Abstract
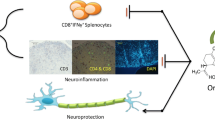
A seven day pretreatment course of an oral antibiotic cocktail (Ampicillin, Metronidazole, Neomycin Sulfate, and Vancomycin) was shown to induce changes in peripheral immune regulation and protect mice from signs of experimental autoimmune encephalomyelitis (EAE). To determine if a shorter course of antibiotic pretreatment could also protect the mice from EAE and induce regulatory immune cells, studies were conducted using the same oral antibiotic cocktail for three days. In addition, the CNS was examined to determine the effects of antibiotic pretreatment on EAE disease course and immune modulation within the affected tissue. The shorter three day pretreatment course was also significantly protective against severe EAE in C57BL/6 mice. Moreover, our study found increased frequencies of regulatory cells and a decrease in the frequency of anti-inflammatory macrophages in the spleen of EAE protected mice. Additionally, a chemokine and chemokine receptor array run on mRNA from spinal cords revealed that genes associated with regulatory T cells and macrophage recruitment were strongly upregulated in the antibiotic pretreated mice. Additional RT-PCR data showed genes associated with anti-inflammatory microglia/macrophages were upregulated and pro-inflammatory genes were downregulated. This suggests the macrophages recruited to the spinal cord by chemokines are subsequently polarized toward an anti-inflammatory phenotype. These results lend strong support to the conclusion that a three day course of antibiotic treatment given prior to the induction of severe EAE profoundly protected the mice by inducing regulatory lymphocytes in the periphery and an anti-inflammatory milieu in the affected spinal cord tissue.






Similar content being viewed by others
References
Berer K et al (2011) Commensal microbiota and myelin autoantigen cooperate to trigger autoimmune demyelination. Nature 479:538–541. https://doi.org/10.1038/nature10554
Bodhankar S, Chen Y, Lapato A, Vandenbark AA, Murphy SJ, Saugstad JA, Offner H (2015) Regulatory CD8(+)CD122 (+) T-cells predominate in CNS after treatment of experimental stroke in male mice with IL-10-secreting B-cells. Metab Brain Dis 30:911–924. https://doi.org/10.1007/s11011-014-9639-8
Dziembowska M, Tham TN, Lau P, Vitry S, Lazarini F, Dubois-Dalcq M (2005) A role for CXCR4 signaling in survival and migration of neural and oligodendrocyte precursors. Glia 50:258–269. https://doi.org/10.1002/glia.20170
Erny D et al (2015) Host microbiota constantly control maturation and function of microglia in the CNS. Nat Neurosci 18:965–977. https://doi.org/10.1038/nn.4030
Fararjeh M, Mohammad MK, Bustanji Y, Alkhatib H, Abdalla S (2008) Evaluation of immunosuppression induced by metronidazole in Balb/c mice and human peripheral blood lymphocytes. Int Immunopharmacol 8:341–350. https://doi.org/10.1016/j.intimp.2007.10.018
Freedman SN, Shahi SK, Mangalam AK (2018) The "gut feeling": breaking down the role of gut microbiome in multiple sclerosis. Neurotherapeutics 15:109–125. https://doi.org/10.1007/s13311-017-0588-x
Ivanov II et al (2008) Specific microbiota direct the differentiation of IL-17-producing T-helper cells in the mucosa of the small intestine. Cell Host Microbe 4:337–349. https://doi.org/10.1016/j.chom.2008.09.009
Iwata Y et al (2011) Characterization of a rare IL-10-competent B-cell subset in humans that parallels mouse regulatory B10 cells. Blood 117:530–541. https://doi.org/10.1182/blood-2010-07-294249
Kowarik MC et al (2012) CXCL13 is the major determinant for B cell recruitment to the CSF during neuroinflammation. J Neuroinflammation 9:93. https://doi.org/10.1186/1742-2094-9-93
Lee YK, Menezes JS, Umesaki Y, Mazmanian SK (2011) Proinflammatory T-cell responses to gut microbiota promote experimental autoimmune encephalomyelitis. Proc Natl Acad Sci U S A 108(Suppl 1):4615–4622. https://doi.org/10.1073/pnas.1000082107
Lim HW, Lee J, Hillsamer P, Kim CH (2008) Human Th17 cells share major trafficking receptors with both polarized effector T cells and FOXP3+ regulatory T cells. J Immunol 180:122–129
Liu J et al (2008) IFN-gamma and IL-17 production in experimental autoimmune encephalomyelitis depends on local APC-T cell complement production. J Immunol 180:5882–5889
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(−Delta Delta C(T)) Method. Methods 25:402–408. https://doi.org/10.1006/meth.2001.1262
Matsumoto M et al (2014) Interleukin-10-producing plasmablasts exert regulatory function in autoimmune inflammation. Immunity 41:1040–1051. https://doi.org/10.1016/j.immuni.2014.10.016
Meiron M, Zohar Y, Anunu R, Wildbaum G, Karin N (2008) CXCL12 (SDF-1alpha) suppresses ongoing experimental autoimmune encephalomyelitis by selecting antigen-specific regulatory T cells. J Exp Med 205:2643–2655. https://doi.org/10.1084/jem.20080730
Mielcarz DW, Kasper LH (2015) The gut microbiome in multiple sclerosis. Curr Treat Options Neurol 17:344. https://doi.org/10.1007/s11940-015-0344-7
Niess JH, Leithauser F, Adler G, Reimann J (2008) Commensal gut flora drives the expansion of proinflammatory CD4 T cells in the colonic lamina propria under normal and inflammatory conditions. J Immunol 180:559–568
Ochoa-Reparaz J, Kasper LH (2014) Gut microbiome and the risk factors in central nervous system autoimmunity. FEBS Lett 588:4214–4222. https://doi.org/10.1016/j.febslet.2014.09.024
Ochoa-Reparaz J, Mielcarz DW, Ditrio LE, Burroughs AR, Foureau DM, Haque-Begum S, Kasper LH (2009) Role of gut commensal microflora in the development of experimental autoimmune encephalomyelitis. J Immunol 183:6041–6050. https://doi.org/10.4049/jimmunol.0900747
Ochoa-Reparaz J, Mielcarz DW, Haque-Begum S, Kasper LH (2010) Induction of a regulatory B cell population in experimental allergic encephalomyelitis by alteration of the gut commensal microflora. Gut Microbes 1:103–108. https://doi.org/10.4161/gmic.1.2.11515
Palm NW, de Zoete MR, Flavell RA (2015) Immune-microbiota interactions in health and disease. Clin Immunol 159:122–127. https://doi.org/10.1016/j.clim.2015.05.014
Rupprecht TA et al (2009) The chemokine CXCL13 is a key regulator of B cell recruitment to the cerebrospinal fluid in acute Lyme neuroborreliosis. J Neuroinflammation 6:42. https://doi.org/10.1186/1742-2094-6-42
Shi Z, Rifa'i M, Lee YH, Shiku H, Isobe K, Suzuki H (2008) Importance of CD80/CD86-CD28 interactions in the recognition of target cells by CD8+CD122+ regulatory T cells. Immunology 124:121–128. https://doi.org/10.1111/j.1365-2567.2007.02747.x
Wang Y et al (2014) A commensal bacterial product elicits and modulates migratory capacity of CD39(+) CD4 T regulatory subsets in the suppression of neuroinflammation. Gut Microbes 5:552–561. https://doi.org/10.4161/gmic.29797
Zhang J, Lapato A, Bodhankar S, Vandenbark AA, Offner H (2015) Treatment with IL-10 producing B cells in combination with E2 ameliorates EAE severity and decreases CNS inflammation in B cell-deficient mice. Metab Brain Dis 30:1117–1127. https://doi.org/10.1007/s11011-015-9661-5
Funding
This work was supported by Deutsche Forschungsgemeinschaft (DFG) EXC1010 SyNergy (JB), NIH, National Institute Of Neurological Disorders And Stroke of the National Institutes R01NS080890 (HO) and the Department of Veterans Affairs IO1 BX000226-09 and 1 IK6 BX004209 (AAV). This material is also the result of work supported with resources and the use of facilities at the VA Portland Health Care Center in Portland, Oregon. The contents do not represent the views of the U.S. Department of Veterans Affairs, the United States Government or the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human and/or animals
All applicable international, national and/or institutional guidelines for the care and use of animals were followed. All procedures performed in studies involving animals were in accordance with the ethical standards of the institution or practice at which the studies were conducted. This article does not contain any studies with human participants performed by any of the authors.
Rights and permissions
About this article
Cite this article
Seifert, H.A., Benedek, G., Nguyen, H. et al. Antibiotics protect against EAE by increasing regulatory and anti-inflammatory cells. Metab Brain Dis 33, 1599–1607 (2018). https://doi.org/10.1007/s11011-018-0266-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-018-0266-7