Abstract
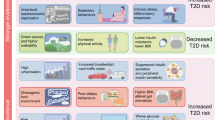
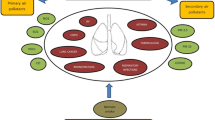
We report integration of the United States Environmental Protection Agency’s (USEPA) United States Environmental Justice Screen (EJSCREEN) database with our Public Health Exposome dataset to interrogate 9232 census blocks to model the complexity of relationships among environmental and socio-demographic variables toward estimating adverse pregnancy outcomes [low birth weight (LBW) and pre-term birth (PTB)] in all Ohio counties. Using a hill-climbing algorithm in R software, we derived a Bayesian network that mapped all controlled associations among all variables available by applying a mapping algorithm. The results revealed 17 environmental and socio-demographic variables that were represented by nodes containing 69 links accounting for a network with 32.85% density and average degree of 9.2 showing the most connected nodes in the center of the model. The model predicts that the socio-economic variables low income, minority, and under age five populations are correlated and associated with the environmental variables; particulate matter (PM2.5) level in air, proximity to risk management facilities, and proximity to direct discharges in water are linked to PTB and LBW in 88 Ohio counties. The methodology used to derive significant associations of chemical and non-chemical stressors linked to PTB and LBW from indices of geo-coded environmental neighborhood deprivation serves as a proxy for design of an African-American women’s cohort to be recruited in Ohio counties from federally qualified community health centers within the 9232 census blocks. The results have implications for the development of severity scores for endo-phenotypes of resilience based on associations and linkages for different chemical and non-chemical stressors that have been shown to moderate cardio-metabolic disease within a population health context.



Similar content being viewed by others
Abbreviations
- PM2.5 :
-
Particulate matter at 2.5 μm
- USEPA:
-
United States Environmental Protection Agency
- EJSCREEN:
-
United States Environmental Justice Screen
- LBW:
-
low birth weight
- PTB:
-
pre-term birth
- IM:
-
infant mortality
- SE:
-
Stambaugh Elwood
- SSHAC:
-
South Side Health Advisory Committee
- CV:
-
cardiovascular
- CVD:
-
cardiovascular disease
- PPGIS:
-
public participatory geographical information system
- TRI:
-
toxic release inventory
- RMP:
-
risk management plan
- NPL site:
-
national priorities list site
References
Greater columbus infant mortality task force final report and implementation plan. Available online: http://gcinfantmortality.org/wp content/uploads/2014/01/IMTF-2014 Final-Report-v10.pdf. Accessed 1 June 2016.
Jiao Y, Bower JK, Im W, Basta N, Obrycki A-HM, Wilder A, et al. Application of citizen science risk communication tools in a vulnerable urban community. Int J Environ Res Public Health. 2016;13(1):11. https://doi.org/10.3390/ijerp13010011.
Reece J, Olinger J, Holley K. Social capital and equitable neighborhood revitalization on Columbus southside. Available online: http://kirwaninstitute.osu.edu/wp-content/uploads/2014/10/01410-southside.pdf. Accessed 11 Aug 2015.
Burgard S, Kalousova L. Effects of the great recession: health and well-being. Annu Rev Sociol. 2015;41(150504162558008):181–201. https://doi.org/10.1146/annurev-soc-073014-112204.
D’Angelo H, Ammerman A, Gordon-Larsen L, L Lytle L, Ribisl KM. Sociodemographic disparities in proximity of schools to tobacco outlets and fast-food restaurants. Am J Public Health. 2016;106(9):1556–62.
Juarez PD, Matthews-Juarez P, Hood DB, Im W, Levine RS, Kilbourne BJ, et al. The public health exposome: a population-based, exposure science approach to health disparities research. Int J Environ Res Public Health. 2014;11(12):12866–95.
Langston MA, Levine RS, Kilbourne BJ, Rogers GL, Kershenbaum AD, Baktash SH, et al. Scalable combinatorial tools for health disparities research. Int J Environ Res Public Health. 2014;11(10):10419–43.
Egli V, Oliver M, Tautolo e-S. The development of a model of community garden benefits to wellbeing. Prev Med Rep. 2016;3:348–52.
Holtzen H, Klein EG, Keller B, Hood N. Perceptions of physical inspections as a tool to protect housing quality and promote health equity. J Health Care Poor Underserved. 2016;27(2):549–59.
Batterman S, Ganguly R, Harbin P. High resolution spatial and temporal mapping of traffic-related air pollutants. Int J Environ Res Public Health. 2015;12(4):3646–66.
U.S. Environmental Protection Agency. Learn about the toxics release inventory. https://www.epa.gov/toxics-release-inventory-tri-program/learn-about-toxics-release-inventory (November 9).
Wild CP. Complementing the genome with an “exposome”: the outstanding challenge of environmental exposure measurement in molecular epidemiology. Cancer Epidemiol Biomark Prev. 2005;14(8):1847–50.
Clark RS, Pellom ST, Booker B, Ramesh A, Zhang T, Shanker A, et al. Validation of research trajectory 1 of an exposome framework: exposure to benzo(a) pyrene confers enhanced susceptibility tobacterial infection. Environ Res. 2016;146:173–84.
EPA. EJSCREEN: Environmental Justice Screening and Mapping Tool. Available online: http://www2.epa.gov/ejscreen. Accessed 15 June 2015.
Al-Hamdan MZ, Crosson WL, Economou SA, et al. Environmental public health applications using remotely sensed data. Geocarto Int. 2014;29(1):85–98.
Scutari M. Learning Bayesian networks with the bnlearn R package. J Stat Softw. 2010;35:1–22.
Healthy People 2020 [Internet]. Washington, DC: U.S. Department of Health and Human Services, Office of Disease Prevention and Health Promotion. Available from: http://www.healthypeople.gov/2020/default.aspx. Accessed 24 Apr 2017.
Ferguson KK, O'Neill MS, Meeker JD. Environmental contaminant exposures and preterm birth: a comprehensive review. J Toxicol Env Heal B. 2013;16:69–113.
Peters A. Particulate matter and heart disease: evidence from epidemiological studies. Toxicol Appl Pharmacol. 2005;207(2, Supplement):477–82.
Beelen R, Hoek G, Raaschou-Nielsen O, Stafoggia M, Andersen ZJ, Weinmayr G, et al. Natural-cause mortality and long-term exposure to particle components: an analysis of 19 European cohorts within the multi-center ESCAPE project. Environ Health Perspect. 2015;123(6):525–33.
Pope Iii CA, Renlund DG, Kfoury AG, May HT, Horne BD. Relation of heart failure hospitalization to exposure to fine particulate air pollution. Am J Cardiol. 2008;102(9):1230–4.
Nelin TD, Joseph AM, Gorr MW, Wold LE. Direct and indirect effects of particulate matter on the cardiovascular system. Toxicol Lett. 2012;208(3):293–9.
Polichetti G, Cocco S, Spinali A, Trimarco V, Nunziata A. Effects of particulate matter (PM10, PM2.5 and PM1) on the cardiovascular system. Toxicology. 2009;261:1–2):1-8.
Link MS, Luttmann-Gibson H, Schwartz J, Mittleman MA, Wessler B, Gold DR, et al. Acute exposure to air pollution triggers atrial fibrillation. J Am Coll Cardiol. 2013;62(9):816–25.
Olson JL, Bild DE, Kronmal RA, Burke GL. Legacy of MESA. Glob Heart. 2016;11(3):269–74.
Kaufman JD, Adar SD, Barr RG, et al. Association between air pollution and coronary artery calcification within six metropolitan areas in the USA (the Multi-Ethnic Study of Atherosclerosis and Air Pollution): a longitudinal cohort study. Lancet. 2016;388(10045):696–704. https://doi.org/10.1016/S0140-6736(16)00378-0.
Kaufman JD, Spalt EW, Curl CL, Hajat A, Jones MR, Kim SY, et al. Advances in understanding air pollution and CVD. Glob Heart. 2016;11(3):343–52.
Brunekreef B, Hoffmann B. Air pollution and heart disease. Lancet. 2016;388(10045):640–2.
Juarez PD, Hood DB, Rogers GL, Baktash SH, Saxton AM, Matthews-Juarez P, et al. A novel approach to analyzing lung cancer mortality disparities: using the exposome and a graph-theoretical toolchain. Environ Dis. 2017;2:33–44.
Steptoe A, Hackett RA, Lazzarino AI, Bostock S, la Marca R, Carvalho LA, et al. Disruption of multisystem responses to stress in type 2 diabetes: investigating the dynamics of allostatic load. Proc Natl Acad Sci U S A. 2014;111(44):15693–8.
McEwen BS, Gianaros PJ. Central role of the brain in stress and adaptation: links to socioeconomic status, health, and disease. Ann N Y Acad Sci. 2010;1186:190–222.
Signorello LB, Hargreaves MK, Blot WJ. The southern community cohort study: investigating health disparities. J Health Care Poor Underserved. 2010;21(1):26–37.
Banerjee PA, Lamb S. A systematic review of factors linked to poor academic performance of disadvantaged students in science and math in schools. Cogent Educ. 2016;3:1. https://doi.org/10.1080/2331186X.2016.1178441.
Kamrath HJ, Osterholm E, Stover-Haney R, George T, O'Connor-Von S, Needle J. Lasting legacy: maternal perspectives of perinatal palliative care. J Palliat Med. 2018; https://doi.org/10.1089/jpm.2018.0303.
Weden MM, Carpiano RM, Robert SA. Subjective and objective neighborhood characteristics and adult health. Soc Sci Med. 2008;66(6):1256–70.
Hajat A, Diez-Roux AV, Adar SD, Auchincloss AH, Lovasi GS, O'Neill MS, et al. Air pollution and individual and neighborhood socioeconomic status: evidence from the Multi-Ethnic Study of Atherosclerosis (MESA). Environ Health Perspect. 2013;121(11–12):1325–33.
Schempf A, Strobino D, O’Campo P. Neighborhood effects on birthweight: an exploration of psychosocial and behavioral pathways in Baltimore, 1995–1996. Soc Sci Med. 2009;68(1):100–10.
Francisco A, El-Sayed A. National income inequality and ineffective health insurance in 35 low and middle income countries. Health Policy Plan. 2017;32:487–92.
Braveman P, Cubbin C, Egerter S, Williams DR, Pamuk E. Socioeconomic disparities in health in the United States: what the patterns tell us. Am J Public Health. 2010;100(Suppl 1):S186–96.
Dourson M, Price P, Unrine J. Health risks from eating contaminated fish. Comments Toxicol. 2002;8(4–6):399–419. https://doi.org/10.1080/08865140215061.
Anderson PD, Dourson M, Unrine J, Sheeshka J, Murkin E, Stober J. Framework and case studies. Comments Toxicol. 2002;8(4–6):431–502. https://doi.org/10.1080/08865140215066.
Hack CE, Haber LT, Maier A, Schulte P, Fowler B, Lotz WG, et al. Bayesian network model biomarker-based dose response. Risk Anal. 2010;30:1037–51.
Williams DR, Collins C. Racial residential segregation: a fundamental cause of racial disparities in health. Public Health Rep. 2001;16(5):404–16.
Acknowledgments
The authors would like to thank the entire Interdisciplinary Cardio-metabolic Exposome Team (ICE Tea) for critical review and comments. This work was supported, in part, by start-up package received from the Ohio State University College of Public Health and US EPA STAR Award RD83927501 (DBH and PDJ). Support was also from a start-up package received from Meharry Medical College for the Health Disparities Research Center of Excellence (PDJ).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM
(PDF 5.09 mb)
Rights and permissions
About this article
Cite this article
Cifuentes, P., Reichard, J., Im, W. et al. Application of the Public Health Exposome Framework to Estimate Phenotypes of Resilience in a Model Ohio African-American Women’s Cohort. J Urban Health 96 (Suppl 1), 57–71 (2019). https://doi.org/10.1007/s11524-018-00338-w
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11524-018-00338-w