Abstract
Objectives
18F-NaF is a bone scanning radiotracer that reflects changes in bone metabolism, and it is applied in oncology to scan bone tumors or metastasis. Dentomaxillofacial alterations can lead to 18F-NaF uptake and could lead to false-positive results in PET/CT examinations. Hence, the objective of this research was to verify if the uptake of 18F-NaF in the mandible or maxilla is correlated to the presence of odontogenic alterations, which could lead to false-positive results in positron emission tomography/computerized tomography (PET/CT) examinations.
Methods
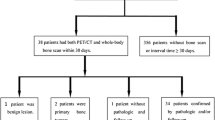
42 patients who underwent 18F-NaF PET/CT examinations and panoramic radiographs to detect bone metastasis and to assess oral conditions before oncologic treatment were included. Edentulous patients and patients with neoplasms in the maxillofacial area, and those whose imaging examinations had technical failures were excluded from the study.
Results
A total of 252 areas from panoramic radiographs and PET/CT examinations were assessed. It was observed that the presence of periodontal bone loss resulted in a higher number of cases with false negatives. Accuracy, sensitivity, and specificity of 18F-NaF uptake—regardless of the type of odontogenic origin alteration—were 76.2%, 53.3%, and 89.4%, respectively.
Conclusion
18F-NaF uptake in the maxilla or mandible could be influenced by oral alterations in the alveolar bones. The alterations in the oral cavity that lead to 18F-NaF accumulation should be recognized by medical radiologists to prevent false-positive results in PET/CT examinations using the tracer 18F-NaF.



Similar content being viewed by others
References
Eekhoff EMW, Botman E, Coen Netelenbos J, Graaf P, Bravenboer N, Micha D, et al. [18F]NaF PET/CT scan as an early marker of heterotopic ossification in fibrodysplasiaossificansprogressiva. Bone. 2018;109:143–6.
Ideguchi H, Yamashiro K, Yamamoto T, Shimoe M, Hongo S, Kochi S, et al. Molecular imaging assessment of periodontitis lesions in an experimental mouse model. Clin Oral Investig. 2019;23:821–7.
Ullmark G, Sörensen J, Maripuu E, Nilsson O. Fingerprint pattern of bone mineralisation on cemented and uncemented femoral stems: analysis by [18F]-fluoride-PET in a randomised clinical trial. Hip In. 2019;29:609–17.
Kim Y, Lee HY, Yoon HJ, Kim BS. Utility of 18F-fluorodeoxy glucose and 18F-sodium fluoride positron emission tomography/computed tomography in the diagnosis of medication-related osteonecrosis of the jaw: a preclinical study in a rat model. J CraniomaxillofacSurg. 2016;44:357–63.
Even-Sapir E, Metser U, Flusser G, Kollender Y, Lerman H, Lievshitz G, et al. Assessment of malignant skeletal disease: initial experience with 18F-fluoride PET/CT and comparison between 18F-fluoride PET and 18F-fluoride PET/CT. J Nucl Med. 2004;45:272–8.
Blau M, Nagler W, Bender MA. Fluorine-18: a new isotope for bone scanning. J Nucl Me. 1962;3:332–4.
Beheshti M. F-sodium fluoride PET/CT and PET/MR imaging of bone and joint disorders. PET Clin. 2018;13:477–90.
Kulshrestha RK, Vinjamuri S, England A, Nightingale J, Hogg P. The role of 18F-sodium fluoride PET/CT bone scans in the diagnosis of metastatic bone disease from breast and prostate cancer. J Nucl Med Technol. 2016;44:217–22.
Drubach LA, Johnston PR, Newton AW, Perez-Rossello JM, Grant FD, Kleinman PK. Skeletal trauma in child abuse: detection with 18F-NaF PET. Radiology. 2010;255:173–81.
Suenaga H, Yokoyama M, Yamaguchi K, Sasaki K. Time course of bone metabolism at the residual ridge beneath dentures observed using 18F-fluoride positron emission computerized-tomography/computed tomography (PET/CT). Ann Nucl Med. 2012;26:817–22.
Sasaki H, Koyama S, Yokoyama M, Yamaguchi K, Itoh M, Sasaki K. Bone metabolic activity around dental implants under loading observed using bone scintigraphy. Int J Oral Maxillofac Implants. 2008;23:827–34.
Yamashiro K, Nakano M, Sawaki K, Okazaki F, Hirata Y, Takashiba S. The potential of positron emission tomography/computerized tomography (PET/CT) scanning as a detector of high-risk patients with oral infection during preoperative staging. Oral Surg Oral Med Oral Pathol Oral Radiol. 2016;122:242–9.
Thomas MV, Puleo DA. Infection, inflammation, and bone regeneration: a paradoxical relationship. J Dent Res. 2011;90:1052–61.
Ebersole JL, Dawson D, Emecen-Huja P, et al. The periodontal war: microbes and immunity. Periodontol. 2017;75:52–115.
Santos SCLT, Couto LA, Fonseca JM, Xavier FCA, Figueiredo ACL, Freitas VS, et al. Participation of osteoclastogenic factors in immunopathogenesis of human chronic periapical lesions. J Oral Pathol Med. 2017;46:846–52.
Weber M, Ries J, Büttner-Herold M, Geppert CI, Kesting M, Wehrhan F. Differences in inflammation and bone resorption between apical granulomas, radicular cysts, and dentigerous cysts. J Endod. 2019;45:1200–8.
Mantovani A, Sica A, Locati M. New vistas on macrophage differentiation and activation. Eur J Immunol. 2007;37:14–6.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Luciana Munhoz, Mayara Aguilar Dias de Brito, Marcelo Taiti Sapienza and Emiko Saito Arita declares no conflicts of interest.
Ethical approval
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008 (5). Ethics approval was obtained obtained in the Ethics Committee of Dentistry and Medical School (number 1641/2020), and the Declaration of Helsinki guidelines were followed in this investigation.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Munhoz, L., de Brito, M.A.D., Arita, E.S. et al. 18F-NaF uptake in dentomaxillofacial bones as a result of oral alterations: a positron emission tomography/computerized tomography scanning study. Oral Radiol 37, 669–676 (2021). https://doi.org/10.1007/s11282-020-00509-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11282-020-00509-z