Abstract
Purpose
Phosphate and tensin homolog (PTEN), a negative regulator of PI3K signaling, is involved in DNA repair. ATR is a key sensor of DNA damage and replication stress. We evaluated whether ATR signaling has clinical significance and could be targeted by synthetic lethality in PTEN-deficient triple-negative breast cancer (TNBC).
Methods
PTEN, ATR and pCHK1Ser345 protein level was evaluated in 1650 human breast cancers. ATR blockade by VE-821 was investigated in PTEN-proficient- (MDA-MB-231) and PTEN-deficient (BT-549, MDA-MB-468) TNBC cell lines. Functional studies included DNA repair expression profiling, MTS cell-proliferation assay, FACS (cell cycle progression & γH2AX accumulation) and FITC-annexin V flow cytometry analysis.
Results
Low nuclear PTEN was associated with higher grade, pleomorphism, de-differentiation, higher mitotic index, larger tumour size, ER negativity, and shorter survival (p values < 0.05). In tumours with low nuclear PTEN, high ATR and/or high pCHK1ser345 level was also linked to higher grade, larger tumour size and poor survival (all p values < 0.05). VE-821 was selectively toxic in PTEN-deficient TNBC cells and resulted in accumulation of double-strand DNA breaks, cell cycle arrest, and increased apoptosis.
Conclusion
ATR signalling adversely impact survival in PTEN-deficient breast cancers. ATR inhibition is synthetically lethal in PTEN-deficient TNBC cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Phosphate and tensin homolog (PTEN) is a key tumor suppressor [5, 7, 14, 22]. Mutations in PTEN have been reported in several tumours including brain, prostrate, melanoma, endometrial and breast cancers. Cytoplasmic PTEN serves as a negative regulator of PI3K/AKT signaling pathway. More recently, nuclear PTEN has been shown to have roles in DNA repair [5, 7, 14, 22]. Ataxia telangiectasia-mutated- and Rad3-related protein (ATR), a serine threonine kinase belonging to the PIKK family (phosphoinositide 3-kinase-like-family of protein kinase), is a critical regulator of DNA repair and genomic integrity [9, 10, 19, 20]. ATR can be activated by single stranded (ss)–double stranded (ds) DNA junctions generated at sites of DNA damage, during nucleotide excision repair, at resected double-strand breaks and stalled replication forks. Activated ATR in turn phosphorylates Chk1 at Ser345 and Ser317, as well as several other target proteins involved in homologous recombination repair and DNA cross-link repair. Phosphorylation of Chk1 at Ser345 (pChk1) leads to its activation which further coordinates cell cycle progression and DNA repair [9, 10, 19, 20].
In the current study, we provide evidence that ATR and pChk1 expression in of PTEN-deficient breast cancer adversely impact on survival. ATR inhibition is synthetically lethal in PTEN-deficient TNBC cells implying a promising personalized therapy approach in breast cancers.
Patients and methods
Clinical study
Patient characteristics and tissue microarray (TMA)
The Nottingham Tenovus Primary Series is a well-characterized consecutive cohort of early-stage primary operable invasive BC patients from which the samples were used for the TMA construction [1, 2, 4, 21]. Patient demographics are summarized in Supplementary Table S1. Breast cancer specific survival (BCSS) was defined as the number of months from diagnosis to the occurrence of BC-related death. Survival was censored if the patient was still alive at the time of analysis, lost to follow-up, or died from other causes.
Immunohistochemistry (IHC)
A mouse monoclonal PTEN antibody clone 6H2.1 (Dako, Denmark) was diluted in 1:20 dilution using Leica Antibody diluent. Antigen retrieval was performed as follows: the TMA slides were incubated at 98 °C (in water bath) for 25 min in target retrieval solution (pH 9.0; Leica Microsystems, Newcastle, UK) then the slides were incubated for 10 min at room temperature in warm Tris buffer saline (TBS, pH 7.6, 50 °C). Finally, slides were cooled by flooding in cold water (pH 6.0) for 5 min. The primary antibody was incubated for 1 h at room temperature. The Novocastra Novolink Max Polymer Detection Systems (RE7280-K: 1250 tests, Leica Biosystems) was used to visualise the staining. Briefly, the slides were heated at 60 °C for 10 min for dewaxing. Following cooling of samples to room temperature, the slides were rehydrated using a Leica Autostainer. After performing antigen retrieval, the slides were loaded onto Shandon Cover plates and fitted on sequenza plates for IHC. Initially, Endogenous peroxidase was blocked for 5 min, and then a protein block was applied for 5 min. The PTEN antibody was added, and the slides were incubated for 1 h at room temperature. After this, post-primary block was run for 30 min and then polymer was applied for further 30 min. The chromogen (DAB) was applied for 5 min, and tissues were counter-stained with haematoxylin for 6 min. Slides were dehydrated using Leica Autostainer and mounted with DPX. Negative (omission of the primary antibody) and positive controls were included according to manufacturer datasheet. ATR and pChk1 staining have been reported previously. Optimisation, specificity and cut-off points of ATR and pChk1 antibodies used in the current study have been reported previously [1]. A set of slides were incubated for 18 h at 4 °C with the primary mouse monoclonal anti-ATR antibody, clone 1E9 (H00000545-M03, Novus Biologicals, Cambridge, UK), at a dilution of 1:20. A further set of slides were incubated for 60 min with the primary rabbit polyclonal anti-phosphorylated Chk1 antibody (Ab58567, Abcam, Cambridge, UK), at a dilution of 1:140 [1].
Evaluation of immunohistochemical staining
The TMA slides were initially assessed through staining quality and specificity under light microscope. Slides were then scanned into high-resolution digital images (0.45 lm/pixel) using a NanoZoomer slide scanner (Hamamtsu Photonics, Welwyn Garden City, UK) and accessed using a web-based interface (Distiller, SlidePath Ltd, Dublin, Ireland). They were scored at ×20 magnification using a minimum of 2400 high-resolution screen (1920 × 1080). Assessment of staining was based on a semi-quantitative approach using a modified histochemical score (H-score) taking the intensity of staining and the percentage of stained cells into account. For the intensity, a score index of 0, 1, 2, and 3 was used, which corresponded to negative, weak, moderate, and strong staining intensity, respectively. The percentage of positive cells per intensity was estimated. PTEN staining in breast tumour cells was detected in the nuclei and cytoplasm of the breast cancer cells. Cut-off was used to classify the tumours with a nuclear-PTEN H-score equal to ‘0’ as negative, and those with an H-score more than 0 as positive. H-score > 90 was taken as the cut-off for high cytoplasmic-PTEN expression. Optimisation, specificity and cut-off points of ATR and pChk1 antibodies used in the current study have been reported previously [1]. H-score of ≥ 60 was taken as the cut-off for high ATR expression, H-score of ≥ 50 was taken as the cut-off for high cytoplasmic pChk1 expression and H-score of ≥ 50 was taken as the cut-off for high nuclear pChk1 expression.
Tumor marker prognostic studies (REMARK) criteria, recommended by McShane et al. [13], were followed throughout this study. Ethical approval was obtained from the Nottingham Research Ethics Committee (C202313).
Statistical analysis
Statistical analysis was performed using SPSS v 22 statistical software. Association with clinical and biological markers was assessed using Chi-squared test. Kaplan–Meier survival curve with log-rank test was plotted to determine the survival distribution of studied patients’ subgroups. Statistical significance was defined as p value ≤ 0.05. Due to multiple comparisons, the adjustment for p values of multiple testing was used according to Benjamini–Hochberg correction method.
Pre-clinical study
Cell lines, tissue culture and chemical reagents
MDA-MB-231 human breast cancer cell line was purchased from American Type culture collection (ATCC, Manassas, USA) and was grown as per ATCC recommendations. MDA-MB-231 cells were cultured in RPMI-1640 medium (Sigma, St. Louis, MO, USA) and Minimum Essential Medium Eagle (Sigma-Aldrich) supplemented with 1% l-glutamine (200 mM) and 1% non-essential amino acids (0.1 mM), respectively. The breast cancer cell lines BT-549 and MDA-MB-468 (Cell Line Service, Eppelheim, Germany) were cultured in Dulbecco’s Modified Eagle Medium/Nutrient Mixture F-12 (Gibco, Carlsbad, USA). All media were supplemented with 10% foetal bovine serum (Sigma) and 1% penicillin/streptomycin (10,000 units penicillin and 10 mg streptomycin/mL) (Sigma, Gillingham, UK). All cell lines were cultured as adherent cultures in a humidified 5% CO2 incubator at 37 °C. ATR inhibitor (VE-821, 10 mM in 1 mL DMSO) was purchased from Selleckchem (Houston, TX, USA). DMSO (Sigma, Gillingham, UK) was used as solvent to dissolve VE-821 and was tested solely as a vehicle control (< 0.1% v/v).
qRT-PCR analysis of DNA repair gene expression in breast cancer cell lines
Real-time PCR was performed using RT2 Profiler DNA Repair PCR Array for 84 DNA repair genes in duplicates as described previously [3]. The data were analyzed as per manufacturer’s recommendations. GAPDH was used for normalization of the data. A twofold change or above in expression was considered significant. All experiments were performed in duplicate.
Western blot analysis
To evaluate the specificity of PTEN-antibody used for the immunohistochemical study, cell lysates were prepared and Western blot analysis was performed. The primary antibodies for PTEN, ATR, and β-actin used in this study were incubated at room temperature for 1 h (PTEN 1:100 dilution [Dako], ATR 1:1000 dilution [Cell signaling] and β-actin 1:5000 dilution [Sigma]). Infrared dye-labelled secondary antibodies (Li-Cor) [IRDye 800CW Donkey Anti-Rabbit IgG and IRDye 680CW Donkey Anti-Mouse IgG] were incubated at a dilution of 1:10,000 for 1 h. Membranes were scanned with a Li-Cor Odyssey machine (700 and 800 nm) to determine protein expression.
MTS cell proliferation assay
Cells were seeded at a density of 1000 cells per well in 96-well plates and allowed to adhere overnight. Inhibitory compounds were added to samples in plates at a range of concentrations after 16 h, followed by incubation of plates for total of 5 days. All steps of MTS assay were performed as per manufacturer’s recommendations. All experiments were performed in triplicate at least three times. Data analysis was performed in Microsoft Excel 2010 (Microsoft, Redmond, USA) and GraphPad Prism 6 (GraphPad, La Jolla, USA).
γH2AX accumulation and cell cycle analysis by flow cytometry
1 × 105 cells were seeded in 6-well tissue culture plates, and were allowed to adhere overnight. VE-821, an ATR inhibitor, was added after 16 h at the concentration of 5 μM. Cells were harvested by trypsinisation and centrifuged at 1000 rpm for 5 min at 24 and 48 h post drug exposure. Cells pellets were then re-suspended in 1 mL of 70% ice-cold ethanol to fix the cells. Following this, samples were stored at 4 °C. Suspensions were centrifuged at 1000 rpm for 5 min followed by removal of the supernatant. Samples were processed using H2AX Phosphorylation Assay Kit (Merckmillipore, Nottingham, UK) as per manufacturer’s recommendations. At least 10,000 cells from each sample were analysed. All experiments were done in duplicate three times. Weasel (Victoria, Australia) flow cytometry analysis software was used for data analysis. Graphical representation and statistical analysis was performed in GraphPad Prism 6 (GraphPad, La Jolla, USA).
Apoptosis detection by FITC-Annexin V flow cytometry
1 × 105 cells were seeded into 6-well tissue culture plates and allowed to adhere overnight. VE-821 was added to tissue culture plates at a concentration of 5 μM after 16 h. 24 and 48 h after VE-821 administration. For detection of apoptosis, FITC-Annexin V flow cytometry was performed using the fluorescein isothiocyanate [FITC]-Annexin V Apoptosis Detection Kit I (BD Pharmingen, San Jose, USA) as per manufacturer’s recommendations. At least 10,000 cells from each sample were analysed. Weasel (Victoria, Australia) flow cytometry analysis software was used for data analysis. The percentage of apoptotic cells (FITC-Annexin V positive, PI positive and FITC-Annexin V positive, PI negative) in the treated population was ascertained by comparing it to a control population of untreated samples. Statistical analysis was performed in GraphPad Prism 6 (GraphPad, La Jolla, USA). All experiments were done in duplicate three times.
Results
Loss of nuclear PTEN and aggressive breast cancers
The loss of nuclear PTEN expression was observed in 508/811 (62.6%) tumours compared with 303/811 (37.4%) tumours which had positive expression of nuclear (PTEN). Low cytoplasmic PTEN expression was seen in 326/811 (40.2%) tumours compared with the 485/811 (59.8%) tumours which had high cytoplasmic expression (Fig. 1a). The negative nuclear PTEN was associated with higher grade, less tubule formation, pleomorphism, higher mitotic index, larger tumour size, high-risk Nottingham Prognostic Index (NPI), ER− and PR− tumours (all adjusted p values < 0.01) (Table 1). Similarly, low cytoplasmic PTEN was also associated with aggressive phenotype including high grade, de-differentiation, higher mitotic index and larger tumours (all adjusted p values < 0.005) (Table 2).
a Nuclear and cytoplasmic staining of PTEN [a negative staining for both, b negative staining for nuclei and weak for cytoplasm, c some weak staining for nuclei and moderate for cytoplasm d strong staining for both; TMA cores pictures were taken using digital pathology interference at ×100 (left) and ×200 (right)]. Kaplan–Meier plot showing breast cancer-specific survival (BCSS) and b nuclear PTEN level. c combined nuclear PTEN and ATR level. d combined nuclear PTEN and cytoplasmic pCHK1 level. e combined ATR and cytoplasmic pCHK1 level nuclear PTEN negative tumours
PTEN, ATR, and pChk1ser345 co-expression and survival
A previous preclinical study has shown that loss of PTEN and activation of AKT can impair Chk1 through phosphorylation, reduce nuclear localization, promote cytoplasmic sequestration, ubiquitination and degradation [18]. Loss of nuclear PTEN can also promote genomic instability and DNA strand breaks which can activate ATR. We, therefore, investigated PTEN, ATR, and pChk1ser345 co-expression in clinical breast cancers. A strong association between negative nuclear PTEN and negative nuclear pChk1 expression was observed. Interestingly, there was also a significant association between low cytoplasmic PTEN and low ATR as well low-cytoplasmic Chk1 expression (Table 3). We then proceeded to evaluate prognostic significance of PTEN, ATR, and pChk1ser345 co-expression.
The nuclear PTEN negativity was associated with shorter breast cancer-specific survival (BCSS) (p = 0.005) compared to nuclear PTEN-positive breast cancer (Fig. 1b). In contrast cytoplasmic PTEN did not influence survival (Supplementary Fig. S1A). When combined together, we observed that tumours with nuclear PTEN-negative/cytoplasmic PTEN-positive tumours had the worst BCSS (p = 0.039) (Supplementary Fig. S1B).
We then investigated the prognostic significance of PTEN, ATR and pChk1ser345 co-expression in patients. Nuclear PTEN negative/high ATR tumours were associated with the worst BCSS (p = 0.029) (Fig. 1c). Similarly, nuclear PTEN-negative/high-cytoplasmic pCHK1ser345 tumours were associated with poor survival (p = 0.031) (Fig. 1d). Nuclear PTEN-negative/high-nuclear pCHK1ser345 tumours were also associated with poor survival (p = 0.037) (Supplementary Fig. 1c). In nuclear PTEN-negative tumours, we then investigated the prognositic significance of ATR- cytoplasmic pCHK1ser345 co-expression. As shown in Fig. 1e, tumours with high-ATR and -cytoplasmic pCHK1ser345 expression had the worst survival compared to those with low-ATR and-cytoplasmic expression (p = 0.014).
ATR and/or pCHK1ser345 did not influence survival in tumours with low- or high-cytoplasmic PTEN expression (Supplementary Fig. S1D–S1G).
Taken together, the clinical data suggest that nuclear PTEN deficiency as well as ATR and pChk1ser345 expression in nuclear PTEN-deficient breast cancers is associated with aggressive breast cancers.
PTEN-deficient breast cancer cell lines demonstrate deregulation in gene expression of multiple DNA repair pathways
We initially screened a panel of TNBC cell lines for expression of PTEN, ATR, total Chk1 and pChk1ser345. As shown in Fig. 2a, MDA-MB-231 cell line is PTEN-proficient, whereas BT-549 and MDA-MB-468 cell lines are PTEN deficient. We did not observe any significant differences in the expression of ATR in MDA-MB-231, BT-549 and MDA-MB-468 TNBC cell lines (Fig. 2a). Previous studies suggest that nuclear PTEN may have roles in DNA repair including in homologous recombination repair. To test whether BT-549 and MDA-MB-468 cells have altered DNA repair expression compared to MDA-MB-231 cells, we profiled the mRNA level expression of 84 DNA repair genes using the RT2-Profiler DNA Repair PCR array. The expression of DNA repair genes in BT-549 and MDA-MB-468 cells was compared with DNA repair expression in MDA-MB-231. The data are shown in Fig. 2b, c as well as in Supplementary Tables S2–S7. We observed more than two-fold downregulation of several genes in HR, BER, NHEJ, MMR and NER. Interestingly, in MDA-MB-468, we observed upregulation of PARP2, XRCC6BP1, LIG1, RPA3 and MGMT. In BT-549 cells, DMC1, XRCC6BP1 and MGMT were significantly upregulated. The data would not only concur with previously published data but also support the hypothesis that PTEN deficiency can alter DNA repair expression status in cells.
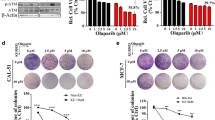
a Western blotting analysis for PTEN, ATR expression in breast cancer cell lines. b DNA repair expression profiling in BT549 cells compared to MDA-MB-231 cells. c DNA repair expression profiling in MDA-MB-468 cells compared to MDA-MB-231 cells. d MTS growth inhibition assay in a panel of PTEN-proficient and—deficient human BC cells treated with VE-821. e γH2AX accumulation by FACS in BC cells treated with VE821
VE-821 (ATR inhibitor) is selectively toxic in PTEN deficient TNBC cells
Given the current pharmaceutical interest in the development of ATR inhibitors for cancer therapy, we pre-clinically tested whether ATR inhibition could be selectively toxic in PTEN-deficient cells. VE-821 is a highly selective ATR kinase inhibitor with an IC50 of 26 nM in cell-free assays for ATR inhibition. In MTS cell proliferation assays, we observed that VE-821 was more toxic to BT-549 and MDA-MB-468 compared to MDA-MB-231 cells (Fig. 2d).
Phosphorylated H2AX (γH2AX) is a marker of double-strand breaks. As expected, there was substantial γH2AX accumulation [thereby suggesting double-strand break (DSBs) accumulation] in BT-549 and MDA-MB-468 cells compared to MDA-MB-231 cells after 24 h of VE-821 treatment (Fig. 2E1, E2). The accumulation of DSBs was associated with S-phase arrest in BT-549 cells and G2/M arrest in MDA-MB-468 cells after 48 h of VE-821 treatment (Figs. 3A1, 3A2). Cell cycle arrest was subsequently followed by accumulation of apoptotic cells (Figs. 3B1, 2B2).
Taken together, the data provides evidence that VE-821 induces synthetic lethality in PTEN-deficient cells through accumulation of DSBs, cell cycle arrest and induction of apoptosis.
Discussion
We provide the first clinical evidence that ATR signaling could have adverse impact on survival in PTEN-deficient breast cancers. In addition, the pre-clinical evidence presented here also suggests that ATR inhibition could be a promising synthetic lethality strategy in PTEN-deficient breast cancers.
Loss of not only cytoplasmic PTEN expression but also nuclear PTEN expression was associated with aggressive ER−, PR− and HER2− phenotypes. Our data concurs with previous studies that correlate PTEN loss with TNBCs [6, 8, 16]. In addition, the negative PTEN expression status either in cytoplasm or nucleus resulted in negative expression of nuclear or cytoplasmic pCHK1ser345. The data are consistent with a previous study showing that the loss of PTEN-impaired Chk1 through phosphorylation mediated by elevated AKT and subsequent Chk1 ubiquitination [18]. Puc et al. also demonstrated that PTEN loss reduces Chk1 nuclear localization, thereby increasing the genomic instability and promoting tumorigenesis [18]. Supporting these observations, our study demonstrated that cytoplasmic/nuclear PTEN loss resulted in significantly increasing tumour size, mitotic index and NPI.
Whereas cytoplasmic PTEN serves as a negative regulator of PI3K/AKT signaling, nuclear PTEN has been shown to have roles in DNA repair [5, 7, 14, 22]. For example, PTEN loss has been shown to trigger downregulation of both RAD51 [15, 23] and BRCA1 [17]. Accordingly, we observed that DNA repair profiling in PTEN-deficient cells, altered expression of several genes involved multiple DNA repair pathways including BER, NHEJ, HR, NER and MMR. The data suggest that PTEN may be directly or indirectly involved in the regulation of multiple DNA repair genes.
Pharmaceutical development of ATR inhibitors for cancer therapy is an attractive anti-cancer strategy [9, 10]. Pre-clinically, we observed that PTEN deficient breast cancer cells were sensitive to ATR inhibition and was associated with accumulation of DSBs, cell cycle arrest and induction of apoptosis. The data imply that PTEN-deficient cells with impaired DNA repair may be reliant upon ATR signaling pathway for survival. ATR blockade in this context could lead to synthetic lethality. Recently, ATM inhibition was also shown to be synthetically lethal in PTEN-deficient cells [12]. Interestingly, ATM-deficient cells are also sensitive to ATR inhibitors via synthetic lethality in leukemic cells [11].
In conclusion, we have demonstrated that ATR signaling adversely impact upon survival in PTEN-deficient breast cancers. ATR targeting could be a promising synthetic lethality approach in PTEN-deficient breast cancers.
References
Abdel-Fatah TM et al (2015) Untangling the ATR-CHEK1 network for prognostication, prediction and therapeutic target validation in breast cancer. Mol Oncol 9:569–585. https://doi.org/10.1016/j.molonc.2014.10.013
Abdel-Fatah TM et al (2014) DNA polymerase beta deficiency is linked to aggressive breast cancer: a comprehensive analysis of gene copy number, mRNA and protein expression in multiple cohorts. Mol Oncol 8:520–532. https://doi.org/10.1016/j.molonc.2014.01.001
Albarakati N et al (2015) Targeting BRCA1-BER deficient breast cancer by ATM or DNA-PKcs blockade either alone or in combination with cisplatin for personalized therapy. Mol Oncol 9:204–217. https://doi.org/10.1016/j.molonc.2014.08.001
Arora A et al (2015) Transcriptomic and protein expression analysis reveals clinicopathological significance of bloom syndrome helicase (BLM) in breast cancer. Mol Cancer Ther 14:1057–1065. https://doi.org/10.1158/1535-7163.MCT-14-0939
Bassi C et al (2013) Nuclear PTEN controls DNA repair and sensitivity to genotoxic stress. Science 341:395–399. https://doi.org/10.1126/science.1236188
Bose S et al (2002) Reduced expression of PTEN correlates with breast cancer progression. Hum Pathol 33:405–409
Chalhoub N, Baker SJ (2009) PTEN and the PI3-kinase pathway in cancer. Annu Rev Pathol 4:127–150. https://doi.org/10.1146/annurev.pathol.4.110807.092311
Depowski PL et al (2001) Loss of expression of the PTEN gene protein product is associated with poor outcome in breast cancer. Mod Pathol 14:672–676. https://doi.org/10.1038/modpathol.3880371
Fokas E et al (2014) Targeting ATR in DNA damage response and cancer therapeutics. Cancer Treat Rev 40:109–117. https://doi.org/10.1016/j.ctrv.2013.03.002
Karnitz LM, Zou L (2015) Molecular Pathways: targeting ATR in Cancer Therapy. Clin Cancer Res 21:4780–4785. https://doi.org/10.1158/1078-0432.CCR-15-0479
Kwok M et al (2016) ATR inhibition induces synthetic lethality and overcomes chemoresistance in TP53- or ATM-defective chronic lymphocytic leukemia cells. Blood 127:582–595. https://doi.org/10.1182/blood-2015-05-644872
McCabe N et al (2015) Mechanistic rationale to target PTEN-deficient tumor cells with inhibitors of the DNA damage response kinase ATM. Cancer Res 75:2159–2165. https://doi.org/10.1158/0008-5472.CAN-14-3502
McShane LM et al (2005) Reporting recommendations for tumor marker prognostic studies (REMARK). J Natl Cancer Inst 97:1180–1184. https://doi.org/10.1093/jnci/dji237
Ming M, He YY (2012) PTEN in DNA damage repair. Cancer Lett 319:125–129. https://doi.org/10.1016/j.canlet.2012.01.003
Mukherjee A, Karmakar P (2013) Attenuation of PTEN perturbs genomic stability via activation of Akt and down-regulation of Rad51 in human embryonic kidney cells. Mol Carcinog 52:611–618. https://doi.org/10.1002/mc.21903
Perren A et al (1999) Immunohistochemical evidence of loss of PTEN expression in primary ductal adenocarcinomas of the breast. Am J Pathol 155:1253–1260. https://doi.org/10.1016/S0002-9440(10)65227-3
Phuah SY et al (2012) Triple-negative breast cancer and PTEN (phosphatase and tensin homologue) loss are predictors of BRCA1 germline mutations in women with early-onset and familial breast cancer, but not in women with isolated late-onset breast cancer. Breast Cancer Res 14:R142. https://doi.org/10.1186/bcr3347
Puc J et al (2005) Lack of PTEN sequesters CHK1 and initiates genetic instability. Cancer Cell 7:193–204. https://doi.org/10.1016/j.ccr.2005.01.009
Saldivar JC et al (2017) The essential kinase ATR: ensuring faithful duplication of a challenging genome. Nat Rev Mol Cell Biol 18:622–636. https://doi.org/10.1038/nrm.2017.67
Smits VA et al (2010) Mechanisms of ATR-mediated checkpoint signalling. Front Biosci 15:840–853
Sultana R et al (2013) Targeting XRCC1 deficiency in breast cancer for personalized therapy. Cancer Res 73:1621–1634. https://doi.org/10.1158/0008-5472.CAN-12-2929
Worby CA, Dixon JE (2014) Pten. Annu Rev Biochem 83:641–669. https://doi.org/10.1146/annurev-biochem-082411-113907
Zhao Q et al (2017) Inhibition of Rad51 sensitizes breast cancer cells with wild-type PTEN to olaparib. Biomed Pharmacother 94:165–168. https://doi.org/10.1016/j.biopha.2017.07.090
Acknowledgements
A part of this work was supported by Breast Cancer Now (Grant Number: 2015MaySP537).
Author information
Authors and Affiliations
Corresponding authors
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Al-Subhi, N., Ali, R., Abdel-Fatah, T. et al. Targeting ataxia telangiectasia-mutated- and Rad3-related kinase (ATR) in PTEN-deficient breast cancers for personalized therapy. Breast Cancer Res Treat 169, 277–286 (2018). https://doi.org/10.1007/s10549-018-4683-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10549-018-4683-4