Abstract
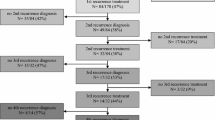
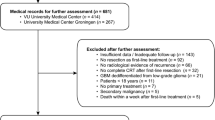
A growing literature supports maximal safe resection followed by standard combined chemoradiotherapy (i.e. maximal first-line therapy) for selected elderly glioblastoma patients. To assess the prognostic factors from recurrence in elderly glioblastoma patients treated by maximal safe resection followed by standard combined chemoradiotherapy as first-line therapy. Multicentric retrospective analysis comparing the prognosis and optimal oncological management of recurrent glioblastomas between 660 adult patients aged of < 70 years (standard group) and 117 patients aged of ≥70 years (elderly group) harboring a supratentorial glioblastoma treated by maximal first-line therapy. From recurrence, both groups did not significantly differ regarding Karnofsky performance status (KPS) (p = 0.482). Oncological treatments from recurrence significantly differed: patients of the elderly group received less frequently oncological treatment from recurrence (p < 0.001), including surgical resection (p < 0.001), Bevacizumab therapy (p < 0.001), and second line chemotherapy other than Temozolomide (p < 0.001). In multivariate analysis, Age ≥70 years was not an independent predictor of overall survival from recurrence (p = 0.602), RTOG-RPA classes 5–6 (p = 0.050) and KPS at recurrence <70 (p < 0.001), available in all cases, were independent significant predictors of shorter overall survival from recurrence. Initial removal of ≥ 90% of enhancing tumor (p = 0.004), initial completion of the standard combined chemoradiotherapy (p = 0.007), oncological treatment from recurrence (p < 0.001), and particularly surgical resection (p < 0.001), Temozolomide (p = 0.046), and Bevacizumab therapy (p = 0.041) were all significant independent predictors of longer overall survival from recurrence. Elderly patients had substandard care from recurrence whereas age did not impact overall survival from recurrence contrary to KPS at recurrence <70. Treatment options from recurrence should include repeat surgery, second line chemotherapy and anti-angiogenic agents.


Similar content being viewed by others
Abbreviations
- PFS:
-
Progression-free survival
- EFGR:
-
Epidermal growth factor receptor
- HR:
-
Hazard ratio
- KPS:
-
Karnofsky performance status
- OS:
-
Overall survival
- RTOG-RPA:
-
Radiation therapy oncology group recursive partitioning analysis
References
Ostrom QT, Gittleman H, Fulop J et al (2015) CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the United States in 2008–2012. Neuro-Oncol 17 Suppl 4:iv1–iv62. doi:10.1093/neuonc/nov189
Colby SL, Ortman JM et al (2015) Projections of the size and composition of the US population: 2014 to 2060. Curr Popul Rep 9:1–13
Rigau V, Zouaoui S, Mathieu-Daudé H et al (2011) French brain tumor DataBase: 5-year histological results on 25 756 cases. Brain Pathol 21:633–644. doi:10.1111/j.1750-3639.2011.00491.x
Curran WJ, Scott CB, Horton J et al (1993) Recursive partitioning analysis of prognostic factors in three Radiation Therapy Oncology Group malignant glioma trials. J Natl Cancer Inst 85:704–710
Mirimanoff R-O, Gorlia T, Mason W et al (2006) Radiotherapy and temozolomide for newly diagnosed glioblastoma: recursive partitioning analysis of the EORTC 26981/22981-NCIC CE3 phase III randomized trial. J Clin Oncol 24:2563–2569. doi:10.1200/JCO.2005.04.5963
Michaelsen SR, Christensen IJ, Grunnet K et al (2013) Clinical variables serve as prognostic factors in a model for survival from glioblastoma multiforme: an observational study of a cohort of consecutive non-selected patients from a single institution. BMC Cancer 13:402. doi:10.1186/1471-2407-13-402
Zouaoui S, Darlix A, Fabbro-Peray P et al (2014) Oncological patterns of care and outcomes for 265 elderly patients with newly diagnosed glioblastoma in France. Neurosurg Rev 37:415–424. doi:10.1007/s10143-014-0528-8
Vuorinen V, Hinkka S, Färkkilä M, Jääskeläinen J (2003) Debulking or biopsy of malignant glioma in elderly people—a randomised study. Acta Neurochir (Wien) 145:5–10. doi:10.1007/s00701-002-1030-6
Chaichana KL, Garzon-Muvdi T, Parker S et al (2011) Supratentorial glioblastoma multiforme: the role of surgical resection versus biopsy among older patients. Ann Surg Oncol 18:239–245. doi:10.1245/s10434-010-1242-6
Scott JG, Suh JH, Elson P et al (2011) Aggressive treatment is appropriate for glioblastoma multiforme patients 70 years old or older: a retrospective review of 206 cases. Neuro-Oncol 13:428–436. doi:10.1093/neuonc/nor005
Keime-Guibert F, Chinot O, Taillandier L et al (2007) Radiotherapy for glioblastoma in the elderly. N Engl J Med 356:1527–1535. doi:10.1056/NEJMoa065901
Gállego Pérez-Larraya J, Ducray F, Chinot O et al (2011) Temozolomide in elderly patients with newly diagnosed glioblastoma and poor performance status: an ANOCEF phase II trial. J Clin Oncol 29:3050–3055. doi:10.1200/JCO.2011.34.8086
Stupp R, Mason WP, van den Bent MJ et al (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352:987–996. doi:10.1056/NEJMoa043330
Perry JR, Laperriere N, O’Callaghan CJ et al (2016) A phase III randomized controlled trial of short-course radiotherapy with or without concomitant and adjuvant temozolomide in elderly patients with glioblastoma (CCTG CE.6, EORTC 26062–22061, TROG 08.02, NCT00482677). J Clin Oncol. doi:10.1093/neuonc/nou209.16
Iwamoto FM, Reiner AS, Panageas KS et al (2008) Patterns of care in elderly glioblastoma patients. Ann Neurol 64:628–634. doi:10.1002/ana.21521
Bauchet L, Zouaoui S, Darlix A et al (2014) Assessment and treatment relevance in elderly glioblastoma patients. Neuro-Oncol 16:1459–1468. doi:10.1093/neuonc/nou063
Morgan ER, Norman A, Laing K, Seal MD (2017) Treatment and outcomes for glioblastoma in elderly compared with non-elderly patients: a population-based study. Curr Oncol Tor Ont 24:e92–e98. doi:10.3747/co.24.3424
Combs SE, Wagner J, Bischof M et al (2008) Postoperative treatment of primary glioblastoma multiforme with radiation and concomitant Temozolomide in elderly patients. Int J Radiat Oncol 70:987–992. doi:10.1016/j.ijrobp.2007.07.2368
Ewelt C, Goeppert M, Rapp M et al (2011) Glioblastoma multiforme of the elderly: the prognostic effect of resection on survival. J Neurooncol 103:611–618. doi:10.1007/s11060-010-0429-9
Park H-K, Koh Y-C, Song SW (2014) The clinico-oncologic outcomes of elderly patients with glioblastoma after surgical resection followed by concomitant chemo-radiotherapy. Brain Tumor Res Treat 2:69. doi:10.14791/btrt.2014.2.2.69
Babu R, Komisarow JM, Agarwal VJ et al (2016) Glioblastoma in the elderly: the effect of aggressive and modern therapies on survival. J Neurosurg 124:998–1007. doi:10.3171/2015.4.JNS142200
Rusthoven CG, Koshy M, Sher DJ et al (2016) Combined-modality therapy with radiation and chemotherapy for elderly patients with glioblastoma in the temozolomide era: a national cancer database analysis. JAMA Neurol. doi:10.1001/jamaneurol.2016.0839
Huang J, Samson PP, Perkins SM et al (2016) Trends in utilization and impact of concurrent chemotherapy with radiation therapy for elderly patients with newly diagnosed glioblastoma: a review of the national cancer data base. J Clin Oncol 34:2034
Martinez-Garcia M, Pineda E, Barco SD et al (2016) Feasibility and efficacy of concomitant chemoradiation (Ch-RT) in the management of newly diagnosed elderly glioblastoma (GB) patients: results from the GLIOCAT study. J Clin Oncol 34:2045
Amsbaugh MJ, Yusuf MB, Gaskins J et al (2017) Patterns of care and predictors of adjuvant therapies in elderly patients with glioblastoma: an analysis of the National Cancer Database. Cancer. doi:10.1002/cncr.30730
Flanigan PM, Jahangiri A, Kuang R et al (2017) Developing an algorithm for optimizing care of elderly patients with glioblastoma. Neurosurgery. doi:10.1093/neuros/nyx148
Weller M, Cloughesy T, Perry JR, Wick W (2013) Standards of care for treatment of recurrent glioblastoma–are we there yet? Neuro-Oncol 15:4–27. doi:10.1093/neuonc/nos273
Macdonald DR, Cascino TL, Schold SC, Cairncross JG (1990) Response criteria for phase II studies of supratentorial malignant glioma. J Clin Oncol 8:1277–1280
Li J, Wang M, Won M et al (2011) Validation and simplification of the radiation therapy oncology group recursive partitioning analysis classification for glioblastoma. Int J Radiat Oncol 81:623–630. doi:10.1016/j.ijrobp.2010.06.012
Wen PY, Macdonald DR, Reardon DA et al (2010) Updated response assessment criteria for high-grade gliomas: response assessment in neuro-oncology working group. J Clin Oncol 28:1963–1972. doi:10.1200/JCO.2009.26.3541
Marko NF, Weil RJ, Schroeder JL et al (2014) Extent of resection of glioblastoma revisited: personalized survival modeling facilitates more accurate survival prediction and supports a maximum-safe-resection approach to surgery. J Clin Oncol Off J Am Soc Clin Oncol 32:774–782. doi:10.1200/JCO.2013.51.8886
Stupp R, Brada M, van den Bent MJ et al (2014) High-grade glioma: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 25(Suppl 3):iii93–i101. doi:10.1093/annonc/mdu050
Mason WP, Maestro RD, Eisenstat D et al (2007) Canadian recommendations for the treatment of glioblastoma multiforme. Curr Oncol Tor Ont 14:110–117
Chargari C, Feuvret L, Bauduceau O et al (2012) Treatment of elderly patients with glioblastoma: from clinical evidence to molecular highlights. Cancer Treat Rev 38:988–995. doi:10.1016/j.ctrv.2011.12.010
Hartmann C, Hentschel B, Wick W et al (2010) Patients with IDH1 wild type anaplastic astrocytomas exhibit worse prognosis than IDH1-mutated glioblastomas, and IDH1 mutation status accounts for the unfavorable prognostic effect of higher age: implications for classification of gliomas. Acta Neuropathol (Berl) 120:707–718. doi:10.1007/s00401-010-0781-z
Yin A, Zhang L, Cheng J et al (2014) The predictive but not prognostic value of MGMT promoter methylation status in elderly glioblastoma patients: a meta-analysis. PLoS ONE 9:e85102. doi:10.1371/journal.pone.0085102
Weller M, Wick W (2011) Are we ready to demystify age in glioblastoma? Or does older age matter in glioblastoma? Neuro-Oncol 13:365–366. doi:10.1093/neuonc/nor019
Wick W, Platten M, Meisner C et al (2012) Temozolomide chemotherapy alone versus radiotherapy alone for malignant astrocytoma in the elderly: the NOA-08 randomised, phase 3 trial. Lancet Oncol 13:707–715. doi:10.1016/S1470-2045(12)70164-X
Mohan DS, Suh JH, Phan JL et al (1998) Outcome in elderly patients undergoing definitive surgery and radiation therapy for supratentorial glioblastoma multiforme at a tertiary care institution. Int J Radiat Oncol Biol Phys 42:981–987
Muacevic A, Kreth FW (2003) Quality-adjusted survival after tumor resection and/or radiation therapy for elderly patients with glioblastoma multiforme. J Neurol 250:561–568. doi:10.1007/s00415-003-1036-x
Stark AM, Hedderich J, Held-Feindt J, Mehdorn HM (2007) Glioblastoma–the consequences of advanced patient age on treatment and survival. Neurosurg Rev 30:56–61. doi:10.1007/s10143-006-0051-7
Filippini G, Falcone C, Boiardi A et al (2008) Prognostic factors for survival in 676 consecutive patients with newly diagnosed primary glioblastoma. Neuro-Oncol 10:79–87. doi:10.1215/15228517-2007-038
Iwamoto FM, Cooper AR, Reiner AS et al (2009) Glioblastoma in the elderly: the Memorial Sloan-Kettering Cancer Center experience (1997–2007). Cancer 115:3758–3766. doi:10.1002/cncr.24413
Roa W, Kepka L, Kumar N et al (2015) International atomic energy agency randomized phase III study of radiation therapy in elderly and/or frail patients with newly diagnosed glioblastoma multiforme. J Clin Oncol 33:4145–4150. doi:10.1200/JCO.2015.62.6606
Minniti G, Scaringi C, Lanzetta G et al (2015) Standard (60 Gy) or short-course (40 Gy) irradiation plus concomitant and adjuvant temozolomide for elderly patients with glioblastoma: a propensity-matched analysis. Int J Radiat Oncol 91:109–115. doi:10.1016/j.ijrobp.2014.09.013
Malmström A, Grønberg BH, Marosi C et al (2012) Temozolomide versus standard 6-week radiotherapy versus hypofractionated radiotherapy in patients older than 60 years with glioblastoma: the Nordic randomised, phase 3 trial. Lancet Oncol 13:916–926. doi:10.1016/S1470-2045(12)70265-6
Kim HR, Kim KH, Kong D-S et al (2015) Outcome of salvage treatment for recurrent glioblastoma. J Clin Neurosci 22:468–473. doi:10.1016/j.jocn.2014.09.018
Socha J, Kepka L, Ghosh S et al (2016) Outcome of treatment of recurrent glioblastoma multiforme in elderly and/or frail patients. J Neurooncol 126:493–498. doi:10.1007/s11060-015-1987-7
Scott JG, Bauchet L, Fraum TJ et al (2012) Recursive partitioning analysis of prognostic factors for glioblastoma patients aged 70 years or older. Cancer 118:5595–5600. doi:10.1002/cncr.27570
Nguyen LT, Touch S, Nehme-Schuster H et al (2013) Outcomes in newly diagnosed elderly glioblastoma patients after concomitant temozolomide administration and hypofractionated radiotherapy. Cancers 5:1177–1198. doi:10.3390/cancers5031177
Wildiers H, Heeren P, Puts M et al (2014) International Society of Geriatric Oncology consensus on geriatric assessment in older patients with cancer. J Clin Oncol 32:2595–2603. doi:10.1200/JCO.2013.54.8347
Pallis AG, Ring A, Fortpied C et al (2011) EORTC workshop on clinical trial methodology in older individuals with a diagnosis of solid tumors. Ann Oncol 22:1922–1926. doi:10.1093/annonc/mdq687
Hurria A, Dale W, Mooney M et al (2014) Designing therapeutic clinical trials for older and frail adults with cancer: U13 conference recommendations. J Clin Oncol 32:2587–2594. doi:10.1200/JCO.2013.55.0418
Park JK, Hodges T, Arko L et al (2010) Scale to predict survival after surgery for recurrent glioblastoma multiforme. J Clin Oncol 28:3838–3843. doi:10.1200/JCO.2010.30.0582
Acknowledgements
Participating centres (in alphabetical order): Amiens University Hospital – University of Amiens, Angers University Hospital – Angers University, Jean-Minjoz Hospital – University of Besançon, Pellegrin Hospital – University Victor Segalen Bordeaux 2, Avicenne University Hospital – Paris 13 University, Morvan Hospital – University of Brest, Caen University Hospital – University Caen Lower-Normandy, Pasteur Hospital in Colmar, Limoges Hospital – University of Limoges, Pierre Wertheimer Hospital – University of Lyon, La Timone Hospital – University Aix-Marseille, Clairval Clinic in Marseille, Gui de Chauliac Hospital – University of Montpellier, Sainte-Anne Hospital Centre - University Paris Descartes, Beaujon Hospital – University Paris Diderot, Maison Blanche Hospital – University of Reims, Pontchaillou Hospital – University of Rennes, Rouen University Hospital – Rouen University, Paul Strauss Cancer Centre – University of Strasbourg, Sainte-Anne Military Teaching Hospital in Toulon, Gustave Roussy University Hospital, Villejuif. These physicians are greatly acknowledged (in alphabetical order): Georges Abi Lahoud, Felipe Andreiuolo, Alin Borha, Céline Botella, André Busson, Laurent Capelle, Françoise Chapon, Isabelle Catry-Thomas, Karl Champeaux, Françine Chassoux, Anaïs Chivet, Fabrice Chrétien, Philippe Colin, Alain Czorny, Phong Dam-Hieu, Jean-Michel Derlon, Bertrand Devaux, Frédéric Dhermain, Marie-Danièle Diebold, Julien Domont, Hugues Duffau, Sarah Dumont, Julien Duntze, Myriam Edjlali-Goujon, Jan Eskandari, Pascale Fabbro-Peray, Anne Fustier, Clément Gantois, Roberto Gadan, Julien Geffrelot, Edouard Gimbert, Joël Godard, Sylvie Godon-Hardy, Marcel Gueye, Jean-Sébastien Guillamo, N Heil, Dominique Hoffmann, Nicolas Jovenin, Michel Kalamarides, Hassan Katranji, Samih Khouri, Maria Koziak, Elisabeth Landré, V Leon, Dominique Liguoro, Guillaume Louvel, Emmanuel Mandonnet, Michael Mann, Eric Méary, Jean-François Meder, Charles Mellerio, Sophie Michalak, Catherine Miquel, Karima Mokhtari, Philippe Monteil, Edmond Nader, Olivier Naggara, Catherine Oppenheim, Isabelle Quintin-Roue, Philippe Paquis, Vladislav Pavlov, Delphine Pedenon, Philippe Peruzzi, Tanguy Riem, Valérie Rigau, Odile Rigaux-Viodé, Adeline Riondel, Alain Rougier, Céline Salon, Elodie Sorbets, Etienne Théret, Baris Turak, Denis Trystram, Fanny Vandenbos, Pascale Varlet, Gabriel Viennet, Anne Vital, Sonia Zouaoui. We would like to thank the Association des Neuro-Oncologues d’Expression Française (ANOCEF).
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
Johan Pallud has received honoraria for consultancy from Kyowa Hakko Kirin Co. Johan Pallud and Alexandre Roux have received honoraria for speaking engagements (including travel and accommodation) from Kyowa Hakko Kirin Co.
Electronic supplementary material
Below is the link to the electronic supplementary material.

11060_2017_2573_MOESM2_ESM.docx
Supplementary Table 1 Progression-free survival. Unadjusted and adjusted prognostic factors by Cox proportional hazards model. Supplementary Table 2 Overall survival after treated recurrence. Unadjusted and adjusted prognostic factors by Cox proportional hazards model (DOCX 74 KB)
Rights and permissions
About this article
Cite this article
Zanello, M., Roux, A., Ursu, R. et al. Recurrent glioblastomas in the elderly after maximal first-line treatment: does preserved overall condition warrant a maximal second-line treatment?. J Neurooncol 135, 285–297 (2017). https://doi.org/10.1007/s11060-017-2573-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-017-2573-y