Abstract
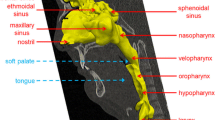
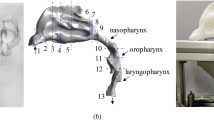
A better understanding of airflow characteristics in the upper airway (UA) is crucial in investigating obstructive sleep apnea (OSA), particle sedimentation, drug delivery, and many biomedical problems. Direct visualization of air flow patterns in in-vitro models with realistic anatomical structures is a big challenge. In this study, we constructed unique half-side transparent physical models of normal UA based on realistic anatomical structures. A smoke-wire method was developed to visualize the air flow in UA models directly. The results revealed that the airflow through the pharynx was laminar but not turbulent under normal inspiration, which suggested that compared with turbulent models, a laminar model should be more suitable in numerical simulations. The flow predicted numerically using the laminar model was consistent with the observations in the physical models. The comparison of the velocity fields predicted numerically using the half-side and complete models confirmed that it was reasonable to investigate the flow behaviors in UA using the half-side model. Using the laminar model, we simulated the flow and evaluated the effects of UA narrowing caused by rostral fluid shift on pharyngeal resistance. The results suggested that fluid shift could play an important role in the formation of hypopnea or OSA during sleep.
Similar content being viewed by others
References
An, Y., Li, Y., Liu, Z., Wang, J., Li, T., Xiong, H., Yin, H., Zhang, X., Xian, J., and Huang, Y. (2015). Effects of fluid shift on upper airway patency and neck circumference in normal-weight subjects. Sleep Med 16, 14-19–1426.
Ball, C.G., Uddin, M., and Pollard, A. (2008). Mean flow structures inside the human upper airway. Flow Turbulence Combust 81, 155–188.
Banko, A.J., Coletti, F., Schiavazzi, D., Elkins, C.J., and Eaton, J.K. (2015). Three-dimensional inspiratory flow in the upper and central human airways. Exp Fluids 56, 117.
Cheng, G.C., Koomullil, R.P., Ito, Y., Shih, A.M., Sittitavornwong, S., and Waite, P.D. (2014). Assessment of surgical effects on patients with obstructive sleep apnea syndrome using computational fluid dynamics simulations. Math Comput Simul 106, 44–59.
Chiu, K.L., Ryan, C.M., Shiota, S., Ruttanaumpawan, P., Arzt, M., Haight, J.S., Chan, C.T., Floras, J.S., and Bradley, T.D. (2006). Fluid shift by lower body positive pressure increases pharyngeal resistance in healthy subjects. Am J Respir Crit Care Med 174, 1378–1383.
Chung, S.K., and Kim, S.K. (2008). Digital particle image velocimetry studies of nasal airflow. Respir Physiol Neurobiol 163, 111–120.
Doorly, D.J., Taylor, D.J., Franke, V.E., and Schroter, R.C. (2008a). Experimental investigation of nasal airflow. Proc Instit Mech Eng Part H 222, 439–453.
Doorly, D.J., Taylor, D.J., Gambaruto, A.M., Schroter, R.C., and Tolley, N. (2008b). Nasal architecture: form and flow. Philos Trans R Soc A Math Phys Eng Sci 366, 3225–3246.
Ferrier, K., Campbell, A., Yee, B., Richards, M., O’Meeghan, T., Weatherall, M., and Neill, A. (2005). Sleep-disordered breathing occurs frequently in stable outpatients with congestive heart failure. Chest 128, 2116–2122.
Goodarzi-Ardakani, V., Taeibi-Rahni, M., Salimi, M.R., and Ahmadi, G. (2016). Computational simulation of temperature and velocity distribution in human upper respiratory airway during inhalation of hot air. Respir Physiol Neurobiol 223, 49–58.
Hahn, I., Scherer, P.W., and Mozell, M.M. (1993). Velocity profiles measured for airflow through a large-scale model of the human nasal cavity. J Appl Physiol 75, 2273–2287.
Hallett, M., Burden, S., Stewart, D., Mahony, J., and Farrell, P. (1995). Sleep apnea in end-stage renal disease patients on hemodialysis and continuous ambulatory peritoneal dialysis. ASAIO J 41, M435–M441.
Heenan, A.F., Matida, E., Pollard, A., and Finlay, W.H. (2003). Experimental measurements and computational modeling of the flow field in an idealized human oropharynx. Exp Fluids 35, 70–84.
Huang, R.H., Li, X.P., and Rong, Q.G. (2013). Control mechanism for the upper airway collapse in patients with obstructive sleep apnea syndrome: a finite element study. Sci China Life Sci 56, 366–372.
Huang, Y., Malhotra, A., and White, D.P. (2005a). Computational simulation of human upper airway collapse using a pressure-/state-dependent model of genioglossal muscle contraction under laminar flow conditions. J Appl Physiol 99, 1138–1148.
Huang, Y., White, D.P., and Malhotra, A. (2005b). The impact of anatomic manipulations on pharyngeal collapse. Chest 128, 1324–1330.
Huang, Y., White, D.P., and Malhotra, A. (2007). Use of computational modeling to predict responses to upper airway surgery in obstructive sleep apnea. Laryngoscope 117, 648–653.
Johnstone, A., Uddin, M., Pollard, A., Heenan, A., and Finlay, W.H. (2004). The flow inside an idealised form of the human extra-thoracic airway. Exp Fluids 37, 673–689.
Kim, S.K., and Chung, S.K. (2004). An investigation on airflow in disordered nasal cavity and its corrected models by tomographic PIV. Meas Sci Technol 15, 1090–1096.
Li, Z., Kleinstreuer, C., and Zhang, Z. (2007). Simulation of airflow fields and microparticle deposition in realistic human lung airway models. Part I: Airflow patterns. Eur J Mech B Fluid 26, 632–649.
Malhotra, A., Huang, Y., Fogel, R.B., Pillar, G., Edwards, J.K., Kikinis, R., Loring, S.H., and White, D.P. (2002). The male predisposition to pharyngeal collapse. Am J Respir Crit Care Med 166, 1388–1395.
Martonen, T.B., Quan, L., Zhang, Z., and Musante, C.J. (2002). Flow simulation in the human upper respiratory tract. Cell Biochem Biophys 37, 27–36.
Moriwaki, H., Inoue, Y., Namba, K., Suto, Y., Chiba, S., and Moriyama, H. (2009). Clinical significance of upper airway obstruction pattern during apneic episodes on ultrafast dynamic magnetic resonance imaging. Auris Nasus Larynx 36, 187–191.
Mylavarapu, G., Murugappan, S., Mihaescu, M., Kalra, M., Khosla, S., and Gutmark, E. (2009). Validation of computational fluid dynamics methodology used for human upper airway flow simulations. J Biomech 42, 1553–1559.
Phuong, N.L., and Ito, K. (2015). Investigation of flow pattern in upper human airway including oral and nasal inhalation by PIV and CFD. Building Environ 94, 504–515.
Shinneeb, A.M., and Pollard, A. (2012). Identification of vortical structures inside the human pharynx/larynx region from POD-reconstructed velocity fields. Exp Fluids 53, 353–367.
Shiota, S., Ryan, C.M., Chiu, K.L., Ruttanaumpawan, P., Haight, J., Arzt, M., Floras, J.S., Chan, C., and Bradley, T.D. (2007). Alterations in upper airway cross-sectional area in response to lower body positive pressure in healthy subjects. Thorax 62, 868–872.
Sittitavornwong, S., Waite, P.D., Shih, A.M., Cheng, G.C., Koomullil, R., Ito, Y., Cure, J.K., Harding, S.M., and Litaker, M. (2013). Computational fluid dynamic analysis of the posterior airway space after maxillomandibular advancement for obstructive sleep apnea syndrome. J Oral Maxillofac Surg 71, 1397–1405.
Wang, C., Zhang, H., Lin, H., Xu, H., Hu, G., Li, Z., and Huang, Y. (2016). Using MRI to study effects of fluid shift on the cross-sectional shape of the upper airway in obstructive sleep apnea patients. Beijing Biomed Eng 35, 31–35.
Weinhold, I., and Mlynski, G. (2004). Numerical simulation of airflow in the human nose. Eur Arch Otorhinolaryngol 261, 452–455.
White, F.M. (2009). Fluid Mechanics. (New York: McGraw-Hill Companies, Inc.).
Young, T., Peppard, P.E., and Gottlieb, D.J. (2002). Epidemiology of obstructive sleep apnea. Am J Respir Crit Care Med 165, 1217–1239.
Acknowledgements
This work was supported by the National Nature Science Foundation of China (31670959, 81171422), the National Science and Technology Pillar Program of China (2012BAI05B03), the Key Projects in Science and Technology Program of Beijing Municipal Education Commission, China (KZ201210025022), Beijing Postdoctoral Research Foundation (2016ZZ-45) and Beijing Key Laboratory of Fundamental Research on Biomechanics in Clinical Application.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wu, H., Wang, M., Wang, J. et al. Direct visualizations of air flow in the human upper airway using in-vitro models. Sci. China Life Sci. 62, 235–243 (2019). https://doi.org/10.1007/s11427-018-9373-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11427-018-9373-y