Abstract
Purpose of Review
Headaches are not only responsible for restrictions in everyday life in adults. In children and adolescents, regular headaches lead also to reduced life quality and limitations in the social sphere, in school education, and in professional careers. Here, we provide an overview on the frequency of headache in children and adolescents with the aim of increasing awareness about this particular health issue.
Recent Findings
Overall, headache prevalence in children and adolescents has been increasing in recent years. From various regions worldwide, data describing headache, its forms, and consequences are growing. In addition, factors frequently correlated with headache are repeatedly investigated and named: besides genetic factors, psychosocial and behavioral factors are linked to the prevalence of headache.
Summary
Increasing evidence indicates that headache is underestimated as a common disorder in children and adolescents. Accordingly, too little emphasis is placed by society on its prevention and treatment. Thus, the extent of the social and health economic burden of frequent headaches in children and adolescents needs to be better illustrated, worldwide. Furthermore, the data collected in this review should support the efforts to improve outpatient therapy paths for young headache patients. Factors correlating with headache in pupils can draw our attention to unmet needs of these patients and allow physicians to derive important therapy contents from this data.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Population-based studies in the European Union (EU) have shown an overall 1-year prevalence of 79% for headache disorders. Headache disorders are ranked as the second most common cause of years of life spent with disability worldwide [1••]. In the EU, headache disorders cost national economies well over 100 billion euros annually [2].
Headaches are the most common type of pain in children and young people with effects on health-related quality of life (HrQoL), school attendance, social functioning [3]. In the global burden of disease study 2016, migraine was ranked first as the most disabling disease in the 15–49 age group [4••].
Until today, the consequences of frequent headaches in children are poorly characterized and early detection and treatment of young headache patients is too rare. Care structures for children and adolescents with regular headaches are not adapted to the needs. Due to lack of or late treatment, the impairments caused by headache change the lives of young people. However, several studies in the last years have addressed the question of increasing prevalence of pediatric and juvenile headache. Here, we summarize the available data to draw a picture of the landscape and upcoming health care topics.
Search Strategy and Results
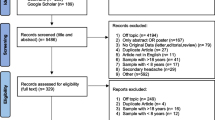
A PubMed search with the terms “epidemiology, prevalence, pediatric/children/adolescents and headache, migraine” has been carried out for publications with dates between 2015 and 2020. Original articles investigating the epidemiology of headache in children and adolescents have been included.
Methods to Study Headache Prevalence in Children and Adolescents
Compared with studies in adults, the number of epidemiological studies on headache in children and adolescents is smaller and includes fewer countries worldwide. In addition, significant methodological differences between individual epidemiological studies limit their comparability. As concluded by an expert consensus group, epidemiological studies in children and adolescents should use a cross-sectional design with school-based samples and questionnaires which specify the investigated age group, collect detailed information, and require restricted time to be completed [5].
An example of such validated tools is the child and adolescent Headache-Attributed Restriction, Disability, and Social Handicap and Impaired Participation (HARDSHIP) structured questionnaire for mediated group self-administration by pupils at school. Most studies relied for data on socio-familial factors, headache characteristics, impact on daily activities, and medication on anonymous multiple-choice questionnaires [3, 6]. Comparison between data quality of structured interviews and prospective diary recordings revealed consistency for recording headache prevalence but inconsistency for reporting “free of headache”. In particular, 50% of adolescents who reported in structured interview no headache, were headache positive in prospective diaries [7•]. This is an indication that minor headaches play a minor role in the perception of many young people and that the number of adolescents with headache is likely underestimated in data derived from structured interviews.
To assess the impact of headache in children and adolescents, validated questionnaires such as the pediatric version of the migraine disability assessment score (PedMIDAS) has been found to be appropriate for epidemiological studies. Notably, PedMIDAS requires responses in numbers of days with headache in the preceding 3 months, but has also some limitations, such as its underestimation of the impact of migraine on non-school days and a reduced recall accuracy compared with a headache diary [8, 9]. KINDL® is another validated questionnaire which scores headache on a 4-point Likert scale and inquires in the preceding 4 weeks about health-related quality of life and the impact of diseases on it in patients < 18-year old (https://www.kindl.org/english/). The pediatric pain disability index is used primarily in chronic juvenile pain patients to assess the burden of pain in everyday life and might be less effective in assessing disability due to episodic headache [10]. Considering data deviation by recall in epidemiological headache studies, the question of whether a headache occurred yesterday can be very useful to reduce the recall bias.
Recent Studies on Headache Prevalence
Headache in children and adolescents is a growing medical but also social task. This is supported on the one hand by the increasing use of medical facilities by children and adolescents with headaches in recent years, as shown in data from South Korea, Italy, and the USA [11,12,13]. On the other hand, various studies have investigated headache prevalence, mostly in school-based cross-sectional studies, with the conclusion that there is a high prevalence of headache in children and adolescents globally (Fig. 1, Table 1).
Starting with Europe, a recent study from Austria found in a representative sample of 3386 pupils aged 10–18 years an overall 1-year headache prevalence of 75.7% (girls: 82.1%; boys: 67.7%) and increasing with age [3]. In addition, this study reported on headache types and differentiated a prevalence of 24.2% migraine, 21.6% tension type headache (TTH), 3.0% chronic headache on ≥ 15 days per month, and undifferentiated headache in 26.1%. Restrictions in daily life occurred in 42% of young people with headache and health-related quality of life was reduced in almost all children and adolescents with headache. Of the pupils with headache, 50% used medication for it—a prevalence which increased to 67% in those with chronic headache. Interestingly, pupils from single parent or patchwork families exhibited a higher probability of migraine (OR 1.5).
A current cross-sectional study from Spain investigated 1619 students of 12–18 years using an anonymous questionnaire [14]. The prevalence of recurrent headache was 30.5%, with 11.3% of probands showing migraine features; 32.9% of the subjects reported at least one headache episode per week, while 44.1% of them suffered from headache-related disabilities as measured by PedMIDAS. Headache was more frequent among girls (35.1%) than in boys (25.5%), in those who had a poorer sleep hygiene, less physical activity, skipped breakfast, smoked, or with frequent caffeine consumption. Chronic pain disorders, mental health problems, and allergies were also found to be significantly associated with headache.
A recently study of our group in Germany investigated headache prevalence in pupils aged 6 to 19 years using anonymous questionnaires and concluded that the majority of pupils suffer from headache at least once a month [15]. Of 2706 children and adolescents, 36.6% indicated headache once a month and 31.5% at least 2 headache days per month within the last 3 months. Headache correlated positively with increasing age, female gender, additional diseases, drug intake on a regular basis, analgesic ingestion for other diseases, caffeine consumption, and lack of sports. Headache and secondary school type showed a tight relationship: 67.2% of the pupils attending 8-year secondary schools (resulting in university entrance level II certificates as precondition for university studies) and 79.5% of those attending 6-year secondary schools (resulting in level I certificates, preparing for general professional training) reported headache. In addition, strong correlations were revealed between headache frequency and school absence and between headache intensity and headache frequency. Among pupils with headache ≥ 2 days a month, 48.1% indicated the intake of analgesics, with ibuprofen (49.1%) and paracetamol (32.8%) being the most frequently used. Moreover, 68.3% of the pupils in this group did not report a specific headache diagnosis.
Additional data from Germany collected through a phone shear survey in > 11,000 participants between 3 and 17 years indicated that in 11- to 17-year-old pupils, recurrent headaches were the leading cause of pain and affected almost every second girl and about every third boy [16]. The 3-month prevalence of recurrent headache, abdominal, and back pain increased in the last years especially in the age groups 7 to 10 years and 11 to 13 years. Teenagers assumed analgesics for repeated headaches almost twice as often compared with children of younger age.
A third German study investigated 1399 students aged 12–19 years with primary headache in the last 6 months for daily living activities, medical care utilization, and drug use. Overall impaired daily activities were predominant in adolescents with migraine. During the past year, only 12% of pupils with headache frequented a physician and approximately 30% were consuming analgesics for headache [31].
A nationwide Italian study using self-reported data from 13,611 15-year-old adolescents reported recurrent headache in almost 45% of the population [17]. In addition, > 30% reported recurrent backpain and 30% abdominal pain. Pain and analgesic consumption were higher in girls and adolescents. Adolescents with recurrent pain consumed analgesics more frequently for other health problems than for pain. Another recent survey in 1950 Italian adolescents of 11 to 16 years used anonymous multiple-choice questionnaires and reported an overall headache prevalence of 65.9%. Of those 9.8% reported headache > 1/week, 14.3% > 1/month, 24.2% monthly, and 17.7% < once a month. Analgesic intake was reported in 69.2% of adolescents, while only 20.6% had a physician’s prescription [6]. School was perceived as the major triggering factor in 67% and girls were more affected in daily life by headache than boys.
In Croatia, 1876 high school students completed a self-administered 36-item questionnaire [18]. Here, the prevalence of migraine was 12.8% (17% in girls and 8.1% in boys), of tension-type headache (TTH) 38.3% (40.6% in girls and 35.7% in boys). Students with migraine reported more analgesic intake, health care use, and smoking.
The prevalence and disability of headache among Norwegian adolescents have been investigated in a cross-sectional school-based study with 493 adolescents aged 12–18 years [19]. The overall 1-year headache prevalence was 88%, the point prevalence 38%. In detail, 1-year headache prevalence of definite migraine was 23%, of probable migraine 13% of TTH 58%, while in 9%, more than one headache type could be diagnosed. For Norway, additional data based on successive, cross-sectional, population-based studies report an increase in all types of recurrent headaches and a significant increase in TTH among adolescents [20•].
In Denmark, the correlation of economic inequality and frequent headache was investigated in 31,102 adolescents of 11 to 15 years between 1991 and 2014 [22]. Overall, 10.4% of adolescents reported frequent headache. A significant increase between 1991 and 2014, 8% versus 12.9%, respectively, was noticed in all economic classes. Lower socio-economic conditions correlated with higher prevalence of frequent headache (OR = 1.50, 95% CI: 1.34–1.67)—this phenomenon did not change over time.
A school-based questionnaire was administered to investigate 7088 pupils aged 6–17-year old in different regions of Turkey [23]. The overall 1-year prevalence of headache was estimated to be 68.8%. In detail, 29.2% reported undifferentiated headache, 26.7% migraine, and 12.9% TTH. Burden of headache was higher and quality of life lower in pupils with migraine and TTH. Another study in Turkish 7–17-year-old pupils rated the prevalence of recurrent headache to be 47.5%. Among these subjects, 21% suffered from primary recurrent headache [24].
A Japanese school-based questionnaire survey in 3285 students of 6–15 years revealed headache in 49.4%, migraine and TTH in 3.5% and 5.4% of elementary school students, and in 5.0% and 11.2% of junior high school students, respectively [25]. Migraine resulted in concentration disturbances and headache-related frustration more often than other headaches. Fifty percent of the students with headache-related disability did not receive medical treatment.
In 2014, a study among > 7000 pupils aged 10 to 18 years in Taiwan found 85.6% of children and adolescents having pain in the last year, and among these, 63% described headache [26].
In China, a study investigated 2849 high school students for recurrent pain. A total of 30.3% of the students described headache at least once a week in the previous 3 months. Sleep disturbances and academic pressure correlated to headache and other recurrent pain [27].
In Kuwait, a study investigated 3423 6–17-year-old children and adolescents using the HARDSHIP questionnaire and reported a 1-year prevalence of headache of 19.4% (migraine 10.9%, TTH 6.2%, chronic headache 0.9%) [28]. Primary headache disorder significantly increased in the 12–17-year-age group when compared with the 6–11-year-age group (25.8% vs. 10.4%; p < 0.001). One-year primary headache prevalence showed non-significant gender differences (10.1% in boys vs. 10.6% in girls; p value < 0.79). Yet, headache prevalence was significantly higher in females than in males in the 12–17-year-age group compared with the 6–11-year-age group (38.1% vs. 15.8%).
In 2017, a questionnaire study in Jordania among students aged 16–18 years reported an overall headache frequency of 2/3, among those 19.0% were classified as having TTH, 8.8% migraine, and 39.0% undifferentiated headache [29]. This study points to headache as one of the major public health problems among high school students and calls for new therapies.
In Nigeria of 1500 students aged 20.9 ± 3.1 years, 23.7% reported headache in the past year, and 3.5% chronic headache [30]. In detail, 12.5% had TTH, 2.4% migraine, 8.9% undifferentiated headache, and none of them had medical consultation for the headache.
In Brasil, 954 adolescents (14 to 19 years) have been studied for headache and use of computer and videogames [32]. Among them, 80.6% reported headache, including 17.9% with TTH, 19.3% with migraine, and 43.4% with undifferentiated headache. The excessive use of electronic devices was a major risk factor (OR = 1.21) for headache, and especially for migraine.
Headache and Education
Regular headache leads to frequently missed school lessons, dropping out of school with poorer learning outcomes. Some patients have to repeat a school grade, or change the type of school toward a less qualified degree. As a consequence, the whole educational path can be negatively affected by headaches in childhood and adolescence.
In Israel, 262 children with headache between 5 and 18 years old have been investigated for learning disabilities [33]. Comparing children with migraine and those with both, migraine and TTH it turned out that in pupils with migraine and TTH the likelihood of learning disabilities was 2.7 times higher than in patients with migraine alone.
A Swedish investigation in 9th grade adolescents reported significantly lower school grades among those with headache or abdominal pain [34]. The relevant conclusion was that identification and treatment of pain symptoms may improve academic results.
A recent study investigated children aged 5 to 17 years in the US for the correlation between prevalent headache and school absenteeism. Frequency of severe headache in the previous 12 months was reported by caregivers in 6% of the investigated 57,272 children [35]. Interestingly, headache became more associated with school absenteeism over time.
Another North-American survey studied anonymously sleep, school performance, headache, and messaging habits in high school students [36•]. A correlation between hypersomnolence, chronic headaches and less sleep was shown, albeit not in students in lower school grades.
The relationship between school start time and headache frequency was investigated in a cross-sectional study of US high schoolers with migraine. A comparison between those who started school at 8:30 AM or later and those with earlier start time schools was carried out and reported no effect of school start time on headache days per month [37].
A Brazilian study in 195 elementary school students aged 10 to 15 years could clearly correlate severe headache and migraine with lower quality of life and lower academic performance [38].
Conclusions
Headache disorders in children and adolescents affect frequently school and social activities and the work performance of the parents. Awareness of early diagnosis and preventive therapies must improve to prevent chronic headaches and its negative impact on performance at school and in the social context. The data summarized in this review highlight the need for improved management and prevention of headaches in children and adolescents.
Excursion to the Practice I: Headache Diagnoses in Children and Adolescents
The primary task for pediatricians taking care of children and adolescents with headaches is to exclude a secondary headache. After a symptomatic headache has been clinically excluded with diagnostic methods such as cranial MRI and lumbar puncture, headache is often no longer addressed as a disorder of the young patient. Therefore, pediatric patients often suffer for months or years before receiving adequate treatment by a pediatrician, neurologist, or pain therapist specialized in headache.
At the beginning of a structured therapy, headaches should be classified as being either primary or secondary following the International Classification of Headache Disease 3rd version 2018 [39]. Red flags as fever, trauma, occipital headaches, suddenly raising headaches, or abnormalities in neurological examination point to underlying diseases such as meningitis, sinus venous thrombosis, intracerebral/subarachnoidal/epi- or subdural hemorrhage, brain tumor, stroke, intracranial hypertension or cerebrospinal fluid (CSF) leak, which all lead to secondary headaches. These secondary causes for headache have to be ruled out with appropriate diagnostic investigations [40].
Primary headaches in childhood and adolescence are most frequently TTH or migraine. In pediatric patients, migraine and TTH occur often together and the clinical presentation shows a mixture of both [41].
TTH is mostly bilateral, characterized by a dull, oppressive pain, up to medium intensity, ranging over a time of 30 min to 7 days, sometimes with photo/phonophobia, improvement by distraction, not worsening by physical activity and sometimes accompanied by increased cervical and pericranial musculature tone increase.
Migraine appears as uni- or bilateral, sharp, pulsating or dull, oppressive pain, up to high intensity, ranging over a time period of 60 min to 72 h (including sleep), mostly with photo/phonophobia, osmophobia, and vegetative syndromes such as nausea and vomiting, improvement by retreating in a dark room and sleep, worsening by physical activity, without any explainable other reason [42]. TTH and migraine are mostly episodic (less than 15 headache days a month), rarely chronic with more than 15 headache days and in chronic migraine at least 8 migraine days per month. Migraine can appear without or with aura symptoms, in the latter case complicated by neurological findings including hypoaesthesia with a migrating aspect (e.g., starting at the finger, involving elbow and tongue) or positive scotoma.
Trigeminal autonomous headaches are very rare in children and adolescents, while other primary headaches such as new daily persistent headache (persistent headache which started at a defined time point with a permanent persistent headache often with high migraine-like intensity) have so far been little studied [43•, 44].
At the beginning of treatment, proper classification of the headache is of critical importance. After secondary headaches have been excluded, patient and family education for the individual headache is the basis for further therapeutic work. In particular, the physician should explain how to treat the headache and what the child or adolescent and the family can do themselves.
Excursion to the Practice II: Headache Management in Children and Adolescents
Therapy for headaches consists out of three pillars: activation, relaxation, and medication. Dependent on the individual headache diagnosis and disease stage, the therapeutic approaches are different.
Acute Medication
The recommended medications are ibuprofen or acetaminophen. These should be used in a body weigh adjusted manner (10 mg/kg/BW for ibuprofen, 15 mg/kg/BW for acetaminophen) early during migraine attacks (hit hard and early), other NSAIDs (e.g., naproxen) are alternatives. Adolescent migraine patients can profit from combined medications such as acetaminophen, acetyl salicylic acid, and caffeine during headache episode.
Triptanes can be prescribed from the age of 12-year old, although specialists may use triptans in younger patients if needed. The starting triptane is 10 mg sumatriptan as nasal application < 30 kg BW, and 20 mg >30 kg BW. Alternatively, zolmitriptan is available as nasal spray [45].
The take home message for pediatric patients is to follow the “3 to 10” rule. This means, do not use acute headache medication more than 3 successive days and not more than 10 days per month. All acute medications can lead to analgesic induced headache, if ingested for more than 10 days a month. If nausea and vomiting are frequent, nasal, sublingual, rectal, or subcutaneous application forms of triptans are indicated and in addition the use of antiemetics, i.e., dimenhydrinate or domperidone should be considered.
Prophylactic Medication
None of the prophylactics used in adults have shown reliable effects in high quality RCTs in children and adolescents, likely due to placebo effects in young patients. Nevertheless, prophylactic drugs in young migraine patients such as flunarizine, metoprolol, amitriptyline, topiramate should be considered, if all non-medication therapies do not decrease the migraine frequency and individual disease load is high. Importantly, when using these drugs information and education of the patient and of the parents is needed as well as a close clinical follow-up [46, 47]. Magnesium as nutritional supplement represents an alternative prophylactic, which should be used 10 mg/kg/BW per day. A side effect of this supplementation can be bowel irritation, in this case a dose reduction is recommended.
Activation as headache prophylaxis includes regular sport twice a week, best in a group of peers, with the aim of enjoying movements in a non-competitive setting.
Relaxation includes regular day structure and daily break of 10 min, which should be accompanied by relaxation techniques such as “safe area imagination” or breathing techniques. It is important though to comfort the child or adolescent, such that they do not feel compelled to reach high goals, and in so doing mitigate the risk of further migraine episodes [48]. Besides improvement of headache scores, studies show that cognitive behavioral therapy can lead to functional changes in brain function being beneficial for migraine therapy [49•]. These techniques should be accompanied by teaching of the parents on how to handle the headache situation [50].
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
•• Saylor D, Steiner TJ. The global burden of headache. Semin Neurol. 2018;38(2):182–90 This paper presents a worldwide overview of burden of headache.
Linde M, Gustavsson A, Stovner LJ, Steiner TJ, Barré J, Katsarava Z, et al. The cost of headache disorders in Europe: the Eurolight project. Eur J Neurol. 2012;19:703–11.
Philipp J, Zeiler M, Wöber C, Wagner G, Karwautz AFK, Steiner TJ, et al. Prevalence and burden of headache in children and adolescents in Austria - a nationwide study in a representative sample of pupils aged 10–18 years. J Headache Pain. 2019;20(1):101.
•• Vos T, Abajobir AA, Abbafati C, Abbas KM, Abate KH, Abd-Allah F, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: a systematic analysis for the global burden of disease study 2016. Lancet. 2017;390:1211–59 This paper shows the burden of headache in relation to other diseases worldwide.
Stovner LJ, Jumah MA, Birbeck GL, Gururaj G, Jensen R, Katsarava Z, et al. The methodology of population surveys of headache prevalence, burden and cost: principles and recommendations from the global campaign against headache. J Headache Pain. 2014;15(1):5.
Foiadelli T, Piccorossi A, Sacchi L, De Amici M, Tucci M, Brambilla I, et al. Clinical characteristics of headache in Italian adolescents aged 11-16 years: a cross-sectional questionnaire school-based study. Ital J Pediatr. 2018;44(1):44.
• Krogh AB, Larsson B, Salvesen Ø, Linde M. Assessment of headache characteristics in a general adolescent population: a comparison between retrospective interviews and prospective diary recordings. J Headache Pain. 2016;17:14 This paper includes a thorough discussion on methodology.
Heyer GL, Merison K, Rose SC, Perkins SQ, Lee JM, Stewart WC. PedMIDAS-based scoring underestimates migraine disability on non-school days. Headache. 2014;54(6):1048–53.
Heyer GL, Perkins SQ, Rose SC, Aylward SC, Lee JM. Comparing patient and parent recall of 90-day and 30-day migraine disability using elements of the PedMIDAS and an Internet headache diary. Cephalalgia. 2014;34:298–306.
Stahlschmidt L, Friedrich Y, Zernikow B, Wager. Assessment of pain-related disability in pediatric chronic pain: a comparison of the functional disability inventory and the pediatric pain disability index. Clin J Pain. 2018;34(12):1173–9.
Jeong YJ, Lee YT, Lee IG, Han JY. Primary headaches in children and adolescents - experiences at a single headache Center in Korea. BMC Neurol. 2018;18(1):70.
Vetri L, Messina LM, Drago F, D'Aiuto F, Vanadia F, Brighina F, et al. Are paediatric headaches in the emergency department increasing? An Italian Experience. Funct Neurol. 2019;34(3):188–95.
Perry MC, Yaeger SK, Toto RL, Suresh S, Hickey RW. A modern epidemic: increasing pediatric emergency department visits and admissions for headache. Pediatr Neurol. 2018;89:19–25.
Torres-Ferrus M, Vila-Sala C, Quintana M, Ajanovic S, Gallardo VJ, Gomez JB, et al. Headache, comorbidities and lifestyle in an adolescent population (the TEENs study). Cephalalgia. 2019;39(1):91–9.
Nieswand V, Richter M, Berner R, von der Hagen M, Klimova A, Roeder I, et al. The prevalence of headache in German pupils of different ages and school types. Cephalalgia. 2019;39(8):1030–40.
Krause L, Sarganas G, Thamm R, Neuhauser H. Headache, abdominal and back pain in children and adolescents in Germany: results from KiGGS wave 2 and trends. Bundesgesundheitsblatt Gesundheitsforschung Gesundheitsschutz. 2019;62(10):1184–94.
Centauri F, Pammolli A, Simi R, Dalmasso P, Berchialla P, Borraccino A, et al. Self-reported recurrent pain and medicine use among 15-year-olds: results from the HBSC Italian study. J Prev Med Hyg. 2019;60(4):E368–75.
Sedlic M, Mahovic D, Kruzliak P. Epidemiology of primary headaches among 1,876 adolescents: a cross-sectional survey. Pain Med. 2016;17(2):353–9.
Krogh AB, Larsson B, Linde M. Prevalence and disability of headache among Norwegian adolescents: a cross-sectional school-based study. Cephalalgia. 2015;35(13):1181–91.
• Jacobsena BA, Dyb G, Hagen K, Stovner L, Holmen TL, Zwart JA. The Nord-Trøndelag Health Study shows increased prevalence of primary recurrent headaches among adolescents over a four-year period. Scand J Pain. 2018;2(3):148–52 Investigates the trend of headache prevalence.
Roberts C, Freeman J, Samdal O, Schnohr CW, de Looze ME, Gabhainn SN, et al. The Health Behaviour in School-aged Children (HBSC) study: methodological developments and current tensions. Int J Public Health. 2009;54(Suppl 2):140–50.
Holstein BE, Andersen A, Denbaek AM, Johansen A, Michelsen SI, Due P. Short communication: persistent socio-economic inequality in frequent headache among Danish adolescents from 1991 to 2014. Eur J Pain. 2018;22(5):935–40.
Wöber C, Wöber-Bingöl Ç, Uluduz D, Aslan TS, Uygunoglu U, Tüfekçi A, et al. Undifferentiated headache: broadening the approach to headache in children and adolescents, with supporting evidence from a nationwide school-based cross-sectional survey in Turkey. J Headache Pain. 2018;19(1):18.
Poyrazoğlu HG, Kumandas S, Canpolat M, Gümüs H, Elmali F, Kara A, et al. The prevalence of migraine and tension-type headache among schoolchildren in Kayseri, Turkey: an evaluation of sensitivity and specificity using multivariate analysis. J Child Neurol. 2015;30(7):889–95.
Goto M, Yokoyama K, Nozaki Y, Itoh K, Kawamata R, Matsumoto S, et al. Characteristics of headaches in Japanese elementary and junior high school students: a school-based questionnaire survey. Brain and Development. 2017;39(9):791–8.
Miao NF, Wang TZ, Chang FC, Lee CH, Chi HY, Huang LJ, et al. Prevalence and association of pain experiences, medication literacy, and use of medication among children and adolescents in Taiwan. J Pediatr Nurs. 2019;46:e64–71.
Zhang Y, Deng G, Zhang Z, Zhou Q, Gao X, Di L, et al. A cross sectional study between the prevalence of chronic pain and academic pressure in adolescents in China (Shanghai). BMC Musculoskelet Disord. 2015;16:219.
Al-Hashel JY, Ahmed SF, Alroughani R. Prevalence and burden of primary headache disorders in Kuwaiti children and adolescents: a community based study. Front Neurol. 2019;10:793.
Al Bashtawy M, Al Qadire M, Aloush S, Tawalbeh L, Al Azzam S, Suliman M, et al. Assessment of headache among high school students in Jordan. J Sch Nurs. 2019;35(2):88–95.
Sanya EO, Desalu OO, Aderibigbe SA, Kolo PM, Mustapha AF, Adeyanju OA. Prevalence and clinical characteristics of headaches among undergraduate students in three tertiary institutions in Ilorin, Nigeria. Niger J Clin Pract. 2017;20(11):1411–6.
Albers L, Straube A, Landgraf MN, Filippopulos F, Heinen F, von Kries R. Migraine and tension type headache in adolescents at grammar school in Germany - burden of disease and health care utilization. J Headache Pain. 2015;16:534.
Xavier MK, Pitangui AC, Silva GR, Oliveira VM, Beltrão NB, Araújo RC. Prevalence of headache in adolescents and association with use of computer and videogames. Cien Saude Colet. 2015;20(11):3477–86.
Genizi J, Khourieh Matar A, Schertz M, Zelnik N, Srugo I. Pediatric mixed headache -the relationship between migraine, tension-type headache and learning disabilities - in a clinic-based sample. J Headache Pain. 2016;17:42.
Grimby-Ekman A, Åberg M, Torén K, Brisman J, Hagberg M, Kim JL. Pain could negatively affect school grades - Swedish middle school students with low school grades most affected. PLoS One. 2018;13(12):e0208435.
Pawlowski C, Buckman C, Tumin D, Smith AW, Crotty J. National trends in pediatric headache and associated functional limitations. Clin Pediatr (Phila). 2019;58(14):1502–8.
• Pecor K, Kang L, Henderson M, Yin S, Radhakrishnan V, Ming X. Sleep health, messaging, headaches, and academic performance in high school students. Brain Dev. 2016;38(6):548–53 This paper exams the correlation of media consumption and headache, sleep, academic performance in high school students.
Gelfand AA, Pavitt S, Greene K, Szperka CL, Irwin S, Grimes B, et al. High school start time and migraine frequency in high school students. Headache. 2019;59(7):1024–103.
Rocha-Filho PA, Santos PV. Headaches, quality of life, and academic performance in schoolchildren and adolescents. Headache. 2014;54(7):1194–202.
Headache Classification Committee of the International Headache Society (IHS) The International Classification of Headache Disorders, 3rd Edition. Cephalalgia. 2018; 38(1):1–211.
Kelly M, Strelzik J, Langdon R, DiSabella M. Pediatric headache: overview. Curr Opin Pediatr. 2018;30(6):748–54.
Blankenburg M, Schroth M, Braun S. Chronic headache in children and adolescents. Klin Padiatr. 2019;231(1):14–20.
Oliveira Bernardo AA, Lys Medeiros F, Sampaio Rocha-Filho PA. Osmophobia and odor-triggered headaches in children and adolescents: prevalence, associated factors, and importance in the diagnosis of migraine. Headache. 2020;60(5):954–66.
• Reidy BL, Riddle EJ, Powers SW, Slater SK, Kacperski J, Kabbouche MA, et al. Clinic-based characterization of continuous headache in children and adolescents: comparing youth with chronic migraine to those with new daily persistent headache. Cephalalgia. 2020;333102420920644. https://doi.org/10.1177/0333102420920644 Online ahead of print. Work for improving headache classification in children and adolescents.
Yamani N, Olesen J. New daily persistent headache: a systematic review on an enigmatic disorder. J Headache Pain. 2019;20(1):80.
Oskoui M, Pringsheim T, Holler-Managan Y, Potrebic S, Billinghurst L, Gloss D, et al. Practice guideline update summary: acute treatment of migraine in children and adolescents: report of the guideline development, dissemination, and implementation subcommittee of the American Academy of Neurology and the American Headache Society. Neurology. 2019;93(11):487–99.
Locher C, Kossowsky J, Koechlin H, Lan Lam T, Barthel J, Berde CB, et al. Efficacy, safety, and acceptability of pharmacologic treatments for pediatric migraine prophylaxis: a systematic review and network meta-analysis. JAMA Pediatr. 2020;174(4):341–9.
Wu X, Zhang Y, Lu M, Yu X, Ye X, Wang X, et al. The efficacy and safety of topiramate in the prevention of pediatric migraine: an update meta-analysis. Front Pediatr. 2020;8:28. https://doi.org/10.3389/fped.2020.00028 eCollection 2020.
Gelfand AA, Irwin SL. Lifestyle advice for pediatric migraine: blaming the patient, or evidence based? Semin Neurol, Semin Neurol. 2020. https://doi.org/10.1055/s-0040-1708868. Online ahead of print.
• Nahman-Averbuch H, Schneider VJ, Chamberlin LA, Kroon Van Diest AM, Peugh JL, Lee GR, et al. Alterations in brain function after cognitive behavioral therapy for migraine in children and adolescents. Headache. 2020. https://doi.org/10.1111/head.13814 Online ahead of print. This study investigates brain activation and resting-state connectivity after CBT in young migraineurs.
Caruso A, Grolnick W, Rabner J, Lebel A. Parenting, self-regulation, and treatment adherence in pediatric chronic headache: a self-determination theory perspective. J Health Psychol. 2019;1359105319884596. https://doi.org/10.1177/1359105319884596. Online ahead of print.
Funding
Open Access funding provided by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Vera Nieswand, Matthias Richter, and Gudrun Gossrau declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Childhood and Adolescent Headache
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Nieswand, V., Richter, M. & Gossrau, G. Epidemiology of Headache in Children and Adolescents—Another Type of Pandemia. Curr Pain Headache Rep 24, 62 (2020). https://doi.org/10.1007/s11916-020-00892-6
Published:
DOI: https://doi.org/10.1007/s11916-020-00892-6