Abstract
Background
Vagal nerve stimulation (VNS) response is not immediate. A progressive decline in seizure frequency is usually found during a period of 12–18 months after implantation. During this time, the patient’s medication is usually modified, which can create doubts about whether their clinical improvement is due to medication changes or to VNS itself. Our goal is to compare two groups of patients treated with VNS, with and without changes in their medication.
Methods
We prospectively analyze 85 patients who were treated with VNS in our hospital between 2005 and 2014. In 43 patients, changes in the antiepileptic drugs (EAD) were not allowed during the postoperative follow-up and they were compared with 42 patients who were left at the option of neurologist make changes in medication. We analyzed the clinical situation at 18 months and compared the two groups.
Results
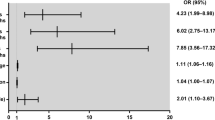
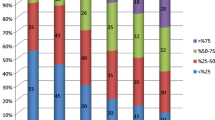
Overall, 54.1% of patients had a reduction in seizures of 50% or higher (responders). In the group with no changes in medication, responders reached 63%, while in the group in which changes in medication were allowed, 45.2% were responders. Between responders and non-responders, there were no statistical differences in type of epilepsy, frequency, previous surgery, or intensity of stimulation.
Conclusions
We did not find a statistical difference in seizure frequency reduction between patients with or without changes in medication during their follow-up, so changes in medication did not improve the outcome. Furthermore, the absence of changes in AED can help to optimize the parameters of the stimulator in order to improve its effectiveness.
Similar content being viewed by others
References
Alonso-Vanegas MA, Austria-Velasquez J, Lopez-Gomez M, Brust-Mascher E (2010) Chronic intermittent vagal nerve stimulation in the treatment of refractory epilepsy: experience in Mexico with 35 cases. Cir Cir 78(15–23):24
Amar AP, Apuzzo ML (2003) Vagus nerve stimulation therapy for patients with persistent seizures after epilepsy surgery. Stereotact Funct Neurosurg 80:9–13
Ben-Menachem E, Hellstrom K, Waldton C, Augustinsson LE (1999) Evaluation of refractory epilepsy treated with vagus nerve stimulation for up to 5 years. Neurology 52:1265–1267
Ben-Menachem E, Manon-Espaillat R, Ristanovic R, Wilder BJ, Stefan H, Mirza W, Tarver WB, Wernicke JF (1994) Vagus nerve stimulation for treatment of partial seizures: 1. A controlled study of effect on seizures. First International Vagus Nerve Stimulation Study Group. Epilepsia 35:616–626
Boon P, Vonck K, De Reuck J, Caemaert J (2001) Vagus nerve stimulation for refractory epilepsy. Seizure 10:448–455
Carius A, Wintermantel A (2013) Vagus nerve stimulation therapy in epilepsy patients: long-term outcome and adverse effects: a retrospective analysis. Nervenarzt 84:1473–1485
Connor DE Jr, Nixon M, Nanda A, Guthikonda B (2012) Vagal nerve stimulation for the treatment of medically refractory epilepsy: a review of the current literature. Neurosurg Focus 32:E12
Ching J, Khan S, White P, Reed J, Ramnarine D, Sieradzan K, Sandeman D (2013) Long-term effectiveness and tolerability of vagal nerve stimulation in adults with intractable epilepsy: a retrospective analysis of 100 patients. Br J Neurosurg 27:228–234
DeGiorgio CM, Schachter SC, Handforth A, Salinsky M, Thompson J, Uthman B, Reed R, Collins S, Tecoma E, Morris GL, Vaughn B, Naritoku DK, Henry T, Labar D, Gilmartin R, Labiner D, Osorio I, Ristanovic R, Jones J, Murphy J, Ney G, Wheless J, Lewis P, Heck C (2000) Prospective long-term study of vagus nerve stimulation for the treatment of refractory seizures. Epilepsia 41:1195–1200
Elliott RE, Morsi A, Geller EB, Carlson CC, Devinsky O, Doyle WK (2011) Impact of failed intracranial epilepsy surgery on the effectiveness of subsequent vagus nerve stimulation. Neurosurgery 69:1210–1217
Elliott RE, Morsi A, Kalhorn SP, Marcus J, Sellin J, Kang M, Silverberg A, Rivera E, Geller E, Carlson C, Devinsky O, Doyle WK (2011) Vagus nerve stimulation in 436 consecutive patients with treatment-resistant epilepsy: long-term outcomes and predictors of response. Epilepsy Behav: E&B 20:57–63
Elliott RE, Morsi A, Tanweer O, Grobelny B, Geller E, Carlson C, Devinsky O, Doyle WK (2011) Efficacy of vagus nerve stimulation over time: review of 65 consecutive patients with treatment-resistant epilepsy treated with VNS > 10 years. Epilepsy Behav: E&B 20:478–483
Englot DJ, Rolston JD, Wright CW, Hassnain KH, Chang EF (2015) Rates and predictors of seizure freedom with vagus nerve stimulation for intractable epilepsy. Neurosurgery 79(3):345–353
Garcia-Navarrete E, Torres CV, Gallego I, Navas M, Pastor J, Sola RG (2013) Long-term results of vagal nerve stimulation for adults with medication-resistant epilepsy who have been on unchanged antiepileptic medication. Seizure 22:9–13
Ghaemi K, Elsharkawy AE, Schulz R, Hoppe M, Polster T, Pannek H, Ebner A (2010) Vagus nerve stimulation: outcome and predictors of seizure freedom in long-term follow-up. Seizure 19:264–268
Handforth A, DeGiorgio CM, Schachter SC, Uthman BM, Naritoku DK, Tecoma ES, Henry TR, Collins SD, Vaughn BV, Gilmartin RC, Labar DR, Morris GL 3rd, Salinsky MC, Osorio I, Ristanovic RK, Labiner DM, Jones JC, Murphy JV, Ney GC, Wheless JW (1998) Vagus nerve stimulation therapy for partial-onset seizures: a randomized active-control trial. Neurology 51:48–55
Janszky J, Hoppe M, Behne F, Tuxhorn I, Pannek HW, Ebner A (2005) Vagus nerve stimulation: predictors of seizure freedom. J Neurol Neurosurg Psychiatry 76:384–389
Labar D (2004) Vagus nerve stimulation for 1 year in 269 patients on unchanged antiepileptic drugs. Seizure 13:392–398
Morris GL 3rd, Gloss D, Buchhalter J, Mack KJ, Nickels K, Harden C (2013) Evidence-based guideline update: vagus nerve stimulation for the treatment of epilepsy: report of the guideline development subcommittee of the American Academy of Neurology. Epilepsy Curr Am Epilepsy Soc 13:297–303
Muller K, Fabo D, Entz L, Kelemen A, Halasz P, Rasonyi G, Eross L (2010) Outcome of vagus nerve stimulation for epilepsy in Budapest. Epilepsia 51(Suppl 3):98–101
Panebianco M, Rigby A, Weston J, Marson AG (2015) Vagus nerve stimulation for partial seizures. Cochrane Database Syst Rev 4:CD002896
Pastor J, Hernando-Requejo V, Dominguez-Gadea L, de Llano I, Meilan-Paz ML, Martinez-Chacon JL, Sola RG (2005) Impact of experience on improving the surgical outcome in temporal lobe epilepsy. Rev Neurol 41:709–716
Ryvlin P, Gilliam FG, Nguyen DK, Colicchio G, Iudice A, Tinuper P, Zamponi N, Aguglia U, Wagner L, Minotti L, Stefan H, Boon P, Sadler M, Benna P, Raman P, Perucca E (2014) The long-term effect of vagus nerve stimulation on quality of life in patients with pharmacoresistant focal epilepsy: the PuLsE (open prospective randomized long-term effectiveness) trial. Epilepsia 55:893–900
Sola RG, Hernando-Requejo V, Pastor J, Garcia-Navarrete E, DeFelipe J, Alijarde MT, Sanchez A, Dominguez-Gadea L, Martin-Plasencia P, Maestu F, DeFelipe-Oroquieta J, Ramon-Cajal S, Pulido-Rivas P (2005) Pharmacoresistant temporal-lobe epilepsy. Exploration with foramen ovale electrodes and surgical outcomes. Rev Neurol 41:4–16
Wasade VS, Schultz L, Mohanarangan K, Gaddam A, Schwalb JM, Spanaki-Varelas M (2015) Long-term seizure and psychosocial outcomes of vagus nerve stimulation for intractable epilepsy. Epilepsy Behav: E&B 53:31–36
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
García-Pallero, M.A., García-Navarrete, E., Torres, C.V. et al. Effectiveness of vagal nerve stimulation in medication-resistant epilepsy. Comparison between patients with and without medication changes. Acta Neurochir 159, 131–136 (2017). https://doi.org/10.1007/s00701-016-3027-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-016-3027-6