Abstract
Summary
In N = 400 women (46.9 ± 15.5 years), the prevalence of severe (< 25 nmol/l) and mild (≥ 25 and < 50 nmol/l) 25(OH)D deficiency was 7 and 32.2%, respectively, while 60.8% women had adequate status. Serum iPTH increased (> 37.0 pg/ml) when 25(OH)D was < 46.9 nmol/l. BMD was not significantly lower in the participants with iPTH > 37.0 pg/ml.
Purpose
Bone mineral density (BMD) is affected by serum 25-hydroxyvitamin D (25(OH)D) and intact parathyroid hormone (iPTH). Our objective was to analyze the association between serum 25(OH)D and iPTH and their mutual regulatory influence on BMD in women with 25(OH)D deficiency. We also attempted to establish a threshold for the serum 25(OH)D below which serum iPTH increases.
Methods
The participants were 400 generally healthy women (46.9 ± 15.5 years) recruited from local communities. BMD was measured by dual-energy X-ray absorptiometry, and serum 25(OH)D, iPTH, calcium, phosphorus, alkaline phosphatase, osteocalcin, and C-telopeptide (CTX) were analyzed from the fasting blood samples. Multivariate regression models were used to investigate the relationships among serum 25(OH)D, iPTH, and BMD.
Results
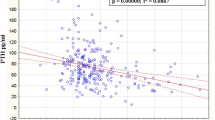
Serum iPTH increased when 25(OH)D concentrations were below 46.9 nmol/l. Severe 25(OH)D deficiency (< 25 nmol/l) was found in 7% of the participants and was associated with significantly higher iPTH compared to participants with serum 25(OH)D ≥ 25 nmol/l. BMD was negatively associated with iPTH only in the group with severe 25(OH)D deficiency. However, BMD was not significantly lower in the participants with severe 25(OH)D deficiency compared to those with mild deficiency or with adequate status.
Conclusions
Our results showed that threshold level of 25(OH)D below which iPTH started to rise was 46.9 nmol/l. There was no negative impact of iPTH on BMD or bone turnover markers in women with severe 25(OH)D deficiency. This might be due to the relatively young age of our participants in whom the unfavorable effect of 25(OH)D deficiency on bone might have not yet appeared.


Similar content being viewed by others
References
Bischoff-Ferrari HA, Giovannucci E, Willett WC, Dietrich T, Dawson-Hughes B (2006) Estimation of optimal serum concentrations of 25-hydroxyvitamin D for multiple health outcomes. Am J Clin Nutr 84:18–28 PMID: 16825677
Heaney RP (2008) Vitamin D in health and disease. Clin J Am Soc Nephrol 3:1535–1541. https://doi.org/10.2215/CJN.01160308
Dawson-Hughes B, Harris SS, Dallal GE (1997) Plasma calcidiol, season, and serum parathyroid hormone concentrations in healthy elderly men and women. Am J Clin Nutr 5:67–71 PMID: 8988915
Lips P (2004) Which circulating level of 25-hudroxyvitamin D is appropriate? J Steroid Biochem 89–90:611–614. https://doi.org/10.1016/j.jsbmb.2004.03.040
Carnevale V, Nieddu L, Romagnoli E, Battista C, Mascia ML, Chiodini I, Eller-Vainicher C, Frusciante V, Santini SA, La Porta M, Minisola S, Scillitani A (2010) Regulation of PTH secretion by 25-hydroxyvitamin D and ionized calcium depends on vitamin D status: a study in a large cohort of healthy subjects. Bone 47:626–630. https://doi.org/10.1016/j.bone.2010.06.013
Saliba W, Barnett O, Rennert HS, Lavi I, Rennert G (2011) The relationship between serum 25(OH)D and parathyroid hormone levels. Am J Med 124:1165–1170. https://doi.org/10.1016/j.amjmed.2011.07.009
Delos Reyes J, Smyth A, Griffin D, O’Shea P, O’Keeffe S, Mulkerrin EC (2017) Vitamin D deficiency and insufficiency prevalence in the west of Ireland-a retrospective study. J Nutr Health Aging 21:1107–1110. https://doi.org/10.1007/s12603-017-0889-0
Sigurdsson G, Franzson L, Steingrimsdottir L, Sigvaldason H (2000) The association between parathyroid hormone, vitamin D and bone mineral density in 70-year-old Icelandic women. Osteoporos Int 11:1031–1035. https://doi.org/10.1007/s001980070024
Vuceljic M, Ilic-Stojanovic O, Lazovic M, Grajic M (2012) Vitamin D and parathyroid hormone in relation to bone mineral density in postmenopausal women. Vojnosanit Pregl 69:243–248. https://doi.org/10.2298/VSP1203243V
Hilmi I, Sunderesvaran K, Ananda V, Sarji SA, Arumugam K, Goh KL (2013) Increased fracture risk and osteoporosis not associated with vitamin D levels in Malaysian patients with inflammatory bowel disease. J Clin Endocrinol Metab 98:2415–2421. https://doi.org/10.1210/jc.2013-1147
Ross AC, Manson JE, Abrams SA, Aloia JF, Brannon PM, Clinton SK, Durazo-Arvizu RA, Gallagher JC, Gallo RL, Jones G, Kovacs CS, Mayne ST, Rosen CJ, Shapses SA (2011) The 2011 report on dietary reference intakes for calcium and vitamin D from the Institute of Medicine: what clinicians need to know. J Clin Endocrinol Metab 96:53–58. https://doi.org/10.1210/jc.2010-2704
Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, Murad MH, Weaver CM (2011) Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 96:1911–1930. https://doi.org/10.1210/jc.2011-0385
van Schoor NM, Lips P (2011) Worldwide vitamin D status. Best Pract Res Clin Endocrinol Metab 25:671–680. https://doi.org/10.1016/j.beem.2011.06.007
Hilger J, Friedel A, Herr R, Rausch T, Roos F, Wahl DA, Pierroz DD, Weber P, Hoffmann K (2014) A systematic review of vitamin D status in populations worldwide. Br J Nutr 111:23–45. https://doi.org/10.1017/S0007114513001840
Rumbak I, Zizic V, Sokolic L, Cvijetic S, Kajfez R, Colic Baric I (2012) Bone mineral density is not associated with homocysteine level, folate and vitamin B12 status. Arch Gynecol Obstet 285:991–1000. https://doi.org/10.1007/s00404-011-2079-3
Keser I, Ilich JZ, Vrkic N, Giljevic Z, Colic Baric I (2013) Folic acid and vitamin B12 supplementation lowers plasma homocysteine but has no effect on serum bone turnover markers in elderly women: a randomized, double-blind, placebo-controlled trial. Nutr Res 33:211–219. https://doi.org/10.1016/j.nutres.2013.01.002
Colic Baric I, Satalic Z, Keser I, Cecic I, Sucic M (2009) Validation of folate food frequency questionnaire with serum and erythrocyte folate and plasma homocysteine. Int J Food Sci Nutr 60(Suppl 5):10–18. https://doi.org/10.1080/09637480802249074
Kaic-Rak A, Antonic K (1990) Food composition tables. Institute of Public Health of Croatia, Orbis, Zagreb
Institute of Medicine (US) Committee to Review Dietary Reference Intakes for Vitamin D and Calcium (2011) In: Ross AC, Taylor CL, Yaktine AL, Del Valle HB (eds) Dietary reference intakes for calcium and vitamin D. National Academies Press (US), Washington (DC) PMID: 21796828
World Health Organization (1993) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis. Report of a WHO study group. WHO tech rep Ser 843, Geneva. PMID: 7941614
Levenberg K (1944) A method for the solution of certain non-linear problems in least squares. Quart Appl Math 2:164–168. https://doi.org/10.1090/qam/10666
Marquardt D (1963) An algorithm for least-squares estimation of nonlinear parameters. SIAM J Appl Math 11:431–441. https://doi.org/10.1137/0111030
Green TJ, Skeaff CM, Rockell JEP, Venn BJ, Lambert A, Todd J, Khor GL, Loh SP, Muslimatun S, Agustina R, Whiting SJ (2008) Vitamin D status and its association with parathyroid hormone concentrations in women of childbearing age living in Jakarta and Kuala Lumpur. Eur J Clin Nutr 62:373–378. https://doi.org/10.1038/sj.ejcn.1602696
Hernandez JL, Olmos JM, Pariente E, Nan D, Martínez J, Llorca J, Valero C, Obregón E, Gonzalez-Macías J (2013) Influence of vitamin D status on vertebral fractures, bone mineral density, and bone turnover markers in normocalcemic postmenopausal women with high parathyroid hormone levels. J Clin Endocrinol Metab 98:1711–1717. https://doi.org/10.1210/jc.2012-3931
Kota S, Jammula S, Kota S, Meher L, Kirtikumar M (2013) Correlation of vitamin D, bone mineral density and parathyroid hormone levels in adults with low bone density. Indian J Orthop 47:402–407. https://doi.org/10.4103/0019-5413.114932
Kim J (2015) Association between serum vitamin D, parathyroid hormone and metabolic syndrome in middle-aged and older Korean adults. Eur J Clin Nutr 69:425–430. https://doi.org/10.1038/ejcn.2014.192
Duan Y, De Luca V, Seeman E (1999) Parathyroid hormone deficiency and excess: similar effects on trabecular bone but differing effects on cortical bone. J Clin Endocrinol Metab 84:718–722. https://doi.org/10.1210/jcem.84.2.549828
Ledger GA, Burritt MF, Kao PC, O'Fallon WM Role of parathyroid hormone in mediating nocturnal and age-related increases in bone resorption. J Clin Endocrinol Metab 80:3304–3310. doi: https://doi.org/10.1210/jcem.80.11.7593443
Sai AJ, Walters RW, Fang X, Gallagher JC (2011) Relationship between vitamin D, parathyroid hormone, and bone health. J Clin Endocrinol Metab 96:E436–E446. https://doi.org/10.1210/jc.2010-1886
Acknowledgements
The authors would like to thank Nada Vrkić, PhD, Associate Professor (University Hospital “Sisters of Mercy,” Zagreb) and Vesna Žižić, PhD (Children’s Hospital Zagreb), for their valuable help and laboratory analyses. The authors truly appreciate and are in debt to the participants of the study.
Funding
The study was supported by the Croatian Ministry of Science and Education (project “Diet, Homocysteine, and Bone Health” No. 058–0222411-2820; PI Irena Colić Barić).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
Irena Keser, Selma Cvijetić, Martina Bituh, Ivana Rumora Samarin, Jasminka Z. Ilich, Irena Colić Barić, and Ivana Rumbak declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Keser, I., Cvijetić, S., Bituh, M. et al. Vitamin D and parathyroid hormone in relation to bone health in Croatian women. Arch Osteoporos 13, 69 (2018). https://doi.org/10.1007/s11657-018-0483-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-018-0483-z