Abstract
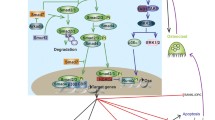
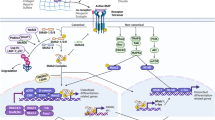
Skeletal homeostasis is determined by systemic hormones and local factors. Bone morphogenetic proteins (BMPs) are unique because they induce the commitment of mesenchymal cells toward cells of the osteoblastic lineage and also enhance the differentiated function of the osteoblast. BMP activities in bone are mediated through binding to specific cell surface receptors and through interactions with other growth factors. BMPs are required for skeletal development and maintenance of adult bone homeostasis, and play a role in fracture healing. BMPs signal by activating the mothers against decapentaplegic (Smad) and mitogen activated protein kinase (MAPK) pathways, and their actions are tempered by intracellular and extracellular proteins. The BMP antagonists block BMP signal transduction at multiple levels including pseudoreceptor, inhibitory intracellular binding proteins, and factors that induce BMP ubiquitination. A large number of extracellular proteins that bind BMPs and prevent their binding to signaling receptors have emerged. The extracellular antagonists are differentially expressed in cartilage and bone tissue and exhibit BMP antagonistic as well as additional activities. Both intracellular and extracellular antagonists are regulated by BMPs, indicating the existence of local feedback mechanisms to modulate BMP cellular activities.
Similar content being viewed by others
References
Canalis E, Economides AN, Gazzerro E. Bone morphogenetic proteins, their antagonists, and the skeleton. Endocr Rev 2003;24:218–35.
Chen D, Zhao M, Mundy GR. Bone morphogenetic proteins. Growth Factors 2004;22:233–41.
Cao X, Chen D. The BMP signaling and in vivo bone formation. Gene 2005;357:1–8.
Kishigami S, Mishina Y. BMP signaling and early embryonic patterning. Cytokine Growth Factor Rev 2005;16:265–78.
Miyazono K, Maeda S, Imamura T. BMP receptor signaling: transcriptional targets, regulation of signals, and signaling cross-talk. Cytokine Growth Factor Rev 2005;16:251–63.
Gupta MC, Khan SN. Application of bone morphogenetic proteins in spinal fusion. Cytokine Growth Factor Rev 2005; 16:347–55.
Seeherman H, Wozney JM. Delivery of bone morphogenetic proteins for orthopedic tissue regeneration. Cytokine Growth Factor Rev 2005;16:329–45.
Anderson HC, Hodges PT, Aguilera XM, Missana L, Moylan PE. Bone morphogenetic protein (BMP) localization in developing human and rat growth plate, metaphysis, epiphysis, and articular cartilage. J Histochem Cytochem 2000;48:1493–502.
Pereira RC, Rydziel S, Canalis E. Bone morphogenetic protein-4 regulates its own expression in cultured osteoblasts. J Cell Physiol 2000;182:239–46.
Helvering LM, Sharp RL, Ou X, Geiser AG. Regulation of the promoters for the human bone morphogenetic protein 2 and 4 genes. Gene 2000;256:123–38.
Ducy P, Starbuck M, Priemel M, Shen J, Pinero G, Geoffroy V, et al. A Cbfa1-dependent genetic pathway controls bone formation beyond embryonic development. Genes Dev 1999; 13:1025–36.
Komori T, Yagi H, Nomura S, Yamaguchi A, Sasaki K, Deguchi K, et al. Targeted disruption of Cbfa1 results in a complete lack of bone formation owing to maturational arrest of osteoblasts. Cell 1997;89:755–64.
Liu W, Toyosawa S, Furuichi T, Kanatani N, Yoshida C, Liu Y, et al. Overexpression of Cbfa1 in osteoblasts inhibits osteoblast maturation and causes osteopenia with multiple fractures. J Cell Biol 2001;155:157–66.
Canalis E, Gabbitas B: Bone morphogenetic protein increases insulin like growth factor I and II synthesis in bone cell cultures. J Bone Miner Res 1994;9:1999–2005.
Nohe A, Keating E, Underhill TM, Knaus P, Petersen NO. Dynamics and interaction of caveolin-1 isoforms with BMP-receptors. J Cell Sci 2005;118:643–50.
Nohe A, Hassel S, Ehrlich M, Neubauer F, Sebald W, Henis YI, et al. The mode of bone morphogenetic protein (BMP) receptor oligomerization determines different BMP-2 signaling pathways. J Biol Chem 2002;277:5330–8.
Nishimura R, Hata K, Ikeda F, Matsubara T, Yamashita K, Ichida F, et al. The role of Smads in BMP signaling. Front Biosci 2003;8:s275–84.
Nohe A, Keating E, Knaus P, Petersen NO. Signal transduction of bone morphogenetic protein receptors. Cell Signal 2004;16(3):291–9.
Lai C-F, Cheng S-L. Signal transductions induced by bone morphogenetic protein-2 and transforming growth factor-β in normal human osteoblastic cells. J Biol Chem 2002;277:15514–22.
Samad TA, Rebbapragada A, Bell E, Zhang Y, Sidis Y, Jeong S-J, et al. DRAGON, a bone morphogenetic protein co-receptor. J Biol Chem 2005;280:14122–9.
Babitt JL, Zhang Y, Samad TA, Xia Y, Tang J, Campagna JA, et al. Repulsive guidance molecule (RGMa), a DRAGON homologue, is a bone morphogenetic protein co-receptor. J Biol Chem 2005;280:29820–7.
Westendorf JJ, Kahler PA, Schroeder TM. Wnt signaling in osteoblasts and bone diseases. Gene 2004;341:19–39.
Gong Y, Slee RB, Fukai N, Rawadi G, Roman-Roman S, Reginato AM, et al. LDL receptor-related protein 5 (LRP5) affects bone accrual and eye development. Cell 2001;107:513–23.
Hu H, Hilton MJ, Tu X, Yu K, Ornitz DM, Long F. Sequential roles of Hedgehog and Wnt signaling in osteoblast development. Development 2005;132:49–60.
Holmen SL, Zylstra CR, Mukherjee A, Sigler RE, Faugere MC, Bouxsein ML, et al. Essential role of beta-catenin in postnatal bone acquisition. J Biol Chem 2005;280:21162–8.
Koay MA, Brown MA. Genetic disorders of the LRP5-Wnt signalling pathway affecting the skeleton. Trends Mol Med 2005;11:129–37.
Hussein SM, Duff EK, Sirard C. Smad4 and β-catenin co-activators functionally interact with lymphoid-enhancing factor to regulate graded expression of Msx2. J Biol Chem 2003;278:48805–14.
de Jong DS, Vaes BL, Dechering KJ, Feijen A, Hendriks JM, Wehrens R, et al. Identification of novel regulators associated with early-phase osteoblast differentiation. J Bone Miner Res 2004;19:947–58.
Rawadi G, Vayssiere B, Dunn F, Baron R, Roman-Roman S. BMP-2 controls alkaline phosphatase expression and osteoblast mineralization by a Wnt autocrine loop. J Bone Miner Res 2003;18:1842–53.
Winkler DG, Sutherland MS, Ojala E, Turcott E, Geoghegan JC, Shpektor D, et al. Sclerostin inhibition of Wnt-3a-induced C3H10T1/2 cell differentiation is indirect and mediated by bone morphogenetic proteins. J Biol Chem 2005;280:2498–502.
He XC, Zhang J, Tong WG, Tawfik O, Ross J, Scoville DH, et al. BMP signaling inhibits intestinal stem cell self-renewal through suppression of Wnt-beta-catenin signaling. Nat Genet 2004;36:1117–21.
de Jong DS, van Zoelen EJ, Bauerschmidt S, Olijve W, Steegenga WT. Microarray analysis of bone morphogenetic protein, transforming growth factor beta, and activin early response genes during osteoblastic cell differentiation. J Bone Miner Res 2002;17:2119–29.
Pereira RC, Delany AM, Canalis E. CCAAT/enhancer binding protein homologous protein (DDIT3) induces osteoblastic cell differentiation. Endocrinology 2004;145(4):1952–60, Apr.
Pereira RC, Stadmeyer L, Marciniak SJ, Ron D, Canalis E. C/EBP homologous protein is necessary for normal osteoblastic function. J Cell Biochem 2006;97:633–40.
Zhang H, Bradley A. Mice deficient for BMP-2 are nonviable and have defects in amnion/chorion and cardiac development. Development 1996;122:2977–86.
Winnier G, Blessing M, Labosky PA, Hogan BLM. Bone morphogenetic protein-4 is required for mesoderm formation and patterning in the mouse. Genes Dev 1995;9:2105–16.
Daluiski A, Engstrand T, Bahamonde ME, Gamer LW, Agius E, Stevenson SL, et al. Bone morphogenetic protein-3 is a negative regulator of bone density. Nat Genet 2001;27:84–8.
Solloway MJ, Dudley AT, Bikoff EK, Lyons KM, Hogan BL, Robertson EJ. Mice lacking Bmp6 function. Dev Genet 1998;22:321–39.
Luo G, Hofmann C, Bronchers AJ, Sohocki M, Bradley A, Karsenty G. BMP-7 is an inducer of nephrogenesis, and is also required for eye development and skeletal patterning. Genes Dev 1995;9:2808–20.
Cox K, Harfe B, Tabin CJ, Rosen V. Absence of both Bmp2 and Bmp4 during skeletal development results in severe defects in osteoblasts but not in chondrocytes. J Bone Miner Res 2004;19:S11.
Guo D, Harris S, Ying W, Zhang J, Feng J, Anderson C, et al. Bmp4 is necessary for bone formation: conditional Bmp4 knock-out using the 3.6 kb and 2.3 kb collagen 1a1 promoter-Cre and Bmp4-floxed mice. J Bone Miner Res 2004;19:S14.
Mishina Y, Suzuki A, Ueno N, Behringer RB. Bmpr encodes a type I bone morphogenetic protein receptor that is essential for gastrulation during mouse embryogenesis. Genes Dev 1995;9:3027–37.
Zhang J, Niu C, Ye L, Huang H, He X, Tong WG, et al. Identification of the haematopoietic stem cell niche and control of the niche size. Nature 2003;425:836–41.
Chen D, Ji X, Harris MA, Feng JQ, Karsenty G, Celeste AJ, et al. Differential roles for BMP receptor type IB and IA in differentiation and specification of mesenchymal precursor cells to osteoblast and adipocyte lineages. J Cell Biol 1998;142:295–305.
Yi SE, Daluiski A, Pederson AR, Rosen V, Lyons KM. The type I BMP receptor BMPRIB is required for chondrogenesis in the mouse limb. Development 2000;127:621–30.
Zhao M, Harris SE, Horn D, Geng Z, Nishimura R, Mundy GR, et al. Bone morphogenetic protein receptor signaling is necessary for normal murine postnatal bone formation. J Cell Biol 2002;157:1049–60.
Tremblay KD, Dunn NR, Robertson E. Mouse embryos lacking Smad1 signals display defects in extra-embryonic tissues and germ cell formation. Development 2001;128:3609–21.
Chen D, et al. BMP signaling through the Smad1 pathway is required for normal postnatal bone formation. J Bone Miner Res 2003;18:S6.
Storm EE, Huynh TV, Copeland NG, Jenkins NA, Kingsley DM, Lee SJ. Limb alterations in brachypodism mice due to mutations in a new member of the TGF β superfamily. Nature 1994;368:639–43.
Thomas JT, Lin K, Nandedkar M, Camargo M, Cervenka J, Luyten FP. A human chondrodysplasia due to a mutation in a TGF β superfamily member. Nat Genet 1996;12:315–7.
Lehmann K, Seemann P, Stricker S, Sammar M, Meyer B, Suring K, et al. Mutations in bone morphogenetic protein receptor 1B cause brachydactyly type A2. Proc Natl Acad Sci USA 2003;100:12277–82.
Demirhan O, Turkmen S, Schwabe GC, Soyupak S, Akgul E, Tastemir D, et al. A homozygous BMPR1B mutation causes a new subtype of acromesomelic chondrodysplasia with genital anomalies. J Med Genet 2005;42:314–7.
Gannon FH, Kaplan FS, Olmsted E, Finkel GC, Zasloff MA, Shore E. Bone morphogenetic protein 2/4 in early fibromatous lesions of fibrodysplasia ossificans progressiva. Human Pathol 1997;28:339–43.
de la Pena LS, Billings PC, Fiori JL, Ahn J, Kaplan FS, Shore EM. Fibrodysplasia ossificans progressiva (FOP), a disorder of ectopic osteogenesis, misregulates cell surface expression and trafficking of BMPRIA. J Bone Miner Res 2005;20:1168–76.
Vitt UA, Hsu SY, Hsueh AJW. Evolution and classification of cystine knot-containing hormones and related extracellular signaling molecules. Mol Endocrinol 2001;15:681–94.
Avsian-Kretchmer O, Hsueh AJ. Comparative genomic analysis of the eight-membered ring cystine knot-containing bone morphogenetic protein antagonists. Mol Endocrinol 2004;18: 1–12.
Zimmerman LB, DeJesus-Escobar JM, Harland RM. The Spemann organizer signal noggin binds and inactivates bone morphogenetic protein 4. Cell 1996;86:599–606.
Groppe J, Greenwald J, Wiater E, Rodriguez-Leon J, Economides AN, Kwiatkowski W, et al. Structural basis of BMP signaling inhibition by the cystine knot protein noggin. Nature 2002;420:636–42.
Gazzerro E, Gangji V, Canalis E. Bone morphogenetic proteins induce the expression of noggin, which limits their activity in cultured rat osteoblasts. J Clin Invest 1998;102:2106–14.
Pathi S, Rutenberg JB, Johnson RL, Vortkamp A. Interaction of Ihh and BMP/noggin signaling during cartilage differentiation. Dev Biol 1999;209:239–53.
Abe E, Yamamoto M, Taguchi Y, Lecka-Czernik B, O’Brien C, Economides AN, et al. Essential requirement of BMPs-2/4 for both osteoblast and osteoclast formation in murine bone marrow cultures from adult mice: antagonism by noggin. J Bone Miner Res 2000;15:663–73.
Devlin RD, Du Z, Pereira RC, Kimble RB, Economides AN, Jorgetti V, et al. Skeletal over-expression of noggin results in osteopenia and reduced bone formation. Endocrinology 2003;144:1972–8.
Brunet LJ, McMahon JA, McMahon AP, Harland RM. Noggin, cartilage morphogenesis, and joint formation in the mammalian skeleton. Science 1998;280:1455–7.
McMahon JA, Takada S, Zimmerman LB, Fan C-M, Harland RM, McMahon AP. Noggin-mediated antagonism of BMP signaling is required for growth and patterning of the neural tube and somite. Genes Dev 1998;12:1438–52.
Wijgerde M, Karp S, McMahon J, McMahon AP. Noggin antagonism of BMP4 signaling controls development of the axial skeleton in the mouse. Dev Biol 2003;286:149–57.
Warren SM, Brunet LJ, Harland RM, Economides AN, Longaker MT. The BMP antagonist noggin regulates cranial suture fusion. Nature 2003;422:625–9.
Gong Y, Krakow D, Marcelino J, Wilkin D, Chitavat D, Babul-Himi R, et al. Heterozygous mutations in the gene encoding noggin affect human joint morphogenesis. Nature Genetics 1999;21:302–4.
Marcelino J, Sciortino CM, Romero MF, Ulatowski LM, Ballock RT, Economides AN, et al. Human disease-causing NOG missense mutations: effects on noggin secretion, dimer formation, and bone morphogenetic protein binding. Proc Natl Acad Sci USA 2001;98:11353–8.
Xu M-Q, Feldman G, Le Merrer M, Shugart YY, Glaser DL, Uritzberea JA, et al. Linkage exclusion and mutational analysis of the noggin gene in patients with fibrodysplasia ossificans progressiva (FOP). Clin Genet 2000;58:291–8.
Glaser DL, Economides AN, Wang L, Liu X, Kimble RD, Fandl JP, et al. In vivo somatic cell gene transfer of an engineered Noggin mutein prevents BMP4-induced heterotopic ossification. J Bone Jt Surg 2003;85:2332–42.
Lories RJ, Derese I, Luyten FP. Modulation of bone morphogenetic protein signaling inhibits the onset and progression of ankylosing enthesitis. J Clin Invest 2005;115:1571–9.
Piccolo S, Sasai Y, Lu B, De Robertis EM. Dorsoventral patterning in Xenopus: inhibition of ventral signals by direct binding of chordin to BMP-4. Cell 1997;86:589–98.
Piccolo S, Agius E, Lu B, Goodman S, Dale L, De Robertis EM. Cleavage of chordin by xolloid metalloprotease suggests a role for proteolytic processing in the regulation of Spemann organizer activity. Cell 1997;91:407–16.
Scott IC, Blitz IL, Pappano WN, Imamura Y, Clark TG, Steiglitz BM, et al. Mammalian BMP-1/tolloid-related metalloproteinases, including novel family member mammalian tolloid-like 2, have differential enzymatic activities and distributions of expression relevant to patterning and skeletogenesis. Dev Biol 1999;283–300.
Reynolds SD, Zhang D, Puzas JE, O’Keefe RJ, Rosier RN, Reynolds PR. Cloning of the chick BMP1/tolloid cDNA and expression in skeletal tissues. Gene 2000;248:233–43.
Suzuki N, Labosky PA, Furuta Y, Hargett L, Dunn R, Fogo AB, et al. Failure of ventral body wall closure in mouse embryos lacking a procollagen C-proteinase encoded by Bmp1, a mammalian gene related to Drosophila tolloid. Development 1996;122:3587–95.
Oelgeschlager M, Larrain J, Geissert D, De Robertis EM. The evolutionarily conserved BMP-binding protein twisted gastrulation promotes BMP signalling. Nature 2000;405:757–63.
Lee HX, Ambrosio AL, Reversade, De Robertis EM. Embryonic dorsal-ventral signaling: secreted frizzled-related proteins as inhibitors of tolloid proteinases. Cell 2006;124:147–59.
Jasuja R, Allen BL, Pappano WN, Rapraeger AC, Greenspan DS. Cell-surface heparan sulfate proteoglycans potentiate chordin antagonism of bone morphogenetic protein signaling and are necessary for cellular uptake of chordin. J Biol Chem 2004; 279:51289–97.
Moreno M, Munoz R, Aroca F, Labrca M, Brandan M, Larrain J. Biglycan is a new extracellular component of the Chordin-BMP4 signaling pathway. EMBO J 2005;24:1397–405.
Zhang D, Ferguson CM, O’Keefe RJ, Puzas JE, Rosier RN, Reynolds PR. A role for the BMP antagonist chordin in endochondral ossification. J Bone Miner Res 2002;17:293–300.
Bachiller D, Klingensmith J, Kemp C, Belo JA, Anderson RM, May SR, et al. The organizer factors chordin and noggin are required for mouse forebrain development. Nature 2000;403:658–61.
Garcia Abreu J, Coffinier C, Larrain J, Oelgeschlager M, De Robertis EM. Chordin-like CR domains and the regulation of evolutionarily conserved extracellular signaling systems. Gene 2002;287:39–47.
Parisi MS, Gazzerro E, Rydziel S, Canalis E. Expression and regulation of CCN genes in murine osteoblasts Bone. 2005 Nov 24; [Epub ahead of print].
Luo Q, Kang Q, Si W, Jiang W, Park JK, Peng Y, et al. Connective tissue growth factor (CTGF) is regulated by Wnt and bone morphogenetic proteins signaling in osteoblast differentiation of mesenchymal stem cells. J Biol Chem 2004;279:55958–68.
Ivkovic S, Yoon BS, Popoff SN, Safadi FF, Libuda DE, Stephenson RC, et al. Connective tissue growth factor coordinates chondrogenesis and angiogenesis during skeletal development. Development 2003;130:2779–91.
French DM, Kaul RJ, D’Souza AL, Crowley CW, Bao M, Frantz GD, et al. WISP-1 is an osteoblastic regulator expressed during skeletal development and fracture repair. Am J Pathol 2004; 165:855–67.
Mason ED, Konrad KD, Webb CD, Marsh JL. Dorsal midline fate in Drosophila embryo requires twisted gastrulation, a gene encoding a secreted protein related to human connective tissue growth factor. Genes Dev 1994;8:1489–501.
Ross JJ, Shimmi O, Vilmos P, Petryk A, Kim H, Gaudenz K, et al. Twisted gastrulation is a conserved extracellular BMP antagonist. Nature 2001;410:479–83.
Chang C, Holtzman DA, Chau S, Chickering T, Woolf EA, Holmgren LM, et al. Twisted gastrulation can function as a BMP antagonist. Nature 2001;410:483–7.
Scott IC, Blitz IL, Pappano WN, Maas SA, Cho KW, Greenspan DS. Homologues of twisted gastrulation are extracellular cofactors in antagonism of BMP signaling. Nature 2001;410: 475–8.
Wills A, Harland RM, Khokha MK. Twisted gastrulation is required for forebrain specification and cooperates with Chordin to inhibit BMP signaling during X. tropicalis gastrulation. Dev Biol 2006;289:166–78.
Larrain J, Oelgeschlager M, Ketpura NI, Reversade B, Zakin L, De Robertis EM. Proteolytic cleavage of chordin as a switch for the dual activities of Twisted gastrulation in BMP signaling. Development 2001;128:4439–47.
Oelgeschlager M, Reversade B, Larrain J, Little S, Mullins MC, De Robertis EM. The pro-BMP activity of twisted gastrulation is independent of BMP binding. Development 2003;130:4047–56.
Nosaka T, Morita S, Kitamura H, Nakajima H, Shibata F, Morikawa Y, et al. Mammalian twisted gastrulation is essential for skeleto-lymphogenesis. Mol Cell Biol 2003;23:2969–80.
Petryk A, Anderson RM, Jarcho MP, Leaf I, Carlson CS, Klingensmith J, et al. The mammalian twisted gastrulation gene functions in foregut and craniofacial development. Dev Biol 2004;267:374–86.
Zakin L, De Robertis EM: Inactivation of mouse twisted gastrulation reveals its role in promoting BMP4 activity during forebrain development. Development 2004;131:413–24.
Zakin L, Reversade B, Kuroda H, Lyons KM, De Robertis EM. Sirenomelia in Bmp 7 and Tsg compound mutant mice: requirements for Bmp signaling in the development of ventral posterior mesoderm. Development 2005;132:2489–99.
Gazzerro E, Deregowski V, Vaira S, Canalis E. Overexpression of twisted gastrulation inhibits bone morphogenetic protein action and prevents osteoblast cell differentiation in vitro. Endocrinology 2005;146:3875–82.
Petryk A, Shimmi O, Jia X, Carlson AE, Tervonen L, Jarcho MP, et al. Twisted gastrulation and chordin inhibit differentiation and mineralization in MC3T3-E1 osteoblast-like cells. Bone 2005; 36:617–26.
Gazzerro E, Deregowski V, Stadmeyer L, Economides AN, Canalis E. Twisted gastrulation is a bone morphogenetic protein agonist in cartilage but not in bone. Proceedings of the Abstract 25th Annual Meeting American Society of Bone and Mineral Research (http://www.asbmr.org/meeting/abstracts.cfm).
Hsu DR, Economides AN, Wang X, Eimon PM, Harland RM. The Xenopus dorsalizing factor gremlin identifies a novel family of secreted proteins that antagonize BMP activities. Mol Cell 1998;1:673–768.
Topol LZ, Marx M, Laugier D, Bogdanova NN, Boubnov NV, Clausen PA, et al. Identification of drm, a novel gene whose expression is suppressed in transformed cells and which can inhibit growth of normal but not transformed cells in culture. Mol Cell Biol 1997;17:4801–10.
Topol LZ, Bardot B, Zhang Q, Resau J, Huillard E, Marx M, et al. Biosynthesis, post-translation modification, and functional characterization of drm/gremlin. J Biol Chem 2000; 275:8785–93.
Chen B, Athanasiou M, Gu Q, Blair DG. Drm/Gremlin transcriptionally activates p21(Cip1 via a novel mechanism and inhibits neoplastic transformation. Biochem Biophys Res Commun 2002;295:1135–41.
Suzuki M, Shigematsu H, Shivapurkar N, Reddy J, Miyajima K, Takahashi T, et al. Methylation of apoptosis related genes in the pathogenesis and prognosis of prostate cancer. Cancer Lett 2006; Feb 1.
Khokha MK, Hsu D, Brunet LJ, Dionne MS, Harland RM. Gremlin is the BMP antagonist required for maintenance of Shh and Fgf signals during limb patterning. Nat Genet 2003; 34: 303–7.
Michos O, Panman L, Vintersten K, Beier K, Zeller R, Zuniga A. Gremlin-mediated BMP antagonism induces the epithelial–mesenchymal feedback signaling controlling metanephric kidney and limb organogenesis. Development 2004;131:3401–10.
Pereira RC, Economides AN, Canalis E. Bone morphogenetic proteins induce gremlin, a protein that limits their activity in osteoblasts. Endocrinology 2000;141:4558–63.
Gazzerro E, Pereira RC, Jorgetti V, Olson S, Economides AN, Canalis E. Skeletal overexpression of gremlin impairs bone formation and causes osteopenia. Endocrinology 2005;146: 655–65.
Dolan V, Murphy M, Sadlier D, Lappin D, Doran P, Godson C, et al. Expression of gremlin, a bone morphogenetic protein antagonist, in human diabetic nephropathy. Am J Kidney Dis 2005;45:1034–9.
van Bezooijen RL, ten Dijke P, Papapoulos SE, Lowik CW. SOST/sclerostin, an osteocyte-derived negative regulator of bone formation. Cytokine Growth Factor Rev 2005;16:319–27.
Otto SM. Sclerostin and Wnt signaling, the pathway to bone strength. J Clin Endocrinol Metab 2005;90:6741–3.
Sutherland MK, Geoghegan JC, Yu C, Winkler DG, Latham JA.Unique regulation of SOST, the sclerosteosis gene, by BMPs and steroid hormones in human osteoblasts. Bone 2004;35:448–54.
Bellido T, Ali AA, Gubrij I, Plotkin LI, Fu Q, O’Brien CA, et al. Chronic elevation of parathyroid hormone in mice reduces expression of sclerostin by osteocytes: a novel mechanism for hormonal control of osteoblastogenesis. Endocrinology 2005;146:4577–83.
Keller H, Kneissel M. SOST is a target gene for PTH in bone. Bone 2005;37:148–58.
Poole KE, van Bezooijen RL, Loveridge N, Hamersma H, Papapoulos SE, Lowik CW, et al. Sclerostin is a delayed secreted product of osteocytes that inhibits bone formation. FASEB J 2005;19:1842–4.
Winkler DG, Sutherland MK, Geoghegan JC, Yu C, Hayes T, Skonier JE, et al. Osteocyte control of bone formation via sclerostin, a novel BMP antagonist. EMBO J 2003;22:6267–76.
Loots GG, Kneissel M, Keller H, Baptist M, Chang J, Collette NM, et al. Genomic deletion of a long-range bone enhancer misregulates sclerostin in Van Buchem disease. Genome Res 2005;15:928–35.
Yanagita M, Okuda T, Endo S, Tanaka M, Takahashi K, Sugiyama F, et al. Uterine sensitization-associated gene-1 (USAG-1), a novel BMP antagonist expressed in the kidney, accelerates tubular injury. J Clin Invest 2006;116(1):70–9.
Li X, Zhang Y, Kang H, Liu W, Liu P, Zhang J, et al. Sclerostin binds to LRP5/6 and antagonizes canonical Wnt signaling. J Biol Chem 2005;280:19883–7.
Winkler DG, Yu C, Geoghegan JC, Ojala EW, Skonier JE, Shpektor D, et al. Noggin and sclerostin bone morphogenetic protein antagonists form a mutually inhibitory complex. J Biol Chem 2004;279:36293–8.
Warnington K, Morony S, Sarosi I, Gong J, Stephens P, Winkler DG, et al. Sclerostin antagonism in adult rodents, via monoclonal antibody mediated blockade, increases bone mineral density and implicates sclerostin as a key regulator of bone mass during adulthood. Proceedings of the Abstract 27th Annual Meeting American Society of Bone and Mineral Research.
Stanley E, Biben C, Kotecha S, Fabri L, Tajbakhsh S, Wang C-C, et al. DAN is a secreted glycoprotein related to Xenopus cerberus. Mech Dev 1998;77:173–84.
Dionne MS, Skarnes WC, Harland RM. Mutation and analysis of Dan, the founding member of the Dan family of transforming growth factor β antagonists. Mol Cell Biol 2001;21:636–43.
Piccolo S, Agius E, Leyns L, Bhattacharyya S, Grunz H, Bouwmeester T, et al. The head inducer Cerberus is a multifunctional antagonist of nodal, BMP and Wnt signals. Nature 1999;397:707–10.
Shawlot W, Deng JM, Behringer RR. Expression of the mouse cerberus-related gene, Cerr1, suggests a role in anterior neural induction and somitogenesis. Proc Natl Acad Sci USA 1998; 95:6198–203.
Yokouchi Y, Vogan KJ, Pearse RV, Tabin CJ. Antagonistic signaling by caronte, a novel cerberus-related gene, establishes left-right asymmetric gene expression. Cell 1999;98:573–83.
Bell E, Munoz-Sanjuan I, Altmann CR, Vonica A, Brivanlou AH. Cell fate specification and competence by Coco, a maternal BMP, TGFbeta and Wnt inhibitor. Development 2003;130: 1381–9.
Pearce JJH, Penny G, Rossant J. A mouse cerberus/Dan-related gene family. Dev Biol 1999;209:98–110.
Minabe-Saegusa C, Saegusa H, Tsukahara M, Noguchi S. Sequence and expression of a novel mouse gene PRDC (protein related to DAN and cerberus) identified by a gene trap approach. Dev Growth Differ 1998;40:343–53.
Laurikkala J, Kassai Y, Pakkasjarvi L, Thesleff I, Itoh N. Identification of a secreted BMP antagonist, ectodin, integrating BMP, FGF, and SHH signals from the tooth enamel knot. Dev Biol 2003;264:91–105.
Onichtchouk D, Chen Y-G, Dosch R, Gawantka V, Delius H, Massague J, et al. Silencing of TGFβ signaling by the pseudoreceptor BAMBI. Nature 1999;401:480–5.
Kalajzic I, Staal A, Yang WP, Wu Y, Johnson SE, Feyen JH, et al. Expression profile of osteoblast lineage at defined stages of differentiation. J Biol Chem 2005;280:24618–26.
Ishida W, Hamamoto T, Kusanagi K, Yagi K, Kawabata M, Takehara K, et al. Smad6 is a Smad1/5-induced smad inhibitor. Characterization of bone morphogenetic protein-responsive element in the mouse Smad6 promoter. J Biol Chem 2000;275: 6075–9.
Itoh F, Asao H, Sugamura K, Heldin CH, ten Dijke P, Itoh S. Promoting bone morphogenetic protein signaling through negative regulation of inhibitory Smads. EMBO J 2001;20: 4132–42.
Luo K. Negative regulation of BMP signaling by the ski oncoprotein. J Bone Jt Surg Am 2003;85:39–43.
Reed JA, Lin Q, Chen D, Mian IS, Medrano EE. SKI pathways inducing progression of human melanoma. Cancer Metastasis Rev 2005;24(2):265–72.
Wang W, Mariani FV, Harland RM, Luo K. Ski represses bone morphogenic protein signaling in Xenopus and mammalian cells. Proc Natl Acad Sci USA 2000;97:14394–9.
Suzuki H, Yagi K, Kondo M, Kato M, Miyazono K, Miyazawa K. c-Ski inhibits the TGF-beta signaling pathway through stabilization of inactive Smad complexes on Smad-binding elements. Oncogene 2004;23:5068–76.
Berk M, Desai SY, Heyman HC, Colmenares C. Mice lacking the ski proto-oncogene have defects in neurulation, craniofacial patterning, and skeletal muscle development. Genes Dev 1997;11:2029–39.
Lana DP, Leferovich JM, Kelly AM, Hughes SH. Selective expression of a ski transgene affects IIb fast muscles and skeletal structure. Dev Dyn 1996;205:13–23.
Yoshida Y, Tanaka S, Umemori H, Minowa O, Michihiko U, Ikematsu N, et al. Negative regulation of BMP/Smad signaling by Tob in osteoblasts. Cell 2000;103:1085–97.
Ikematsu N, Yoshida Y, Kawamura-Tsuzuku J, Ohsugi M, Onda M, Hirai M, et al. Tob2, a novel anti-proliferative Tob/BTG1 family member, assoicates with a component of the CCR4 transcriptional regulatory complex capable of binding cyclin-dependent kinases. Oncogene 1999;18:7432–41.
Zhang Y, Chang C, Gehling DJ, Hemmati-Brivanlou A, Derynck R. Regulation of Smad degradation and activity by Smurf2, and E3 ubiquitin ligase. Proc Natl Acad Sci USA 2001;98:974–9.
Murakami G, Watabe T, Takaoka K, Miyazono K, Imamura T. Cooperative inhibition of bone morphogenetic protein signaling by Smurf1 and inhibitory Smads. Mol Biol Cell 2003;14: 2809–17.
Horiki M, Imamura T, Okamoto M, Hayashi M, Murai J, Myoui A, et al. Smad6/Smurf1 overexpression in cartilage delays chondrocyte hypertrophy and causes dwarfism with osteopenia. J Cell Biol 2004;165:433–45.
Zhao M, Qiao M, Oyajobi B, Mundy GR, Chen D. E3 ubiquitin ligase Smurf1 mediates core-binding factor a1/Runx2 degradation and plays a specific role in osteoblast differentiation. J Biol Chem 2003;278:27939–44.
Shen R, Chen M, Wang YJ, Kaneki H, Xing L, O’keefe RJ, et al. Smad6 interacts with Runx2 and mediates Smad ubiquitin regulatory factor 1-induced Runx2 degradation. J Biol Chem 2006;281:3569–76.
Zhao M, Qiao M, Harris SE, Oyajobi B, Mundy GR, Chen D. Smurf1 inhibits osteoblast differentiation and bone formation in vitro and in vivo. J Biol Chem 2004;279:12854–9.
Yamashita M, Ying SX, Zhang GM, Li C, Cheng SY, Deng CX, et al. Ubiquitin ligase Smurf1 controls osteoblast activity and bone homeostasis by targeting MEKK2 for degradation. Cell 2005;121:101–13.
Tsumaki N, Nakase T, Miyaji T, Kakiuchi M, Kimura T, Ochi T, et al. Bone morphogenetic protein signals are required for cartilage formation and differently regulate joint development during skeletogenesis. J Bone Miner Res 2005; 17:898–906.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by Grant AR21707 from the National Institute of Arthritis and Musculoskeletal and Skin Diseases.
Rights and permissions
About this article
Cite this article
Gazzerro, E., Canalis, E. Bone morphogenetic proteins and their antagonists. Rev Endocr Metab Disord 7, 51–65 (2006). https://doi.org/10.1007/s11154-006-9000-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11154-006-9000-6