Abstract
Aims
Glomerular basement membrane (GBM) thickening is considered as one of the earliest detectable pathological features of diabetic nephropathy (DN). However, whether the thickness of GBM will impact the prognosis of DN remains largely unknown. Our aim was to explore the relationship between thickness of GBM and DN progression in patients with type 2 diabetes mellitus (T2DM).
Methods
A total of 118 patients with T2DM and biopsy-proven DN who received follow-up for at least 1 year were recruited. The patients were divided into two groups according to the median (787 nm) of the GBM thickness: Group 1: GBM thickness < 787 nm (n = 59), and Group 2: GBM thickness ≥ 787 nm (n = 59). The GBM width was estimated by the direct GBM measurements as recently modified by Haas. Renal outcomes were defined by progression to ESRD and/or doubling of serum creatinine (D-Cr). The influence of GBM thickness on renal outcomes was assessed using Cox regression.
Results
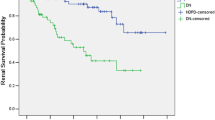
Compared with the Group 1, patients in Group 2 had more serious renal insufficiency and glomerular lesions. During the follow-up, ESRD occurred in 39.8% of patients, and 8.5% of patients progressed to D-Cr. The univariate analysis indicated the greater width of GBM the higher risk of renal outcomes in T2DM patients with DN (HR [95% CI] = 2.180 [1.246–3.814], p = 0.006). However, the multivariate COX analysis demonstrated that the GBM thickness was not an independent risk factor for progression to ESRD or D-Cr (HR [95% CI] = 0.825 [0.404–1.685], p = 0.597) when adjusting for important clinical variables and pathological findings.
Conclusions
In conclusion, the DN patients with greater width of GBM had relatively poorer renal prognosis, although it did not emerge as an independent indicator of disease progression.






Similar content being viewed by others
References
Alicic RZ, Rooney MT, Tuttle KR (2017) Diabetic kidney disease: challenges, progress, and possibilities. Clin J Am Soc Nephrol CJASN 12:2032–2045
O’Shaughnessy MM, Hogan SL, Poulton CJ, Falk RJ, Singh HK, Nickeleit V, Jennette JC (2017) Temporal and demographic trends in glomerular disease epidemiology in the southeastern United States, 1986–2015. Clin J Am Soc Nephrol CJASN 12:614–623
Liu ZH (2013) Nephrology in china. Nat Rev Nephrol 9:523–528
Zhang L, Long J, Jiang W, Shi Y, He X, Zhou Z, Li Y, Yeung RO, Wang J, Matsushita K, Coresh J, Zhao MH, Wang H (2016) Trends in chronic kidney disease in China. N Engl J Med 375:905–906
Gregg EW, Li Y, Wang J, Burrows NR, Ali MK, Rolka D, Williams DE, Geiss L (2014) Changes in diabetes-related complications in the United States, 1990–2010. N Engl J Med 370:1514–1523
Motawi TK, Shehata NI, ElNokeety MM, El-Emady YF (2018) Potential serum biomarkers for early detection of diabetic nephropathy. Diabetes Res Clin Pract 136:150–158
Al-Rubeaan K, Siddiqui K, Al-Ghonaim MA, Youssef AM, Al-Sharqawi AH, AlNaqeb D (2017) Assessment of the diagnostic value of different biomarkers in relation to various stages of diabetic nephropathy in type 2 diabetic patients. Sci Rep 7:2684
Peired AJ, Sisti A, Romagnani P (2016) Mesenchymal stem cell-based therapy for kidney disease: a review of clinical evidence. Stem Cells Int 2016:4798639
Doshi SM, Friedman AN (2017) Diagnosis and management of type 2 diabetic kidney disease. Clin J Am Soc Nephrol CJASN 12:1366–1373
Najafian B, Mauer M (2012) Morphologic features of declining renal function in type 1 diabetes. Semin Nephrol 32:415–422
Marshall CB (2016) Rethinking glomerular basement membrane thickening in diabetic nephropathy: adaptive or pathogenic? Am J Physiol Ren Physiol 311:F831–f843
Moriya T, Tanaka K, Moriya R (2000) Glomerular structural changes and structural-functional relationships at early stage of diabetic nephropathy in Japanese type 2 diabetic patients. Med Electron Microsc Off J Clin Electron Microsc Soc Jpn 33:115–122
Caramori ML, Parks A, Mauer M (2013) Renal lesions predict progression of diabetic nephropathy in type 1 diabetes. J Am Soc Nephrol JASN 24:1175–1181
Miner JH (2012) The glomerular basement membrane. Exp Cell Res 318:973–978
Miner JH (1999) Renal basement membrane components. Kidney Int 56:2016–2024
Falk RJ, Scheinman JI, Mauer SM, Michael AF (1983) Polyantigenic expansion of basement membrane constituents in diabetic nephropathy. Diabetes 32(Suppl 2):34–39
Kim Y, Kleppel MM, Butkowski R, Mauer SM, Wieslander J, Michael AF (1991) Differential expression of basement membrane collagen chains in diabetic nephropathy. Am J Pathol 138:413–420
Osterby R, Gundersen HJ (1975) Glomerular size and structure in diabetes mellitus. I. Early abnormalities. Diabetologia 11:225–229
Pagtalunan ME, Miller PL, Jumping-Eagle S, Nelson RG, Myers BD, Rennke HG, Coplon NS, Sun L, Meyer TW (1997) Podocyte loss and progressive glomerular injury in type II diabetes. J Clin Investig 99:342–348
Perrin NE, Torbjornsdotter T, Jaremko GA, Berg UB (2010) Risk markers of future microalbuminuria and hypertension based on clinical and morphological parameters in young type 1 diabetes patients. Pediatr Diabetes 11:305–313
Pinsker JE, Shank T, Dassau E, Kerr D (2015) Comment on American Diabetes Association. Approaches to glycemic treatment. Section 7. In: Standards of medical care in diabetes-2015. Diabetes care 2015, vol 38(Suppl. 1):S41–S48. Diabetes Care 38:e174
An Y, Xu F, Le W, Ge Y, Zhou M, Chen H, Zeng C, Zhang H, Liu Z (2015) Renal histologic changes and the outcome in patients with diabetic nephropathy. Nephrol Dial Transplant Off Publ Eur Dial Transplant Assoc Eur Ren Assoc 30:257–266
Tervaert TW, Mooyaart AL, Amann K, Cohen AH, Cook HT, Drachenberg CB, Ferrario F, Fogo AB, Haas M, de Heer E, Joh K, Noel LH, Radhakrishnan J, Seshan SV, Bajema IM, Bruijn JA (2010) Pathologic classification of diabetic nephropathy. J Am Soc Nephrol JASN 21:556–563
Alkayyali S, Lajer M, Deshmukh H, Ahlqvist E, Colhoun H, Isomaa B, Rossing P, Groop L, Lyssenko V (2013) Common variant in the HMGA2 gene increases susceptibility to nephropathy in patients with type 2 diabetes. Diabetologia 56:323–329
Mauer SM, Steffes MW, Ellis EN, Sutherland DE, Brown DM, Goetz FC (1984) Structural-functional relationships in diabetic nephropathy. J Clin Investig 74:1143–1155
Caramori ML, Kim Y, Huang C, Fish AJ, Rich SS, Miller ME, Russell G, Mauer M (2002) Cellular basis of diabetic nephropathy: 1. Study design and renal structural-functional relationships in patients with long-standing type 1 diabetes. Diabetes 51:506–513
Hayashi H, Karasawa R, Inn H, Saitou T, Ueno M, Nishi S, Suzuki Y, Ogino S, Maruyama Y, Kouda Y et al (1992) An electron microscopic study of glomeruli in Japanese patients with non-insulin dependent diabetes mellitus. Kidney Int 41:749–757
Fufaa GD, Weil EJ, Lemley KV, Knowler WC, Brosius FC 3rd, Yee B, Mauer M, Nelson RG (2016) Structural predictors of loss of renal function in American Indians with type 2 diabetes. Clin J Am Soc Nephrol CJASN 11:254–261
White KE, Bilous RW (2000) Type 2 diabetic patients with nephropathy show structural-functional relationships that are similar to type 1 disease. J Am Soc Nephrol JASN 11:1667–1673
Nosadini R, Velussi M, Brocco E, Bruseghin M, Abaterusso C, Saller A, Dalla Vestra M, Carraro A, Bortoloso E, Sambataro M, Barzon I, Frigato F, Muollo B, Chiesura-Corona M, Pacini G, Baggio B, Piarulli F, Sfriso A, Fioretto P (2000) Course of renal function in type 2 diabetic patients with abnormalities of albumin excretion rate. Diabetes 49:476–484
Meyer TW, Bennett PH, Nelson RG (1999) Podocyte number predicts long-term urinary albumin excretion in Pima Indians with type II diabetes and microalbuminuria. Diabetologia 42:1341–1344
Drummond KN, Kramer MS, Suissa S, Levy-Marchal C, Dell’Aniello S, Sinaiko A, Mauer M (2003) Effects of duration and age at onset of type 1 diabetes on preclinical manifestations of nephropathy. Diabetes 52:1818–1824
Krolewski AS, Skupien J, Rossing P, Warram JH (2017) Fast renal decline to end-stage renal disease: an unrecognized feature of nephropathy in diabetes. Kidney Int 91:1300–1311
Li L, Zhang X, Li Z, Zhang R, Guo R, Yin Q, Yang L, Yue R, Su B, Huang S, Xu H, He C, Liu F (2017) Renal pathological implications in type 2 diabetes mellitus patients with renal involvement. J Diabetes Complic 31:114–121
Moriya T, Tanaka K, Hosaka T, Hirasawa Y, Fujita Y (2008) Renal structure as an indicator for development of albuminuria in normo- and microalbuminuric type 2 diabetic patients. Diabetes Res Clin Pract 82:298–304
Gambara V, Mecca G, Remuzzi G, Bertani T (1993) Heterogeneous nature of renal lesions in type II diabetes. J Am Soc Nephrol JASN 3:1458–1466
Osterby R, Gall MA, Schmitz A, Nielsen FS, Nyberg G, Parving HH (1993) Glomerular structure and function in proteinuric type 2 (non-insulin-dependent) diabetic patients. Diabetologia 36:1064–1070
Guan M, Ma J, Keaton JM, Dimitrov L, Mudgal P, Stromberg M, Bonomo JA, Hicks PJ, Freedman BI, Bowden DW, Ng MC (2016) Association of kidney structure-related gene variants with type 2 diabetes-attributed end-stage kidney disease in African Americans. Hum Genet 135:1251–1262
Chen C, Wang C, Hu C, Han Y, Zhao L, Zhu X, Xiao L, Sun L (2017) Normoalbuminuric diabetic kidney disease. Front Med 11:310–318
Ekinci EI, Jerums G, Skene A, Crammer P, Power D, Cheong KY, Panagiotopoulos S, McNeil K, Baker ST, Fioretto P, Macisaac RJ (2013) Renal structure in normoalbuminuric and albuminuric patients with type 2 diabetes and impaired renal function. Diabetes Care 36:3620–3626
Acknowledgements
This study was supported by a Grant 81670662 from the National Natural Science Foundation of China, and a grand from National Research and Development Program (2016YFC1305502).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest that is relevant to this article.
Ethical approval
The ethics committee of West China Hospital approved this research. The study protocol was in compliance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
Additional informed consent was obtained from all individual participants for whom identifying information is included in this article.
Additional information
Managed by Massimo Federici.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhang, J., Wang, Y., Gurung, P. et al. The relationship between the thickness of glomerular basement membrane and renal outcomes in patients with diabetic nephropathy. Acta Diabetol 55, 669–679 (2018). https://doi.org/10.1007/s00592-018-1128-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-018-1128-9