Abstract
Purpose
To evaluate the long-term safety and effectiveness of the Preserflo MicroShunt in Japanese primary open-angle glaucoma (POAG) patients.
Study design
Single-site, nonrandomized observational study.
Patients and methods
Eight eyes of 7 POAG patients were included. The surgical complications and interventions were monitored. The preoperative and postoperative intraocular pressures (IOPs), numbers of antiglaucoma medications, logarithm of the minimum angle of resolution visual acuity (VA), mean deviation (MD) slope, and corneal endothelial cell density (CECD) were compared retrospectively.
Results
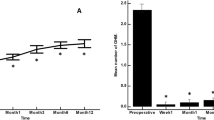
The mean follow-up period was 68.9 months (range, 48–76 months). The baseline IOP of 17.9 ± 3.5 mmHg and the number of glaucoma medications of 3.5 ± 0.5 were significantly reduced at subsequent follow-up visits. At 1, 2, 3, 4, 5, and 6 years postoperatively, the IOPs were 13.8 ± 2.9, 12.8 ± 2.3, 12.1 ± 3.2, 12.6 ± 2.5, 12.3 ± 1.0, and 13.5 ± 3.1 mmHg, respectively, with the use of 1.6 ± 1.4, 1.6 ± 1.6, 1.5 ± 1.4, 1.5 ± 1.4, 1.9 ± 1.3, and 2.0 ± 1.1 medications. Postoperative transient hyphema occurred in 1 eye. Postoperative needling was required in 5 eyes, 12 times in total. No eyes showed significant VA decline, except for 1 eye with a severe central visual field defect that existed preoperatively. The preoperative MD slope of − 1.6 ± 1.2 dB/year improved significantly, to − 0.3 ± 0.2 dB/year (P = 0.023), postoperatively. The baseline CECD decreased from 2595 ± 292 to 2478.4 ± 255 postoperatively.
Conclusion
The microshunt surgical procedure is safe and effective for Japanese POAG patients.



Similar content being viewed by others
References
Group CN-TGS. Comparison of glaucomatous progression between untreated patients with normal-tension glaucoma and patients with therapeutically reduced intraocular pressures. Am J Ophthalmol. 1998;126:487–97.
A Investigators. The advanced glaucoma intervention study (AGIS): 7 the relationship between control of intraocular pressure and visual field deterioration. Am J Ophthalmol. 2000;130:429–40.
Garway-Heath DF, Crabb DP, Bunce C, Lascaratos G, Amalfitano F, Anand N, et al. Latanoprost for open-angle glaucoma (UKGTS): a randomised, multicentre, placebo-controlled trial. Lancet. 2015;385:1295–304.
Kashiwagi K, Kogure S, Mabuchi F, Chiba T, Yamamoto T, Kuwayama Y, et al. Change in visual acuity and associated risk factors after trabeculectomy with adjunctive mitomycin C. Acta Ophthalmol (Copenh). 2016;94:e561–70.
Kirwan JF, Lockwood AJ, Shah P, Macleod A, Broadway DC, Kinget AJ, et al. Trabeculectomy in the 21st century: a multicenter analysis. Ophthalmology. 2013;120:2532–9.
Razeghinejad MR, Havens SJ, Katz LJ. Trabeculectomy bleb-associated infections. Surv Ophthalmol. 2017;62:591–610.
Gedde SJ, Herndon LW, Brandt JD, Budenz DL, Feuer WJ, Schiffman JC, et al. Postoperative complications in the tube versus trabeculectomy (TVT) study during five years of follow-up. Am J Ophthalmol. 2012;153:804–14.
Saheb H, Ahmed IIK. Micro-invasive glaucoma surgery: current perspectives and future directions. Curr Opin Ophthalmol. 2012;23:96–104.
Ittoop SM, Kahook MY, Seibold LK. Trabecular meshwork bypasses. In: Kahook MY, editor. MIGS: advances in glaucoma surgery. West Deptford: Slack Incorporated; 2014. p. 27–55.
Beckers HJ, Kinders KC, Webers CA. Five-year results of trabeculectomy with mitomycin C. Graefes Arch Clin Exp Ophthalmol. 2003;241:106–10.
Batlle JF, Fantes F, Riss I, Pinchuk L, Alburquerque R, Kato YP, et al. Three-year follow-up of a novel aqueous humor microshunt. J Glaucoma. 2016;25:e58-65.
Pinchuk L, Wilson GJ, Barry JJ, Schoephoerster RT, Parel J-M, Kennedy JP. Medical applications of poly (styrene-block-isobutylene-block-styrene)(“SIBS”). Biomaterials. 2008;29:448–60.
Acosta AC, Espana EM, Yamamoto H, Davis S, Pinchuk L, Weber BA, et al. A newly designed glaucoma drainage implant made of poly (styrene-b-isobutylene-b-styrene): biocompatibility and function in normal rabbit eyes. Arch Ophthalmol. 2006;124:1742–9.
Pinchuk L, Riss I, Batlle JF, Kato YP, Martin JB, Arrieta E, et al. The development of a micro-shunt made from poly (styrene-block-isobutylene-block-styrene) to treat glaucoma. J Biomed Mater Res B Appl Biomater. 2017;105:211–21.
Schlenker MB, Durr GM, Michaelov E, Ahmed IIK. Intermediate outcomes of a novel standalone ab externo SIBS Microshunt with mitomycin C. Am J Ophthalmol. 2020;215:141–53.
Honjo M, Sakata R, Fujishiro T, Shirato S, Aihara M. One-year postoperative outcomes of filtration minimally invasive glaucoma surgery using the PRESERFLOⓇ MicroShunt for primary open angle glaucoma in Japanese patients. Nippon Ganka Gakkai Zasshi. 2020;124:705–12 (in Japanese).
Batlle JF, Corona A, Albuquerque R. Long-term results of the PRESERFLO MicroShunt in patients with primary open-angle glaucoma from a single-center nonrandomized study. J Glaucoma. 2021;30:281–6.
Rao HL, Addepalli UK, Jonnadula GB, Kumbar T, Senthil S, Garudadri CS. Relationship between intraocular pressure and rate of visual field progression in treated glaucoma. J Glaucoma. 2013;22:719–24.
Sakata R, Yoshitomi T, Iwase A, Matsumoto C, Higashide T, Shirakashi M, et al. Factors associated with progression of Japanese open-angle glaucoma with lower normal intraocular pressure. Ophthalmology. 2019;126:1107–16.
Fujita A, Sakata R, Ueda K, Nakajima K, Fujishiro T, Honjo M, et al. Evaluation of fornix-based trabeculectomy outcomes in Japanese glaucoma patients based on concrete long-term preoperative data. Jpn J Ophthalmol. 2021;65:306–12.
Costa VP, Spaeth GL, Eiferman RA, Orengo-Nania S. Wound healing modulation in glaucoma filtration surgery. Ophthalmic Surg Lasers Imaging Retina. 1993;24:152–70.
Costa VP, Moster MR, Wilson RP, Schmidt CM, Gandham S, Smith M. Effects of topical mitomycin C on primary trabeculectomies and combined procedures. Br J Ophthalmol. 1993;77:693–7.
Seol BR, Lee SY, Kim YJ, Kim YK, Jeoung JW, Park KH. Comparison of the efficacy and safety of trabeculectomy with mitomycin C according to concentration: a prospective randomized clinical trial. J Clin Med. 2021;10:59.
Lenzhofer M, Kersten-Gomez I, Sheybani A, Gulamhusein H, Strohmaier C, Hohensinn M, et al. Four-year results of a minimally invasive transscleral glaucoma gel stent implantation in a prospective multi-centre study. Clin Experiment Ophthalmol. 2019;47:581–7.
Schargus M, Busch C, Rehak M, Meng J, Schmidt M, Bormann C, et al. Functional monitoring after trabeculectomy or XEN Microstent implantation using spectral domain optical coherence tomography and visual field indices: a retrospective comparative cohort study. Biology (Basel). 2021;10:273.
Acknowledgements
This work was supported by the Japan Society for the Promotion of Science (JSPS), grant number 19K09965 (to M.H.) and Kakenhi grant number 20H03839 (to M.A.). The sponsor or funding organization had no role in the design of this research nor in how the research was conducted. The Preserflo MicroShunt was provided without financial compensation by InnFocus MicroShunt (Santen).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
T. Ahmed, None; M. Honjo, None; R. Sakata, None; T. Fujishiro, None; S. Shirato, None; M. Aihara, None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Corresponding Author: Makoto Aihara
About this article
Cite this article
Ahmed, T., Honjo, M., Sakata, R. et al. Long-term results of the safety and effectiveness of a novel microshunt in Japanese patients with primary open-angle glaucoma. Jpn J Ophthalmol 66, 33–40 (2022). https://doi.org/10.1007/s10384-021-00893-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-021-00893-x