Abstract
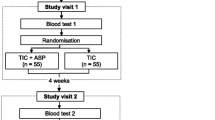
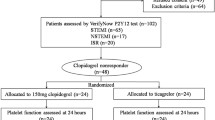
Early clustering of adverse cardiovascular events after abrupt cessation of clopidogrel has been reported in patients with acute coronary syndromes. A platelet rebound phenomenon may contribute to this increased thrombotic risk and a gradual drug tapering may attenuate this proposed platelet effect. Accordingly, we aimed to assess the effect of clopidogrel tapering on platelet reactivity. Twenty patients who underwent elective percutaneous coronary interventions with bare metal stents receiving 3 months of clopidogrel therapy (75 mg daily) were randomized to either of two discontinuation strategies: (1) Off group–abrupt drug cessation or (2) Tapering group–receiving clopidogrel 75 mg every other day for 4 weeks duration. Light transmission aggregometry, induced by ADP (5 and 10 μM) and collagen, was measured at four time-points (at baseline and 2, 4 and 6 weeks after randomization). In the off group, there was an early rise in platelet reactivity at 2 weeks after abrupt drug cessation compared to baseline, as measured by ADP 5 μmol/l (39.6 ± 2.8 vs. 67.9 ± 6.0, P < 0.001). The tapering regimen suppressed this rebound platelet aggregation by ADP 5 μmol/l at 2 weeks (P = 0.001) and 4 weeks (P = 0.001). Similar results were found with ADP 10 μmol/l and collagen agonists. Abrupt cessation of clopidogrel results in an early rise in platelet aggregability in patients with BMS that is attenuated by a tapering regimen. Clopidogrel administration every other day may achieve similar levels of platelet inhibition as full dose therapy. Further investigations evaluating clopidogrel tapering strategies and their potential clinical impact are warranted.

Similar content being viewed by others
Abbreviations
- MI:
-
Myocardial infarction
- DES:
-
Drug eluting stent
- BMS:
-
Bare metal stent
- PCI:
-
Percutaneous coronary intervention
- ACS:
-
Acute coronary syndrome
- LTA:
-
Light transmission aggregometry
- PRP:
-
Platelet-rich plasma
- CAD:
-
Coronary artery disease
References
Yusuf S, Zhao F, Mehta SR, Chrolavicius S, Tognoni G, Fox KK (2001) Effects of clopidogrel in addition to aspirin in patients with acute coronary syndromes without ST-segment elevation. N Engl J Med 345:494–502
Steinhubl SR, Berger PB, Mann JT 3rd et al (2002) Early and sustained dual oral antiplatelet therapy following percutaneous coronary intervention: a randomized controlled trial. JAMA 288:2411–2420
Anderson JL, Adams CD, Antman EM et al (2007) ACC/AHA 2007 guidelines for the management of patients with unstable angina/non-ST-Elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines (Writing Committee to revise the 2002 guidelines for the management of patients with unstable angina/non-ST-elevation myocardial infarction) developed in collaboration with the American College of Emergency Physicians, the Society for Cardiovascular Angiography and Interventions, and the Society of Thoracic Surgeons endorsed by the American Association of Cardiovascular and Pulmonary Rehabilitation and the Society for Academic Emergency Medicine. J Am Coll Cardiol 50:e1–e157
Kushner FG, Hand M, Smith SC Jr et al (2009) 2009 focused updates: ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction (updating the 2004 guideline and 2007 focused update) and ACC/AHA/SCAI guidelines on percutaneous coronary intervention (updating the 2005 guideline and 2007 focused update) a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 54:2205–2241
Smith SC Jr, Feldman TE, Hirshfeld JW Jr et al (2006) ACC/AHA/SCAI 2005 guideline update for percutaneous coronary intervention-summary article: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (ACC/AHA/SCAI Writing Committee to update the 2001 guidelines for percutaneous coronary intervention). J Am Coll Cardiol 47:216–235
Ho PM, Peterson ED, Wang L et al (2008) Incidence of death and acute myocardial infarction associated with stopping clopidogrel after acute coronary syndrome. JAMA 299:532–539
Iakovou I, Schmidt T, Bonizzoni E et al (2005) Incidence, predictors, and outcome of thrombosis after successful implantation of drug-eluting stents. JAMA 293:2126–2130
Jeremias A, Sylvia B, Bridges J et al (2004) Stent thrombosis after successful sirolimus-eluting stent implantation. Circulation 109:1930–1932
Spertus JA, Kettelkamp R, Vance C et al (2006) Prevalence, predictors, and outcomes of premature discontinuation of thienopyridine therapy after drug-eluting stent placement: results from the PREMIER registry. Circulation 113:2803–2809
Valgimigli M, Campo G, Arcozzi C et al (2007) Two-year clinical follow-up after sirolimus-eluting versus bare-metal stent implantation assisted by systematic glycoprotein IIb/IIIa inhibitor infusion in patients with myocardial infarction: results from the STRATEGY study. J Am Coll Cardiol 50:138–145
Angiolillo DJ, Fernandez-Ortiz A, Bernardo E et al (2006) Clopidogrel withdrawal is associated with proinflammatory and prothrombotic effects in patients with diabetes and coronary artery disease. Diabetes 55:780–784
Buonamici P, Marcucci R, Migliorini A et al (2007) Impact of platelet reactivity after clopidogrel administration on drug-eluting stent thrombosis. J Am Coll Cardiol 49:2312–2317
Hochholzer W, Trenk D, Bestehorn HP et al (2006) Impact of the degree of peri-interventional platelet inhibition after loading with clopidogrel on early clinical outcome of elective coronary stent placement. J Am Coll Cardiol 48:1742–1750
Sibbing D, Stegherr J, Braun S et al (2010) A double-blind, randomized study on prevention and existence of a rebound phenomenon of platelets after cessation of clopidogrel treatment. J Am Coll Cardiol 55:558–565
Geraghty OC, Paul NL, Chandratheva A, Rothwell PM (2010) Low risk of rebound events after a short course of clopidogrel in acute TIA or minor stroke. Neurology 74:1891–1896
Trenk D, Hochholzer W, Fromm MF et al (2008) Cytochrome P450 2C19 681G > A polymorphism and high on-clopidogrel platelet reactivity associated with adverse 1 year clinical outcome of elective percutaneous coronary intervention with drug-eluting or bare-metal stents. J Am Coll Cardiol 51:1925–1934
Savi P, Pereillo JM, Uzabiaga MF et al (2000) Identification and biological activity of the active metabolite of clopidogrel. Thromb Haemost 84:891–896
Conflict of interest
There are no potential sources of conflict for this research.
Funding
There are no sources of financial support for this research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yedidya, I., Netzer, A., Vaduganathan, M. et al. Clopidogrel tapering as a strategy to attenuate platelet rebound phenomenon in patients with bare-metal stents. J Thromb Thrombolysis 33, 16–21 (2012). https://doi.org/10.1007/s11239-011-0652-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-011-0652-z