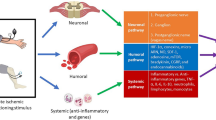
Abstract
Reperfusion injury is a complex process involving several cell types (endothelial cells, neutrophils, and cardiomyocytes), soluble proinflammatory mediators, oxidants, ionic and metabolic dyshomeostasis, and cellular and molecular signals. These participants in the pathobiology of reperfusion injury are not mutually exclusive. Some of these events take place during the very early moments of reperfusion, while others, seemingly triggered in part by the early events, are activated within a later timeframe. Postconditioning is a series of brief mechanical interruptions of reperfusion following a specific prescribed algorithm applied at the very onset of reperfusion. This algorithm lasts only from 1 to 3 minutes depending on species. Although associated with re–occlusion of the coronary artery or re–imposition of hypoxia in cell culture, the reference to ischemia has been dropped. Postconditioning has been observed to reduce infarct size and apoptosis as the “end games” in myocardial therapeutics; salvage of infarct size was similar to that achieved by the gold standard of protection, ischemic preconditioning. The cardioprotection was also associated with a reduction in: endothelial cell activation and dysfunction, tissue superoxide anion generation, neutrophil activation and accumulation in reperfused myocardium, microvascular injury, tissue edema, intracellular and mitochondrial calcium accumulation. Postconditioning sets in motion triggers and signals that are functionally related to reduced cell death. Adenosine has been implicated in the cardioprotection of postconditioning, as has e–NOS, nitric oxide and guanylyl cyclase, opening of KATP channels and closing of the mitochondrial permeability transition pore. Cardioprotection by postconditioning has also been associated with the activation of intracellular survival pathways such as ERK1/2 and PI3 kinase – Akt pathways. Other pathways have yet to be identified. Although many of the pathways involved in postconditioning have also been identified in ischemic preconditioning, some may not be involved in preconditioning (ERK1/2). The timing of action of these pathways and other mediators of protection in postconditioning differs from that of preconditioning. In contrast to preconditioning, which requires a foreknowledge of the ischemic event, postconditioning can be applied at the onset of reperfusion at the point of clinical service, i.e. angioplasty, cardiac surgery, transplantation.
Similar content being viewed by others
References
Alker KJ, Bellows SD, Kloner RA (1996) Stuttering reperfusion of ischemic myocardium does not exacerbate myocardial infarction: Evidence against lethal cell reperfusion injury in the rabbit. J Thrombosis Thrombolysis 3:185–188
Allen DG, Xiao X-H (2003) Role of the cardiac Na+/H+ exchanger during ischemia and reperfusion. Cardiovasc Res 57:934–941
Ambrosio G, Zweier JL, Flaherty JT (1991) The relationship between oxygen radical generation and impairment of myocardial energy metabolism following post-ischemic reperfusion. J Mol Cell Cardiol 23:1359–1374
Argaud L, Gateau-Roesch O, Raisky O, Loufouat J, Robert D, Ovize M (2005) Post-conditioning inhibits mitochondrial permeability transition. Circulation 111:194–197
Balligand JL, Kobzik L (1995) Nitric oxide-dependent parasympathetic signaling is due to activation of constitutive endothelial (type III) nitric oxide synthase in cardiac myocytes. J Biol Chem 270:14582–14586
Baxter GF (2002) The neutrophil as a mediator of myocardial ischemia-reperfusion injury: time to move on. Basic Res Cardiol 97:268–275
Baxter GF, Yellon DM (2003) Current trends and controversies in ischemiareperfusion research. Meeting report of the Hatter Institute 3rd International Workshop on Cardioprotection. Basic Res Cardiol 98:133–136
Bolli R, Becker L, Gross G, Mentzer RM, Jr., Balshaw D, Lathrop DA (2004) Myocardial protection at a crossroads: The need for translation into clinical therapy. Circ Res 95:125–134
Braunwald E, Kloner RA (1985) Myocardial reperfusion: a double-edged sword? J Clin Invest 76:1713–1719
Buckberg GD (1986) Studies of controlled reperfusion after ischemia: I. When is cardiac muscle damaged irreversibly? J Thorac Cardiovasc Surg 92:483–487
Budde JM, Velez DA, Zhao Z, Clark KL, Morris CD, Muraki S, Guyton RA, Vinten-Johansen J (2000) Comparative study of AMP579 and adenosine in inhibition of neutrophil-mediated vascular and myocardial injury during 24 h of reperfusion. Cardiovasc Res 47:294–305
Cooley DA, Ruel GJ, Wukasch DC (1972) Ischemic contracture of the heart: “Stone Heart”. Am J Cardiol 29:575–577
Crompton M (1999) The mitochondrial permeability transition pore and its role in cell death. Biochem J 341:233–249
Cronstein BN, Kramer SB, Weissmann G, Hirschhorn R (1983) Adenosine: a physiological modulator of superoxide anion generation by human neutrophils. J Exp Med 158:1160–1177
Cronstein BN, Levin RI, Belanoff J, Weissmann G, Hirschhorn R (1986) Adenosine: an endogenous inhibitor of neutrophil-mediated injury to endothelial cells. J Clin Invest 78:760–770
Cronstein BN, Levin RI, Philips M, Hirschhorn R, Abramson SB, Weissmann G (1992) Neutrophil adherence to endothelium is enhanced via adenosine A1 receptors and inhibited via adenosine A2 receptors. J Immunol 148:2201–2206
Cronstein BN, Rosenstein ED, Kramer SB, Weissmann G, Hirschhorn R (1985) Adenosine: a physiologic modulator of superoxide anion generation by human neutrophils. Adenosine acts via an A2 receptor on human neutrophils. J Immunol 135:1366–1371
Darling C, Maynard M, Przyklenk K (2004) Post-conditioning via stuttering reperfusion limits myocardial infarct size in rabbit heart. Acad Emerg Med 11:536-a
Davenpeck KL, Gauthier TW, Albertine KH, Lefer AM (1994) Role of P-selectin in microvascular leukocyte-endothelial interaction in splanchnic ischemiareperfusion. Am J Physiol (Heart Circ Physiol) 267:H622–H630
Deguchi H, Takeya H, Urano H, Gabazza EC, Zhou H, Suzuki K (1998) Adenosine Regulates Tissue Factor Expression on Endothelial Cells. Thromb Res 91:57–64
Diaz RJ, Wilson GJ (2004) Modifying the .rst minute of reperfusion: potential for myocardial salvage. Cardiovasc Res 62:4–6
Duilio C, Ambrosio G, Kuppusamy P, DiPaula A, Becker LC, Zweier JL (2001) Neutrophils are primary source of O2 radicals during reperfusion after prolonged myocardial ischemia. Am J Physiol (Heart Circ Physiol) 280:H2649–H2657
Follette DM, Fey K, Buckberg GD, Helly Jr JJ, Steed DL, Foglia RP, Maloney JV Jr (1981) Reducing postischemic damage by temporary modification of reperfusate calcium, potassium, pH, and osmolarity. J Thorac Cardiovasc Surg 82:221–238
Gabazza EC, Hayashi T, Ido M, Adachi Y, Suzuki K (2002) Adenosine inhibits thrombin-induced expression of tissue factor on endothelial cells by a nitric oxide-mediated mechanism. Clin Sci (Colch) 102:167–175
Galagudza M, Kurapeev D, Minasian S, Valen G, Vaage J (2004) Ischemic postconditioning: brief ischemia during reperfusion converts persistent ventricular fibrillation into regular rhythm. Eur J Cardio-thorac Surg 25:1006–1010
Garcia-Dorado D, Gonzalez MA, Barrabes JA, Ruiz-Meana M, Solares J, Lidon R-M, Blanco J, Puigfel Y, Piper HM, Soler-Soler J (1997) Prevention of ischemic rigor contracture during coronary occlusion by inhibition of Na+-H+ exchange. Cardiovasc Res 35:80–89
Griffiths EJ, Halestrap AP (1995) Mitochondrial non-specific pores remain closed during cardiac ischaemia, but open upon reperfusion. Biochem J 307:93–98
Gross GJ, Gumina RJ (2001) Cardioprotective effects of Na+/H+ exchange inhibitors. Drugs of the Future 26:253–260
Gumina RJ, Auchampach JA, Wang R, Buerger E, Eickmeier C, Moore J, Daemmgen J, Gross GJ (2000) Na+/H+ exchange inhibition-induced cardioprotection in dogs: effects on neutrophils versus cardiomyocytes. Am J Physiol (Heart Circ Physiol) 279:H1563–H1570
Guo J-P, Murohara T, Buerke M, Scalial R, Lefer AM (1996) Direct measurement of nitric oxide release from vascular endothelial cells. J Appl Physiol 81:774–779
Halestrap AP, Kerr PM, Javadov S, Woodfield KY (1998) Elucidating the molecular mechanism of the permeability transition pore and its role in reperfusion injury of the heart. Biochim Biophys Acta 1366:79–94
Halkos ME, Kerendi F, Corvera JS, Wang N-P, Kin H, Payne CS, Sun H-Y, Guyton RA, Vinten-Johansen J, Zhao Z-Q (2004) Myocardial protection with postconditioning is not enhanced by ischemic preconditioning. Ann Thorac Surg 78:961–969
Hausenloy DJ, Duchen MR, Yellon DM (2003) Inhibiting mitochondrial permeability transition pore opening at reperfusion protects against ischaemia-reperfusion injury. Cardiovasc Res 60:617–625
Hausenloy DJ, Maddock HL, Baxter GF, Yellon DM (2002) Inhibiting mitochondrial permeability transition pore opening: a new paradigm for myocardial preconditioning? Cardiovasc Res 55:534–543
Hausenloy DJ, Tsang A, Mocanu MM, and Yellon DM (2005) Ischemic preconditioning protects by activating prosurvival kinases at reperfusion. Am J Physiol (Heart Circ Physiol) 288:H971–H976
Hausenloy DJ, Yellon DM (2004) New directions for protecting the heart against ischaemia-reperfusion injury: targeting the Reperfusion Injury Salvage Kinase (RISK)-pathway. Cardiovasc Res 61:448–460
Heusch G (2004) Postconditioning – old wine in a new bottle? J Am Coll Cardiol 44:1111–1112
Hori M, Kitakaze M, Sato H, Takashima S, Iwakura K, Inoue M, Kitabatake A, Kamada T (1991) Staged reperfusion attenuates myocardial stunning in dogs. Role of transient acidosis during early reperfusion. Circulation 84:2135–2145
Hurtado C, Pierce GN (2001) Sodiumhydrogen exchange inhibition: pre-versus post-ischemic treatment. Basic Res Cardiol 96:312–317
Isobe N, Oshima S, Taniguchi K, Hoshizaki H, Adachi H, Toyama T, Naito S, Nogami A, Sugawara M (2000) Does repeated balloon in.ation during coronary angioplasty induce ischemic tolerance? Analysis based on regional work. Heart Vessels 15:117–123
Jennings RB, Reimer KA, Steenbergen C (1986) Myocardial ischemia revisited: the osmolar load, membrane damage and reperfusion. J Mol Cell Cardiol 18:769–780
Johnson G, III, Tsao PS, Lefer AM (1991) Cardioprotective effects of authentic nitric oxide in myocardial ischemia with reperfusion. Crit Care Med 19:244–252
Jordan JE, Zhao Z-Q, Sato H, Taft S, Vinten-Johansen J (1997) Adenosine A2 receptor activation attenuates reperfusion injury by inhibiting neutrophil accumulation, superoxide generation and coronary endothelial adherence. J Pharmacol Exp Ther 280:301–309
Kelly RA, Balligand J-L, Smith TW (1996) Nitric oxide and cardiac function. Circ Res 79:363–380
Kevin LG, Camara AKS, Riess ML, Novalija E, Stowe DF (2003) Ischemic preconditioning alters real-time measure of O2 radicals in intact hearts with ischemia and reperfusion. Am J Physiol (Heart Circ Physiol) 284:H566–H574
Kim SO, Baines CP, Critz SD, Pelech SL, Katz S, Downey JM, Cohen MV (1999) Ischemia induced activation of heat shock protein 27 kinases and casein kinase 2 in the preconditioned rabbit heart. Biochemistry and Cell Biology-Biochimie et Biologie Cellulaire 77:559–567
Kin H, Lofye MT, Amerson BS, Zatta AJ, Kerendi F, Halkos ME, Zhao Z-Q, Headrick JP, Guyton RA, Vinten- Johansen J (2004) Cardioprotection by “postconditioning” is mediated by increased retention of endogenous intravascular adenosine and activation of A2a receptors during reperfusion. Circulation 110:III-168
Kin H, Zatta AJ, Lofye MT, Amerson BS, Halkos ME, Kerendi F, Zhao Z-Q, Guyton RA, Headrick JP, Vinten- Johansen J (2005) Postconditioning reduces infarct size via adenosine receptor activation by endogenous adenosine. Cardiovasc Res (In Press)
Kin H, Zhao Z-Q, Sun H-Y, Wang N-P, Corvera JS, Halkos ME, Kerendi F, Guyton RA, Vinten-Johansen J (2004) Postconditioning attenuates myocardial ischemia-reperfusion injury by inhibiting events in the early minutes of reperfusion. Cardiovasc Res 62:74–85
Klein HH, Pich S, Bohle RM, Lindert- Heimberg S, Nebendahl K (2000) Na+/H+ Exchange inhibitor cariporide attenuates cell injury predominantly during ischemia and not at onset of reperfusion in porcine hearts with low residual blood flow. Circulation 102:1977–1982
Lefer AM, Ma X-L, Weyrich A, Lefer DJ (1993) Endothelial dysfunction and neutrophil adherence as critical events in the development of reperfusion injury. Agents Actions (Suppl) 41:127–135
Lefer AM, Tsao PS, Lefer DJ, Ma X-L (1991) Role of endothelial dysfunction in the pathogenesis of reperfusion injury after myocardial ischemia. FASEB J 5:2029–2034
Lefer AM, Weyrich AS, Buerke M (1994) Role of selectins, a new family of adhesion molecules, in ischaemia-reperfusion injury. Cardiovasc Res 28:289–294
Lefer DJ, Nakanishi K, Johnston WE, Vinten-Johansen J (1993) Anti-neutrophil and myocardial protecting action of SPM-5185, a novel nitric oxide (NO) donor, following acute myocardial ischemia and reperfusion in dogs. Circulation 88:2337–2350
Lefer DJ, Shandelya SM, Serrano CV Jr, Becker LC, Kuppusamy P, Zweier JL (1993) Cardioprotective actions of a monoclonal antibody against CD-18 in myocardial ischemia-reperfusion injury. Circulation 88:1779–1787
Lucchesi BR (1994) Complement, neutrophils and free radicals: mediators of reperfusion injury. [Review]. Arzneim-Forsch/Drug Res 44:420–432
Ma X-L, Weyrich AS, Lefer DJ, Lefer AM (1993) Diminished basal nitric oxide release after myocardial ischemia and reperfusion promotes neutrophil adherence to coronary endothelium. Circ Res 72:403–412
Meng H, McVey M, Perrone M, Clark KL (2000) Intravenous AMP 579, a novel adenosine A(1)/A(2a) receptor agonist, induces a delayed protection against myocardial infarction in minipig. Eur J Pharmacol 387:101–105
Miki T, Liu GS, Cohen MV, Downey JM (1998) Mild Hypothermia reduces infarct size in the beating rabbit heart: A practical intervention for acute myocardial infarction? Basic Res Cardiol 93:372–383
Miller TD, Christian TF, Hopfenspirger MR, Hodge DO, Gersh BJ, Gibbons RJ (1995) Infarct size after acute myocardial infarction measured by quantitative tomographic 99mTc sestamibi imaging predicts subsequent mortality. Circulation 92:334–341
Nakamura M, Zhao Z-Q, Clark KL, Guyton RA, Vinten-Johansen J (1999) AMP579, a new adenosine analog, inhibits neutrophil O2 – generation, degranulation, adherence, and neutrophil- induced injury to coronary vascular endothelium by A2A receptor mechanism. Circulation 100:I-832
Nakanishi K, Vinten-Johansen J, Lefer DJ, Zhao Z-Q, Fowler WC, III, McGee DS, Johnston WE (1992) Intracoronary L-arginine during reperfusion improves endothelial function and reduces infarct size. Am J Physiol (Heart Circ Physiol) 263:H1650–H1658
Okamoto F, Allen BS, Buckberg GD, Bugyi H, Leaf J (1986) Studies of controlled reperfusion after ischemia. XIV. Reperfusion conditons: Importance of ensuring gentle versus sudden reperfusion during relief of coronary occlusion. J Thorac Cardiovasc Surg 92:613–620
Pagliaro PR, Rastaldo R, Penna C, Mancardi D, Cappello S, Losano GA (2004) Nitric oxide (NO)-cylic guanosine monophosphate (cGMP) pathway is involved in ischemic postconditioning in the isolated rat heart. Circulation 110:III-136
Philipp SD, Downey JM, Cohen MV (2004) Postconditioning must be initiated in less than 1 minute following reperfusion and is dependent on adenosine receptors and P13-kinase. Circulation 110:III-168
Piantadosi CA, Tatro LG, Whorton AR (2002) Nitric oxide and differential effects of ATP on mitochondrial permeability transition. Nitric Oxide-Biology and Chemistry 6:45–60
Piper HM (1989) Energy deficiency, calcium overload or oxidative stress: possible causes of irreversible ischemic myocardial injury. Klin Wochenschr 67:465–476
Piper HM, Garcia-Dorado D (1999) Prime cause of rapid cardiomyocyte death during reperfusion. Ann Thorac Surg 68:1913–1919
Piper HM, Garcia-Dorado D, Ovize M (1998) A fresh look at reperfusion injury. Cardiovasc Res 38:291–300
Piper HM, Schafer AC (2004) The .rst minutes of reperfusion: a window of opportunity for cardioprotection. Cardiovasc Res 61:365–371
Pisarenko OI, Shulzhenko VS, Studneva IM, Kapelko VI (1993) Effects of gradual reperfusion on postischemic metabolism and functional recovery of isolated guinea pig heart. Biochemical Medicine and Metabolic Biology 50:127–134
Przyklenk K (1997) Lethal myocardial “reperfusion injury”: The opinions of good men. J Thrombosis Thrombolysis 4:5–6
Qian T, Nieminen AL, Herman B, Lemasters JJ (1997) Mitochondrial permeability transition in pH-dependent reperfusion injury to rat hepatocytes. Am J Physiol (Cell Physiology) 273:C1783–C1792
Sato H, Jordan JE, Zhao Z-Q, Sarvotham SS, Vinten-Johansen J (1997) Gradual reperfusion reduces infarct size and endothelial injury but augments neutrophil accumulation. Ann Thorac Surg 64:1099–1107
Schultz JE, Gross GJ (2001) Opioids and cardioprotection. Pharmacol Ther 89:123–137
Schwartz LM (2004) Ischemic postconditioning during reperfusion fails to protect against lethal myocardial ischemia-reperfusion injury in pigs. Circulation 110:III-106
Steenbergen C, Hill ML, Jennings RB (1985) Volume regulation and plasma membrane injury in aerobic, anaerobic, and ischemic myocardium in vitro. Effects of osmotic cell swelling on plasma membrane integrity. Circ Res 57:864–875
Sun H-Y, Wang N-P, Kerendi F, Halkos ME, Kin H, Guyton RA, Vinten-Johansen J, Zhao Z-Q (2004) Hypoxic postconditioning reduces cardiomyocyte loss by inhibiting the generation of reactive oxygen species and intracellular calcium overload. Am J Physiol (Heart Circ Physiol) (In Press)
Todd J, Zhao ZQ, Williams MW, Sato H, Van Wylen DG, Vinten-Johansen J (1996) Intravascular adenosine at reperfusion reduces infarct size and neutrophil adherence. Ann Thorac Surg 62:1364–1372
Tsang A, Hausenloy DJ, Macanu MM, Yellon DM (2004) Postconditioning-A form of “modi.ed reperfusion” protects the myocardium by activating the P13KAkt pathway. Circulation 110:III-167
Tsang A, Hausenloy DJ, Mocanu MM, Yellon DM (2004) Postconditioning: a form of “modi.ed reperfusion” protects the myocardium by activating the phosphatidylinositol 3-kinase-Akt pathway. Circ Res 95:230–232
Tsao PS, Aoki N, Lefer DJ, Johnson G, III, Lefer AM (1990) Time course of endothelial dysfunction and myocardial injury during myocardial ischemia and reperfusion in the cat. Circulation 82:1402–1412
Tsao PS, Lefer AM (1990) Time course and mechanism of endothelial dysfunction in isolated ischemic- and hypoxicperfused rat hearts. Am J Physiol (Heart Circ Physiol) 259:H1660–H1666
Ueno T, Yamada T, Yoshikai M, Natsuaki M, Itoh T (1993) Effect of gradual reperfusion on ventricular function after 6-h preservation. Cardiovasc Surg 1:695–700
Vinten-Johansen J (2004) Involvement of neutrophils in the pathogenesis of lethal myocardial reperfusion injury. Cardiovasc Res 61:481–497
Vinten-Johansen J, Buckberg GD, Okamoto F, Rosenkranz ER, Bugyi H, Leaf J (1986) Studies of controlled reperfusion after ischemia. V. Superiority of surgical versus medical reperfusion after regional ischemia. J Thorac Cardiovasc Surg 92:525–534
Vinten-Johansen J, Edgerton TA, Howe HR, Gayheart PA, Mills SA, Howard G, Cordell AR (1985) Immediate functional recovery and avoidance of reperfusion injury with surgical revascularization of short-term coronary occlusion. Circulation 72:431–439
Vinten-Johansen J, Lefer DJ, Nakanishi K, Johnston WE, Brian CA, Cordell AR (1992) Controlled coronary hydrodynamics at the time of reperfusion reduces postischemic injury. Cor Art Dis 3:1081–1093
Vinten-Johansen J, Ronson RS, Thourani VH, Wechsler AS (2000) Surgical myocardial protection. In: Gravlee GP, Davis RF, Kurusz M, Utley JR (eds) Cardiopulmonary Bypass Principles and Practice. Lippincott Williams & Wilkins Philadelphia, PA, pp 214–264
Vinten-Johansen J, Rosenkranz ER, Buckberg GD, Leaf J, Bugyi H (1986) Studies of controlled reperfusion after ischemia: VI. Metabolic and histochemical benefits of regional blood cardioplegic reperfusion without cardiopulmonary bypass. J Thorac Cardiovasc Surg 92:535–542
Vinten-Johansen J, Zhao Z-Q (1995) Cardioprotection from ischemic-reperfusion injury by adenosine. In: Abd-Elfattah AS, Wechsler AS (eds) Purines and Myocardial Protection. Kluwer Academic Publishers Boston, MA, pp 315–344
Xu Z, Yang XM, Cohen MV, Neumann T, Heusch G, Downey JM (2000) Limitation of infarct size in rabbit hearts by the novel adenosine receptor agonist AMP 579 administered at reperfusion. J Mol Cell Cardiol 32:2339–2347
Yang X-M, Downey JM, Cohen MV (2003) Multiple, brief coronary occlusions during early reperfusion protect rabbit hearts by activation of ERK and production of nitric oxide. Circulation (Suppl) 108:158
Yang X-M, Downey JM, Cohen MV (2004) Postconditioning’s protection is not dependent on circulating blood factors or cells but requires P13-kinase and guanylyl cyclase activation. Circulation 110:III-168
Yang X-M, Philipp S, Downey JM, Cohen MV (2005) Postconditioning’s protection is not dependent on circulating blood factors or cells but involves adenosine receptors and requires PI3- kinase and guanylyl cyclase activation. Basic Res Cardiol 100:57–63
Yang X-M, Proctor JB, Cui L, Krieg T, Downey JM, Cohen MV (2004) Multiple, brief coronary occlusions during early reperfusion protect rabbit hearts by targeting cell signaling pathways. J Am Coll Cardiol 44:1103–1110
Zhao Z-Q, Budde JM, Morris CD, Wang N-P, Velez DA, Muraki S, Guyton RA, Vinten-Johansen J (2001) Adenosine Attenuates Reperfusion-induced Apoptotic Cell Death by Modulating Expression of Bcl-2 and Bax Proteins. J Mol Cell Cardiol 33:57–68
Zhao Z-Q, Clark KL, Wang N-P, Velez DA, Guyton RA, Vinten-Johansen J (2000) Comparison of AMP579 and adenosine in inhibition of cell-cell interaction between human neutrophil and vascular endothelial cell. Drug Devel Res 49:266–272
Zhao Z-Q, Corvera JS, Halkos ME, Kerendi F, Wang N-P, Guyton RA, Vinten-Johansen J (2003) Inhibition of myocardial injury by ischemic postconditioning during reperfusion: comparison with ischemic preconditioning. Am J Physiol (Heart Circ Physiol) 285:579–588
Zhao Z-Q, Corvera JS, Wang N-P, Guyton RA, Vinten-Johansen J (2002) Reduction in infarct size and preservation of endothelial function by ischemic postconditioning: Comparison with ischemic preconditioning. Circulation (Suppl) 106:II314
Zhao Z-Q, McGee DS, Nakanishi K, Toombs CF, Johnston WE, Ashar MS, Vinten-Johansen J (1993) Receptormediated cardioprotective effects of endogenous adenosine are exerted primarily during reperfusion after coronary occlusion in the rabbit. Circulation 88:709–719
Zhao Z-Q, Nakamura M, Wang N-P, Wilcox JN, Shearer S, Guyton RA, Vinten-Johansen J (1999) Administration of adenosine during reperfusion reduces injury of vascular endothelium and death of myocytes. Cor Art Dis 10:617–628
Zhao Z-Q, Sato H, Williams MW, Fernandez AZ, Vinten-Johansen J (1996) Adenosine A2-receptor activation inhibits neutrophil-mediated injury to coronary endothelium. Am J Physiol (Heart Circ Physiol) 271:H1456–H1464
Zhao Z-Q, Sun H-Y, Wang N-P, Kerendi F, Guyton RA, Vinten-Johansen J (2003) Hypoxic post-conditioning reduces cardiomyocyte loss by inhibiting reactive oxygen species-triggered mitochondrial calcium overload. Circulation (Suppl) 108:IV-174
Zhao Z-Q, Todd JC, Sato H, Vinten-Johansen J (1997) Adenosine A2-mediated cardioprotection during reperfusion does not involve KATP channel activation. Am J Physiol (Heart Circ Physiol) 273:H1677–H1678
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vinten-Johansen, J., Zhao, ZQ., Zatta, A.J. et al. Postconditioning A new link in nature’s armor against myocardial ischemia–reperfusion injury. Basic Res Cardiol 100, 295–310 (2005). https://doi.org/10.1007/s00395-005-0523-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00395-005-0523-x