Abstract
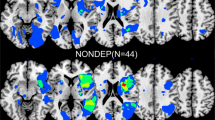
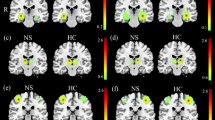
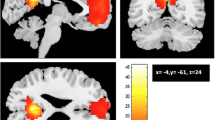
Depression and anxiety symptoms are common after stroke and associated to reduction in quality of life and poor physical and social outcomes. The Default Mode Network (DMN) plays an important role in the emotional processing. We investigated whether these symptoms are associated to a disruption of DMN functional connectivity in the first month after stroke. Thirty-four subacute ischemic stroke patients were submitted to: 1) behavioral assessment through Beck Depression Inventory (BDI), Beck Anxiety Inventory (BAI) and Structured Clinical Interview for DSM Disorders; 2) neuropsychological assessment using Mini Mental State Examination and Montreal Cognitive Assessment; 3) resting state functional magnetic resonance imaging acquisition using a 3 T scanner (Philips Achieva). Patients with depression and/or anxiety symptoms showed an increased DMN functional connectivity in left inferior parietal gyrus and left basal nuclei, when compared to stroke controls. Specific correlation between BDI/BAI scores and DMN functional connectivity indicated that depression symptoms are correlated with increased functional connectivity in left inferior parietal gyrus, while anxiety symptoms are correlated with increased functional connectivity in cerebellum, brainstem and right middle frontal gyrus. Our study provides new insights into the underlying mechanisms of post stroke depression and anxiety, suggesting an alternate explanation other than regional structural damage following ischemic event, that these psychiatric symptoms are related to brain network dysfunction.

Similar content being viewed by others
References
Andersen, G. (1997). Post-stroke depression: diagnosis and incidence. European Psychiatry, 12(3), 255–260.
Andreescu, C., Wu, M., Butters, M. A., Figurski, J., Reynolds, C. F. 3rd, Aizenstein, H. J. (2011). The default mode network in late-life anxious depression. The American Journal of Geriatric Psychiatry, 19(11), 980–983.
Astrom, M. (1996). Generalized anxiety disorder in stroke patients: a 3-year longitudinal study. Stroke, 27(2), 270–275.
Astrom, M., Adolfsson, R., & Asplund, K. (1993). Major depression in stroke patients. A 3-year longitudinal study. Stroke, 24(7), 976–982.
Barker-Collo, S. L. (2007). Depression and anxiety 3 months post stroke: prevalence and correlates. Archieves of. Clinical Neuropsychology, 22(4), 519–531.
Barkhof, F., Fox, N. C., Bastos-Leite, A. J., & Scheltens, P. (2011). Neuroimaging in dementia. Berlim: Springer-Verlag.
Beck, A. T., Ward, C. H., Mendelson, M., Mock, J., & Erbaugh, J. (1961). An inventory for measuring depression. Archives of General Psychiatry, 4, 561–571.
Beck, A. T., Epstein, N., Brown, G., & Steer, R. A. (1988). An inventory for measuring clinical anxiety: psychometric properties. Journal of Consulting and Clinical Psychology, 56(6), 893–897.
Biswal, B., Yetkin, F. Z., Haughton, V. M., & Hyde, J. S. (1995). Functional connectivity in the motor cortex of resting human brain using echo-planar MRI. Magnetic Resonance in Medicine, 34(4), 537–541.
Bostan, A. C., Dum, R. P., & Strick, P. L. (2013). Cerebellar networks with the cerebral cortex and basal ganglia. Trends in Cognitive Sciences, 17(5), 241–254.
Brott, T., Adams, H. P., Olinger, C. P., Marler, J. R., Barsan, W. G., Biller, J., et al. (1989). Measurements of acute cerebral infarction: a clinical examination scale. Stroke, 20(7), 864–870.
Burton, C. A. C., Murray, J., Holmes, J., Astin, F., Greenwood, D., & Knapp, P. (2013). Frequency of anxiety after stroke: a systematic review and meta-analysis of observational studies. International Journal of Stroke, 8(7), 545–559.
Carson, A. J., MacHale, S., Allen, K., Lawrie, S. M., Dennis, M., House, A., et al. (2000). Depression after stroke and lesion location: a systematic review. Lancet, 356(9224), 122–126.
Caulfield, M.D., Zhu, D.C., McAuley, J.D., Servatius, R.J. (2015). Individual differences in resting-state functional connectivity with the executive network: support for a cerebellar role in anxiety vulnerability. Brain structure & function
Chemerinski, E., & Robinson, R. G. (2000). The neuropsychiatric of stroke. Psychosomatics, 41(1), 5–14.
Chemerinski, E., Robinson, R. G., & Kosier, J. T. (2001). Improved recovery in activities of daily living associated with remission of poststroke depression. Stroke, 32(1), 113–117.
Chrousos, G. P. (1998). Stressors, stress, and neuroendocrine integration of the adaptive response. The 1997 Hans Selye memorial lecture. Annals of the New York Academy of. Science, 851, 311–335.
Coutinho, J.F., Fernandes, S.V., Soares, J.M., Maia, L., Gonçalves, O.F., Sampaio, A. (2015). Default mode network dissociation in depressive and anxiety states. Brain Imaging and Behavior.
Cunha, J. A. (2001). Manual da versão em português das escalas de Beck. São Paulo: Editora Casa do Psicólogo.
de Campos, B. M., Coan, A. C., Lin Yasuda, C., Casseb, R. F., & Cendes F. 2016). Large-scale brain networks are distinctly affected in right and left mesial temporal lobe epilepsy. Human Brain Mapping, 37(9), 3137–3152.
First, M. B., Spitzer, R. L., Gibbon, M., & Williams, J. B. W. (1996). Structures clinical interview for DSM-IV axis I disorders - clinician version (SCID-CV). Washington: American Psychiatric Press Inc..
Folstein, M. F., Folstein, S. E., & McHugh, P. R. (1975). Mini-mental state": a practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research, 12(3), 189–198.
Fornito, A., Zalesky, A., & Breakspear, M. (2015). The connectomics of brain disorders. Nature Reviews Neuroscience, 16(3), 159–172.
Friston, K. J., Frith, C. D., Liddle, P. F., & Frackowiak, R. S. (1993). Functional connectivity: the principal-component analysis of large (PET) data sets. Journal of Cerebral Blood Flow and Metabolism, 13(1), 5–14.
Greicius, M. D., Krasnow, B., Reiss, A. L., & Menon, V. (2003). Functional connectivity in the resting brain: a network analysis of the default mode hypothesis. Proceedings of the National Academy of Sciences of the United States of America, 100(1), 253–258.
Greicius, M. D., Flores, B. H., Menon, V., Glover, G. H., Solvason, H. B., Kenna, H., et al. (2007). Resting-state functional connectivity in major depression: abnormally increased contributions from subgenual cingulate cortex and thalamus. Biological Psychiatry, 62(5), 429–437.
Griffiths, D., & Sturm, J. (2011). Epidemiology and etiology of young stroke. Stroke research and treatment. doi:10.4061/2011/209370.
Grimm, S., Boesiger, P., Beck, J., Schuepbach, D., Bermpohl, F., Walter, M., et al. (2009a). Altered negative BOLD responses in the default-mode network during emotion processing in depressed subjects. Neuropsychopharmacology, 34(4), 932–943.
Grimm, S., Ernst, J., Boesiger, P., Schuepbach, D., Hell, D., Boeker, H., et al. (2009b). Increased self-focus in major depressive disorder is related to neural abnormalities in subcortical-cortical midline structures. Human Brain Mapping, 30(8), 2617–2627.
Habas, C. (2012). Functional imaging and the cerebellum: recent developments and challenges. Editorial. Cerebellum, 11(2), 311–313.
Hackett, M. L., Yapa, C., Parag, V., & Anderson, C. S. (2005). Frequency of depression after stroke: a systematic review of observational studies. Stroke, 36, 1330–1340.
Hermans, E. J., Henckens, M. J., Joëls, M., & Fernández, G. (2014). Dynamic adaptation of large-scale brain networks in response to acute stressors. Trends in Neurosciences, 37(6), 304–314.
Lassalle-Lagadec, S., Sibon, I., Dilharreguy, B., Renou, P., Fleury, O., & Allard, M. (2012). Subacute default mode network dysfunction in the prediction of post-stroke depression severity. Radiology, 264(1), 218–224.
Leppänen, J. M. (2006). Emotional information processing in mood disorders: a review of behavioral and neuroimaging findings. Current Opinion in Psychiatry, 19(1), 34–39.
Manoliu, A., Meng, C., Brandl, F., Doll, A., Tahmasian, M., Scherr, M., et al. (2014). Insular dysfunction within the salience network is associated with severity of symptoms and aberrant inter-network connectivity in major depressive disorder. Frontiers in Human Neuroscience. doi:10.3389/fnhum.2013.00930.
Maresh, E. L., Allen, J. P., & Coan, J. A. (2014). Increased default mode network activity in socially anxious individuals during reward processing. Biology of Mood & Anxiety Disorders. doi:10.1186/2045–5380–4–7.
McEwen, B. S. (2003). Mood disorders and allostatic load. Biological Psychiatry, 54(3), 200–207.
Menlove, L., Crayton, E., Kneebone, I., Allen-Crooks, R., Otto, E., & Harder, H. (2015). Predictors of anxiety after stroke: a systematic review of observational studies. Journal of Stroke and Cerebrovascular Diseases, 24(6), 1107–1117.
Modi, S., Kumar, M., Kumar, P., & Khushu, S. (2015). Aberrant functional connectivity of resting state networks associated with trait anxiety. Psychiatry Research. doi:10.1016/j.pscychresns.2015.07.006.
Narushima, K., & Robinson, R. G. (2003). The effect of early versus late antidepressant treatment on physical impairment associated with poststroke depression. The Journal of Nervous and Mental Disease, 191(10), 645–652.
Nasreddine, Z. S., Phillips, N. A., Bédirian, V., Charbonneau, S., Whitehead, V., Collin, I., et al. (2005). The Montreal cognitive assessment, MoCA: a brief screening tool for mild cognitive impairment. Journal of the American Geriatrics Society, 53(4), 695–699.
Northoff, G. (2013). What the brain’s intrinsic activity can tell us about consciousness? A tri-dimensional view. Neuroscience and Biobehavioral Reviews, 37(4), 726–738.
Northoff, G., Heinzel, A., de Greck, M., Bermpohl, F., Dobrowolny, H., & Panksepp, J. (2006). Self-referential processing in our brain - a meta-analysis of imaging studies on the self. NeuroImage, 31(1), 440–457.
Pan, J. H., Song, X. Y., Lee, S. Y., & Kwok, T. (2008). Longitudinal analysis of quality of life for stroke survivors using latent curve models. Stroke, 39(10), 2795–2802.
Peters, R. (2006). Ageing and the brain. Postgraduate Medical Journal, 82(964), 84–88.
Peterson, A., Thome, J., Frewen, P., & Lanius, R. A. (2014). Resting-state neuroimaging studies: a new way of identifying differences and similarities among the anxiety disorders? Canadian Journal of Psychiatry, 59(6), 294–300.
Qiu, C., Liao, W., Ding, J., Feng, Y., Zhu, C., Nie, X., et al. (2011). Regional homogeneity changes in social anxiety disorder: a resting-state fMRI study. Psychiatry Research, 194(1), 47–53.
Raichle, M. E., MacLeod, A. M., Snyder, A. Z., Powers, W. J., Gusnard, D. A., & Shulman, G. L. (2001). A default mode of brain function. Proceedings of the National Academy of Sciences of the United States of America, 98(2), 676–682.
Raison, C. L., & Miller, A. H. (2003). When not enough is too much: the role of insufficient glucocorticoid signaling in the pathophysiology of stress-related disorders. American Journal of Psychiatry, 160(9), 1554–1565.
Ramasubbu, R., Robinson, R. G., Flint, A. J., Kosier, T., & Price, T. R. (1998). Functional impairment associated with acute poststroke depression: the stroke data Bank study. The Journal of Neuropsychiatry and Clinical Neurosciences, 10(1), 26–33.
Robinson, R. G. (2006). Prevalence of depressive disorders. In R. G. Robinson (Ed.), The clinical neuropsychiatry of stroke (pp. 52–59). New York: Cambridge Univesity Press..
Sharpe, M., Hawton, K., House, A., Molyneux, A., Sandercock, P., Bamford, J., et al. (1990). Mood disorders in long-term survivors of stroke: associations with brain lesion location and volume. Psychological Medicine, 20(4), 815–828.
Sheline, Y. I., Barch, D. M., Price, J. L., Rundle, M. M., Vaishnavi, S. N., Snyder, A. Z., et al. (2009). The default mode network and self-referential process in depression. Proceedings of the National Academy of Sciences of the United States of America, 106(6), 1942–1947.
Shimoda, K., & Robinson, R. G. (1998). Effects of anxiety disorder on impairment and recovery from stroke. The Journal of Neuropsychiatry and Clinical Neuroscience, 10(1), 34–40.
Shomstein, S. (2012). Cognitive functions of the posterior parietal cortex: top-down and bottom-up attentional control. Frontiers in Integrative Neuroscience. doi:10.3389/fnint.2012.00038.
Stoodley, C. J. (2012). The cerebellum and cognition: evidence from functional imaging studies. Cerebellum, 11(2), 352–365.
van den Heuvel, M. P., & Hulshoff Pol, H. E. (2010). Exploring the brain network: a review on resting-state functional connectivity. European Neuropsychopharmacology, 20(8), 519–534.
van Swieten, J. C., Koudstall, P. J., Visser, M. C., Schouten, H. J. A., & van Gijn, J. (1988). Interobserver agreement for the assessment of handicap in stroke patients. Stroke, 19(5), 604–607.
Wagner, A. D., Shannon, B. J., Kahn, I., & Buckner, R. L. (2005). Parietal lobe contributions to episodic memory retrieval. Trends in Cognitive Sciences, 9(9), 445–453.
Wang, L., Hermens, D. F., Hickie, I. B., & Lagopoulos, J. (2012). A systematic review of resting-state functional-MRI studies in major depression. Journal of Affective Disorders, 142(1–3), 6–12.
Wei, N., Yong, W., Li, X., & Zhou, Y. (2015). Post-stroke depression and lesion location: a systematic review. Journal of Neurology, 262(1), 81–90.
Yu, L., Liu, C. K., Chen, J. W., Wang, S. Y., Wu, Y. H., & Yu, S. H. (2004). Relationship between post-stroke depression and lesion location: a meta analysis. The Kaohsiung Journal of Medical Sciences, 20(8), 372–380.
Zhang, P., Xu, Q., Dai, J., Wang, J., Zhang, N., & Luo, Y. (2014). Dysfunction of affective network in post ischemic stroke depression: a resting-state functional magnetic resonance imaging study. BioMed Research International. doi:10.1155/2014/846830.
Zhou, Y., Chunshui, Y., Zheng, H., Liu, Y., Song, M., Qin, W., et al. (2010). Increased neural resources recruitment in the intrinsic organization in major depression. Journal of Affective Disorders, 121(3), 220–230.
Zhu, X., Wang, X., Xiao, J., Liao, J., Zhong, M., Wang, W., et al. (2012). Evidence of a dissociation pattern in resting-state default mode network connectivity in first-episode, treatment-naive major depression patients. Biological Psychiatry, 71(7), 611–617.
Acknowledgments
This study is funded by Cepid-Brainn-Fapesp 2013/07559-3. Jéssica Elias Vicentini was recipient of Fapesp scholarship 2013/23183-3 and Marina Weiler is recipient of Fapesp scholarship 2015/06163-4.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Jéssica Elias Vicentini, Marina Weiler, Sara Regina Meira Almeida, Brunno Machado de Campos, Lenise Valler and Li Min Li declare that they have no conflict of interest.
Informed consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, and the applicable revisions at the time of the investigation. Informed consent was obtained from all patients for being included in the study. The study was approved by Ethics Committee number: 483.401.
Rights and permissions
About this article
Cite this article
Vicentini, J.E., Weiler, M., Almeida, S.R.M. et al. Depression and anxiety symptoms are associated to disruption of default mode network in subacute ischemic stroke. Brain Imaging and Behavior 11, 1571–1580 (2017). https://doi.org/10.1007/s11682-016-9605-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-016-9605-7