Abstract
Objectives
To study the effects of a standard acute medication withdrawal program on short-term cortical plasticity mechanisms in patients with medication overuse headache (MOH).
Methods
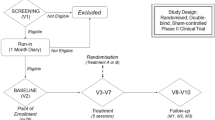
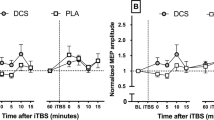
Thirteen patients with MOH and 16 healthy volunteers underwent repetitive transcranial magnetic stimulation (rTMS) over the left motor cortex; in patients with MOH, recordings were performed before and after a 3-week medication withdrawal program. Ten trains of 10 stimuli each (120% resting motor threshold) were delivered at 1 Hz or 5 Hz in two separate sessions in a randomised order. Motor evoked potential (MEP) amplitudes were measured from the right first dorsal interosseous muscle and the slope of the linear regression line from the first to the tenth stimuli was calculated for each participant.
Results
All subjects exhibited MEP amplitude inhibition in response to 1 Hz rTMS. Alternatively, the 5-Hz trains of rTMS inhibited rather than potentiated MEP amplitudes in patients with MOH. The physiological potentiating effect of 5 Hz rTMS on MEP amplitudes was restored after drug withdrawal and in proportion with the percentage reduction in monthly headache days in patients with MOH.
Conclusions
The results suggest that acute medication withdrawal normalises brain responses in patients with MOH. Clinical improvements after medication withdrawal may reflect the reversal of neurophysiological dysfunction. Accordingly, medication withdrawal should be offered to patients with MOH as early as possible in order to prevent the development of more pronounced alterations in brain plasticity.



Similar content being viewed by others
References
No authors listed (2018) Headache Classification Committee of the International Headache Society (IHS) the international classification of headache disorders, 3rd edition. Cephalalgia 38:1–211. https://doi.org/10.1177/0333102417738202
Coppola G, Currà A, Di Lorenzo C et al (2010) Abnormal cortical responses to somatosensory stimulation in medication-overuse headache. BMC Neurol 10:126. https://doi.org/10.1186/1471-2377-10-126
Siniatchkin M, Gerber WD, Kropp P, Vein A (1998) Contingent negative variation in patients with chronic daily headache. Cephalalgia 18:565–569 discussion 531
Ferraro D, Vollono C, Miliucci R, Virdis D, de Armas L, Pazzaglia C, le Pera D, Tarantino S, Balestri M, di Trapani G, Valeriani M (2012) Habituation to pain in “medication overuse headache”: a CO2 laser-evoked potential study. Headache 52:792–807
Rankin CH, Abrams T, Barry RJ, Bhatnagar S, Clayton DF, Colombo J, Coppola G, Geyer MA, Glanzman DL, Marsland S, McSweeney FK, Wilson DA, Wu CF, Thompson RF (2009) Habituation revisited: an updated and revised description of the behavioral characteristics of habituation. Neurobiol Learn Mem 92:135–138. https://doi.org/10.1016/j.nlm.2008.09.012
Cortese F, Pierelli F, Pauri F, di Lorenzo C, Lepre C, Malavolta G, Merluzzo C, Parisi V, Serrao M, Coppola G (2018) Short-term cortical synaptic depression/potentiation mechanisms in chronic migraine patients with or without medication overuse. Cephalalgia 033310241878474. https://doi.org/10.1177/0333102418784747
Currà A, Coppola G, Gorini M, Porretta E, Bracaglia M, di Lorenzo C, Schoenen J, Pierelli F (2011) Drug-induced changes in cortical inhibition in medication overuse headache. Cephalalgia 31:1282–1290. https://doi.org/10.1177/0333102411415877
Rossi P, Faroni JV, Tassorelli C, Nappi G (2013) Advice alone versus structured detoxification programmes for complicated medication overuse headache (MOH): a prospective, randomized, open-label trial. J Headache Pain 14:10. https://doi.org/10.1186/1129-2377-14-10
Pascual-Leone A, Valls-Solé J, Wassermann EM, Hallett M (1994) Responses to rapid-rate transcranial magnetic stimulation of the human motor cortex. Brain 117(Pt 4):847–858
Pascual-Leone A, Tormos JM, Keenan J, Tarazona F, Cañete C, Catalá MD (1998) Study and modulation of human cortical excitability with transcranial magnetic stimulation. J Clin Neurophysiol 15:333–343
Chen R, Classen J, Gerloff C, Celnik P, Wassermann EM, Hallett M, Cohen LG (1997) Depression of motor cortex excitability by low-frequency transcranial magnetic stimulation. Neurology 48:1398–1403
García-Larrea L, Peyron R, Mertens P, Gregoire CM, Lavenne F, le Bars D, Convers P, Mauguière F, Sindou M, Laurent B (1999) Electrical stimulation of motor cortex for pain control: a combined PET-scan and electrophysiological study. Pain 83:259–273
Pagano RL, Fonoff ET, Dale CS, Ballester G, Teixeira MJ, Britto LRG (2012) Motor cortex stimulation inhibits thalamic sensory neurons and enhances activity of PAG neurons: possible pathways for antinociception. Pain 153:2359–2369. https://doi.org/10.1016/j.pain.2012.08.002
Uddin LQ (2017) Anatomy of the salience network. In: Uddin LQ (ed) Salience Network of the Human Brain. Academic Press, Cambridge, pp 5–10
Ayzenberg I, Obermann M, Nyhuis P, Gastpar M, Limmroth V, Diener HC, Kaube H, Katsarava Z (2006) Central sensitization of the trigeminal and somatic nociceptive systems in medication overuse headache mainly involves cerebral supraspinal structures. Cephalalgia 26:1106–1114. https://doi.org/10.1111/j.1468-2982.2006.01183.x
Perrotta A, Serrao M, Sandrini G, Burstein R, Sances G, Rossi P, Bartolo M, Pierelli F, Nappi G (2010) Sensitisation of spinal cord pain processing in medication overuse headache involves supraspinal pain control. Cephalalgia 30:272–284
Peyron R, García-Larrea L, Grégoire MC, Costes N, Convers P, Lavenne F, Mauguière F, Michel D, Laurent B (1999) Haemodynamic brain responses to acute pain in humans: sensory and attentional networks. Brain 122:1765–1780
Riederer F, Gantenbein AR, Marti M, Luechinger R, Kollias S, Sandor PS (2013) Decrease of gray matter volume in the midbrain is associated with treatment response in medication-overuse headache: possible influence of orbitofrontal cortex. J Neurosci 33:15343–15349
Chen Z, Chen X, Liu M, Liu S, Ma L, Yu S (2017) Disrupted functional connectivity of periaqueductal gray subregions in episodic migraine. J Headache Pain 18:36. https://doi.org/10.1186/s10194-017-0747-9
Chen Z, Chen X, Liu M, Liu S, Ma L, Yu S (2017) Texture features of periaqueductal gray in the patients with medication-overuse headache. J Headache Pain 18:14. https://doi.org/10.1186/s10194-017-0727-0
Michels L, Christidi F, Steiger VR, Sándor PS, Gantenbein AR, Landmann G, Schreglmann SR, Kollias S, Riederer F (2017) Pain modulation is affected differently in medication-overuse headache and chronic myofascial pain – a multimodal MRI study. Cephalalgia 37:764–779. https://doi.org/10.1177/0333102416652625
Chen Z, Jia Z, Chen X, Liu M, Liu S, Ma L, Yu S (2017) Volumetric abnormalities of thalamic subnuclei in medication-overuse headache. J Headache Pain 18:82. https://doi.org/10.1186/s10194-017-0791-5
Fumal A, Laureys S, Di Clemente L et al (2006) Orbitofrontal cortex involvement in chronic analgesic-overuse headache evolving from episodic migraine. Brain 129:543–550. https://doi.org/10.1093/brain/awh691
Mehnert J, Hebestreit J, May A (2018) Cortical and subcortical alterations in medication overuse headache. Front Neurol 9:499. https://doi.org/10.3389/fneur.2018.00499
Funding
The contribution of the G.B. Bietti Foundation to this article was supported by the Italian Ministry of Health and Fondazione Roma.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cortese, F., Pierelli, F., Pauri, F. et al. Withdrawal from acute medication normalises short-term cortical synaptic potentiation in medication overuse headache. Neurol Sci 40, 963–969 (2019). https://doi.org/10.1007/s10072-019-03735-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-019-03735-4