Abstract
Objective
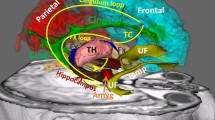
The findings of resting-state functional MRI studies have suggested that abnormal functional integration between interconnected cortical networks characterises the brain of patients with migraine. The aim of this study was to investigate the functional connectivity between the hypothalamus, brainstem, considered as the migraine generator, and the following areas/networks that are reportedly involved in the pathophysiology of migraine: default mode network (DMN), executive control network, dorsal attention system, and primary and dorsoventral visual networks.
Methods
Twenty patients with chronic migraine (CM) without medication overuse and 20 healthy controls (HCs) were prospectively recruited. All study participants underwent 3-T MRI scans using a 7.5-min resting-state protocol. Using a seed-based approach, we performed a ROI-to-ROI analysis selecting the hypothalamus as the seed.
Results
Compared to HCs, patients with CM showed significantly increased neural connectivity between the hypothalamus and brain areas belonging to the DMN and dorsal visual network. We did not detect any connectivity abnormalities between the hypothalamus and the brainstem. The correlation analysis showed that the severity of the migraine headache was positively correlated with the connectivity strength of the hypothalamus and negatively with the connectivity strength of the medial prefrontal cortex, which belongs to the DMN.
Conclusion
These data provide evidence for hypothalamic involvement in large-scale reorganisation at the functional-network level in CM and in proportion with the perceived severity of the migraine pain.

Similar content being viewed by others
References
Haanes KA, Edvinsson L (2019) Pathophysiological mechanisms in migraine and the identification of new therapeutic targets. CNS Drugs. https://doi.org/10.1007/s40263-019-00630-6
Coppola G, Di Lorenzo C, Serrao M et al (2016) Pathophysiological targets for non-pharmacological treatment of migraine. Cephalalgia 36:1103–1111. https://doi.org/10.1177/0333102415620908
ICHD (2018) Headache classification committee of the international headache society (IHS) The International Classification of Headache disorders, 3rd edition. Cephalalgia 38:1–211. https://doi.org/10.1177/0333102417738202
May A (2017) Understanding migraine as a cycling brain syndrome: reviewing the evidence from functional imaging. Neurol Sci 38:125–130. https://doi.org/10.1007/s10072-017-2866-0
Schulte LH, Allers A, May A (2017) Hypothalamus as a mediator of chronic migraine. Neurology 88:2011–2016. https://doi.org/10.1212/WNL.0000000000003963
Lerebours F, Boulanouar K, Barège M et al (2019) Functional connectivity of hypothalamus in chronic migraine with medication overuse. Cephalalgia. https://doi.org/10.1177/0333102419833087
Lee MJ, Park BY, Cho S et al (2019) Increased connectivity of pain matrix in chronic migraine: a resting-state functional MRI study. J Headache Pain 20:29. https://doi.org/10.1186/s10194-019-0986-z
Coppola G, Di Renzo A, Petolicchio B et al (2019) Aberrant interactions of cortical networks in chronic migraine. Neurology 92:e2550–e2558. https://doi.org/10.1212/wnl.0000000000007577
Weiller C, May A, Limmroth V et al (1995) Brain stem activation in spontaneous human migraine attacks. Nat Med 1:658–660
Bahra A, Matharu MS, Buchel C et al (2001) Brainstem activation specific to migraine headache. Lancet 357:1016–1017
Stankewitz A, May A (2011) Increased limbic and brainstem activity during migraine attacks following olfactory stimulation. Neurology 77:476–482
Olesen J, Bes A, Kunkel R, Lance JW, Nappi G, Pfaffenrath V, Rose FC, Schoenberg BS, Soyka D, Tfelt-Hansen P, Welch KMA (2013) The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia 33:629–808. doi: 10.1177/0333102413485658.
Coppola G, Petolicchio B, Di Renzo A et al (2017) Cerebral gray matter volume in patients with chronic migraine: correlations with clinical features. J Headache Pain 18:115. https://doi.org/10.1186/s10194-017-0825-z
Talairach J, Tournoux P (1988) Co-planar stereotaxic atlas of the human brain. Georg Thieme, Thieme
Whitfield-Gabrieli S, Nieto-Castanon A (2012) Conn: a functional connectivity toolbox for correlated and anticorrelated brain networks. Brain Connect 2:125–141. https://doi.org/10.1089/brain.2012.0073
Pujol J, Macià D, Garcia-Fontanals A et al (2014) The contribution of sensory system functional connectivity reduction to clinical pain in fibromyalgia. PAIN® 155:1492–1503. https://doi.org/10.1016/J.PAIN.2014.04.028
Shen W, Tu Y, Gollub RL et al (2019) Visual network alterations in brain functional connectivity in chronic low back pain: a resting state functional connectivity and machine learning study. NeuroImage Clin 22:101775. https://doi.org/10.1016/j.nicl.2019.101775
Messina R, Rocca MA, Colombo B et al (2018) Gray matter volume modifications in migraine. Neurology 91:e280–e292. https://doi.org/10.1212/WNL.0000000000005819
Baroncini M, Jissendi P, Balland E et al (2012) MRI atlas of the human hypothalamus. Neuroimage 59:168–180. https://doi.org/10.1016/j.neuroimage.2011.07.013
Sakai Y, Dobson C, Diksic M et al (2008) Sumatriptan normalizes the migraine attack-related increase in brain serotonin synthesis. Neurology 70:431–439. https://doi.org/10.1212/01.wnl.0000299095.65331.6f
Matharu MS, Bartsch T, Ward N et al (2004) Central neuromodulation in chronic migraine patients with suboccipital stimulators: a PET study. Brain 127:220–230. https://doi.org/10.1093/brain/awh022
Aurora SK, Barrodale PM, Tipton RL, Khodavirdi A (2007) Brainstem dysfunction in chronic migraine as evidenced by neurophysiological and positron emission tomography studies. Headache 47:996–1003
Denuelle M, Fabre N, Payoux P et al (2007) Hypothalamic activation in spontaneous migraine attacks. Headache 47:1418–1426
Maniyar F, Sprenger T, Monteith T et al (2014) Brain activations in the premonitory phase of nitroglycerin-triggered migraine attacks. Brain 137:232–241
Schulte LH, May A (2016) The migraine generator revisited: continuous scanning of the migraine cycle over 30 days and three spontaneous attacks. Brain 139:1987–1993. https://doi.org/10.1093/brain/aww097
Raichle M, MacLeod AM, Snyder AZ et al (2001) A default mode of brain function. Proc Natl Acad Sci USA 98:676–682
Gazzaley A, Nobre AC (2012) Top-down modulation: bridging selective attention and working memory. Trends Cogn Sci 16:129–135. https://doi.org/10.1016/j.tics.2011.11.014
Heinzel S, Lorenz RC, Duong Q-L et al (2017) Prefrontal-parietal effective connectivity during working memory in older adults. Neurobiol Aging 57:18–27. https://doi.org/10.1016/j.neurobiolaging.2017.05.005
Galletti C, Fattori P (2018) The dorsal visual stream revisited: Stable circuits or dynamic pathways? Cortex 98:203–217. https://doi.org/10.1016/j.cortex.2017.01.009
Corbetta M, Shulman GL (2002) Control of goal-directed and stimulus-driven attention in the brain. Nat Rev 3:201–215
Vossel S, Geng JJ, Fink GR (2014) Dorsal and ventral attention systems. Neuroscientist 20:150–159. https://doi.org/10.1177/1073858413494269
Mishkin M, Ungerleider LG, Macko KA (1983) Object vision and spatial vision: two cortical pathways. Trends Neurosci 6:414–417. https://doi.org/10.1016/0166-2236(83)90190-X
Bekrater-Bodmann R, Foell J, Diers M et al (2014) The importance of synchrony and temporal order of visual and tactile input for illusory limb ownership experiences—an fMRI study applying virtual reality. PLoS ONE 9:e87013. https://doi.org/10.1371/journal.pone.0087013
Boulloche N, Denuelle M, Payoux P et al (2010) Photophobia in migraine: an interictal PET study of cortical hyperexcitability and its modulation by pain. J Neurol Neurosurg Psychiatry 81:978–984
Mehnert J, Bader D, Nolte G, May A (2019) Visual input drives increased occipital responsiveness and harmonized oscillations in multiple cortical areas in migraineurs. NeuroImage Clin 23:101815. https://doi.org/10.1016/j.nicl.2019.101815
Razavi BM, Hosseinzadeh H (2017) A review of the role of orexin system in pain modulation. Biomed Pharmacother 90:187–193. https://doi.org/10.1016/j.biopha.2017.03.053
Roohbakhsh A, Alavi MS, Azhdari-Zarmehri H (2018) The orexinergic (hypocretin) system and nociception: an update to supraspinal mechanisms. Curr Med Chem 25:3917–3929. https://doi.org/10.2174/0929867324666170529072554
Jin J, Chen Q, Qiao Q et al (2016) Orexin neurons in the lateral hypothalamus project to the medial prefrontal cortex with a rostro-caudal gradient. Neurosci Lett 621:9–14. https://doi.org/10.1016/j.neulet.2016.04.002
Wiech K, Ploner M, Tracey I (2008) Neurocognitive aspects of pain perception. Trends Cogn Sci 12:306–313. https://doi.org/10.1016/j.tics.2008.05.005
Tu Y, Jung M, Gollub RL et al (2019) Abnormal medial prefrontal cortex functional connectivity and its association with clinical symptoms in chronic low back pain. Pain 160:1308–1318. https://doi.org/10.1097/j.pain.0000000000001507
Schreiber KL, Loggia ML, Kim J et al (2017) Painful after-sensations in fibromyalgia are linked to catastrophizing and differences in brain response in the medial temporal lobe. J Pain 18:855–867. https://doi.org/10.1016/j.jpain.2017.02.437
James MH, Campbell EJ, Dayas CV (2017) Role of the orexin/hypocretin system in stress-related psychiatric disorders. Current topics in behavioral neurosciences. Springer, Cham, pp 197–219
Grafe LA, Eacret D, Luz S et al (2017) Orexin 2 receptor regulation of the hypothalamic–pituitary–adrenal (HPA) response to acute and repeated stress. Neuroscience 348:313–323. https://doi.org/10.1016/j.neuroscience.2017.02.038
Sarchielli P, Rainero I, Coppola F et al (2008) Involvement of corticotrophin-releasing factor and orexin-A in chronic migraine and medication-overuse headache: findings from cerebrospinal fluid. Cephalalgia 28:714–722. https://doi.org/10.1111/j.1468-2982.2008.01566.x
Rainero I, Ferrero M, Rubino E et al (2006) Endocrine function is altered in chronic migraine patients with medication-overuse. Headache J Head Face Pain 46:597–603. https://doi.org/10.1111/j.1526-4610.2006.00409.x
Siva ZO, Uluduz D, Keskin FE et al (2018) Determinants of glucose metabolism and the role of NPY in the progression of insulin resistance in chronic migraine. Cephalalgia 38:1773–1781. https://doi.org/10.1177/0333102417748928
Acknowledgements
The contribution of the G.B. Bietti Foundation in this paper was supported by the Italian Ministry of Health and the Fondazione Roma.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no financial or other conflicts of interest.
Ethical standard
The study was approved by ethical review board of the Faculty of Medicine, University of Rome, Italy. Written informed consent was obtained from all participants in this study.
Rights and permissions
About this article
Cite this article
Coppola, G., Di Renzo, A., Petolicchio, B. et al. Increased neural connectivity between the hypothalamus and cortical resting-state functional networks in chronic migraine. J Neurol 267, 185–191 (2020). https://doi.org/10.1007/s00415-019-09571-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-019-09571-y