Abstract
Background
This study, promoted by Italian Association of Radiotherapy and Clinical Oncology (AIRO) Head and Neck Group, aimed to assess the current national practice of target volume delineation on a case of neck lymph node metastases from unknown primary evaluating inter-observer variability, in a setting of primary radiotherapy.
Materials and methods
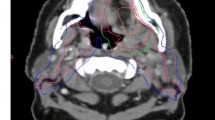
A case of metastatic neck lymph node from occult primary was proposed to 17 radiation oncologists. A national reference RT center was identified and considered as benchmark. Participants were requested to delineate target volumes. A structured questionnaire was administered. A comparison between following parameters of the CTVs was performed: centroids distances, Dice similarity index (DSI), Jaccard index and mean distance to agreement (MDA). Volume expressed in cubic centimeters and CTVs cranio-caudal extension were evaluated.
Results
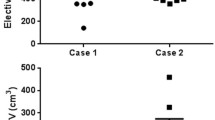
Sixteen of 17 radiation oncologists recommended three CTVs dose levels. (CTV HD, CTV ID and CTV LD); CTV ID was not delineated by one of the participants and by the reference center. The distance between the reference centroid and the mean centroid of CTVs HD was 1.09 cm (0.36–3.99 cm); for CTV LD, a mean centroids distance of 2.45 (0.27–4.83 cm) was found, and for CTV HD, mean DSI is 0.48 and mean Jaccard index is 0.32 and MDA was 8.89 mm. CTV LD showed a mean DSI of 0.46, mean Jaccard index of 0.31 and MDA of 14.87 when compared to the reference.
Conclusion
Many aspects concerning treatment optimization of cervical nodes metastases from occult primary remain unclear, and we found a notable heterogeneity of global radiotherapy management reporting discordances both in target volume delineation and volume prescription.


Similar content being viewed by others
References
Vinod SK, Min M, Jameson MG, Holloway LC (2016) A review of interventions to reduce inter-observer variability in volume delineation in radiation oncology. J Med Imag Radiat Oncol 60:393–406
Morarji K, Fowler A, Vinod SK, Ho Shon I, Laurence JM (2012) Impact of FDG-PET on lung cancer delineation for radiotherapy. J Med Imaging Radiat Oncol 56:195–203
Pitkanen MA, Holli KA, Ojala AT, Laippala P (2001) Quality assurance in radiotherapy of breast cancer-variability in planning target volume delineation. Acta Oncol 40:50–55
Jansen EP, Nijkamp J, Gubanski M, Lind PA, Verheij M (2010) Interobserver variation of clinical target volume delineation in gastric cancer. Int J Radiat Oncol Biol Phys 77:1166–1170
Tai P, Van DJ, Battista J et al (2002) Improving the consistency in cervical esophageal target volume definition by special training. Int J Radiat Oncol Biol Phys 53:766–774
Seddon B, Bidmead M, Wilson J, Khoo V, Dearnaley D (2000) Target volume definition in conformal radiotherapy for prostate cancer: quality assurance in the MRC RT-01 trial. Radiother Oncol 56:738
Gregoire V, Ang K, Budach W et al (2014) Delineation of the neck node levels for head and neck tumors: a 2013 update. DAHANCA, EORTC, HKNPCSG, NCIC CTG, NCRI, RTOG, TROG consensus guidelines. Radiother Oncol 110:172–181
Commowick O, Grégoire V, Malandain G (2008) Atlas-based delineation of lymph node levels in head and neck computed tomography images. Radiother Oncol 87:281–289
Ausili Cefaro, Perez, C.A., Genovesi, D., Vinciguerra, A (2008) A guide for delineation of lymph nodal clinical target volume in radiation therapy. Edn. Springer, Milan
Loo SW, Martin WM, Smith P, Cherian S, Roques TW (2012) Interobserver variation in parotid gland delineation: a study of its impact on intensity-modulated radiotherapy solutions with a systematic review of the literature. J Radiol 85(1016):1070–1077
Feng M, Demiroz C, Vineberg KA, Eisbruch A, Balter JM (2012) Normal tissue anatomy for oropharyngeal cancer: contouring variability and its impact on optimization. Int J Radiat Oncol Biol Phys 84(2):e245–e249
Müller von der Grün J, Tahtali A, Ghanaati S, Rödel C and Balermpas P (2017) Diagnostic and treatment modalities for patients with cervical lymph node metastases of unknown primary site—current status and challenges Radiat Oncol 12:82
Pavlidis N et al (2003) Diagnostic and therapeutic management of cancer of an unknown primary. Eur J Cancer 39(14):1990–2005
Ries LAG, Eisner MP, Kosary CL et al (1999) SEER cancer statistics review. National Cancer Institute, Bethesda
Levi F et al (2002) Epidemiology of unknown primary tumours. Eur J Cancer 38(13):1810–1812
van de Wouw AJ et al (2002) Epidemiology of unknown primary tumours; incidence and population-based survival of 1285 patients in Southeast Netherlands, 1984-1992. Eur J Cancer 38(3):409–413
Merlotti A, Alterio D, Vigna-Taglianti R, Muraglia A, Lastrucci L, Manzo R, Gambaro G, Caspiani O, Miccichè F, Deodato F, Pergolizzi S, Franco P, Corvò R, Russi EG, Sanguineti G (2014) Technical guidelines for head and neck cancer IMRT on behalf of the Italian association of radiation oncology-head and neck working group. Radiat Oncol 9:264
Yao M, Nguyen T, Buatti JM, Dornfeld KJ, Tan H, Wacha J, Bayouth JE, Clamon GH, Funk GF, Smith RB, Chang K, Hoffman HT (2006) Changing failure patterns in oropharyngeal squamous cell carcinoma treated with intensity modulated radiotherapy and implications for future research. Am J Clin Oncol 29:606–612
Weiss MH, Harrison LB, Isaacs R (1994) Use of decision analysis in planning a management strategy for the stage no neck. Arch Otolaryngol Neck Surg 120:699–702
Genovesi D, Ausili-Cèfaro G, Vinciguerra A, Augurio A, Di Tommaso M, Marchese R, Ricardi U, Filippi AR, Girinsky T, Di Biagio K, Belfiglio M, Barbieri E, Valentini V (2011) Interobserver variability of clinical target volume delineation in supra-diaphragmatic Hodgkin’s disease: a multi-institutional experience. Strahlenther Onkol 187:357–366
Genovesi D, Ausili-Cèfaro G, Trignani M, Vinciguerra A, Augurio A, Di Tommaso M, Perrotti F, De Paoli A, Olmi P, Valentini V, Di Nicola M (2014) Interobserver variability of clinical target volume delineation in soft-tissue sarcomas. Cancer Radiothérapie 18(2):89–96
Caravatta L, Macchia G, Mattiucci GC, Sainato A, Cernusco NL, Mantello G, Di Tommaso M, Trignani M, De Paoli A, Boz G, Friso ML, Fusco V, Di Nicola M, Morganti AG, Genovesi D (2014) Inter-observer variability of clinical target volume delineation in radiotherapy treatment of pancreatic cancer: a multi-institutional contouring experience. Radiat Oncol 8(9):198
Dice LR (1945) Measures of the amount of ecologic association between species. Ecology 26:297–302
Fotina I, Lütgendorf-Caucig C, Stock M, Pötter R, Georg D (2012) Critical discussion of evaluation parameters for inter-observer variability in target definition for radiation therapy. Strahlenther Onkol 188:160–167
Langendijk JA, Doornaert P, Verdonck-de Leeuw IM, Leemans CR, Aaronson NK, Slotman BJ (2008) Impact of late treatment-related toxicity on quality of life among patients with head and neck cancer treated with radiotherapy. J Clin Oncol 26:3770–3776
Allozi R, Li XA, White J, Apte A, Tai A, Michalski JM, Bosch WR, El Naqa I (2010) Tools for consensus analysis of experts contours for radiotherapy structure definitions. Radiother Oncol 97(3):572–578
Wondergem BCM, van Bommel P, van der Weide ThP (2000) Matching index expressions for information retrieval. Inf Retrieval 2:24
Speight R, Karakaya E, Prestwich R, Sen M, Lindsay R, Harding R, Sykes J (2014) Evaluation of atlas based auto-segmentation for head and neck target volume delineation in adaptive/replan IMRT. J Phys Conf Ser 489:1
Thomson D (2014) Evaluation of an automatic segmentation algorithm for definition of head and neck organs at risk. Radiat Oncol 9:173
Huttenlocher DP (1993) Iee comparing images using the hausdorff distance. Trans Pattern Anal Mach Intell 15(9)
Fabri Daniella (2013) A quantitative comparison of the performance of three deformable registration algorithms in radiotherapy. Z Med Phys 23(4):279–290
Waltonen JD, Ozer E, Hall NC et al (2009) Metastatic carcinoma of the neck of unknown primary origin: evolution and efficacy of the modern workup. Arch Otolaryngol Head Neck Surg 135:1024–1029
Miller FR, Karnad AB, Eng T et al (2008) Management of the unknown primary carcinoma: long-term follow-up on a negative PET scan and negative panendoscopy. Head Neck 30:28–34
Grau C, Johansen LV, Jakobsen J et al (2000) Cervical lymph node metastases from unknown primary tumours. Results from a national survey by the Danish Society for Head and Neck Oncology. Radiother Oncol 55:121–129
Paleri V, Urbano T G, Mehanna H Repanos C, Lancaster J, Roques T, Patel M, Sen M (2016) Management of neck metastases in head and neck cancer: United Kingdom National Multidisciplinary Guidelines. J Laryngol Otol. 130(Suppl 2): S161–S169
Yamazaki T, Kodaira T, Ota Y, Akimoto T, Wada H, Hiratsuka J, Nishimura Y, Ishihara S, Nonoshita T, Hayakawa K, Sekii S, Uchida N (2017) Retrospective analysis of definitive radiotherapy for neck node metastasis from unknown primary tumor: Japanese Radiation Oncology Study Group study. Jpn J Clin Oncol 1;47(9):856–862
Frank SJ, Rosenthal DI, Petsuksiri J, Ang KK, Morrison WH, Weber RS, Glisson BS, Chao KSC, Schwartz DL, Chronowski GM, El-Naggar AK, Garden AS (2010) Intensity-modulated radiotherapy for cervical node squamous cell carcinoma metastases from unknown head-and-neck primary site: M. D. Anderson cancer center outcomes and patterns of failure. Int J Radiat Oncol 78:1005–1010
Riaz N, Chen A, Lee NY (2013) Squamous cell carcinoma of unknown primary in the head and neck. In: Lee NY, Lu JJ (eds) Target volume delineation and field setup. Springer, Berlin, pp 65–71
Beldì D, Jereczek-Fossa BA, D’Onofrio A, Gambaro G, Fiore MR, Pia F, Chiesa F, Orecchia R, Krengli M (2007) Role of radiotherapy in the treatment of cervical lymph node metastases from an unknown primary site: retrospective analysis of 113 patients. Int J Radiat Oncol 69:1051–1058
Villeneuve H, Després P, Fortin B, Filion E, Donath D, Soulières D, Guertin L, Ayad T, Christopoulos A, Nguyen-Tan PF (2012) Cervical lymph node metastases from unknown primary cancer: a single-institution experience with intensity-modulated radiotherapy. Int J Radiat Oncol 82:1866–1871
Ligey A, Gentil J, Créhange G, Montbarbon X, Pommier P, Peignaux K, Truc G, Maingon P (2009) Impact of target volumes and radiation technique on loco-regional control and survival for patients with unilateral cervical lymph node metastases from an unknown primary. Radiother Oncol 93:483–487
Nieder C et al (2001) Cervical lymph node metastases from occult squamous cell carcinoma: cut down a tree to get an apple? Int J Radiat Oncol Biol Phys 50(3):727–733
Reddy SP, Marks JE (1997) Metastatic carcinoma in the cervical lymph nodes from an unknown primary site: results of bilateral neck plus mucosal irradiation vs. ipsilateral neck irradiation. Int J Radiat Oncol Biol Phys 37:797–802
Liu X, et al. (2016) Optimization of radiotherapy for neck carcinoma metastasis from unknown primary sites: a meta-analysis. Oncotarget. doi:10. 18632/oncotarget.12852
NCCN: National Comprehensive Cancer Network. https://www.nccn.org/professionals/physician_gls/pdf/head-and-neck.pdfAccessed 28 Nov 2016
Batumalai V, Koh ES, Delaney GP, Holloway LC, Jameson MG, Papadatos G, Lonergan DM (2011) Interobserver variability in clinical target volume delineation in tangential breast irradiation: a comparison between radiation oncologists and radiation therapists. Clin Oncol (R Coll Radiol) 23:108–113
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Trignani, M., Argenone, A., Di Biase, S. et al. Inter-observer variability of clinical target volume delineation in definitive radiotherapy of neck lymph node metastases from unknown primary. A cooperative study of the Italian Association of Radiotherapy and Clinical Oncology (AIRO) Head and Neck Group. Radiol med 124, 682–692 (2019). https://doi.org/10.1007/s11547-019-01006-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-019-01006-y