Abstract
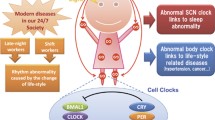
In our consumer-oriented society, in which productivity requires around-the-clock activity and demanding shift work, the biologic system that regulates our internal rhythms is being compromised. Poor sleep patterns and hectic lifestyle are detrimental to harmonious physiological and metabolic body systems, with severe impact on public health. Over a trillion peripheral cellular clocks throughout the body, supervised by the master clock located in the hypothalamic suprachiasmatic nucleus, govern most aspects of physiology and behavior. To exemplify the importance of the biologic clock for health, we have recently demonstrated that mice that are arrhythmic because of the deletion of Cry1 and Cry2 clock genes suffer from salt-sensitive hypertension. In these mice, a novel 3β-hydroxyl-steroid dehydrogenase (3β–Hsd) gene under clock control is severely overexpressed specifically in aldosterone-producing cells in the adrenal cortex, leading to hyperaldosteronism and ultimately to salt-sensitive hypertension. The human homologue of this aldosterone-producing, cell-specific enzyme was also characterized and represents a new possibility in the pathogenesis of hypertension.

Similar content being viewed by others
References
Recently published papers of interest have been highlighted as: • Of importance •• Of major importance
Hastings MH, Maywood ES, O’Neil JS: Cellular circadian pacemaking and the role of cytosolic rhythms. Curr Biol 2008, 18(17):R805-R815.
• Scheer FA, Hilton MF, Mantzoros CS, et al.: Adverse metabolic and cardiovascular consequences of circadian misalignment. Proc Natl Acad Sci U S A 2009;106(11):4453-4458. Scheer et al. applied a forced desynchrony protocol in humans and examined how the internal desynchrony between the clock and the shifted behavior affects systems involved in cardiovascular and metabolic physiology. Core body temperature was recorded continuously for 10 days to assess circadian phase. Circadian misalignment, when subjects ate and slept approximately 12 hours out of phase from their habitual times, completely reversed the daily cortisol rhythm and increased mean arterial pressure. These findings demonstrate the adverse cardiac and metabolic implications of circadian misalignment, as occurs acutely with jet lag and chronically with shift work. This paper provides evidence to support the hypothesis that circadian systems are important to cardiovascular and metabolic risk not just in mice but also in humans.
• Suwazono Y, Dochi M, Sakata K, et al.: Shift work is a risk factor for increased blood pressure in Japanese men: a 14-year historical cohort study. Hypertension 2008, 52(3):581-586. This is a 14-year historical cohort study on the effect of shift work on blood pressure in 3,963 day workers and 2,748 alternating-shift workers in a Japanese company. The authors reported that alternating shift work was a significant independent risk factor for an increase in blood pressure in male Japanese workers. Moreover, the effect of shift work on blood pressure was more pronounced than other well-established factors, such as age and body mass index.
Sega R, Facchetti R, Bombelli M, et al.: Prognostic values of ambulatory and home blood pressure compared with office blood pressure in the beneral population follow up results from the Pressioni Arteriose Monitorate e Loro Associazioni (PAMELA) study, Circulation 2005, 111(14):1777-1783.
Okamura H, Doi M, Fustin JM, et al.: Mammalian circadian clock system: molecular mechanisms for pharmaceutical and medical sciences. Adv Drug Deliv Rev. 2010, 62(9-10):876-884.
Yamaguchi S, Isejima H, Matsuo T, et al.: Synchronization of cellular clocks in the suprachiasmatic nucleus. Science 2003, 302(5649):255-259.
van der Horst GT, Muijtjens M, Kobayashi K et al.: Mammalian Cry1 and Cry2 are essential for maintenance of circadian rhythms. Nature 1999, 398(6728):627-630.
Okamura H, Miyake S, Sumi Y, et al.: Photic induction of mPer1 and mPer2 in Cry-deficient mice lacking a biological clock. Science 1999, 286(5449):2531-2534.
Yagita K, Tamanini F, van der Horst GTJ, et al.: Molecular mechanisms of the biological clock in cultured fibroblasts. Science 2001, 292(5515):278-292.
Denton D, Weisinger R, Mundy NI, et al.: The effect of increased salt intake on blood pressure of chimpanzees. Nature Med, 1995, 1(10), 1009-1016.
•• Doi M, Takahashi Y, Komatsu R, et al.: Salt-sensitive hypertension in circadian clock-deficient mice involves dysregulated adrenal Hsd3b6. Nat Med 2010, 16(1):67-74. Doi et al. show that mice lacking the core clock components Cry1 and Cry2 (Cry-null mice) show salt-sensitive hypertension owing to abnormally high synthesis of the mineralocorticoid aldosterone by the adrenal gland. An extensive search for the underlying cause led us to identify type VI 3β-hydroxyl-steroid dehydrogenase (Hsd3b6) as a new hypertension risk factor in mice. These data place Hsd3b6 in a pivotal position through which circadian clock malfunction is coupled with the development of hypertension. Translation of these findings to humans will require clinical examination of the human HSD3B1 gene, which we found to be functionally similar to mouse Hsd3b6.
Yamaguchi S, Mitsui S, Yan L, et al.: Role of DBP in the circadian oscillatory mechanism. Mol Cell Biol 2000, 20(13):4773-4781.
Ripperger JA, Shearman LP, Reppert SM, et al.: CLOCK, an essential pacemaker component, controls expression of the circadian transcription factor DBP. Genes Dev 2000; 14(6):679-689.
Mitsui S, Yamaguchi S, Matsuo T, et al.: Antagonistic role of E4BP4 and PAR proteins in the circadian oscillatory mechanism. Genes Dev 2001, 15(8):995-1006.
Conn JW: Presidential Addresses. Part I. Painting background. Part II. Primary aldosteronism, a new clinical syndrome. J Lab Clin Med 1955, 45(1):3-17.
Kaplan NM: Primary aldosteronism. In Kaplan’s Clinical Hypertension. Edited by Kaplan NM and Flynn JT. Philadelphia: Lippincott William & Wilkins; 2006:410-433.
Rosmond R, Chagnon M, Bouchard C, et al. Polymorphism in exon 4 of the human 3 beta-hydroxysteroid dehydrogenase type I gene (HSD3B1) and blood pressure. Biochem Biophys Res Commun 2002, 293(1):629-632.
Shimodaira M, Nakayama T, Sato N, et al. Association of HSD3B1 and HSD3B2 gene polymorphisms with essential hypertension, aldosterone level, and left ventricular structure. Eur J Endocrinol 2010, 163(4):671-680.
Gordon RD, Laragh JH, Funder JW: Low renin hypertensive states: perspectives, unsolved problems, future research. Trends Endocrinol Metab 2005, 16(3):108–113.
Funder JW: Aldosterone and Mineralocorticoid Receptors: Past, Present, and Future. Endocrinology, 2010, 151(11):5098-5102.
Masuki S, Todo T, Nakano Y, et al.: Reduced alpha-adrenoceptor responsiveness and enhanced baroreflex sensitivity in Cry-deficient mice lacking biological clock. J Physiol 2005, 566(Pt 1):213-224.
Acknowledgments
The research from our laboratory reported in this review was supported by grants from the Special Coordination Funds and a Grant-in-Aid for Scientific Research on Priority Areas from the Ministry of Education, Culture, Sports, Science and Technology of Japan, and from Health Labour Sciences Research Grant Research on Measures for Intractable Diseases from The Ministry of Health, Labour and Welfare, Japan.
Disclosure
No potential conflicts of interest relevant to this article were reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Okamura, H., Doi, M., Yamaguchi, Y. et al. Hypertension Due to Loss of Clock: Novel Insight From the Molecular Analysis of Cry1/Cry2–Deleted Mice. Curr Hypertens Rep 13, 103–108 (2011). https://doi.org/10.1007/s11906-011-0181-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11906-011-0181-3