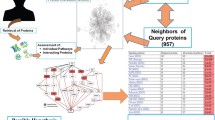
Abstract
Dementia is one of the diabetic complications under intensive study. Alteration of synaptic adhesion protein (SAP) associates with neurological diseases, including Alzheimer’s disease. However, the regulation of SAPs in the brain of diabetes mellitus remains elusive. To pinpoint the candidate SAPs underlining the mechanism of diabetic dementia, we investigated expression profiling of SAPs in both streptozotocin (STZ)-induced diabetic mice, AppNL-G-F/NL-G-F mice, and amyloid precursor protein intracellular domain (AICD)-induced human neural cell line from public databases. DST (Dystonin/BPAG1) was identified upregulated in both models. Our finding suggests that DST alteration may involve in the mechanism of diabetic dementia.




Similar content being viewed by others
Abbreviations
- SAP:
-
Synaptic adhesion protein
- STZ:
-
Streptozotocin
- AICD:
-
Amyloid precursor protein intracellular domain
- AD:
-
Alzheimer’s disease
- BP:
-
Bullous pemphigoid
References
Biessels GJ, Staekenborg S, Brunner E, Brayne C, Scheltens P (2006) Risk of dementia in diabetes mellitus: a systematic review. Lancet Neurol 5(1):64–74
Chen S-Y, Hsu YM, Lin YJ, Huang YC, Chen CJ, Lin WD, Liao WL, Chen YT, Lin WY, Liu YH, Yang JS, Sheu JC, Tsai FJ (2016) Current concepts regarding developmental mechanisms in diabetic retinopathy in Taiwan. Biomedicine 6(2):7
Ahtiluoto S, Polvikoski T, Peltonen M, Solomon A, Tuomilehto J, Winblad B, Sulkava R, Kivipelto M (2010) Diabetes, Alzheimer disease, and vascular dementia: a population-based neuropathologic study. Neurology 75(13):1195–1202
Matsuzaki T, Sasaki K, Tanizaki Y, Hata J, Fujimi K, Matsui Y, Sekita A, Suzuki SO, Kanba S, Kiyohara Y, Iwaki T (2010) Insulin resistance is associated with the pathology of Alzheimer disease The Hisayama Study. Neurology 75(9):764–770
Vagelatos NT, Eslick GD (2013) Type 2 diabetes as a risk factor for Alzheimer’s disease: the confounders, interactions, and neuropathology associated with this relationship. Epidemiol Rev 35(1):152–160
Abner EL, Nelson PT, Kryscio RJ, Schmitt FA, Fardo DW, Woltjer RL, Cairns NJ, Yu L, Dodge HH, Xiong C, Masaki K, Tyas SL, Bennett DA, Schneider JA, Arvanitakis Z (2016) Diabetes is associated with cerebrovascular but not Alzheimer’s disease neuropathology. Alzheimers Dement 12(8):882–889
Hachinski V (2019) Dementia: new vistas and opportunities. Neurol Sci
Leshchyns’ka I, Liew HT, Shepherd C, Halliday GM, Stevens CH, Ke YD, Ittner LM, Sytnyk V (2015) Aβ-dependent reduction of NCAM2-mediated synaptic adhesion contributes to synapse loss in Alzheimer’s disease. Nat Commun 6:8836
Brose N (1999) Synaptic cell adhesion proteins and synaptogenesis in the mammalian central nervous system. Naturwissenschaften 86(11):516–524
Yamagata M, Sanes JR, Weiner JA (2003) Synaptic adhesion molecules. Curr Opin Cell Biol 15(5):621–632
Missler M, Südhof TC, Biederer T (2012) Synaptic cell adhesion. Cold Spring Harb Perspect Biol 4:a005694
Rolf B, Kutsche M, Bartsch U (2001) Severe hydrocephalus in L1-deficient mice. Brain Res 891(1–2):247–252
Montag-Sallaz M, Schachner M, Montag D (2002) Misguided axonal projections, neural cell adhesion molecule 180 mRNA upregulation, and altered behavior in mice deficient for the close homolog of L1. Mol Cell Biol 22(22):7967–7981
Wyss L, Schäfer J, Liebner S, Mittelbronn M, Deutsch U, Enzmann G, Adams RH, Aurrand-Lions M, Plate KH, Imhof BA, Engelhardt B (2012) Junctional adhesion molecule (JAM)-C deficient C57BL/6 mice develop a severe hydrocephalus. PLoS One 7(9):e45619
Tucci V, Kleefstra T, Hardy A, Heise I, Maggi S, Willemsen MH, Hilton H, Esapa C, Simon M, Buenavista MT, McGuffin LJ, Vizor L, Dodero L, Tsaftaris S, Romero R, Nillesen WN, Vissers LELM, Kempers MJ, Vulto-van Silfhout AT, Iqbal Z, Orlando M, Maccione A, Lassi G, Farisello P, Contestabile A, Tinarelli F, Nieus T, Raimondi A, Greco B, Cantatore D, Gasparini L, Berdondini L, Bifone A, Gozzi A, Wells S, Nolan PM (2014) Dominant β-catenin mutations cause intellectual disability with recognizable syndromic features. J Clin Invest 124(4):1468–1482
Moon Y, Choi YJ, Kim JO, Han SH (2018) Muscle profile and cognition in patients with Alzheimer’s disease dementia. Neurol Sci 39(11):1861–1866
Cheng J, Liu HP, Lee CC, Chen MY, Lin WY, Tsai FJ (2018) Matrix metalloproteinase 14 modulates diabetes and Alzheimer’s disease cross-talk: a meta-analysis. Neurol Sci 39(2):267–274
Zhang W et al (2006) SynDB: a synapse protein DataBase based on synapse ontology. Nucleic Acids Res 35(suppl_1):D737–D741
Huang DW, Sherman BT, Lempicki RA (2008) Systematic and integrative analysis of large gene lists using DAVID bioinformatics resources. Nat Protoc 4(1):44
Suzuki R, Lee K, Jing E, Biddinger SB, McDonald JG, Montine TJ, Craft S, Kahn CR (2010) Diabetes and insulin in regulation of brain cholesterol metabolism. Cell Metab 12(6):567–579
Castillo E, Leon J, Mazzei G, Abolhassani N, Haruyama N, Saito T, Saido T, Hokama M, Iwaki T, Ohara T, Ninomiya T, Kiyohara Y, Sakumi K, LaFerla FM, Nakabeppu Y (2017) Comparative profiling of cortical gene expression in Alzheimer’s disease patients and mouse models demonstrates a link between amyloidosis and neuroinflammation. Sci Rep 7(1):17762
Müller T, Concannon CG, Ward MW, Walsh CM, Tirniceriu AL, Tribl F, Kögel D, Prehn JHM, Egensperger R (2007) Modulation of gene expression and cytoskeletal dynamics by the amyloid precursor protein intracellular domain (AICD). Mol Biol Cell 18(1):201–210
Suckow AT (2010) The role of synaptogenic synaptic adhesion molecules in insulin secretion. UC San Diego
Franklin IK, Wollheim CB (2004) GABA in the endocrine pancreas: its putative role as an islet cell paracrine-signalling molecule. J Gen Physiol 123(3):185–190
Suckow AT, Comoletti D, Waldrop MA, Mosedale M, Egodage S, Taylor P, Chessler SD (2008) Expression of neurexin, neuroligin, and their cytoplasmic binding partners in the pancreatic β-cells and the involvement of neuroligin in insulin secretion. Endocrinology 149(12):6006–6017
Ferrier A, Boyer JG, Kothary R (2013, Elsevier) Cellular and molecular biology of neuronal dystonin, in International review of cell and molecular biology. Int Rev Cell Mol Biol 300:85–120
Lynch-Godrei A, Kothary R (2016, Elsevier) Functional and genetic analysis of neuronal isoforms of BPAG1. Methods Enzymol 569:355–372
Di Zenzo G et al (2012) Bullous pemphigoid: from the clinic to the bench. Clin Dermatol 30(1):3–16
Foureur N et al (2001) Bullous pemphigoid in a leg affected with hemiparesia: a possible relation of neurological diseases with bullous pemphigoid? Eur J Dermatol 11(3):230–233
Brick KE, Weaver CH, Savica R, Lohse CM, Pittelkow MR, Boeve BF, Gibson LE, Camilleri MJ, Wieland CN (2014) A population-based study of the association between bullous pemphigoid and neurologic disorders. J Am Acad Dermatol 71(6):1191–1197
Tarazona MJM, Mota ANCM, Gripp AC, Unterstell N, Bressan AL (2015) Bullous pemphigoid and neurological disease: statistics from a dermatology service. An Bras Dermatol 90(2):280–282
Chuang T-Y, Korkij W, Soltani K, Clayman J, Cook J (1984) Increased frequency of diabetes mellitus in patients with bullous pemphigoid: a case-control study. J Am Acad Dermatol 11(6):1099–1102
Pasmatzi E, Monastirli A, Habeos J, Georgiou S, Tsambaos D (2011) Dipeptidyl peptidase-4 inhibitors cause bullous pemphigoid in diabetic patients: report of two cases. Diabetes Care 34(8):e133–e133
Skandalis K, Spirova M, Gaitanis G, Tsartsarakis A, Bassukas ID (2012) Drug-induced bullous pemphigoid in diabetes mellitus patients receiving dipeptidyl peptidase-IV inhibitors plus metformin. J Eur Acad Dermatol Venereol 26(2):249–253
Geller S, Kremer N, Zeeli T, Sprecher E (2018) Bullous pemphigoid and diabetes mellitus: are we missing the larger picture. J Am Acad Dermatol 79(2):e27
Funding
This work was supported by grants from the Ministry of Science and Technology in Taiwan (MOST 106-2320-B-039-023, MOST 107-2314-B-039 -042 -MY2, MOST 104-2320-B-039-009, MOST 105-2632-B-039-002, MOST 106-2632-B-039-001) and grants from China Medical University and Hospital (CMU107-S-51, CMU107-S-08, CMU104-S-14-03, CMU105-S-53, DMR-101-065, and DMR-103-099). This study is also supported in part by the Chang Gung Memorial Hospital (grants CMRPF6D0051, CMRPF6D0052, CMRPF6D0053).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cheng, J., Liu, HP., Hwang, SL. et al. Dystonin/BPAG1 modulates diabetes and Alzheimer’s disease cross-talk: a meta-analysis. Neurol Sci 40, 1577–1582 (2019). https://doi.org/10.1007/s10072-019-03879-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-019-03879-3