Abstract
Purpose
Circulating endothelial progenitor cells (cEPCs) are vital to vascular repair by re-endothelialization. We aimed to explore the effect of proprotein convertase subtilisin kexin type 9 inhibitors (PCSK9i) on cEPCs hypothesizing a possible pleiotropic effect.
Methods
Patients with cardiovascular disease (CVD) were sampled for cEPCs at baseline and following the initiation of PCSK9i. cEPCs were assessed using flow cytometry by the expression of CD34(+)/CD133(+) and vascular endothelial growth factor receptor (VEGFR)-2(+), and by the formation of colony-forming units (CFUs) and production of VEGF.
Results
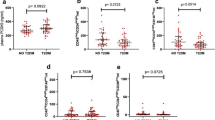
Our cohort included 26 patients (median age 68 (IQR 63, 73) years; 69% male). Following 3 months of treatment with PCSK9i and a decline in low-density lipoprotein cholesterol levels (153 (IQR 116, 176) to 56 (IQR 28, 72) mg/dl), p < 0.001), there was an increase in CD34(+)/CD133(+) and VEGFR-2(+) cell levels (0.98% (IQR 0.37, 1.55) to 1.43% (IQR 0.90, 4.51), p = 0.002 and 0.66% (IQR 0.22, 0.99) to 1.53% (IQR 0.73, 2.70), p = 0.05, respectively). Functionally, increase in EPCs-CFUs was microscopically evident following treatment with PCSK9i (1 CFUs (IQR 0.0, 1.0) to 2.5 (IQR 1.5, 3), p < 0.001) with a concomitant increase in EPC’s viability as demonstrated by an MTT assay (0.15 (IQR 0.11, 0.19) to 0.21 (IQR 0.18, 0.23), p < 0.001). VEGF levels increased following PCSK9i treatment (57 (IQR 18, 24) to 105 (IQR 43, 245), p = 0.006).
Conclusions
Patients with CVD treated with PCSK9i demonstrate higher levels of active cEPCs, reflecting the promotion of endothelial repair. These findings may represent a novel mechanism of action of PCSK9i.




Similar content being viewed by others
Data Availability
Data will be made available by the corresponding author upon request.
References
Steg PG, Szarek M, Bhatt DL, Bittner VA, Bregeault MF, Dalby AJ, et al. Effect of alirocumab on mortality after acute coronary syndromes. Circulation. 2019;140(2):103–12.
Sabatine MS, Giugliano RP, Keech AC, Honarpour N, Wiviott SD, Murphy SA, et al. Evolocumab and clinical outcomes in patients with cardiovascular disease. N Engl J Med. 2017;376(18):1713–22.
Eisen A, Giugliano RP. Advances in the field of proprotein convertase subtilisin kexin type 9 inhibitors. Curr Opin Cardiol. 2016;31(6):644–53.
Karagiannis AD, Liu M, Toth PP, Zhao S, Agrawal DK, Libby P, et al. Pleiotropic anti-atherosclerotic effects of PCSK9 inhibitors from molecular biology to clinical translation. Curr Atheroscler Rep. 2018;20(4):20.
Ferri N, Tibolla G, Pirillo A, Cipollone F, Mezzetti A, Pacia S, et al. Proprotein convertase subtilisin kexin type 9 (PCSK9) secreted by cultured smooth muscle cells reduces macrophages LDLR levels. Atherosclerosis. 2012;220(2):381–6.
Hill JM, Zalos G, Halcox JP, Schenke WH, Waclawiw MA, Quyyumi AA, et al. Circulating endothelial progenitor cells, vascular function, and cardiovascular risk. N Engl J Med. 2003;348(7):593–600.
Lasala GP, Silva JA, Kusnick BA, Minguell JJ. Combination stem cell therapy for the treatment of medically refractory coronary ischemia: a phase I study. Cardiovasc Revasc Med. 2011;12(1):29–34.
Li CJ, Gaol RL, Yang YJ, Hu FH, Yang WX, You SJ, et al. Effect of intracoronary infusion of bone marrow mononuclear cells or peripheral endothelial progenitor cells on myocardial ischemia-reperfusion injury in mini-swine. Chin Med Sci J. 2010;25(3):176–81.
Fadini GP, Losordo D, Dimmeler S. Critical reevaluation of endothelial progenitor cell phenotypes for therapeutic and diagnostic use. Circ Res. 2012;110(4):624–37.
Friedrich EB, Walenta K, Scharlau J, Nickenig G, Werner N. CD34-/CD133+/VEGFR-2+ endothelial progenitor cell subpopulation with potent vasoregenerative capacities. Circ Res. 2006;98(3):e20–5.
Werner N, Kosiol S, Schiegl T, Ahlers P, Walenta K, Link A, et al. Circulating endothelial progenitor cells and cardiovascular outcomes. N Engl J Med. 2005;353(10):999–1007.
Hur J, Yoon CH, Kim HS, Choi JH, Kang HJ, Hwang KK, et al. Characterization of two types of endothelial progenitor cells and their different contributions to neovasculogenesis. Arterioscler Thromb Vasc Biol. 2004;24(2):288–93.
Balistreri CR, Buffa S, Pisano C, Lio D, Ruvolo G, Mazzesi G. Are endothelial progenitor cells the real solution for cardiovascular diseases? Focus on controversies and perspectives. Biomed Res Int. 2015;2015:835934–17.
Lev EI, Leshem-Lev D, Mager A, Vaknin-Assa H, Harel N, Zimra Y, et al. Circulating endothelial progenitor cell levels and function in patients who experienced late coronary stent thrombosis. Eur Heart J. 2010;31(21):2625–32.
Chen JZ, Zhu JH, Wang XX, Zhu JH, Xie XD, Sun J, et al. Effects of homocysteine on number and activity of endothelial progenitor cells from peripheral blood. J Mol Cell Cardiol. 2004;36(2):233–9.
Ruggeri A, Paviglianiti A, Volt F, Kenzey C, Rafii H, Rocha V, et al. Endothelial and circulating progenitor cells in hematological diseases and allogeneic hematopoietic stem cell transplantation. Curr Med Chem. 2018;25(35):4535–44.
Kondo T, Hayashi M, Takeshita K, Numaguchi Y, Kobayashi K, Iino S, et al. Smoking cessation rapidly increases circulating progenitor cells in peripheral blood in chronic smokers. Arterioscler Thromb Vasc Biol. 2004;24(8):1442–7.
Benndorf RA, Gehling UM, Appel D, Maas R, Schwedhelm E, Schlagner K, et al. Mobilization of putative high-proliferative-potential endothelial colony-forming cells during antihypertensive treatment in patients with essential hypertension. Stem Cells Dev. 2007;16(2):329–38.
Rupp S, Badorff C, Koyanagi M, Urbich C, Fichtlscherer S, Aicher A, et al. Statin therapy in patients with coronary artery disease improves the impaired endothelial progenitor cell differentiation into cardiomyogenic cells. Basic Res Cardiol. 2004;99(1):61–8.
Eisen A, Leshem-Lev D, Yavin H, Orvin K, Mager A, Rechavia E, et al. Effect of high dose statin pretreatment on endothelial progenitor cells after percutaneous coronary intervention (HIPOCRATES study). Cardiovasc Drugs Ther. 2015;29(2):129–35.
Tang ZH, Peng J, Ren Z, Yang J, Li TT, Li TH, et al. New role of PCSK9 in atherosclerotic inflammation promotion involving the TLR4/NF-kappaB pathway. Atherosclerosis. 2017;262:113–22.
Ruscica M, Tokgözoğlu L, Corsini A, Sirtori CR. PCSK9 inhibition and inflammation: a narrative review. Atherosclerosis. 2019;288:146–55.
Ding Z, Liu S, Wang X, Deng X, Fan Y, Sun C, et al. Hemodynamic shear stress via ROS modulates PCSK9 expression in human vascular endothelial and smooth muscle cells and along the mouse aorta. Antioxid Redox Signal. 2015;22(9):760–71.
Ding Z, Liu S, Wang X, Deng X, Fan Y, Shahanawaz J, et al. Cross-talk between LOX-1 and PCSK9 in vascular tissues. Cardiovasc Res. 2015;107(4):556–67.
Ruscica M, Ferri N, Fogacci F, Rosticci M, Botta M, Marchiano S, et al. Circulating levels of proprotein convertase subtilisin/kexin type 9 and arterial stiffness in a large population sample: data from the Brisighella Heart Study. J Am Heart Assoc. 2017;6(5):e005764.
Werner C, Hoffmann MM, Winkler K, Böhm M, Laufs U. Risk prediction with proprotein convertase subtilisin/kexin type 9 (PCSK9) in patients with stable coronary disease on statin treatment. Vasc Pharmacol. 2014;62(2):94–102.
Macchi C, Banach M, Corsini A, Sirtori CR, Ferri N, Ruscica M. Changes in circulating pro-protein convertase subtilisin/kexin type 9 levels – experimental and clinical approaches with lipid-lowering agents. Eur J Prev Cardiol. 2019;26:204748731983150–949.
Gauthier MS, Awan Z, Bouchard A, Champagne J, Tessier S, Faubert D, et al. Posttranslational modification of proprotein convertase subtilisin/kexin type 9 is differentially regulated in response to distinct cardiometabolic treatments as revealed by targeted proteomics. J Clin Lipidol. 2018;12(4):1027–38.
Shapiro MD, Miles J, Tavori H, Fazio S. Diagnosing resistance to a proprotein convertase subtilisin/kexin type 9 inhibitor. Ann Intern Med. 2018;168(5):376–9.
Nicholls SJ, Puri R, Anderson T, Ballantyne CM, Cho L, Kastelein JJ, et al. Effect of Evolocumab on progression of coronary disease in statin-treated patients: the GLAGOV randomized clinical trial. Jama. 2016;316(22):2373–84.
Schuster S, Rubil S, Endres M, Princen HMG, Boeckel J-N, Winter K, et al. Anti-PCSK9 antibodies inhibit pro-atherogenic mechanisms in APOE*3Leiden.CETP mice. Sci Rep. 2019;9(1):11079.
Kuliczkowski W, Derzhko R, Prajs I, Podolak-Dawidziak M, Serebruany VL. Endothelial progenitor cells and left ventricle function in patients with acute myocardial infarction: potential therapeutic considertions. Am J Ther. 2012;19(1):44–50.
Sun H, Krauss RM, Chang JT, Teng BB. PCSK9 deficiency reduces atherosclerosis, apolipoprotein B secretion, and endothelial dysfunction. J Lipid Res. 2018;59(2):207–23.
Funding
This study was supported by an unrestricted research grant from AMGEN pharmaceutical company (Protocol #20197006).
Author information
Authors and Affiliations
Contributions
A.E., E.L., and D.L.L. contributed to the study conception and design. Material preparation, data collection, and analysis were performed by O.I.B.Z. and D.L.L. The first draft of the manuscript was written by O.I.B.Z and all authors commented on previous versions of the manuscript. A.E., E.L., D.L.L., A.M., and R.K. read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 2332 kb)
Rights and permissions
About this article
Cite this article
Itzhaki Ben Zadok, O., Mager, A., Leshem-Lev, D. et al. The Effect of Proprotein Convertase Subtilisin Kexin Type 9 Inhibitors on Circulating Endothelial Progenitor Cells in Patients with Cardiovascular Disease. Cardiovasc Drugs Ther 36, 85–92 (2022). https://doi.org/10.1007/s10557-020-07119-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-020-07119-1