Abstract
Background
The variability in progression-free survival (PFS) and overall survival (OS) among patients with epithelial ovarian cancer (EOC) makes it difficult to reliably predict outcomes. A predictive biomarker of bevacizumab efficacy as first-line therapy in EOC is still lacking.
Objective
The MITO group conducted a multicenter, retrospective study (MITO 24) to investigate the role of inflammatory indexes as prognostic factors and predictors of treatment efficacy in FIGO stage III–IV EOC patients treated with first-line chemotherapy alone or in combination with bevacizumab.
Patients and Methods
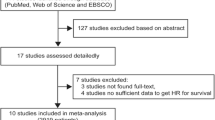
Of the 375 patients recruited, 301 received chemotherapy alone and 74 received chemotherapy with bevacizumab. The pre-treatment neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), and systemic immune inflammation index (SII) were evaluated to identify a potential correlation with PFS and OS in both the overall population and the two treatment arms.
Results
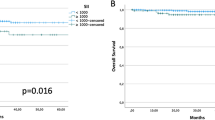
In the overall population, the PFS and OS were significantly longer in patients with low inflammatory indexes (p < 0.0001). In multivariate analyses, the NLR was significantly associated with OS (p = 0.016), and the PLR was significantly associated with PFS (p = 0.024). Inflammatory indexes were significantly correlated with patient prognosis in the chemotherapy-alone group (p < 0.0001). Patients in the chemotherapy with bevacizumab group with a high NLR had a higher PFS and OS (p = 0.026 and p = 0.029, respectively) than those in the chemotherapy-alone group. Conversely, PFS and OS were significantly poorer in patients with a high SII (p = 0.024 and p = 0.017, respectively).
Conclusion
Our results suggest that bevacizumab improves clinical outcome in patients with a high NLR but may be detrimental in those with a high SII.



Similar content being viewed by others
References
Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell. 2011;144:646–74.
Karam A, Ledermann JA, Kim JW, et al. 5th ovarian Cancer consensus conference. In: Fifth Ovarian Cancer Consensus Conference of the gynecologic Cancer InterGroup: First-Line Interventions. Ann Oncol. 2017;28:711–7.
Perren TJ, Swart AM, Pfisterer J, et al. A phase 3 trial of bevacizumab in ovarian cancer. N Engl J Med. 2011;365:2484–96.
Burger RA, Brady MF, Bookman MA, et al. Incorporation of bevacizumab in the primary treatment of ovarian cancer. N Engl J Med. 2011;365:2473–83.
Oza AM, Cook AD, Pfisterer J, et al. Standard chemotherapy with or without bevacizumab for women with newly diagnosed ovarian cancer (ICON7): overall survival results of a phase 3 randomised trial. Lancet Oncol. 2015;16:928–36.
Wilson MK, Pujade-Lauraine E, Aoki D, et al. Fifth ovarian Cancer consensus conference of the gynecologic Cancer InterGroup: recurrent disease. Ann Oncol. 2017;28:727–32.
Aghajanian C, Goff B, Nycum LR, et al. Final overall survival and safety analysis of OCEANS, a phase 3 trial of chemotherapy with or without bevacizumab in patients with platinum-sensitive recurrent ovarian cancer. Gynecol Oncol. 2015;139:10–6.
Lambrechts D, Lenz HJ, de Haas S, Carmeliet P, Scherer SJ. Markers of response for the antiangiogenic agent bevacizumab. J Clin Oncol 2013;31:1219–1230.
Bais C, Mueller B, Brady MF, et al. Tumor microvessel density as a potential predictive marker for bevacizumab benefit: GOG-0218 biomarker analyses. J Natl Cancer Inst. 2017;109(11):djx066. https://doi.org/10.1093/jnci/djx066.
Idzko M, Ferrari D, Eltzschig HK. Nucleotide signalling during inflammation. Nature. 2014;509:310–7.
Grivennikov SI, Greten FR, Karin M. Immunity, inflammation, and cancer. Cell. 2010;140:883–99.
Templeton AJ, McNamara MG, Seruga B, et al. Prognostic role of neutrophil-to-lymphocyte ratio in solid tumors: a systematic review and meta-analysis. J Natl Cancer Inst. 2014;106:u124.
Santoni M, De Giorgi U, Iacovelli R, et al. Pre-treatment neutrophil-to-lymphocyte ratio may be associated with the outcome in patients treated with everolimus for metastatic renal cell carcinoma. Br J Cancer. 2013;109:1755–9.
Chua W, Charles KA, Baracos VE, Clarke SJ. Neutrophil/ lymphocyte ratio predicts chemotherapy outcomes in patients with advanced colorectal cancer. Br J Cancer. 2011;104:1288–95.
Rossi L, Santoni M, Crabb SJ, et al. High neutrophil-to-lymphocyte ratio persistent during first-line chemotherapy predicts poor clinical outcome in patients with advanced urothelial Cancer. Ann Surg Oncol. 2015;22:1377–84.
Conteduca V, Crabb SJ, Jones RJ, et al. Persistent neutrophil to lymphocyte ratio >3 during treatment with enzalutamide and clinical outcome in patients with castration-resistant prostate cancer. PLoS One. 2016;11:e0158952.
Huang QT, Zhou L, Zeng WJ, et al. Prognostic significance of neutrophil-to-lymphocyte ratio in ovarian cancer: a systematic review and meta-analysis of observational studies. Cell Physiol Biochem. 2017;41:2411–8.
Kwon HC, Kim SH, Oh SY, et al. Clinical significance of preoperative neutrophil-lymphocyte versus platelet-lymphocyte ratio in patients with operable colorectal cancer. Biomarkers. 2012;17:216–22.
Hu B, Yang XR, Xu Y, et al. Systemic immune- inflammation index predicts prognosis of patients after curative resection for hepatocellular carcinoma. Clin Cancer Res. 2014;20:6212–22.
Passardi A, Scarpi E, Cavanna L, et al. Inflammatory indexes as predictors of prognosis and bevacizumab efficacy in patients with metastatic colorectal cancer. Oncotarget. 2016;7:33210–9.
Lolli C, Caffo O, Scarpi E, et al. Systemic immune-inflammation index predicts the clinical outcome in patients with mcrpc treated with abiraterone. Front Pharmacol. 2016;7:376.
Clarke S, Burge M, Cordwell C, et al. An australian translational study to evaluate the prognostic role of inflammatory markers in patients with metastatic colorectal cancer treated with bevacizumab (Avastin) [ASCENT]. BMC Cancer. 2013;13:120.
Eisenhauer EA, Therasse P, Bogaerts J, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45:228–47.
Moses K, Brandau S. Human neutrophils: their role in cancer and relation to myeloid-derived suppressor cells. Semin Immunol. 2016;28:187–96.
Balkwill F, Mantovani A. Inflammation and cancer: back to Virchow? Lancet. 2001;357:539–45.
Labelle M, Begum S, Hynes RO. Direct signaling between platelets and cancer cells induces epithelial-mesenchymal-like transition and promote metastasis. Cancer Cell. 2011;20:576–90.
Zhang L, Conejo-Garcia JR, Katsaros D, et al. Intratumoral T cells, recurrence, and survival in epithelial ovarian cancer. N Engl J Med. 2003;348:203–13.
Leffers N, Gooden MJ, de Jong RA, et al. Prognostic significance of tumor-infiltrating T-lymphocytes in primary and metastatic lesions of advanced stage ovarian cancer. Cancer Immunol Immunother. 2009;58:449–59.
Manning EA, Ullman JG, Leatherman JM, et al. A vascular endothelial growth factor receptor-2 inhibitor enhances antitumor immunity through an immune-based mechanism. Clin Cancer Res. 2007;13:3951–9.
Shrimali RK, Yu Z, Theoret MR, et al. Antiangiogenic agents can increase lymphocyte infiltration into tumor and enhance the effectiveness of adoptive immunotherapy of cancer. Cancer Res. 2010;70:6171–80.
Lambert AW, Pattabiraman DR, Weinberg RA. Emerging biological principles of metastasis. Cell. 2017;168:670–91.
Kim HS, Choi HY, Lee M, et al. Systemic inflammatory response markers and CA-125 levels in ovarian clear cell carcinoma: a two center cohort study. Cancer Res Treat. 2016;48:250–8.
Labelle M, Begum S, Hynes RO. Platelets guide the formation of early metastatic niches. Proc Natl Acad Sci USA. 2014;111:E3053–61.
Grepin R, Guyot M, Jacquin M, et al. Acceleration of clear cell renal cell carcinoma growth in mice following bevacizumab/Avastin treatment: the role of CXCL cytokines. Oncogene. 2012;31:1683–94.
Stone RL, Nick AM, McNeish IA, et al. Paraneoplastic thrombocytosis in ovarian cancer. N Engl J Med. 2012;366:610–8. N Engl J Med. 2012;367:1768 (Erratum).
Middleton K, Jones J, Lwin Z, Coward JI. Interleukin-6: an angiogenic target in solid tumours. Crit Rev Oncol Hematol. 2014;89:129–39.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No external funding was used in the preparation of this manuscript.
Conflict of Interest
Alberto Farolfi, Micaela Petrone, Emanuela Scarpi, Valentina Gallà, Filippo Greco, Claudia Casanova, Lucia Longo, Gennaro Cormio, Michele Orditura, Alessandra Bologna, Laura Zavallone, Jole Ventriglia, Elisena Franzese, Vera Loizzi, Donatella Giardina, Eva Pigozzi, Raffaella Cioffi, Sandro Pignata, Giorgio Giorda, and Ugo De Giorgi declare that they have no conflicts of interest that might be relevant to the contents of this manuscript.
Rights and permissions
About this article
Cite this article
Farolfi, A., Petrone, M., Scarpi, E. et al. Inflammatory Indexes as Prognostic and Predictive Factors in Ovarian Cancer Treated with Chemotherapy Alone or Together with Bevacizumab. A Multicenter, Retrospective Analysis by the MITO Group (MITO 24). Targ Oncol 13, 469–479 (2018). https://doi.org/10.1007/s11523-018-0574-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11523-018-0574-1