Abstract
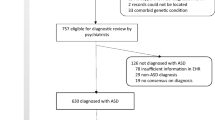
This study describes antipsychotic use and metabolic monitoring rates among individuals with developmental disabilities enrolled in a subspecialty medical home (N = 826). Four hundred ninety-nine participants (60.4 %) were taking antipsychotics, which was associated with male gender (p = 0.01), intellectual disability with and without autism spectrum disorder (p = 0.001 and p = 0.04, respectively), and inversely associated with the youngest and oldest age categories (p = 0.001 and p = 0.04, respectively). Among those taking antipsychotics, annual metabolic monitoring rates ranged from 89 % (lipids) to 99 % (weight). Age was positively associated with glucose (p < 0.001) and lipid monitoring (p < 0.001). Adult participants with dyslipidemia (p < 0.01), prediabetes/diabetes (p = 0.04), and hypertension (p = 0.02) were significantly more likely to obtain lipid monitoring. These values exceeded previously reported rates suggesting the importance of an integrated care model.
Similar content being viewed by others
References
Aman, M. G., Lam, K. L., & Van Bourgondien, M. E. (2005). Medication patterns in patients with autism: Temporal, regional, and demographic influences. Journal of Child and Adolescent Psychopharmacology, 15(1), 116–126.
Baburaj, R., & El Tahir, M. (2011). Monitoring for metabolic syndrome in people with intellectual disability on antipsychotic medication. Advances in Mental Health and Intellectual Disabilities, 5(3), 38–44.
Bansal, S., Buring, J., Rifai, N., Mora, S., Sacks, F. M., & Ridker, P. M. (2007). Fasting compared with nonfasting triglycerides and risk of cardiovascular events in women. Journal of American Medical Association, 298(3), 309–316.
Barnes, T. P. (2008). Screening for the metabolic syndrome in community psychiatric patients prescribed antipsychotics: A quality improvement programme. Acta Psychiatrica Scandinavica, 118(1), 26–33.
Bhaumik, S. W. (2008). Body mass index in adults with intellectual disability: Distribution, associations and service implications: A population-based prevalence study. Journal of Intellectual Disability Research, 52(4), 287–298.
Buck, T. R., Viskochil, J., Farley, M., Coon, H., McMahon, W. M., Morgan, J., & Bilder, D. A. (2014). Psychiatric comorbidity and medication use in adults with autism spectrum disorder. Journal of Autism and Developmental Disorders, 44(12), 3063–3071.
Consensus development conference on antipsychotic drugs and obesity and diabetes. (2004). Journal of Clinical Psychiatry, 65(2), 267–272. doi:10.4088/JCP.v65n0219
Coury, D. L., Anagnostou, E., Manning-Courtney, P., Reynolds, A., Cole, L., McCoy, R., & Perrin, J. M. (2012). Use of psychotropic medication in children and adolescents with autism spectrum disorders. Pediatrics, 130(Suppl 2), S69–S76.
Devapriam, J., Anand, A., Raju, L., & Bhaumik, S. (2009). Monitoring for metabolic syndrome in adults with intellectual disability on atypical antipsychotic drugs. British Journal of Developmental Disabilities, 55(Part 1(108)), 3–13.
Eberly, L. E., Stamler, J., & Neaton, J. D. (2003). Relation of triglyceride levels, fasting and nonfasting, to fatal and nonfatal coronary heart disease. Archives of Internal Medicine, 163(1), 1077–1083.
Fontaine, K. R., Heo, M., Harrigan, E. P., Shear, C. L., Lakshminarayanan, M., Casey, D. E., & Allison, D. B. (2001). Estimating the consequences of anti-psychotic induced weight gain on health and mortality rate. Psychiatry Research, 101(3), 277–288. doi:10.1016/S0165-1781(01)00234-7.
Frighi, V., Stephenson, M. T., Morovat, A., Jolley, I. E., Trivella, M., Dudley, C. A., & Goodwin, G. M. (2011). Safety of antipsychotics in people with intellectual disability. The British Journal of Psychiatry: The Journal of Mental Science, 199(4), 289–295. doi:10.1192/bjp.bp.110.085670.
Ghate, S. I. (2012). Predictors of metabolic parameter monitoring in adolescents on antipsychotics in a primary care setting. Mental Health In Family Medicine, 9(3), 137–148.
Haupt, D. W., Rosenblatt, L. C., Kim, E., Baker, R. A., Whitehead, R., & Newcomer, J. W. (2009). Prevalence and predictors of lipid and glucose monitoring in commercially insured patients treated with second-generation antipsychotic agents. The American Journal of Psychiatry, 166(3), 345–353.
Hsu, C., Ried, L. D., Bengtson, M. A., Garman, P. M., McConkey, J. R., & Rahnavard, F. (2008). Metabolic monitoring in veterans with schizophrenia-related disorders and treated with second-generation antipsychotics: Findings from a Veterans Affairs-based population. Journal of the American Pharmacists Association: Japha, 48(3), 393–400. doi:10.1331/JAPhA.2008.07007.
Koch, D. A., & Scott, A. J. (2012). Weight gain and lipid–glucose profiles among patients taking antipsychotic medications: Comparisons for prescriptions administered using algorithms versus usual care. Journal of Psychiatric and Mental Health Nursing, 19(5), 389–394. doi:10.1111/j.1365-2850.2011.01781.x.
Mitchell, A. J., Delaffon, V., Vancampfort, D., Correll, C. U., & De Hert, M. (2012). Guideline concordant monitoring of metabolic risk in people treated with antipsychotic medication: Systematic review and meta-analysis of screening practices. Psychological Medicine, 42(1), 125–147. doi:10.1017/S003329171100105X.
Moeller, K. E., Rigler, S. K., Mayorga, A., Nazir, N., & Shireman, T. I. (2011). Quality of monitoring for metabolic effects associated with second generation antipsychotics in patients with schizophrenia on public insurance. Schizophrenia Research, 126(1–3), 117–123. doi:10.1016/j.schres.2010.11.015.
Morgan, C. N., Roy, M., & Chance, P. (2003). Psychiatric comorbidity and medication use in autism: A community survey. Psychiatric Bulletin, 27(10), 378–381. doi:10.1192/pb.27.10.378.
Morrato, E., Nicol, G., Maahs, D., Druss, B., Hartung, D., Valuck, R., & Newcomer, J. (2010). Metabolic screening in children receiving antipsychotic drug treatment. Archives of Pediatrics and Adolescent Medicine, 164(4), 344–351. doi:10.1001/archpediatrics.2010.48.
Mukherjee, S., Schnur, D. B., & Reddy, F. (1989). Family history of type 2 diabetes in schizophrenia patients. Lancet, 1, 495.
Nordestgaard, B. G., Benn, M., Schnohr, P., & Tybjærg-Hansen, A. (2007). Nonfasting triglycerides and risk of myocardial infarction, ischemic heart disease, and death in men and women. Journal Of American Medical Association, 298(3), 299–308.
Paton, C. T. (2011). Nature and quality of antipsychotic prescribing practice in UK psychiatry of intellectual disability services. Journal of Intellectual Disability Research, 55(7), 665–674.
Ryan, M. C., Collins, P., & Thakore, M. B. (2003). Impaired fasting glucose tolerance in first-episode, drug-naïve patients with schizophrenia. American Journal of Psychiatry, 160(2), 284–289.
Shi, L., Ascher-Svanum, H., Chiang, Y., Zhao, Y., Fonseca, V., & Winstead, D. (2009). Predictors of metabolic monitoring among schizophrenia patients with a new episode of second-generation antipsychotic use in the Veterans Health Administration. BMC Psychiatry. doi:10.1186/1471-244X-9-80.
Teeluckdharry, S., Sharma, S., O’Rourke, E., Tharian, P., Gondalekar, A., Nainar, F., & Roy, M. (2013). Monitoring metabolic side effects of atypical antipsychotics in people with an intellectual disability. Journal of Intellectual Disabilities, 17(3), 223–235. doi:10.1177/1744629513495261.
Tsiouris, J., Kim, S., Brown, W., Pettinger, J., & Cohen, I. (2013). Prevalence of psychotropic drug use in adults with intellectual disability: Positive and negative findings from a large scale study. Journal of Autism and Developmental Disorders, 43(3), 719–731.
Weedon, D., Carbone, P., Bilder, D., O’Brien, S., & Dorius, J. (2012). Building a person-centered medical home: Lessons from a program for people with developmental disabilities. Journal of Health Care for the Poor and Underserved, 23(4), 1600–1608.
Wysokiński, A., Kowman, M., & Kłoszewska, I. (2012). The prevalence of metabolic syndrome and Framingham cardiovascular risk scores in adult inpatients taking antipsychotics—a retrospective medical records review. Psychiatria Danubina, 24(3), 314–322.
Acknowledgments
We are grateful for the participation of our HOME Program clients and the support we received from Kimberly Treadway, Nirupma Singh, Kirk Stephens and our partners in the Utah Department of Health’s Medicaid Program.
Author Contributions
Dr. Ruiz assisted with the conceptualization of the study through her review of the relevant literature, wrote the initial draft of the introduction and discussion sections, reviewed and revised the manuscript, and approved the final manuscript as submitted; Ms. Damron coordinated the data collection, wrote the methods section, reviewed and revised the manuscript, and approved the final manuscript as submitted; Dr. Jones provided expertise in the conceptualization of the study, reviewed and revised the manuscript, and approved the final version of the manuscript as submitted; Mr. Weedon provided critical insight into all aspects of this study’s conceptualization, reviewed and revised the manuscript, and approved the final manuscript as submitted. Dr. Carbone provided expertise in the conceptualization of the study, reviewed and revised the manuscript, and approved the final version of the manuscript as submitted; Dr. Bakian supervised the data analysis, wrote the results section, reviewed and revised the manuscript, and approved the final manuscript as submitted. Dr. Bilder conceptualized and designed the study, revised the initial manuscript, and approved the final manuscript as submitted.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ruiz, L.M., Damron, M., Jones, K.B. et al. Antipsychotic Use and Metabolic Monitoring in Individuals with Developmental Disabilities Served in a Medicaid Medical Home. J Autism Dev Disord 46, 1887–1894 (2016). https://doi.org/10.1007/s10803-016-2712-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-016-2712-x