Abstract
Purpose
To compare the effect of high-intensity aerobic (AER), resistance (RES), and combined (COMB: RES + AER) exercise, on interstitial glucose (IG) variability and skeletal muscle signalling pathways in type 1 diabetes (T1D).
Methods
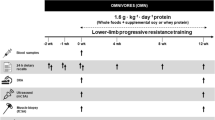
T1D participants (6 M/6F) wore a flash glucose monitoring system in four randomized sessions: one control (CONT), and one AER, RES and COMB (40 min each). Mean amplitude of glycemic excursions (MAGE), standard deviation (SD) and coefficient variation (CV) of IG were used to compare the 24 h post-exercise IG variability. Blood and muscle samples were collected to compare exercise-induced systemic and muscle signalling responses related to metabolic, growth and inflammatory adaptations.
Results
Both RES and COMB decreased the 24 h MAGE compared to CONT; additionally, COMB decreased the 24 h SD and CV. In the 6–12 h post-exercise, all exercise modalities reduced the IG CV while SD decreased only after COMB. Both AER and COMB stimulated the PGC-1α mRNA expression and promoted the splicing of IGF-1Ea variant, while Akt and p38MAPK phosphorylation increased only after RES and COMB. Additionally, COMB enhanced eEF2 activation and RES increased myogenin and MRF4 mRNA expression. Blood lactate and glycerol levels and muscle IL-6, TNF-α, and MCP-1 mRNAs increased after all exercise sessions, while serum CK and LDH level did not change.
Conclusion
COMB is more effective in reducing IG fluctuations compared to single-mode AER or RES exercise. Moreover, COMB simultaneously activates muscle signalling pathways involved in substrate metabolism and anabolic adaptations, which can help to improve glycaemic control and maintain muscle health in T1D.








Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
- AER:
-
Aerobic
- Akt:
-
AKT serine/threonine kinase 1
- AMPK:
-
Protein kinase AMP-activated catalytic subunit alpha 1
- ANOVA:
-
Analysis of variance
- ATP:
-
Adenosine triphosphate
- B2M:
-
Beta-2-microglobulin
- BMI:
-
Body mass index
- CK:
-
Creatine kinase
- COMB:
-
Combined
- CONT:
-
Control
- CV:
-
Coefficient of variation
- DEXA:
-
Dual-energy X-ray absorptiometry
- eEF2:
-
Eukaryotic translation elongation factor 2
- ERK1/2:
-
Extracellular signal-regulated protein kinases 1 and 2
- FGM:
-
Flash interstitial glucose monitoring
- GAPDH:
-
Glyceraldehyde-3-phosphate dehydrogenase
- GLUT4:
-
Solute carrier family 2, facilitated glucose transporter member 4
- GPAQ:
-
Global Physical Activity Questionnaire
- HbA1c:
-
Glycated hemoglobin
- HR:
-
Heart rate
- HRR:
-
Heart rate reserve
- IG:
-
Interstitial glucose
- IGF-1:
-
Insulin-like growth factor 1
- IGF1R:
-
Insulin-like growth factor 1 Receptor
- IL-6:
-
Interleukin-6
- LDH:
-
Lactate dehydrogenase
- MAGE:
-
Mean amplitude of glycemic excursions
- MCP-1:
-
Monocyte chemoattractant protein 1/C–C motif chemokine 2
- MRF4:
-
Myogenic regulatory factor 4/Myogenic factor 6
- mRNA:
-
Messenger ribonucleic acid
- mTOR:
-
Mechanistic target of rapamycin kinase
- Myf5:
-
Myogenic factor 5
- MyoD:
-
Myogenic differentiation 1
- p38MAPK:
-
P38 map kinase
- PGC-1α:
-
Peroxisome proliferative activated receptor, gamma, coactivator 1 alpha
- PI3K:
-
Phosphatidylinositol-4,5-bisphosphate 3-kinase
- 1RM:
-
One-repetition maximum
- RES:
-
Resistance
- RT-PCR:
-
Real-time polymerase chain reaction
- SD:
-
Standard deviation
- T1D:
-
Type 1 diabetes
- TNF-α:
-
Tumor necrosis factor-alpha
References
Aksamitiene E, Hoek JB, Kholodenko B, Kiyatkin A (2007) Multi-strip Western blotting to increase quantitative data output. Electrophoresis 28(18):3163–3173. https://doi.org/10.1002/elps.200700002
Annibalini G, Bielli P, De Santi M, Agostini D, Guescini M, Sisti D, Contarelli S, Brandi G, Villarini A, Stocchi V, Sette C, Barbieri E (2016) MIR retroposon exonization promotes evolutionary variability and generates species-specific expression of IGF-1 splice variants. BBA - Gene Regulatory Mechanisms 1859:757–768
Bohn B, Herbst A, Pfeifer M, Krakow D, Zimny S, Kopp F, Melmer A, Steinacker JM, Holl RW, Initiative DPV (2015) Impact of physical activity on glycemic control and prevalence of cardiovascular risk factors in adults with type 1 diabetes: a cross-sectional multicenter study of 18,028 patients. Diabetes Care 38(8):1536–1543. https://doi.org/10.2337/dc15-0030
Bradford MM (1976) A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal Biochem 72(1–2):248–254. https://doi.org/10.1006/abio.1976.9999
Brownlee M (2005) The pathobiology of diabetic complications: a unifying mechanism. Diabetes 54(6):1615–1625. https://doi.org/10.2337/diabetes.54.6.1615
Chatzinikolaou A, Fatouros I, Petridou A, Jamurtas A, Avloniti A, Douroudos I, Mastorakos G, Lazaropoulou C, Papassotiriou I, Tournis S, Mitrakou A, Mougios V (2008) Adipose tissue lipolysis is upregulated in lean and obese men during acute resistance exercise. Diabetes Care 31(7):1397–1399. https://doi.org/10.2337/dc08-0072
Church TS, Blair SN, Cocreham S, Johannsen N, Johnson W, Kramer K, Mikus CR, Myers V, Nauta M, Rodarte RQ, Sparks L, Thompson A, Earnest CP (2010) Effects of aerobic and resistance training on hemoglobin A1c levels in patients with type 2 diabetes. JAMA 20:2253–2262
Coffey VG, Hawley JA (2007) The molecular bases of training adaptation. Sports Med 37(9):737–763. https://doi.org/10.2165/00007256-200737090-00001
Colberg SR, Sigal RJ, Yardley JE, Riddell MC, Dunstan DW, Dempsey PC, Horton ES, Castorino K, Tate DF (2016) Physical activity/exercise and diabetes: a position statement of the American Diabetes Association. Diabetes Care 39(11):2065–2079. https://doi.org/10.2337/dc16-1728
Coyle EF, González-Alonso J (2001) Cardiovascular drift during prolonged exercise: new perspectives. Exerc Sports Sci 29(2):88–92. https://doi.org/10.1097/00003677-200104000-00009
Egerman MA, Glass DJ (2014) Signaling pathways controlling skeletal muscle mass. Crit Rev Biochem Mol Biol 49(1):59–68. https://doi.org/10.3109/10409238.2013.857291
Farinha JB, Krause M, Rodrigues-Krause J, Reischak-Oliveira A (2017) Exercise for type 1 diabetes mellitus management: general considerations and new directions. Med Hypotheses 104:147–153. https://doi.org/10.1016/j.mehy.2017.05.033
Friedmann-Bette B, Schwartz FR, Eckhardt H, Billeter R, Bonaterra G, Kinscherf R (2011) Similar changes of gene expression in human skeletal muscle after resistance exercise and multiple fine needle biopsies. J Appl Physiol 112(2):289–295
Fyfe JJ, Bishop DJ, Stepto NK (2014) Interference between concurrent resistance and endurance exercise: molecular bases and the role of individual training variables. Sports Med 44(6):743–762. https://doi.org/10.1007/s40279-014-0162-1
Gomez AM, Gomez C, Aschner P, Veloza A, Muñoz O, Rubio C, Vallejo S (2015) Effects of performing morning versus afternoon exercise on glycemic control and hypoglycemia frequency in type 1 diabetes patients on sensor-augmented insulin pump therapy. J Diabetes Sci Technol 9(3):619–624. https://doi.org/10.1177/1932296814566233
Gorst C, Kwok CS, Aslam S, Buchan I, Kontopantelis E, Myint PK, Heatlie G, Loke Y, Rutter MK, Mamas MA (2015) Long-term glycemic variability and risk of adverse outcomes: A systematic review and meta-analysis. Diabetes Care 38(12):2354–2369. https://doi.org/10.2337/dc15-1188
Goto K, Ishii N, Sugihara S, Yoshioka T, Takamatsu K (2007) Effects of resistance exercise on lipolysis during subsequent submaximal exercise. Med Sci Sports Exerc 39(2):308–315. https://doi.org/10.1249/01.mss.0000246992.33482.cb
Hill NR, Oliver NS, Choudhary P, Levy JC, Hindmarsh P, Matthews DR (2011) Normal reference range for mean tissue glucose and glycemic variability derived from continuous glucose monitoring for participants without diabetes in different ethnic groups. Diabetes Technol Ther 13(9):921–928. https://doi.org/10.1089/dia.2010.0247
Jäger S, Handschin C, Pierre J, Soiegelman J (2007) AMP-activated protein kinase (AMPK) action in skeletal muscle via direct phosphorylation of PGC-1α. Proc Natl Acad Sci USA 104(29):12017–12022. https://doi.org/10.1073/pnas.0705070104
Karvonen MJ, Kentala E, Mustala O (1957) The effects of training on heart rate; a longitudinal study. Ann Med Exp Biol Fenn 35(3):307–315
Krause MP, Riddell MC, Hawke TJ (2011) Effects of type 1 diabetes mellitus on skeletal muscle: clinical observations and physiological mechanisms. Pediatr Diabetes 12(4):345–364. https://doi.org/10.1111/j.1399-5448.2010.00699.x
Mancini G, Berioli MG, Santi E, Rogari F, Toni G, Tascini G, Crispoldi R, Ceccarini G, Esposito S (2018) Flash glucose monitoring: a review of the literature with a special focus on type 1 diabetes. Nutrients. https://doi.org/10.3390/nu10080992
McCarthy MM, Funk M, Grey M (2016) Cardiovascular health in adults with type 1 diabetes. Prev Med 91:138–143. https://doi.org/10.1016/j.ypmed.2016.08.019
Minnock D, Krause M, Le Roux CW, De Vito G (2019) Effects of acute exercise on glucose control in type 1 diabetes: a systematic review. Transl Sports Med 2(2):49–57. https://doi.org/10.1002/tsm2.64
Monaco CMF, Perry CGR, Hawke TJ (2017) Diabetic myopathy: current molecular understanding of this novel neuromuscular disorder. Curr Opin Neurol 30(5):545–552. https://doi.org/10.1097/WCO.0000000000000479
Montain SJ, Coyle EF (1992) Fluid ingestion during exercise increases skin blood flow independent of increases in blood volume. J Appl Physiol. 73(3):903–910
Nambam B, Schatz D (2018) Growth hormone and insulin-like growth factor-I axis in type 1 diabetes. Growth Horm IGF Res 38:49–52. https://doi.org/10.1016/j.ghir.2017.12.005
O'Neill BT, Lauritzen HP, Hirshman MF, Smyth G, Goodyear LJ, Kahn CR (2015) Differential role of insulin/IGF-1 receptor signaling in muscle growth and glucose homeostasis. Cell Rep 11(8):1220–1235. https://doi.org/10.1016/j.celrep.2015.04.037
Reddy R, Wittenberg A, Castle JR, El Youssef J, Winters-Stone K, Gillingham M, Jacobs PG (2019) Effect of aerobic and resistance exercise on glycemic control in adults with type 1 diabetes. Can J Diabetes. https://doi.org/10.1016/j.jcjd.2018.08.193
Riddell M, Perkins BA (2009) Exercise and glucose metabolism in persons with diabetes mellitus: perspectives on the role for continuous glucose monitoring. J Diabetes Sci Technol 3(4):914–923. https://doi.org/10.1177/193229680900300439
Riddell MC, Gallen IW, Smart CE, Taplin CE, Adolfsson P, Lumb AN, Kowalski A, Rabasa-Lhoret R, McCrimmon RJ, Hume C, Annan F, Fournier PA, Graham C, Bode B, Galassetti P, Jones TW, Millán IS, Heise T, Peters AL, Petz A, Laffel LM (2017) Exercise management in type 1 diabetes: a consensus statement. Lancet Diabetes Endocrinol 5(5):377–390. https://doi.org/10.1016/S2213-8587(17)30014-1
Röhling M, Herder C, Stemper T, Müssig K (2016) Influence of acute and chronic exercise on glucose uptake. J Diabetes Res. https://doi.org/10.1155/2016/2868652
Rose AJ, Broholm C, Kiillerich K, Finn SG, Proud CG, Rider MH, Richter EA, Kiens B (2005) Exercise rapidly increases eukaryotic elongation factor 2 phosphorylation in skeletal muscle of men: exercise and skeletal muscle eEF2. J Physiol 569(1):223–228. https://doi.org/10.1113/jphysiol.2005.097154
Sawka MN, Burke LM, Eichner ER, Maughan RJ, Montain SJ, Stachenfeld NS (2007) American College of Sports Medicine position stand: exercise and fluid replacement. Med Sci Sports Exerc 39:377–390. https://doi.org/10.1249/mss.0b013e31802ca597
Summermatter S, Santos G, Pérez-Schindler J, Handschin C (2013) Skeletal muscle PGC-1α controls whole-body lactate homeostasis through estrogen-related receptor α-dependent activation of LDH B and repression of LDH A. Proc Natl Acad Sci USA 110(21):8738–8743. https://doi.org/10.1073/pnas.1212976110
Turner D, Luzio S, Kilduff LP, Gray BJ, Dunseath G, Bain SC, Campbell MD, West DJ, Bracken RM (2014) Reductions in resistance exercise-induced hyperglycaemic episodes are associated with circulating interleukin-6 in type 1 diabetes. Diabetes Med 31(8):1009–1013. https://doi.org/10.1111/dme.12462
Turner D, Gray BJ, Luzio S, Dunseath G, Bain SC, Hanley S, Richards A, Rhydderch DC, Ayles M, Kilduff LP, Campbell MD, West DJ, Bracken RM (2016) Similar magnitude of post-exercise hyperglycemia despite manipulating resistance exercise intensity in type 1 diabetes individuals. Scand J Med Sci Sports 26(4):404–412. https://doi.org/10.1111/sms.12472
Vassilakos G, Lei H, Yang Y, Puglise J, Matheny M, Durzynska J, Ozery M, Bennett K, Spradlin R, Bonanno H, Park S, Ahima RS, Barton ER (2019) Deletion of muscle IGF-I transiently impairs growth and progressively disrupts glucose homeostasis in male mice. FASEB J 33(1):181–194. https://doi.org/10.1096/fj.201800459R
Yardley JE, Kenny GP, Perkins BA, Riddell MC, Malcolm J, Boulay P, Khandwala F, Sigal RJ (2012) Effects of performing resistance exercise before versus after aerobic exercise on glycemia in type 1 diabetes. Diabetes Care 35(4):669–675. https://doi.org/10.2337/dc11-1844
Yardley JE, Kenny GP, Perkins BA, Riddell MC, Balaa N, Malcolm J, Boulay P, Khandwala F, Sigal RJ (2013) Resistance versus aerobic exercise acute effects on glycemia in type 1 diabetes. Diabetes Care 36(3):537–542. https://doi.org/10.2337/dc12-0963
Zaccardi F, Di Stefano P, Busetto E, Federici MO, Manto A, Infusino F, Lanza GA, Pitocco D, Ghirlanda G (2008) Group of signs: a new method to evaluate glycemic variability. J Diabetes Sci Technol 2(6):1061–1065. https://doi.org/10.1177/193229680800200614
Acknowledgements
Mr. Minnock was supported in this research by the Irish Research Council, where he is the recipient of the IRC EBS fellowship award (EBPPG/2016/278). All sensors and FGM systems were generously provided by Innovation Zed Ltd, Dublin, Ireland. We also thank Dr. Patricia Martins Bock (Hospital de Clínicas de Porto Alegre) for the advice on the glucose variability analysis.
Funding
This research was supported by the Irish Research Council where Dean Minnock is the recipient of the IRC EBS fellowship award (EBPPG/2016/278).
Author information
Authors and Affiliations
Contributions
DM and GDV conceived and designed the study. DM, GA and GDV analysed the data and drafted the manuscript. DM, CWLR, MK and GDV designed, prescribed and supervised the exercise sessions and contributed to the drafting of the manuscript. DM, SC, RS, GV and GDV collected, processed and stored the biological samples. GA, SC, RS, GV and EB performed the RT-PCR experiments and western blotting. CWLR, MK, VS, EB, and GDV provided overall direction to the project and revised the manuscript. All authors contributed to manuscript revision, read and approved the submitted version.
Corresponding author
Ethics declarations
Conflict of interest
Innovation Zed Ltd, are a medical technology company based in Dublin, Ireland developing technologies for self-injection devices and declares no conflict of interest or self-gain from this study. This study has no other potential conflicts of interest relevant to this study.
Ethical approval
This study was approved by the Human Research Ethics Committee of University College Dublin (Application ID-LS-16-67-Minnock-DeVito).
Consent to participate
All participants gave their written, informed consent to participate in the study prior to its commencement.
Consent for publication
All participants gave their written, informed consent for publication.
Additional information
Communicated by Philip D Chilibeck.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Minnock, D., Annibalini, G., Le Roux, C.W. et al. Effects of acute aerobic, resistance and combined exercises on 24-h glucose variability and skeletal muscle signalling responses in type 1 diabetics. Eur J Appl Physiol 120, 2677–2691 (2020). https://doi.org/10.1007/s00421-020-04491-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-020-04491-6