Abstract
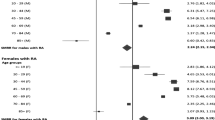
The objectives of this study were to estimate and compare the prevalence of heart disease, cancer, chronic lower respiratory disease, stroke, Alzheimer’s, diabetes, nephrosis, flu/pneumonia, hypertension, and atherosclerosis between Arab Americans and whites attending a large, metropolitan hospital system. The sample included 68,047 patients, 18 years of age or older, who visited the hospital during 2012. Demographic and disease variables were electronically abstracted. Demographic characteristics were compared between Arab Americans and whites using Chi square tests. Sex specific, age-adjusted prevalence ratios (PR) and 95 % confidence intervals were estimated for these two groups using a log-binomial regression model. Compared to white men, Arab American men had a higher prevalence of diabetes (PR 1.40, 95 % CI 1.29–1.52) and hypertension (PR 1.07, 95 % CI 1.04–1.10), and a lower prevalence of chronic lower respiratory disease (PR 0.74, 95 % CI 0.66–0.83). Compared to white women, Arab American women had a higher prevalence of chronic lower respiratory disease (PR 1.12, 95 % CI 1.01–1.25), diabetes (PR 1.49, 95 % CI 1.38–1.60), influenza/pneumonia (PR 1.26, 95 % CI 1.05–1.51) and hypertension (PR 1.04, 95 % CI 1.01–1.08). This study supports previous findings that health disparities exist for Arab Americans, who are classified as “white” in health statistics. Standard inclusion of Arab American as a separate ethnicity category will aid researchers in assessing the health care needs of this growing minority community.
Similar content being viewed by others
References
Burgos AE, Schetzina KE, Dixon LB, Mendoza FS. Importance of generational status in examining access to and utilization of health care services by Mexican American children. Pediatrics. 2005;115:e322–30.
Coughlin SS, Leadbetter S, Richards T, Sabatino SA. Contextual analysis of breast and cervical cancer screening and factors associated with health care access among United States women, 2002. Soc Sci Med. 2008;66:260–75.
Harris MI. Racial and ethnic differences in health care access and health outcomes for adults with type 2 diabetes. Diabetes Care. 2001;24:454–9.
American Fact Finder. 2014. http://factfinder.census.gov/faces/nav/jsf/pages/index.xhtml. Accessed 28 Jan 2014.
Revisions to the Standards for the Classification of Federal Data on Race and Ethnicity. The White House. 2014. https://www.whitehouse.gov/omb/fedreg_1997standards. Accessed 28 Jan 2014.
Steiner CA, Friedman B. Hospital utilization, costs, and mortality for adults with multiple chronic conditions, Nationwide Inpatient Sample, 2009. Prev Chronic Dis. 2013;10:E62.
Campbell R, Dean B, Nathanson B, Haidar T, Strauss M, Thomas S. Length of stay and hospital costs among high-risk patients with hospital-origin Clostridium difficile-associated diarrhea. J Med Econ. 2013;16:440–8.
Mandelberg JH, Kuhn RE, Kohn MA. Epidemiologic analysis of an urban, public emergency department’s frequent users. Acad Emerg Med. 2000;7:637–46.
Miller CM, Shi J, Wheeler KK, Yin H, Smith GA, Groner JI, Xiang H. Chronic conditions and outcomes of pediatric trauma patients. J Trauma Acute Care Surg. 2013;75:250–7.
Myint PK, Vowler SL, Redmayne O, Fulcher RA. Cognition, continence and transfer status at the time of discharge from an acute hospital setting and their associations with an unfavourable discharge outcome after stroke. Gerontology. 2008;54:202–9.
O’Mahony L, O’Mahony DS, Simon TD, Neff J, Klein EJ, Quan L. Medical complexity and pediatric emergency department and inpatient utilization. Pediatrics. 2013;131:e559–65.
Reich O, Signorell A, Busato A. Place of death and health care utilization for people in the last 6 months of life in Switzerland: a retrospective analysis using administrative data. BMC Health Serv Res. 2013;13:116.
Sim JJ, Bhandari SK, Shi J, Liu IL, Calhoun DA, McGlynn EA, Kalantar-Zadeh K, Jacobsen SJ. Characteristics of resistant hypertension in a large, ethnically diverse hypertension population of an integrated health system. Mayo Clin Proc. 2013;88:1099–107.
Simon TD, Berry J, Feudtner C, Stone BL, Sheng X, Bratton SL, Dean JM, Srivastava R. Children with complex chronic conditions in inpatient hospital settings in the United States. Pediatrics. 2010;126:647–55.
Sutherland JM, Steinum O. Hospital factors associated with clinical data quality. Health Policy. 2009;91:321–6.
Reed M, Huang J, Brand R, Graetz I, Neugebauer R, Fireman B, Jaffe M, Ballard DW, Hsu J. Implementation of an outpatient electronic health record and emergency department visits, hospitalizations, and office visits among patients with diabetes. JAMA. 2013;310:1060–5.
Demographics. The Arab American Institute. 2014. http://www.aaiusa.org/demographics. Accessed 28 Jan 2014.
Nasseri K. Construction and validation of a list of common Middle Eastern surnames for epidemiological research. Cancer Detect Prev. 2007;31:424–9.
Schwartz KL, Kulwicki A, Weiss LK, Fakhouri H, Sakr W, Kau G, Severson RK. Cancer among Arab Americans in the metropolitan Detroit area. Ethn Dis. 2004;14:141–6.
Perkins R. Evaluating the Passel-Word Spanish surname list: 1990 decennial census post enumeration survey results. Washington, DC: Population Division, U.S. Bureau of the Census; 1993. Working Paper No. 4. https://www.census.gov/population/www/documentation/twps0004.html. Accessed 28 Jan 2014.
Carroll NM, Ritzwoller DP, Stopponi MA, Johnson CC. Identifying and oversampling hispanics by the passel-word surname list for enrollment in a web-based nutritional intervention. Ethn Dis. 2010;20:15–21.
Wei II, Virnig BA, John DA, Morgan RO. Using a Spanish surname match to improve identification of Hispanic women in medicare administrative data. Health Serv Res. 2006;41:1469–81.
Nasseri K. Thyroid cancer in the Middle Eastern population of California. Cancer Causes Control. 2008;19:1183–91.
Nasseri K. Breast cancer in the Middle Eastern population of California, 1988–2004. Breast J. 2009;15:182–8.
Nasseri K, Mills PK, Allan M. Cancer incidence in the Middle Eastern population of California, 1988–2004. Asian Pac J Cancer Prev. 2007;8:405–11.
Schwartz K, Fakhouri M, Bartoces M, Monsur J, Younis A. Mammography screening among Arab American women in metropolitan Detroit. J Immigr Minor Health. 2008;10:541–9.
Dallo FJ, Schwartz K, Ruterbusch JJ, Booza J, Williams DR. Mortality rates among Arab Americans in Michigan. J Immigr Minor Health. 2012;14:236–41.
Dallo FJ, Borrell LN. Self-reported diabetes and hypertension among Arab Americans in the United States. Ethn Dis. 2006;16:699–705.
Dallo FJ, Kindratt TB, Snell T. Serious psychological distress among non-Hispanic whites in the United States: the importance of nativity status and region of birth. Soc Psychiatry Psychiatr Epidemiol. 2013;48:1923–30.
Schwartz K, Beebani G, Sedki M, Tahhan M, Ruterbusch JJ. Enhancement and validation of an Arab surname database. J Regist Manag. 2013;40:176–9.
Schwartz KL, Kulwicki A, Weiss LK, Fakhouri H, Sakr W, Kau G, Severson RK. Cancer among Arab Americans in the metropolitan Detroit area. Ethn Dis. 2004;14:141–6.
ICD-9-CM Volume 1 Diagnosis Codes. 2013. http://www.icd9data.com/. Accessed 28 Jan 2014.
Centers for Disease Control and Prevention. Classification of Diseases and Injuries. 2014. http://www.cdc.gov/nchs/icd/icd9cm.htm. Accessed 28 Jan 2014.
SAS Institute Inc. SAS 9.3. 2002–2010. Cary, NC: SAS Institute Inc.
Crude and Age-Adjusted Estimates for Chronic Health Conditions, Risk Factors, Health Indicators, and Preventive Health Practices by Expanded Race/Ethnicity. 2011–2013. https://www.michigan.gov/documents/mdch/2011-2013_Expanded_Race_Tables_FINAL_466325_7.pdf. Accessed 28 Jan 2014.
Jaber LA, Brown MB, Hammad A, Nowak SN, Zhu Q, Ghafoor A, Herman WH. Epidemiology of diabetes among Arab Americans. Diabetes Care. 2003;26:308–13.
Jamil H, Dallo F, Fakhouri M, Templin T, Khoury R, Fakhouri H. The prevalence of self-reported chronic conditions among Arab, Chaldean, and African Americans in southeast Michigan. Ethn Dis. 2009;19:293–300.
Jaber LA, Brown MB, Hammad A, Nowak SN, Zhu Q, Ghafoor A, Herman WH. Epidemiology of diabetes among Arab Americans. Diabetes Care. 2003;26:308–13.
Hajjar I, Kotchen TA. Trends in prevalence, awareness, treatment, and control of hypertension in the United States, 1988–2000. JAMA. 2003;290:199–206.
Jamil H, Fakhouri M, Dallo F, Templin T, Khoury R, Fakhouri H. Self-reported heart disease among Arab and Chaldean American women residing in southeast Michigan. Ethn Dis. 2008;18:19–25.
Jamil H, Dallo F, Fakhouri M, Templin T, Khoury R, Fakhouri H. The prevalence of self-reported chronic conditions among Arab, Chaldean, and African Americans in southeast Michigan. Ethn Dis. 2009;19:293–300.
Tailakh AK. Hypertension prevalence, awareness, adherence behaviors, and control among Arab Americans in Southern California. ProQuest Dissertations and Theses 2011.
Hekman K, Weir S, Fussman C, Lyon-Callo S. Health risk behaviors among Arab adults within the state of Michigan: 2013 Arab behavioral risk factor survey. Lansing, MI: Michigan Department of Health and Human Services, Lifecourse Epidemiology and Genomics Division and Health Disparities Reduction and Minority Health Section; 2015. http://www.michigan.gov/documents/mdch/Health_Risk_Behavior_Full_Arab_491350_7.pdf. Accessed 10 Oct 2015.
Moving toward health equity in Michigan: an overview. https://www.michigan.gov/documents/mdch/Health_Equity_Toolkit_Presentation_411023_7.pdf. Accessed 28 Jan 2014.
Lerner RC, Kirchner C. Social and economic characteristics of municipal hospital outpatients. Am J Public Health Nations Health. 1969;59:29–39.
Ullman R, Block JA, Stratmann WC. An emergency room’s patients: their characteristics and utilization of hospital services. Med Care. 1975;13:1011–20.
Wingert WA, Friedman DB, Larson WR. The demographical and ecological characteristics of a large urban pediatric outpatient population and implications for improving community pedatric care. Am J Public Health Nations Health. 1968;58:859–76.
Jamil H, Templin T, Fakhouri M, Rice VH, Khouri R, Fakhouri H, Al-omran H, Al-fauori I, Baker O. Comparison of personal characteristics, tobacco use, and health states in Chaldean, Arab American, and non-Middle Eastern White adults. J Immigr Minor Health. 2009;11:310–7.
Bergmans R, Soliman AS, Ruterbusch J, Meza R, Hirko K, Graff J, Schwartz K. Cancer incidence among Arab Americans in California, Detroit, and New Jersey SEER registries. Am J Public Health. 2014;104:e83–91.
Khan F, Ruterbusch JJ, Gomez SL, Schwartz K. Differences in the cancer burden among foreign-born and US-born Arab Americans living in metropolitan Detroit. Cancer Causes Control. 2013;24:1955–61.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any financial or non-financial conflicts of interest with this research study.
Human and animal rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Because this is a retrospective chart review, formal consent is not required.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Dallo, F.J., Ruterbusch, J.J., Kirma, J.D. et al. A Health Profile of Arab Americans in Michigan: A Novel Approach to Using a Hospital Administrative Database. J Immigrant Minority Health 18, 1449–1454 (2016). https://doi.org/10.1007/s10903-015-0296-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10903-015-0296-8