Abstract
Objective
This study aimed to systematically review clinical trials about the effect of statins as adjunct to mechanical periodontal therapy, on probing pocket depth, clinical attachment level, and intrabony defects, in comparison to mechanical periodontal therapy alone or in association with placebo.
Material and methods
Three databases were searched for controlled clinical trials that used any locally delivered or systemically statin as a sole adjunctive therapy to mechanical periodontal treatment. Weighted mean differences between baseline and 6 months after periodontal treatment for clinical attachment level (CAL), probing pocket depth (PPD), and intrabony defect (IBD) were calculated. A high heterogeneity was detected. Therefore, a meta-regression adjusted for type of statin and year of publication was performed.
Results
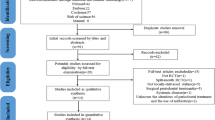
Fifteen studies were included in the systematic review, and ten studies were included in the meta-analysis. In the meta-regression, the adjunct use of simvastatin, rosuvastatin, and atorvastatin additionally reduced PPD in comparison to mechanical periodontal therapy and a placebo gel (2.90 ± 0.35, 3.90 ± 0.77, 3.06 ± 0.71 mm, respectively; p < 0.05). Regarding the resolution of IBD, simvastatin and rosuvastatin significantly improved in comparison to control group (0.89 ± 0.35 and 1.93 ± 0.77 mm, respectively; p < 0.05). No statistically significant difference was found between the statins for both PPD and IBD (p < 0.05). Regarding CAL gain, simvastatin provided a statistically significant improvement as compared to the control group (2.02 ± 0.79 mm; p = 0.043).
Conclusions
The use of statins, used as sole adjuncts to mechanical periodontal treatment, improved the periodontal parameters. In the quantitative analyses, simvastatin was the only drug that showed additional benefits in all evaluated parameters.
Clinical relevance
Statins promote significantly clinical periodontal improvements when administered in association with non-surgical scaling and root planning (SRP), when compared to SRP alone or in association with a placebo.


Similar content being viewed by others

References
Baigent C, Keech A, Kearney PM et al (2005) Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet 366:1267–1278
Maron DJ, Fazio S, Linton MF (2000) Current perspectives on statins. Circulation 101:207–213
Todd PA, Goa KL (1990) Simvastatin. A review of its pharmacological properties and therapeutic potential in hypercholesterolaemia. Drugs 40(4):583–607
Zhou Q, Liao JK (2009) Statins and cardiovascular diseases: from cholesterol lowering to pleiotropy. Curr Pharm Des 15(5):467–478. https://doi.org/10.2174/138161209787315684
Ramfjord SP, Knowles JW, Nissle RR, Burgett FG, Shick RA (1975) Results following three modalities of periodontal therapy. J Periodontol 46(9):522–526. https://doi.org/10.1902/jop.1975.46.9.522
Deas DE, Moritz AJ, Sagun RS, Gruwell SF, Powell CA (2016) Scaling and root planing vs. conservative surgery in the treatment of chronic periodontitis. Periodontol 2000 71:128–139
Muniz FW, de Oliveira CC, de Sousa Carvalho R, Moreira MM, de Moraes ME, Martins RS (2013) Azithromycin: a new concept in adjuvant treatment of periodontitis. Eur J Pharmacol 705(1-3):135–139. https://doi.org/10.1016/j.ejphar.2013.02.044
Caton JG, Greenstein G (1993) Factors related to periodontal regeneration. Periodontol 2000 1:9–15
Dye BA (2012) Global periodontal disease epidemiology. Periodontol 58(1):10–25. https://doi.org/10.1111/j.1600-0757.2011.00413.x
Chen J, Chen Q, Hu B, Wang Y, Song J (2016) Effectiveness of alendronate as an adjunct to scaling and root planing in the treatment of periodontitis: a meta-analysis of randomized controlled clinical trials. J Periodontal Implant Sci 46(6):382–395. https://doi.org/10.5051/jpis.2016.46.6.382
Estanislau IM, Terceiro IR, Lisboa MR, Teles PB, Carvalho RS, Martins RS, Moreira MM (2015) Pleiotropic effects of statins on the treatment of chronic periodontitis—a systematic review. Br J Clin Pharmacol 79(6):877–885. https://doi.org/10.1111/bcp.12564
Mundy G, Garrett R, Harris S, Chan J, Chen D, Rossini G, Boyce B, Zhao M, Gutierrez G (1999) Stimulation of bone formation in vitro and in rodents by statins. Science 286(5446):1946–1949. https://doi.org/10.1126/science.286.5446.1946
Mennickent CS, Bravo DM, Calvo MC, Avello LM (2008) Pleiotropic effects of statins. Rev Med Chil 136:775–782
Kavalipati N, Shah J, Ramakrishan A, Vasnawala H (2015) Pleiotropic effects of statins. Indian J Endocrinol Metab 19(5):554–562. https://doi.org/10.4103/2230-8210.163106
Adam O, Laufs U (2008) Antioxidative effects of statins. Arch Toxicol 82(12):885–892. https://doi.org/10.1007/s00204-008-0344-4
Cicek Ari V, Ilarslan YD, Erman B, Sarkarati B, Tezcan I, Karabulut E, Oz SG, Tanriover MD, Sengun D, Berker E (2016) Statins and IL-1β, IL-10, and MPO levels in gingival crevicular fluid: preliminary results. Inflammation 39(4):1547–1557. https://doi.org/10.1007/s10753-016-0390-7
Lindy O, Suomalainen K, Mäkelä M, Lindy S (2008) Statin use is associated with fewer periodontal lesions: a retrospective study. BMC Oral Health 8(1):16. https://doi.org/10.1186/1472-6831-8-16
Cunha-Cruz J, Saver B, Maupome G, Hujoel PP (2006) Statin use and tooth loss in chronic periodontitis patients. J Periodontol 77(6):1061–1066. https://doi.org/10.1902/jop.2006.050280
Saxlin T, Suominen-Taipale L, Knuuttila M, Alha P, Ylöstalo P (2009) Dual effect of statin medication on the periodontium. J Clin Periodontol 36:997–1003
Saver BG, Hujoel PP, Cunha-Cruz J, Maupomé G (2007) Are statins associated with decreased tooth loss in chronic periodontitis? J Clin Periodontol 34(3):214–219. https://doi.org/10.1111/j.1600-051X.2006.01046.x
de Mones E, Schlaubitz S, Catros S, Fricain JC (2015) Statins and alveolar bone resorption: a narrative review of preclinical and clinical studies. Oral Surg Oral Med Oral Pathol Oral Radiol 119(1):65–73. https://doi.org/10.1016/j.oooo.2014.09.030
Sterne JA, Hernán MA, Reeves BC (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919. https://doi.org/10.1136/bmj.i4919
Higgins JP, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA, C.B.M. Group, C.S.M. Group (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343(oct18 2):d5928. https://doi.org/10.1136/bmj.d5928
Guyatt GH, Oxman AD, Schünemann HJ, Tugwell P, Knottnerus A (2011) GRADE guidelines: a new series of articles in the journal of clinical epidemiology. J Clin Epidemiol 64(4):380–382. https://doi.org/10.1016/j.jclinepi.2010.09.011
Higgins JPT, Green S (editors) Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. The Cochrane Collaboration, 2011. Available from www.cochrane-handbook.org. Chichester, UK: John Wiley & Sons, Ltd. Acessed 22th Nov 2016
Harbord R, Higgins J (2008) Meta-regression in Stata. Stata J 8:493–519
Sterne J, Bradburn M, Egger M (2008) Meta-analysis in StataTM. In: Egger M, Smith G, Altman D (eds) Systematic review in health care, 2nd edn. BMJ Publishing Group, London, pp. 347–369
Fajardo ME, Rocha ML, Sanchez-Marin FJ, Espinosa-Chavez EJ (2010) Effect of atorvastatin on chronic periodontitis: a randomized pilot study. J Clin Periodontol 37(11):1016–1022. https://doi.org/10.1111/j.1600-051X.2010.01619.x
Fentoglu O, Kirzioglu FY, Ozdem M, Kocak H, Sutcu R, Sert T (2012) Proinflammatory cytokine levels in hyperlipidemic patients with periodontitis after periodontal treatment. Oral Dis 18(3):299–306. https://doi.org/10.1111/j.1601-0825.2011.01880.x
Sangwan A, Tewari S, Singh H, Sharma RK, Narula SC (2016) Effect of hyperlipidemia on response to nonsurgical periodontal therapy: statin users versus nonusers. Eur J Dent 10(1):69–76. https://doi.org/10.4103/1305-7456.175685
Rosenberg DR, Andrade CX, Chaparro AP, Inostroza CM, Ramirez V, Violant D, Nart J (2015) Short-term effects of 2% atorvastatin dentifrice as an adjunct to periodontal therapy: a randomized double blind clinical trial. J Periodontol 86(5):623–630. https://doi.org/10.1902/jop.2015.140503
Pradeep AR, Thorat MS (2010) Clinical effect of subgingivally delivered simvastatin in the treatment of patients with chronic periodontitis: a randomized clinical trial. J Periodontol 81(2):214–222. https://doi.org/10.1902/jop.2009.090429
Pradeep AR, Priyanka N, Kalra N, Naik SB, Singh SP, Martande S (2012) Clinical efficacy of subgingivally delivered 1.2-mg simvastatin in the treatment of individuals with class II furcation defects: a randomized controlled clinical trial. J Periodontol 83(12):1472–1479. https://doi.org/10.1902/jop.2012.110716
Rath A, Mahenra J, Thomas L, Sandhu M, Namasi A, Ramakrishna T (2012) A clinical, radiological and IL-6 evaluation of subgingivally delivered simvastatin in the treatment of chronic periodontitis. Int J Drug Deliv 4:70–81
Pradeep AR, Rao NS, Bajaj P, Kumari M (2013) Efficacy of subgingivally delivered simvastatin in the treatment of patients with type 2 diabetes and chronic periodontitis: a randomized double-masked controlled clinical trial. J Periodontol 84(1):24–31. https://doi.org/10.1902/jop.2012.110721
Pradeep AR, Kumari M, Rao NS, Martande SS, Naik SB (2013) Clinical efficacy of subgingivally delivered 1.2% atorvastatin in chronic periodontitis: a randomized controlled clinical trial. J Periodontol 84(7):871–879. https://doi.org/10.1902/jop.2012.120393
Rao NS, Pradeep AR, Bajaj P, Kumari M, Naik SB (2013) Simvastatin local drug delivery in smokers with chronic periodontitis: a randomized controlled clinical trial. Aust Dent J 58(2):156–162. https://doi.org/10.1111/adj.12042
Pradeep AR, Karvekar S, Nagpal K, Patnaik K, Guruprasad CN, Kumaraswamy KM (2015) Efficacy of locally delivered 1.2% rosuvastatin gel to non-surgical treatment of patients with chronic periodontitis: a randomized, placebo-controlled clinical trial. J Periodontol 86(6):738–745. https://doi.org/10.1902/jop.2015.140631
Surve SM, Acharya AB, Thakur SL (2015) Efficacy of subgingivally delivered atorvastatin and simvastatin as an adjunct to scaling and root planing. Drug Metabol Personal Ther 30(4):263–269. https://doi.org/10.1515/dmpt-2015-0024
Kumari M, Martande SS, Pradeep AR (2016) Subgingivally delivered 1.2% atorvastatin in the treatment of chronic periodontitis among smokers: a randomized, controlled clinical trial. J Investig Clin Dent 8(2):e12213. https://doi.org/10.1111/jicd.12213
Pradeep AR, Garg V, Kanoriya D, Singhal S (2016) 1.2% Rosuvastatin versus 1.2% atorvastatin gel local drug delivery and re-delivery in treatment of intrabony defects in chronic periodontitis: a randomized placebo controlled clinical trial. J Periodontol 87(7):756–762. https://doi.org/10.1902/jop.2016.150706
Pradeep AR, Kanoriya D, Singhal S, Garg V, Manohar B, Chatterjee A (2016) Comparative evaluation of subgingivally delivered 1% alendronate versus 1.2% atorvastatin gel in treatment of chronic periodontitis: a randomized placebo-controlled clinical trial. J Investig Clin Dent 8(3):e12215. https://doi.org/10.1111/jicd.12215
Fentoğlu Ö, Kirzioğlu FY, Tözüm Bulut M et al (2015) Serum Lp-PLA2: as a novel viewpoint in periodontal treatment of hyperlipidaemics. Turk J Med Sci 45(3):619–626. https://doi.org/10.3906/sag-1406-75
Sirtori CR (2014) The pharmacology of statins. Pharmacol Res 88:3–11. https://doi.org/10.1016/j.phrs.2014.03.002
Viereck V, Gründker C, Blaschke S et al (2005) Atorvastatin stimulates the production of osteoprotegerin by human osteoblasts. J Cell Biochem 96:1244–1253
Blanco-Colio LM, Tuñón J, Martín-Ventura JL, Egido J (2003) Anti-inflammatory and immunomodulatory effects of statins. Kidney Int 63(1):12–23. https://doi.org/10.1046/j.1523-1755.2003.00744.x
Sakoda K, Yamamoto M, Negishi Y, Liao JK, Node K, Izumi Y (2006) Simvastatin decreases IL-6 and IL-8 production in epithelial cells. J Dent Res 85(6):520–523. https://doi.org/10.1177/154405910608500608
Jerwood S, Cohen J (2008) Unexpected antimicrobial effect of statins. J Antimicrob Chemother 61(2):362–364. https://doi.org/10.1093/jac/dkm496
Kamio K, Liu XD, Sugiura H, Togo S, Kawasaki S, Wang X, Ahn Y, Hogaboam C, Rennard SI (2010) Statins inhibit matrix metalloproteinase release from human lung fibroblasts. Eur Respir J 35(3):637–646. https://doi.org/10.1183/09031936.00134707
Dalcico R, de Menezes AM, Deocleciano OB et al (2013) Protective mechanisms of simvastatin in experimental periodontal disease. J Periodontol 84(8):1145–1157. https://doi.org/10.1902/jop.2012.120114
Goes P, Lima NA, Rodrigues JA, Benevides NM, Brito GA, Lima V (2016) Anti-inflammatory and anti-resorptive effects of atorvastatin on alveolar bone loss in Wistar rats. Braz Dent J 27(3):267–272. https://doi.org/10.1590/0103-6440201600600
Thapa S, Wei F (2016) The association between high serum Total cholesterol and periodontitis—an NHANES 2011–2012 study of American adults. J Periodontol 87(11):1286–1294. https://doi.org/10.1902/jop.2016.150648
Zhou X, Zhang W, Liu X, Li Y (2015) Interrelationship between diabetes and periodontitis: role of hyperlipidemia. Arch Oral Biol 60(4):667–674. https://doi.org/10.1016/j.archoralbio.2014.11.008
Pragati S, Ashok S, Kuldeep S (2011) Recent advances in periodontal drug delivery systems. Int. J Drug Deliv 1:1–14
Needleman IG, Pandya NV, Smith SR, Foyle DM (1995) The role of antibiotics in the treatment of periodontitis (part 2—controlled drug delivery). Eur J Prosthodont Restor Dent 3(3):111–117
Bertl K, Parllaku A, Pandis N, Buhlin K, Klinge B, Stavropoulos A (2017) The effect of local and systemic statin use as an adjunct to non-surgical and surgical periodontal therapy—a systematic review and meta-analysis. J Dent 67:18–28. https://doi.org/10.1016/j.jdent.2017.08.011
Sgolastra F, Gatto R, Petrucci A, Monaco A (2012) Effectiveness of systemic amoxicillin/metronidazole as adjunctive therapy to scaling and root planing in the treatment of chronic periodontitis: a systematic review and meta-analysis. J Periodontol 83(10):1257–1269. https://doi.org/10.1902/jop.2012.110625
Matesanz-Pérez P, García-Gargallo M, Figuero E, Bascones-Martínez A, Sanz M, Herrera D (2013) A systematic review on the effects of local antimicrobials as adjuncts to subgingival debridement, compared with subgingival debridement alone, in the treatment of chronic periodontitis. J Clin Periodontol 40(3):227–241. https://doi.org/10.1111/jcpe.12026
Jeger R, Dieterle T (2012) Statins: have we found the holy grail? Swiss Med Wkly 142:w13515
Schachter M (2005) Chemical, pharmacokinetic and pharmacodynamic properties of statins: an update. Fundam Clin Pharmacol 19(1):117–125. https://doi.org/10.1111/j.1472-8206.2004.00299.x
Funding
This study was self-funded by the authors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Ethical approval does not apply to systematic reviews.
Informed consent
Informed consent does not apply to systematic reviews.
Electronic supplementary material
Figure S1
Forest plot of PPD reduction. (GIF 25 kb)
Figure S2
Funnel plot of the risk of bias analysis of pocket depth at 6-months follow-up. (GIF 10 kb)
Figure S3
Cumulative meta-analysis of pocket depth at 6-months follow-up. (GIF 17 kb)
Figure S4
Forest plot of IBD decrease. (GIF 18 kb)
Figure S5
Funnel plot of the risk of bias analysis of intrabony defect at 6-months follow-up. (GIF 7 kb)
Figure S6
Cumulative meta-analysis of intrabony defect at 6-months follow-up. (GIF 2 kb)
Figure S7
Forest plot of CAL gain. (GIF 18 kb)
Figure S8
Funnel plot of the risk of bias analysis of clinical attachment level at 6-months follow-up. (GIF 9 kb)
Figure S9
Cumulative meta-analysis of clinical attachment level at 6-months follow-up. (GIF 17 kb)
Rights and permissions
About this article
Cite this article
Muniz, F.W.M.G., Taminski, K., Cavagni, J. et al. The effect of statins on periodontal treatment—a systematic review with meta-analyses and meta-regression. Clin Oral Invest 22, 671–687 (2018). https://doi.org/10.1007/s00784-018-2354-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-018-2354-9