Abstract
Background
Balloon enteroscopy-assisted endoscopic retrograde cholangiopancreatography (BE-ERCP) has been reported to be effective for patients with surgically altered gastrointestinal anatomy. However, selective biliary cannulation remains difficult in BE-ERCP. We examined the usefulness of a modified double-guidewire technique using an uneven double lumen cannula (the uneven method) for BE-ERCP in patients with surgically altered gastrointestinal anatomy.
Methods
To clarify the usefulness of the uneven method for selective biliary cannulation in BE-ERCP in comparison to the pancreatic guidewire (PGW) method, 40 patients with surgically altered gastrointestinal anatomy who underwent BE-ERCP with successful placement of a guidewire in the pancreatic duct were evaluated. The uneven method was used in 18 cases (uneven group) and the PGW method was used in the remaining 22 cases (PGW group).
Results
The technical success rate of biliary cannulation was higher in the uneven group than in the PGW group (83.3 vs. 59.0%; P = 0.165). In addition, the time to biliary cannulation were significantly shorter in the uneven group than in the PGW group (6 vs. 18 min; P = 0.004; respectively). In the PGW group, post-ERCP pancreatitis (PEP) occurred in 3 of 22 cases (13.6%). No adverse events, including PEP, occurred in the uneven group.
Conclusions
The uneven method may be a useful option of selective biliary cannulation in BE-ERCP for the patients with surgically altered gastrointestinal anatomy.





Similar content being viewed by others
References
Ishii K, Itoi T, Tonozuka R, Itokawa F, Sofuni A, Tsuchiya T et al (2016) Balloon enteroscopy-assisted ERCP in patients with Roux-en-Y gastrectomy and intact papillae (with videos). Gastrointest Endosc 83(2):37786.e6
Itoi T, Ishii K, Sofuni A, Itokawa F, Tsuchiya T, Kurihara T et al (2010) Single-balloon enteroscopy-assisted ERCP in patients with Billroth II gastrectomy or Roux-en-Y anastomosis (with video). Am J Gastroenterol 105(1):93–99
Nakai Y, Kogure H, Yamada A, Isayama H, Koike K (2018) Endoscopic management of bile duct stones in patients with surgically altered anatomy. Dig Endosc 30(Suppl 1):67–74
Yane K, Hayashi T, Katanuma A (2018) Successful emergency endoscopic drainage for afferent limb syndrome-induced severe acute cholangitis in a patient with altered Roux-en Y anatomy. Dig Endosc 30(6):802–803
Dumonceau JM, Deviere J, Cremer M (1998) A new method of achieving deep cannulation of the common bile duct during endoscopic retrograde cholangiopancreatography. Endoscopy 30(7):S80
Draganov P, Devonshire DA, Cunningham JT (2005) A new technique to assist in difficult bile duct cannulation at the time of endoscopic retrograde cholangiopancreatography. JSLS 9(2):218–221
Gronroos JM, Vihervaara H, Gullichsen R, Laine S, Karvonen J, Salminen P (2011) Double-guidewire-assisted biliary cannulation: experiences from a single tertiary referral center. Surg Endosc 25(5):1599–1602
Herreros de Tejada A, Calleja JL, Diaz G, Pertejo V, Espinel J, Cacho G et al (2009) Double-guidewire technique for difficult bile duct cannulation: a multicenter randomized, controlled trial. Gastrointest Endosc 70(4):700–709
Ito K, Fujita N, Noda Y, Kobayashi G, Obana T, Horaguchi J et al (2008) Pancreatic guidewire placement for achieving selective biliary cannulation during endoscopic retrograde cholangio-pancreatography. World J Gastroenterol 14(36):5595–5600 discussion 9
Ito K, Horaguchi J, Fujita N, Noda Y, Kobayashi G, Koshita S et al (2014) Clinical usefulness of double-guidewire technique for difficult biliary cannulation in endoscopic retrograde cholangiopancreatography. Dig Endosc 26(3):442–449
Maeda S, Hayashi H, Hosokawa O, Dohden K, Hattori M, Morita M et al (2003) Prospective randomized pilot trial of selective biliary cannulation using pancreatic guide-wire placement. Endoscopy 35(9):721–724
Sasahira N, Kawakami H, Isayama H, Uchino R, Nakai Y, Ito Y et al (2015) Early use of double-guidewire technique to facilitate selective bile duct cannulation: the multicenter randomized controlled EDUCATION trial. Endoscopy 47(5):421–429
Tanaka R, Itoi T, Sofuni A, Itokawa F, Kurihara T, Tsuchiya T et al (2013) Is the double-guidewire technique superior to the pancreatic duct guidewire technique in cases of pancreatic duct opacification? J Gastroenterol Hepatol 28(11):1787–1793
Xinopoulos D, Bassioukas SP, Kypreos D, Korkolis D, Scorilas A, Mavridis K et al (2011) Pancreatic duct guidewire placement for biliary cannulation in a single-session therapeutic ERCP. World J Gastroenterol 17(15):1989–1995
Takenaka M, Arisaka Y, Sakai A, Kobayashi T, Shiomi H, Masuda A et al (2018) A novel biliary cannulation method for difficult cannulation cases using a unique, uneven, double-lumen cannula (Uneven method). Endoscopy 50(8):E229–E230
Shimatani M, Takaoka M, Okazaki K (2018) Tips for endoscopic stone extraction using new short-type double balloon endoscope for common bile duct stones in patients with surgically altered gastrointestinal anatomy. Dig Endosc 30(1):130–131
Takenaka M, Yamao K, Kudo M (2018) A novel method of biliary cannulation for patients with Roux-en-Y anastomosis using a unique, uneven, double lumen cannula (Uneven method). Dig Endosc 30(6):808–809
Takenaka M, Minaga K, Kudo M (2018) Cannulation method for intradiverticular papilla with long oral protrusion using biopsy forceps for axis alignment. Dig Endosc 30(5):700–701
Cotton PB, Burney PG, Mason RR (1979) Transnasal bile duct catheterisation after endoscopic sphincterotomy: method for biliary drainage, perfusion, and sequential cholangiography. Gut 20(4):285–287
Dumonceau JM, Andriulli A, Elmunzer BJ, Mariani A, Meister T, Deviere J et al (2014) Prophylaxis of post-ERCP pancreatitis: european Society of Gastrointestinal Endoscopy (ESGE) guideline—updated June 2014. Endoscopy 46(9):799–815
Nakai Y, Isayama H, Sasahira N, Kogure H, Sasaki T, Yamamoto N et al (2015) Risk factors for post-ERCP pancreatitis in wire-guided cannulation for therapeutic biliary ERCP. Gastrointest Endosc 81(1):119–126
Author information
Authors and Affiliations
Contributions
MT: manuscript drafting, study conception and design, performing ERCP. KM, KK, KY, TY, RI, AO, TY, AN, and SO: performing ERCP and contribution to writing and revising the manuscript. YC: performing statistical analysis of data. YK, TS, TW, NNi, CK, SJ, and TL: contribution to writing and revising the manuscript. MK: Final approvement of submission
Corresponding author
Ethics declarations
Disclosures
Mamoru Takenaka, Kosuke Minaga, Ken Kamata, Kentaro Yamao, Tomoe Yoshikawa, Rei Ishikawa, Ayana Okamoto, Tomohiro Yamazaki, Atsushi Nakai, Shunsuke Omoto, Yoriaki Komeda, Toshiharu Sakurai, Tomohiro Watanabe, Naoshi Nishida, Yasutaka Chiba, Chang-Il Kwon, Seok Jeong, Tae Hoon Lee, and Masatoshi Kudo have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
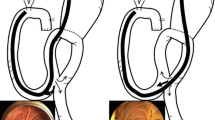
This video shows how to perform modified double-guidewire technique using an uneven double lumen cannula (uneven method) in patients with surgically altered gastrointestinal anatomy depending on the two situations (“axis matched” and “lumen-replaced”) in detail. Supplementary material 1 (MP4 227604 kb)
Rights and permissions
About this article
Cite this article
Takenaka, M., Minaga, K., Kamata, K. et al. Efficacy of a modified double-guidewire technique using an uneven double lumen cannula (uneven method) in patients with surgically altered gastrointestinal anatomy (with video). Surg Endosc 34, 1432–1441 (2020). https://doi.org/10.1007/s00464-019-07228-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07228-5