Abstract
Background
Anxiety and depression levels are higher in obese compared to those in normal weight pregnant women. The aims of this study are to examine anxiety and depression in pregnancy following bariatric surgery and to compare with obese pregnant controls considering the dietary intake of polyunsaturated fatty acids (PUFA), folate, and vitamin B12.
Methods
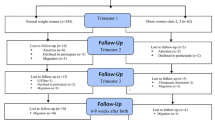
Anxiety (State-Trait Anxiety Inventory) and depression (Edinburgh Postnatal Depression Scale) were examined in the first (T1) and third (T3) pregnancy trimester in 54 women with bariatric surgery and 25 obese. T1 and T3 dietary intake of PUFA, folate, and vitamin B12 intake was assessed using a 3-day food record. Mixed models with a compound symmetry covariance structure and regression models were applied.
Results
About half of the women with surgery had high state and trait anxiety scores (≥ 40), which did not significantly change during pregnancy. Every 10-kg postoperative weight loss was associated with an increase in T1 state and trait anxiety with respectively 2.7 and 2.3 points. A smoking woman had a 8.6-point higher state anxiety score than a non-smoking woman in T1. In T3, every additional hour of sleep was associated with a decrease in trait anxiety score with 1.59 points. Anxiety and depression scores were not associated with and could not be explained by inadequate PUFAs, folate, and vitamin B12 intakes. Anxiety scores were higher following surgery than those in untreated obesity at both time points.
Conclusion
Pregnancy following bariatric surgery induces high levels of anxiety that are not associated with an inadequate maternal diet.
Similar content being viewed by others
References
Bogaerts AF, Devlieger R, Nuyts E, et al. Anxiety and depressed mood in obese pregnant women: a prospective controlled cohort study. Obes Facts. 2013;6(2):152–64. https://doi.org/10.1159/000346315.
Laraia BA, Siega-Riz AM, Dole N, et al. Pregravid weight is associated with prior dietary restraint and psychosocial factors during pregnancy. Obesity (Silver Spring). 2009;17(3):550–8. https://doi.org/10.1038/oby.2008.585.
Bodnar LM, Wisner KL, Moses-Kolko E, et al. Prepregnancy body mass index, gestational weight gain, and the likelihood of major depressive disorder during pregnancy. J Clin Psychiatry. 2009;70(9):1290–6. https://doi.org/10.4088/JCP.08m04651.
Claesson IM, Josefsson A, Sydsjö G. Prevalence of anxiety and depressive symptoms among obese pregnant and postpartum women: an intervention study. BMC Public Health. 2010;10(1):766. https://doi.org/10.1186/1471-2458-10-766.
Guelinckx I, Devlieger R, Vansant G. Reproductive outcome after bariatric surgery: a critical review. Hum Reprod Update. 2009;15(2):189–201. https://doi.org/10.1093/humupd/dmn057.
Jans G, Matthys C, Bogaerts A, et al. Maternal micronutrient deficiencies and related adverse neonatal outcomes after bariatric surgery: a systematic review. Adv Nutr. 2015;6(4):420–9. https://doi.org/10.3945/an.114.008086.
Vannevel V, Jans G, Bialecka M, et al. Internal herniation in pregnancy after gastric bypass: a systematic review. Obstet Gynecol. 2016;127(6):1013–20. https://doi.org/10.1097/AOG.0000000000001429.
Chevrot A, Lesage N, Msika S, et al. Digestive surgical complications during pregnancy following bariatric surgery: experience of a center for perinatology and obesity. J Gynecol Obstet Biol Reprod. 2016;45(4):372–9. https://doi.org/10.1016/j.jgyn.2015.04.007.
Leung BM, Kaplan BJ. Perinatal depression: prevalence, risks, and the nutrition link--a review of the literature. J Am Diet Assoc. 2009;109(9):1566–75. https://doi.org/10.1016/j.jada.2009.06.368.
Jans G, Matthys C, Bogaerts A, et al. Maternal micronutrient deficiencies and related adverse neonatal outcomes following bariatric surgery: a systematic review. Adv Nutr. 2015;6:420–9.
Jans G, Guelinckx I, Voets W, et al. Vitamin K1 monitoring in pregnancies after bariatric surgery: a prospective cohort study. Surg Obes Relat Dis. 2014;10:885–90.
Devlieger R, Guelinckx I, Jans G, et al. Micronutrient levels and supplement intake in pregnancy after bariatric surgery: a prospective cohort study. PLoS One. 2014;9(12):e114192. https://doi.org/10.1371/journal.pone.0114192.
Knight BA, Shields BM, Brook A, et al. Lower circulating B12 is associated with higher obesity and insulin resistance during pregnancy in a non-diabetic White British population. PLoS One. 2015;10(8):e0135268. https://doi.org/10.1371/journal.pone.0135268.
Guelinckx I, Devlieger R, Mullie P, et al. Effect of lifestyle intervention on dietary habits, physical activity, and gestational weight gain in obese pregnant women: a randomized controlled trial. Am J Clin Nutr. 2010;91(2):373–80. https://doi.org/10.3945/ajcn.2009.28166.
Guelinckx I, Devlieger R, Donceel P, et al. Lifestyle after bariatric surgery: a multicenter, prospective cohort study in pregnant women. Obes Surg. 2012;22(9):1456–64. https://doi.org/10.1007/s11695-012-0675-3.
Su KP, Huang SY, Chiu TH, et al. Omega-3 fatty acids for major depressive disorder during pregnancy: results from a randomized, double-blind, placebo-controlled trial. J Clin Psychiatry. 2008;69(4):644–51. https://doi.org/10.4088/JCP.v69n0418.
Chalut-Carpentier A, Pataky Z, Golay A, et al. Involvement of dietary fatty acids in multiple biological and psychological functions, in morbidly obese subjects. Obes Surg. 2015;25(6):1031–8. https://doi.org/10.1007/s11695-014-1471-z.
De Vriese SR, Matthys C, De Henauw S, et al. Maternal and umbilical fatty acid status in relation to maternal diet. Prostaglandins Leukot Essent Fat Acids. 2002;67(6):389–96. https://doi.org/10.1054/plef.2002.0446.
Jans G, Matthys C, Bel S, et al. AURORA: bariatric surgery registration in women of reproductive age—a multicenter prospective cohort study. BMC Pregnancy Childbirth. 2016;16(1):195. https://doi.org/10.1186/s12884-016-0992-y.
van der Ploeg H. Handleiding bij de Zelf-Beoordelings Vragenlijst. Een Nederlandse bewerking van Spielberger State-Trait Anxiety Inventory STAI-DY. In. Lisse, Swets & Zeitlinger B.V. Test Publishers 2000.
Spielberger C, Gorsuch R, Lushene R. StAI manual for the state-trait anxiety inventory. Palo Alto: Consulting Psychologists Press; 1970.
Grant KA, McMahon C, Austin MP. Maternal anxiety during the transition to parenthood: a prospective study. J Affect Disord. 2008;108(1-2):101–11. https://doi.org/10.1016/j.jad.2007.10.002.
Cox JL, Holden JM, Sagovsky R. Detection of postnatal depression. Development of the 10-item Edinburgh Postnatal Depression Scale. Br J Psychiatry. 1987;150(6):782–6. https://doi.org/10.1192/bjp.150.6.782.
Pop VJ, Komproe IH, van Son MJ. Characteristics of the Edinburgh Postnatal Depression Scale in The Netherlands. J Affect Disord. 1992;26(2):105–10. https://doi.org/10.1016/0165-0327(92)90041-4.
Murray L, Carothers AD. The validation of the Edinburgh Post-natal Depression Scale on a community sample. Br J Psychiatry. 1990;157(2):288–90. https://doi.org/10.1192/bjp.157.2.288.
European Food Safety Authority (EFSA). Scientific opinion on dietary reference values for cobalamin. EFSA J. 2015;13.
European Food Safety Authority (EFSA). Scientific opinion on dietary reference values for folat. EFSA J. 2014;12:3893.
Vandevijvere S, Geelen A, Gonzalez-Gross M, et al. Evaluation of food and nutrient intake assessment using concentration biomarkers in European adolescents from the Healthy Lifestyle in Europe by Nutrition in Adolescence study. Br J Nutr. 2013;109(04):736–47. https://doi.org/10.1017/S0007114512002012.
Watanabe F. Vitamin B12 sources and bioavailability. Exp Biol Med (Maywood). 2007;232(10):1266–74. https://doi.org/10.3181/0703-MR-67.
Bae S, West AA, Yan J, et al. Vitamin B-12 status differs among pregnant, lactating, and control women with equivalent nutrient intakes. J Nutr. 2015;145(7):1507–14. https://doi.org/10.3945/jn.115.210757.
Gesquiere I, Foulon V, Augustijns P, et al. Micronutrient intake, from diet and supplements, and association with status markers in pre- and post-RYGB patients. Clin Nutr. 2016;36:1175–81.
Sukumar N, Rafnsson SB, Kandala NB, et al. Prevalence of vitamin B-12 insufficiency during pregnancy and its effect on offspring birth weight: a systematic review and meta-analysis. Am J Clin Nutr. 2016;103(5):1232–51. https://doi.org/10.3945/ajcn.115.123083.
Lopresti AL, Hood SD, Drummond PD. A review of lifestyle factors that contribute to important pathways associated with major depression: diet, sleep and exercise. J Affect Disord. 2013;148(1):12–27. https://doi.org/10.1016/j.jad.2013.01.014.
Tomfohr-Madsen LM, Clayborne ZM, Rouleau CR, et al. Sleeping for two: an open-pilot study of cognitive behavioral therapy for insomnia in pregnancy. Behav Sleep Med. 2016;15:1–17.
Bayon V, Leger D, Gomez-Merino D, et al. Sleep debt and obesity. Ann Med. 2014;46(5):264–72. https://doi.org/10.3109/07853890.2014.931103.
Toor P, Kim K, Buffington CK. Sleep quality and duration before and after bariatric surgery. Obes Surg. 2012;22(6):890–5. https://doi.org/10.1007/s11695-011-0541-8.
Lee AM, Lam SK, Sze Mun Lau SM, et al. Prevalence, course, and risk factors for antenatal anxiety and depression. Obstet Gynecol. 2007;110(5):1102–12. https://doi.org/10.1097/01.AOG.0000287065.59491.70.
Teixeira C, Figueiredo B, Conde A, et al. Anxiety and depression during pregnancy in women and men. J Affect Disord. 2009;119(1-3):142–8. https://doi.org/10.1016/j.jad.2009.03.005.
Mathus-Vliegen EM. Long-term health and psychosocial outcomes from surgically induced weight loss: results obtained in patients not attending protocolled follow-up visits. Int J Obes. 2007;31(2):299–307. https://doi.org/10.1038/sj.ijo.0803404.
Mozurkewich EL, Clinton CM, Chilimigras JL, et al. The Mothers, Omega-3, and Mental Health Study: a double-blind, randomized controlled trial. Am J Obstet Gynecol. 2013;208:313.e311–9.
Acknowledgments
We would like to thank the UCLL students for their contribution in analyzing the dietary data.
Funding
RD is recipient of a postdoctoral research grant from the FWO Flanders (2010–2015).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Consent Statement
Informed consent was obtained from all individual participants included in the study.
Ethical Statement
This study was in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Jans, G., Matthys, C., Bogaerts, A. et al. Depression and Anxiety: Lack of Associations with an Inadequate Diet in a Sample of Pregnant Women with a History of Bariatric Surgery—a Multicenter Prospective Controlled Cohort Study. OBES SURG 28, 1629–1635 (2018). https://doi.org/10.1007/s11695-017-3060-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-3060-4