt DM, Poulsen KA, Brændstrup CT, Gegelashvili G, Waagepetersen H, Kolko M (2014) Limited energy supply in Müller cells alters glutamate uptake. Neurochem Res 39:941–949. https://doi.org/10.1007/s11064-014-1289-z
Waagepetersen HS, Bakken IJ, Larsson OM, Sonnewald U, Schousboe A (1998) Comparison of lactate and glucose metabolism in cultured neocortical neurons and astrocytes using 13C-NMR spectroscopy. Dev Neurosci 20:310–320
Bak LK, Walls AB (2018) CrossTalk opposing view: lack of evidence supporting an astrocyte-to-neuron lactate shuttle coupling neuronal activity to glucose utilisation in the brain. J Physiol Lond 596:351–353. https://doi.org/10.1113/JP274945
Wang L, Kondo M, Bill A (1997) Glucose metabolism in cat outer retina. Effects of light and hyperoxia. Invest Ophthalmol Vis Sci 38:48–55
Brown AM, Wender R, Ransom BR (2001) Metabolic substrates other than glucose support axon function in central white matter. J Neurosci Res 66:839–843. https://doi.org/10.1002/jnr.10081
Chidlow G, Wood JPM, Graham M, Osborne NN (2005) Expression of monocarboxylate transporters in rat ocular tissues. Am J Physiol, Cell Physiol 288:C416–C428. https://doi.org/10.1152/ajpcell.00037.2004
Kolko M, Vosborg F, Henriksen UL, Hasan-Olive MM, Diget EH, Vohra R, Gurubaran IRS, Gjedde A et al (2016) Lactate transport and receptor actions in retina: potential roles in retinal function and disease. Neurochem Res 41:1229–1236. https://doi.org/10.1007/s11064-015-1792-x
Roland CL, Arumugam T, Deng D, Liu SH, Philip B, Gomez S, Burns WR, Ramachandran V et al (2014) Cell surface lactate receptor GPR81 is crucial for cancer cell survival. Cancer Res 74:5301–5310. https://doi.org/10.1158/0008-5472.CAN-14-0319
Rinholm JE, Hamilton NB, Kessaris N, Richardson WD, Bergersen LH, Attwell D (2011) Regulation of oligodendrocyte development and myelination by glucose and lactate. J Neurosci 31:538–548. https://doi.org/10.1523/JNEUROSCI.3516-10.2011
Frenzel J, Richter J, Eschrich K (2005) Pyruvate protects glucose-deprived Müller cells from nitric oxide-induced oxidative stress by radical scavenging. Glia 52:276–288. https://doi.org/10.1002/glia.20244
Poole RC, Cranmer SL, Halestrap AP, Levi AJ (1990) Substrate and inhibitor specificity of monocarboxylate transport into heart cells and erythrocytes. Further evidence for the existence of two distinct carriers. Biochem J 269:827–829
Wang X, Poole RC, Halestrap AP, Levi AJ (1993) Characterization of the inhibition by stilbene disulphonates and phloretin of lactate and pyruvate transport into rat and guinea-pig cardiac myocytes suggests the presence of two kinetically distinct carriers in heart cells. Biochem J 290(Pt 1):249–258
Smith D, Pernet A, Hallett WA, Bingham E, Marsden PK, Amiel SA (2003) Lactate: a preferred fuel for human brain metabolism in vivo. J Cereb Blood Flow Metab 23:658–664. https://doi.org/10.1097/01.WCB.0000063991.19746.11
Bouzier-Sore A-K, Voisin P, Canioni P, Magistretti PJ, Pellerin L (2003) Lactate is a preferential oxidative energy substrate over glucose for neurons in culture. J Cereb Blood Flow Metab 23:1298–1306. https://doi.org/10.1097/01.WCB.0000091761.61714.25
Bergersen LH (2007) Is lactate food for neurons? Comparison of monocarboxylate transporter subtypes in brain and muscle. Neuroscience 145:11–19. https://doi.org/10.1016/j.neuroscience.2006.11.062
van Hall G, Strømstad M, Rasmussen P, Jans O, Zaar M, Gam C et al (2009) Blood lactate is an important energy source for the human brain. J Cereb Blood Flow Metab 29:1121–1129. https://doi.org/10.1038/jcbfm.2009.35
Hertz L, Peng L, Dienel GA (2007) Energy metabolism in astrocytes: high rate of oxidative metabolism and spatiotemporal dependence on glycolysis/glycogenolysis. J Cereb Blood Flow Metab 27:219–249. https://doi.org/10.1038/sj.jcbfm.9600343
Toft-Kehler AK, Skytt DM, Kolko M (2017) A perspective on the Müller cell-neuron metabolic partnership in the inner retina. Mol Neurobiol. https://doi.org/10.1007/s12035-017-0760-7
Johnson NF (1977) Retinal glycogen content during ischaemia. Albrecht Von Graefes Arch Klin Exp Ophthalmol 203:271–282
Goldman SS (1990) Evidence that the gluconeogenic pathway is confined to an enriched Müller cell fraction derived from the amphibian retina. Exp Eye Res 50:213–218
Pfeiffer-Guglielmi B, Francke M, Reichenbach A, Fleckenstein B, Jung G, Hamprecht B (2005) Glycogen phosphorylase isozyme pattern in mammalian retinal Müller (glial) cells and in astrocytes of retina and optic nerve. Glia 49:84–95. https://doi.org/10.1002/glia.20102
Swanson RA (1992) Astrocyte glutamate uptake during chemical hypoxia in vitro. Neurosci Lett 147:143–146
Swanson RA, Chen J, Graham SH (1994) Glucose can fuel glutamate uptake in ischemic brain. J Cereb Blood Flow Metab 14:1–6. https://doi.org/10.1038/jcbfm.1994.1
Acknowledgements
The authors thank Laboratory Technician Charlotte Taul Brændstrup for skillful assistance to the study. The study was supported by the Michaelsen Foundation, the Velux Foundation, Denmark and Fight for Sight, Denmark.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Vohra, R., Aldana, B.I., Skytt, D.M. et al. Essential Roles of Lactate in Müller Cell Survival and Function. Mol Neurobiol 55, 9108–9121 (2018). https://doi.org/10.1007/s12035-018-1056-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-018-1056-2