Abstract
Objectives
To evaluate excision histology outcome of B3a lesions diagnosed at imaging-guided core biopsy and assess whether clinical and radiologic features may predict upgrade to malignancy.
Methods
A total of 153 B3a lesions (74 papillomas, 51 radial scars and 28 fibro-epithelial lesions) that underwent surgical excision were assessed. PPV for malignancy in all B3a lesions and specific for each sub-category was evaluated. Multivariate analysis was conducted to identify association between clinical (age, family or personal history of breast cancer, symptoms), diagnostic findings (imaging modality, lesion size, final BI-RADS category) and final excision outcome.
Results
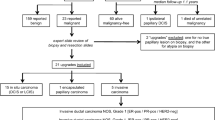
Eleven (7%) of 153 B3a lesions were upgraded to malignancy. All carcinomas diagnosed on excision were non-high grade DCIS. Following features were significantly associated with malignancy: lesions identified only on mammography (3/21; 14%), both mammography and ultrasound (7/44; 16%), lesion size > 10 mm (10/74; 13.5%) and BI-RADS category 4-5 (8/29; 27.6%). The absence of residual microcalcification after biopsy was associated with decreased risk for malignancy (15/16[93.7%]; p = 0.0297). Lesion size > 10 mm (OR = 9.3832; 95%; p = 0.0398) and BI-RADS category 4–5 (OR = 12.6004; 95%; p = 0.0006) were found to be independent predictors of upgrade to malignancy.
Conclusions
B3a lesions are associated with low risk of malignancy at excision. Lesion size > 10 mm and BI-RADS 4–5 category may represent useful predictors of upgrade to malignancy.



Similar content being viewed by others
References
Fajardo LL, Pisano ED, Caudry DJ, Gatsonis CA, Berg WA, Connolly J et al (2004) Stereotactic and sonographic large-core biopsy of nonpalpable breast lesions: results of the Radiologic Diagnostic Oncology Group V study. Acad Radiol 11:293–308
Litherland JC, Evans AJ, Wilson AR, Kollias J, Pinder SE, Elston CW et al (1996) The impact of core-biopsy on pre-operative diagnosis rate of screen detected breast cancers. Clin Radiol 51:562–565
Ellis O, Humphreys S, Michell M, Pinder SE, Wells CA, Zakhour HD (2001) Guidelines for non-operative diagnostic procedures and reporting in cancer screening. NHSBSP Publ 50:35–40
El-Sayed ME, Rakha EA, Reed J, Lee AH, Evans AJ, Ellis IO (2008) Predictive value of needle core biopsy diagnoses of lesions of uncertain malignant potential (B3) in abnormalities detected by mammographic screening. Histopathology 53:650–657
Houssami N, Ciatto S, Bilous M, Vezzosi V, Bianchi S (2007) Borderline breast core needle histology: predictive values for malignancy in lesions of uncertain malignant potential (B3). Br J Cancer 96:253–257
Rakha EA, Ellis IO (2007) An overview of assessment of prognostic and predictive factors in breast cancer needle core biopsy specimens. J Clin Pathol 60:1300–1306
Ibrahim AE, Bateman AC, Theaker JM, Low JL, Addis B, Tidbury P et al (2001) The role and histological classification of needle core biopsy in comparison with fine needle aspiration cytology in the preoperative assessment of impalpable breast lesions. J Clin Pathol 54:121–125
Rakha EA, Lee AH, Jenkins JA, Murphy AE, Hamilton LJ, Ellis IO (2011) Characterization and outcome of breast needle core biopsy diagnoses of lesions of uncertain malignant potential (B3) in abnormalities detected by mammographic screening. Int J Cancer 129:1417–1424
de Beca FF, Rasteiro C, Correia A, Costa S, Amendoeira I (2013) Improved malignancy prediction by B3 breast lesions subclassification. Ann Diagn Pathol 17:434–436
Yu CC, Ueng SH, Cheung YC, Shen SC, Kuo WL, Tsai HP et al (2015) Predictors of underestimation of malignancy after image-guided core needle biopsy diagnosis of flat epithelial atypia or atypical ductal hyperplasia. Breast J 21:224–232
Lee AHS, Denley HE, Pinder S et al (2003) Excision biopsy findings of patients with breast needle core biopsies reported as suspicious of malignancy (B4) or lesion of uncertain malignant potential (B3). Histopathology 42:331–336
Dillon MF, McDermott EW, Hill AD, O’Doherty A, O’Higgins N, Quinn CM (2007) Predictive value of breast lesions of “uncertain malignant potential” determined by needle core biopsy. Ann Surg Oncol 14:704–711
Lieske B, Ravichandran D, Alvi A, Lawrence DAS, Wright DJ (2008) Screen-detected breast lesions with an indeterminate (B3) core needle biopsy should be excised. Eur J Surg Oncol 34:1293–1298
Hayes BD, O’Doherty A, Quinn CM (2009) Correlation of needle core biopsy with excision histology in screen-detected B3 lesions: the Merriot Breast Screening Unit experience. J Clin Pathol 62:1136–1140
Noske A, Pahl S, Fallenberg E, Richter-Ehrenstein C, Buckendahl AC, Weichert W et al (2010) Flat epithelial atypia is a common subtype of B3 breast lesions and associated with noninvasive cancer but not with invasive cancer in final excision histology. Hum Pathol 41:522–527
Rageth CJ, O’Flynn EAM, Comstock C et al (2016) First international consensus conference on lesions of uncertain malignant potential in the breast (B3 lesions). Breast Cancer Res Treat 159:203–213
Bianchi S, Caini S, Renne G et al (2011) Positive predictive value for malignancy on surgical excision of breast lesions of uncertain malignant potential (B3) diagnosed by stereotactic vacuum-assisted needle core biopsy (VANCB): a large multi-institutional study in Italy. Breast 20:264–270
Mayer S, Kayser G, Rücker G et al (2017) Absence of epithelial atypia in B3-lesions of the breast is associated with decreased risk for malignancy. Breast 31:144–149
Bernik SF, Troob S, Ying BL, Simpson SA, Axelrod DM, Siegel B et al (2009) Papillary lesions of the breast diagnosed by core needle biopsy: 71 cases with surgical follow-up. Am J Surg 197:473–478
Johnson NB, Collins LC (2009) Update on percutaneous needle biopsy of non-malignant breast lesions. Adv Anat Pathol 16:183–195
Tennant SL, Evans A, Hamilton LJ, James J, Lee AHS, Hodi Z et al (2008) Vacuumassisted excision of breast lesions of uncertain malignant potential (B3) e an alternative to surgery in selected cases. Breast 17:546–549
Resetkova E, Edelweiss M, Albarracin CT, Yang WT (2008) Management of radial sclerosing lesions of the breast diagnosed using percutaneous vacuum-assisted core needle biopsy: recommendations for excision based on seven years’ of experience at a single institution. Breast Cancer Res Treat 127:335 [Epubahead of print]
Rakha EA, Lee AH, Evans AJ et al (2010) Tubular carcinoma of the breast: further evidence to support its excellent prognosis. J Clin Oncol 28:99–104
Maclean GM, Courtney SP, Umeh H, Sanjeev S, McCormick C, Smith BM (2013) Is mode of presentation of B3 breast core biopsies (screen-detected or symptomatic) a distinguishing factor in the final histopathologic result or risk of diagnosis of malignancy? World J Surg 37:2607–2612
Youk JH, Kim EK, Kwak JY, Son EJ, Park BW, Kim S (2011) Benign papilloma without atypia diagnosed at US-guided 14-gauge core-needle biopsy: clinical and US features predictive of upgrade to malignancy. Radiology 258:81–88
Kil WH, Cho EY, Kim JH, Nam SJ, Yang JH (2008) Is surgical excision necessary in benign papillary lesions initially diagnosed at core biopsy? Breast 17:258–262
Chang JM, Moon WK, Cho N et al (2010) Risk of carcinoma after subsequent excision of benign papilloma initially diagnosed with an ultrasound (US)-guided 14-gauge core needle biopsy: a prospective observational study. Eur Radiol 20:1093–1100
Shin HJ, Kim HH, Kim SM et al (2008) Papillary lesions of the breast diagnosed at percutaneous sonographically guided biopsy: comparison of sonographic features and biopsy methods. AJR Am J Roentgenol 190:630–636
Hoffmann O, Stamatis GA, Bittner AK et al (2016) B3-lesions of the breast and cancer risk—an analysis of mammography screening patients. Mol Clin Oncol 4:705–708
Linda A, Zuiani C, Bazzocchi M, Furlan A, Londero V (2008) Borderline breast lesions diagnosed at core needle biopsy: can magnetic resonance mammography rule out associated malignancy? Preliminary results based on 79 surgically excised lesions. Breast 7:125–131
Pediconi F, Padula S, Dominelli V et al (2010) Role of breast MR imaging for predicting malignancy of histologically borderline lesions diagnosed at core needle biopsy: prospective evaluation. Radiology 257:653–661
Londero V, Zuiani C, Linda A, Girometti R, Bazzocchi M, Sardanelli F (2012) High-risk breast lesions at imaging-guided needle biopsy: usefulness of MRI for treatment decision. AJR 199:240–250
Zuiani C, Londero V, Bestagno A, Puglisi F, Di Loreto C, Bazzocchi M (2005) Proliferative high-risk lesions of the breast: contribution and limits of US-guided core biopsy. Radiol Med 110:589–602
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Guarantor
The scientific guarantor of this publication is Chiara Zuiani.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained with waiver of patient informed consent.
Methodology
This is a retrospective, observational study, performed at one institution.
Rights and permissions
About this article
Cite this article
Bednarova, I., Londero, V., Linda, A. et al. Do clinical and radiologic features help predict malignancy of B3 breast lesions without epithelial atypia (B3a)?. Radiol med 123, 809–817 (2018). https://doi.org/10.1007/s11547-018-0914-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-018-0914-3