Abstract
Background
In bariatric surgery, there are no guidelines available for intraoperative fluid administration. Goal-directed fluid therapy (GDFT) is a new concept of perioperative fluid management that has been shown to improve the prognosis of patients undergoing abdominal surgery. The aim of our study is to assess the impact of the implementation of a GDFT protocol in morbidly obese patients who underwent laparoscopic sleeve gastrectomy (LSG).
Methods
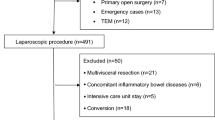
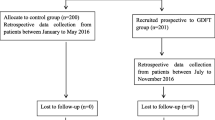
A before-after intervention study, in morbidly obese patients who underwent LSG, was conducted at the Obesity Unit of the General University Hospital Elche. Data from the GDFT implementation group (January 2014 to December 2015) were prospectively collected and compared with a preimplementation group (January 2012 to December 2013).
Results
Baseline demographic and comorbidity data between the two groups of patients were similar. The length of stay in the hospital was significantly shortened in GDFT group from 4.5 to 3.44 days (p < 0.001). Intraoperative fluid administration was significantly lower in the GDFT group (1002.4 vs 1687.2 ml in preimplementation group, p < 0.001). In the postoperative period, there was a statistically significant reduction in postoperative nausea and vomiting (PONV) after GDFT implementation (48 to 14.3 %, p < 0.001).
Conclusions
Implementation of GDFT protocols can prevent intraoperative fluid overload in patients undergoing bariatric surgery. It could improve outcomes, for example decreasing PONV or even hospital stay.

Similar content being viewed by others
References
O’Neill T, Allam J. Anesthetic considerations and management of the obese patient presenting for bariatric surgery. Curr Anaesth Crit Care. 2010;21:16–23.
Chappell D, Jecob M, Hofmann-Kiefer K, et al. A rational approach to perioperative fluid management. Anesthesiology. 2008;109(4):723–40.
Marik PE, Baram M, Vahid B. Does central venous pressure predict fluid responsiveness? A systematic review of the literature and the tale of seven mares. Chest. 2008;134(1):172–8.
Osman D, Ridel C, Ray P, et al. Cardiac filling pressures are not appropriate to predict hemodynamic response to volume challenge. Crit Care Med. 2007;35(1):64–8.
Hamilton MA, Cecconi M, Rhodes A. A systematic review and meta-analysis on the use of preemptive hemodynamic intervention to improve postoperative outcomes in moderate and high-risk surgical patients. Anesth Analg. 2011;112(6):1392–402.
Pearse RM, Harrison DA, MacDonald N, et al. Effect of a perioperative, cardiac output-guided hemodynamic therapy algorithm on outcomes following major gastrointestinal surgery: a randomized clinical trial and systematic review. JAMA. 2014;311(21):2181–90.
Corcoran T, Rhodes JE, Carke S, et al. Perioperative fluid management strategies in major surgery: a stratified meta-analysis. Anesth Analg. 2012;114(3):640–51.
Dalfino L, Giglio MT, Puntillo F, et al. Haemodynamic goal-directed therapy and postoperative infections: earlier is better. A systematic review and meta-analysis. Crit Care. 2011;15(3):R154.
Benes J, Giglio M, Brianza N, et al. The effects of goal-directed fluid therapy based on dynamic parameters on post-surgical outcome: a meta-analysis of randomized controlled trials. Crit Care. 2014;18(5):584.
Jain AK, Dutta A. Stroke volume variation as a guide to fluid administration in morbidly obese patients undergoing laparoscopic bariatric surgery. Obes Surg. 2010;20(6):709–15.
Wool DB, Lemmens HJM, Brodsky JB, et al. Intraoperative fluid replacement and postoperative creatine phosphokinase levels in laparoscopic bariatric patients. Obes Surg. 2010;20(6):698–01.
Marik PE, Cavallazzi R, Vasu T, et al. Dynamic changes in arterial waveform derived variables and fluid responsiveness in mechanically ventilated patients. A systematic review of the literature. Crit Care Med. 2009;37(9):2642–7.
Benes J, Chytra I, Altmann P, et al. Intraoperative fluid optimization using stroke volume variation in high risk surgical patients: results of prospective randomized study. Crit Care. 2010;14:R118.
Lansdorp B, Lemson J, vanPutten MJ, et al. Dynamic indices do not predict volume responsiveness in routine clinical practice. Br J Anaesth. 2012;108:395–401.
Michard F. Rational fluid management/dissecting facts from fiction. Br J Anaesth. 2012;108(3):369–71.
Salome CM, King GG, Berend N. Physiology of obesity and effects on lung function. J Appl Physiol. 2010;108(1):206–11.
Serpa Neto A, Hemmes SN, Barbas CS, et al. Protective versus conventional ventilation for surgery: a systematic review and individual patient data meta-analysis. Anesthesiology. 2015;123(1):66–78.
Fernandez-Bustamante A, Hashimoto S, Serpa Neto A, et al. Perioperative lung protective ventilation in obese patients. BMC Anesthesiol. 2015;15:56.
Starling EH. The Linacre Lecture on the Law of the Heart. London: Longmans, Green & Co; 1918.
Lobo S, Oliveira NE. Clinical review: What are the best hemodynamic targets for noncardiac surgical patients? Crit Care. 2013;17(2):210.
Kuper M, Gold SJ, Callow C, et al. Intraoperative fluid management guided by oesophageal Doppler monitoring. BMJ. 2011;342:d3016.
Noblett SE, Snowden CP, Shenton BK, et al. Randomized clinical trial assessing the effect of Doppler-optimized fluid management on outcome after elective colorectal resection. Br J Surg. 2006;93(9):1069–76.
Abbas SM, Hill AG. Systematic review of the literature for the use of oesophageal Doppler monitor for fluid replacement in major abdominal surgery. Anaesthesia. 2008;63(1):44–51.
Cecconi M, Fasano N, Langiano N, et al. Goal-directed haemodynamic therapy during elective total hip arthroplasty under regional anaesthesia. Crit Care. 2011;15(3):R132.
Vincent JL, Pelosi P, Pearse R, et al. Perioperative cardiovascular monitoring of high-risk patients: a consensus of 12. Crit Care. 2015;19:224.
Dubin A, Pozo MO, Casabella CA, et al. Comparison of 6% hydroxyethyl starch 130/0.4 and saline solution for resuscitation of the microcirculation during the early goal-directed therapy of septic patients. J Crit Care. 2010;25(4):659.
Ripolles J, Espinosa A, Casans R, et al. Colloids versus crystalloids in objective-guided fluid therapy, systematic review and meta-analysis. Too early or too late to draw conclusions. Braz J Anesthesiol. 2015;65(4):281–91.
Yates D, Davies SJ, Milner HE, et al. Crystalloid or colloid for goal-directed fluid therapy in colorectal surgery. Br J Anaesth. 2014;112(2):281–9.
Giglio MT, Marucci M, Testini M, et al. Goal-directed haemodynamic therapy and gastrointestinal complications in major surgery: a meta-analysis of randomized controlled trials. Br J Anaesth. 2009;103(5):637–46.
Gomez-Izquierdo JC, Feldman LS, Carli F, et al. Meta-analysis of the effect of goal-directed therapy on bowel function after abdominal surgery. Br J Surg. 2015;102(6):577–89.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the local ethics committee prior to conduction of the study.
Conflict of Interest
All authors declare that they have no conflict of interest.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Muñoz, J.L., Gabaldón, T., Miranda, E. et al. Goal-Directed Fluid Therapy on Laparoscopic Sleeve Gastrectomy in Morbidly Obese Patients. OBES SURG 26, 2648–2653 (2016). https://doi.org/10.1007/s11695-016-2145-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-016-2145-9