Abstract
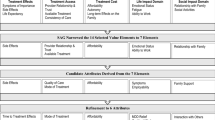
We developed three methods (rating, ranking, and discrete choice) for identifying patients’ preferred depression treatments based on their prioritization of specific treatment attributes (e.g., medication side effects, psychotherapy characteristics) at treatment intake. Community mental health patients with depressive symptoms participated in separate studies of predictive validity (N = 193) and short-term (1-week) stability (N = 40). Patients who received non-preferred initial treatments (based on the choice method) switched treatments significantly more often than those who received preferred initial treatments. Receiving a non-preferred treatment at any point (based on rating and choice methods) was a significant predictor of longer treatment duration. All three methods demonstrated good short-term stability.
Similar content being viewed by others
References
American Psychiatric Association. (1994). Diagnostic and statistical manual of mental disorders: DSM- IV (4th ed.). Washington: American Psychiatric Association.
APA Presidential Task Force on Evidence-Based Practice. (2006). Evidence-based practice in psychology. American Psychologist, 61(4), 271–285.
Brodie, M. J., & Kwan, P. (2001). The star systems: Overview and use in determining antiepileptic drug choice. CNS Drugs, 15(1), 1–12. doi:10.2165/00023210-200115010-00001.
Chilvers, C., Dewey, M., Fielding, K., Gretton, V., Miller, P., Palmer, B., & Harrison, G. (2001). Antidepressant drugs and generic counselling for treatment of major depression in primary care: Randomised trial with patient preference arms. BMJ, 322(7289), 772–775. doi:10.1136/bmj.322.7289.772.
Citrome, L., & Ketter, T. A. (2013). When does a difference make a difference? Interpretation of number needed to treat, number needed to harm, and likelihood to be helped or harmed. International Journal of Clinical Practice, 67, 407–411.
Clever, S. L., Ford, D. E., Rubenstein, L. V., Rost, K. M., Meredith, L. S., Sherbourne, C. D., & Cooper, L. A. (2006). Primary care patients’ involvement in decision-making is associated with improvement in depression. Medical Care, 44(5), 398–405. doi:10.1097/01.mlr.0000208117.15531.da.
Cohen, E. (2009). Applying best-worst scaling to wine marketing. International Journal of Wine Business Research, 21(1), 8–23. doi:10.1108/17511060910948008.
Dolan, J. G. (1989). Medical decision making using the analytic hierarchy process: Choice of initial antimicrobial therapy for acute pyelonephritis. Medical Decision Making, 9(1), 51–56. doi:10.1177/0272989X8900900109.
Dolan, J. G., & Bordley, D. R. (1994). Isoniazid prophylaxis: The importance of individual values. Medical Decision Making, 14(1), 1–8. doi:10.1177/0272989X9401400101.
Dolan, J. G., & Frisina, S. (2002). Randomized controlled trial of a patient decision aid for colorectal cancer screening. Medical Decision Making, 22(2), 125–139. doi:10.1177/02729890222063017.
Dwight-Johnson, M., Unutzer, J., Sherbourne, C., Tang, L., & Wells, K. B. (2001). Can quality improvement programs for depression in primary care address patient preferences for treatment? Medical Care, 39(9), 934–944. doi:10.1097/00005650-200109000-00004.
Ferguson, J. M. (2001). SSRI antidepressant medications: Adverse effects and tolerability. Primary Care Companion Journal of Clinical Psychiatry, 3(1), 22–27.
Finn, A., & Louviere, J. J. (1992). Determining the appropriate response to evidence of public concern: The case of food safety. Journal of Public Policy and Marketing, 11(2), 12–25.
Flynn, T. N., Louviere, J. J., Peters, T. J., & Coast, J. (2007). Best-worst scaling: What it can do for health care research and how to do it. Journal of Health Economics, 26(1), 171–189. doi:10.1016/j.jhealeco.2006.04.002.
Flynn, T. N., Louviere, J. J., Peters, T. J., & Coast, J. (2008). Estimating preferences for a dermatology consultation using best-worst scaling: Comparison of various methods of analysis. BMC Medical Research Methodology, 8(1), 76. doi:10.1186/1471-2288-8-76.
Gartlehner, G., Hansen, R. A., Morgan, L. C., Thaler, K., Lux, L., Van Noord, M., & Lohr, K. N. (2011). Comparative benefits and harms of second-generation antidepressants for treating major depressive disorder: An updated meta-analysis. Annals of Internal Medicine, 155, 772–785.
Gitlin, M. (2003). Sexual dysfunction with psychotropic drugs. Expert Opinion on Pharmacotherapy, 4, 2259–2269.
Goadsby, P. J., Dodick, D. W., Ferrari, M. D., McCrory, D. C., & Williams, P. (2004). TRIPSTAR: Prioritizing oral triptan treatment attributes in migraine management. Acta Neurologica Scandinavica, 110(3), 137–143. doi:10.1111/j.1600-0404.2004.00310.x.
Guyatt, G., Cairns, J., Churchill, D., Cook, D., Haynes, B., Hirsh, J., & Tugwell, P. (1992). Evidence-based medicine: A new approach to teaching the practice of medicine. JAMA, 268(17), 2420–2425. doi:10.1001/jama.1992.03490170092032.
Hamilton, M. (1960). A rating scale for depression. Journal of Neurology, Neurosurgery and Psychiatry, 23(1), 56–62. doi:10.1136/jnnp.23.1.56.
Hummel, M. J. M., Volz, F., van Manen, J. G., Danner, M., Dintsios, C. M., Ijzerman, M. J., & Gerber, A. (2012). Using the analytic hierarchy process to elicit patient preferences: Prioritizing multiple outcome measures of antidepressant drug treatment. Patient, 5(4), 225–237. doi:10.2165/11635240-000000000-00000.
Iacoviello, B. M., McCarthy, K. S., Barrett, M. S., Rynn, M., Gallop, R., & Barber, J. P. (2007). Treatment preferences affect the therapeutic alliance: Implications for randomized controlled trials. Journal of Consulting and Clinical Psychology, 75(1), 194–198. doi:10.1037/0022-006X.75.1.194.
Institute of Medicine. (2001). Crossing the quality chasm: A new health system for the 21st century. Washington: National Academy Press.
Intercontinental Medical Systems. (2004). National disease and therapeutic index. Plymouth Meeting: IMS Health.
Keating, N. L., Guadagnoli, E., Landrum, M. B., Borbas, C., & Weeks, J. C. (2002). Treatment decision making in early-stage breast cancer: Should surgeons match patients’ desired level of involvement? Journal of Clinical Oncology, 20(6), 1473–1479. doi:10.1200/JCO.20.6.1473.
Kocher, M. S., Bishop, J., Marshall, R., Briggs, K. K., & Hawkins, R. J. (2002). Operative versus nonoperative management of acute achilles tendon rupture: Expected-value decision analysis. American Journal of Sports Medicine, 30(6), 783–790. doi:10.1177/03635465020300060501.
Lin, P., Campbell, D. G., Chaney, E. F., Liu, C. F., Heagerty, P., Felker, B. L., & Hedrick, S. C. (2005). The influence of patient preference on depression treatment in primary care. Annals of Behavioral Medicine, 30(2), 164–173. doi:10.1207/s15324796abm3002_9.
Louviere, J. J., Flynn, T. N., & Marley, A. A. J. (2015). Best-worst scaling: Theory, methods and applications. Cambridge: Cambridge University Press.
Marley, A. A. J., Flynn, T. N., & Louviere, J. J. (2008). Probabilistic models of set-dependent and attribute-level best-worst choice. Journal of Mathematical Psychology, 52(5), 281–296. doi:10.1016/j.jmp.2008.02.002.
Marley, A. A. J., & Louviere, J. J. (2005). Some probabilistic models of best, worst, and best–worst choices. Journal of Mathematical Psychology, 49(6), 464–480. doi:10.1016/j.jmp.2005.05.003.
Montejo, A. L., Llorca, G., Izquierdo, J. A., Rico-Villademoros, F., & and the Spanish Working Group for the Study of Psychotropic Related Sexual Dysfunction. (2001). Incidence of sexual dysfunction associated with antidepressant agents. A prospective multicenter study of 1022 outpatients. Journal of Clinical Psychiatry, 62(supplement 3), 10–21.
Pagel, J. F., & Parnes, B. L. (2001). Medications for the treatment of sleep disorders. Primary Care Companion Journal of Clinical Psychiatry, 3, 125–188.
Riche, N., Duvinage, M., Mancas, M., Gosselin, B., & Dutoit, T. (2013). A study of parameters affecting visual saliency assessment. Proceedings of the 6 th International Symposium on Attention in Cognitive Systems. (ISACS’13),). Beijing, China, August 3–5. http://arxiv.org/abs/1307.5691v1.
Rush, A. J., Trivedi, M. H., Ibrahim, H. M., Carmody, T. J., Arnow, B., Klein, D. N., & Keller, M. B. (2003). The 16-item Quick Inventory Of Depressive Symptomatology (QIDS), clinician rating (QIDS-C), and self-report (QIDS-SR): A psychometric evaluation in patients with chronic major depression. Biological Psychiatry, 54(5), 573–583. doi:10.1016/S0006-3223(02)01866-8.
Sackett, D. L. (2000). Evidence-based medicine. New York: Wiley.
Schumacher, G. E. (1991). Multiattribute evaluation in formulary decision making as applied to calcium-channel blockers. American Journal of Hospital Pharmacy, 48(2), 301–308.
Schweitzer, I., Mcguire, K., & Chee, N. (2009). Sexual side-effects of contemporary antidepressants: Review. Australian and New Zealand Journal of Psychiatry, 43, 795–808.
Serritti, A., & Chiesa, A. (2011). A meta-analysis of sexual dysfunction in psychiatric patients taking antipsychotics. International Clinical Psychopharmacology, 26, 130–140.
van Schaik, D. J., Klijn, A. F., van Hout, H. P., van Marwijk, H. W., Beekman, A. T., de Haan, M., & van Dyck, R. (2004). Patients’ preferences in the treatment of depressive disorder in primary care. General Hospital Psychiatry, 26(3), 184–189. doi:10.1016/j.genhosppsych.2003.12.001.
Watanabe, N., Omori, I. O., Nakagawa, A., Cipriani, A., Barbui, C., McGuire, H., et al. (2010). Safety reporting and adverse-event profile of mirtazapine described in randomized controlled trials in comparison with other classes of antidepressants in the acute-phase treatment of adults with depression: Systematic review and meta-analysis. CNS Drugs, 24(1), 35–53.
Wittink, M. N., Cary, M., TenHave, T., Baron, J., & Gallo, J. J. (2010). Towards patient-centered care for depression. The Patient: Patient-Centered Outcomes Research, 3(3), 145–157. doi:10.2165/11530660-000000000-00000.
Wittink, M. N., Morales, K. H., Cary, M., Gallo, J. J., & Bartels, S. J. (2013). Towards personalizing treatment for depression: developing treatment values markers. The Patient: Patient-Centered Outcomes Research, 6(1), 35–43. doi:10.1007/s40271-013-0003-6.
Yoon, K., & Hwang, C.-L. (1995). Multiple attribute decision making. Thousand Oaks: SAGE Publications Inc.
Zimmermann, T. M., Clouth, J., Elosge, M., Heurich, M., Schneider, E., Wilhelm, S., & Wolfrath, A. (2013). Patient preferences for outcomes of depression treatment in Germany: A choice-based conjoint analysis study. Journal of Affective Disorder, 148(2–3), 210–219. doi:10.1016/j.jad.2012.11.062.
Funding
This research was funded by National Institute of Mental Health Grant R34-MH085817. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health or the University of Pennsylvania.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors report no conflicts of interest.
Ethical Approval
This research was reviewed and approved by the University of Pennsylvania IRB and City of Philadelphia IRB. All procedures involving human participants were in accordance with the ethical standards of the IRB, the 1964 Declaration of Helsinki, and its later amendments.
Informed Consent
Informed consent was obtained from all individual participants included in the study in accordance with HIPAA standards.
Rights and permissions
About this article
Cite this article
Crits-Christoph, P., Gallop, R., Diehl, C.K. et al. Methods for Incorporating Patient Preferences for Treatments of Depression in Community Mental Health Settings. Adm Policy Ment Health 44, 735–746 (2017). https://doi.org/10.1007/s10488-016-0746-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10488-016-0746-1