Abstract
Objective
To explore the clinical effificacy and safety of acupuncture in treating gastroesophageal reflux (GER).
Methods
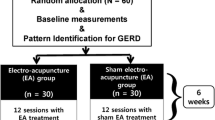
Sixty patients with confirmed diagnosis of GER were randomly assigned to two groups. The 30 patients in the treatment group were treated with acupuncture at acupoints Zhongwan (CV 12), bilateral Zusanli (ST36), Sanyinjiao (SP6), and Neiguan (PC6), once a day, for 1 week as a therapeutic course, with interval of 2–3 days between courses; the 30 patients in the control group were administered orally with omeprazole 20 mg twice a day and 20 mg mosapride thrice a day. The treatment in both group lasted 6 weeks. Patients’ symptoms and times of reflux attacking were recorded, the 24-h intraesophageal acid/bile reflflux were monitored, and the endoscopic feature of esophageal mucous membrane was graded and scored at three time points, i.e., pre-treatment (T0), immediately after ending the treatment course (T1) and 4 weeks after it (T2). Besides, the adverse reactions were also observed.
Results
Compared with those detected at T0, 24-h intraesophageal pH and bile reflux, endoscopic grading score and symptom score were all decreased signifificantly at T1 in both groups similarly (P<0.01), showing insignifificant difference between groups (P>0.05). These indices were reversed at T2 to high level in the control group (P<0.05), but the reversion did not occur in the treatment group (P>0.05). No serious adverse reaction was found during the therapeutic period.
Conclusion
Acupuncture can effectively inhibit the intraesophageal acid and bile reflflux in GER patients to alleviate patients’ symptoms with good safety and is well accepted by patients.
Similar content being viewed by others
References
Lin SR, Xu GM, Hu PJ. Consensus on the diagnosis and treatment of gastroesophageal reflux disease in China. Chin J Gastroenterol (Chin) 2007;12:233–239.
Chinese Gastroesophageal Reflux Disease Study Group. The value of reflux diagnostic questionnaires in the diagnosis of gastroesophageal reflux disease. Chin J Dis (Chin) 2003;23:651–654.
DeVault KR, Castell DO. Updated guidelines for diagnosis and treatment of gastroesophageal reflux disease. Am J Gastroenterol 1999;94:1434–1442.
Cao JB, Yan W, Guo H. Route of clinical diagnosis of gastroesophageal reflux disease. Chin J Gastroenterol (Chin) 2009;14:651–654.
Sun CB, Lu B. The pathogenesis of gastroesophageal reflux disease. Int J Dig Dis (Chin) 22008,28:394–396.
Fang L, Meng L N. Pathogeneticfactors and pharmacotherapy of gastroesophageal reflux disease. Chin J Gastroenterol (Chin) 2008;13:696–698.
Fang HL, Fang QH. Clinical effects of combination of rabeprazole, hydrotalcite and mosapride on 202 patients with refractory gastroesophageal reflex disease (GERD). Chin J Clin Gastroenterol (Chin) 2009;21:49–51.
Zhou GY, Zhou GS. Efficacy observation on transcutaneous electrical stimulation in treating functional dyspepsia. Chin Acupunct Moxibust (Chin) 2009;29:436–440.
Wang JJ, Xia DY, Lu W, Liu L, Huang YX. Influence on gastric motility by acupuncture at Zusanli in functional dyspepsia patients. Chin J Gastroenterol Hepatol (Chin) 2008;17:561–565.
Bardhan KD, Bodemar G, Geldof H. A double-blind, randomized, placebo-controlled dose-ranging study to evaluate the efficacy of alosetron in the treatment of irritable bowel syndrome. Aliment Pharmacol Ther 2002;14:23–34.
Niu HY, Yang M, Qiang BJ, Guo QJ, Yang ZG. Multicentral randomized controlled trials of acupuncture at Zhongwan (CV12) for treatment of peptic ulcer. Chin Acupunct Moxibust (Chin) 2007;27:89–92.
Yang FJ, Wang JJ. Effects of acupuncture of “Zusanli” on gastric mucosal blood flow and level of gastrointestinal hormone in rats with experimental spleen deficiency. Med J Chin People Armed Police Forces (Chin) 2008,19:716–718.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, Cx., Qin, Ym. & Guo, Br. Clinical study on the treatment of gastroesophageal reflux by acupuncture. Chin. J. Integr. Med. 16, 298–303 (2010). https://doi.org/10.1007/s11655-010-0516-y
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-010-0516-y