Abstract
Objective
This study aimed to evaluate the relationship between telomere length and rheumatoid arthritis (RA).
Methods
We performed a meta-analysis of studies comparing the telomere length in RA patients and healthy controls, and conducted subgroup analysis based on ethnicity, age-matched status, study quality, sample type, assay method, subject number, and shared epitope (SE) status.
Results
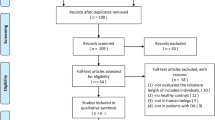
Nine studies from seven articles, with 388 RA patients and 362 controls, were included. Meta-analysis showed that the telomere length was significantly shorter in all individuals of the RA group than in those of the control group (SMD = −0.833, 95 % CI = −1.332 to −0.334, p = 0.001). Stratification by ethnicity showed significantly shortened telomere lengths in both mixed and age-matched Caucasian populations with RA (SMD = −1.415, 95 % CI = −1.709 to −1.120, p < 1.0 × 10−8; SMD = −0.658, 95 % CI = −1.187 to −0.0.128, p = 0.015). The telomere length was significantly shorter in the RA group than in the age-matched control group; however, this was not the case in the RA group that was not age-matched (SMD = −1.070, 95 % CI = −1.489 to −0.650, p = 5.7 × 10−7; SMD = 0.155, 95 % CI = −0.119 to 0.429, p = 0.267). Stratification by SE status revealed a significantly shortened telomere length in the SE-positive group, but not in the SE-negative group (SMD = −1.033, 95 % CI = −1.398 to −0.768, p < 1.0 × 10−8; SMD = −0.967, 95 % CI = −2.382 to 0.449, p = 0.181). In addition, the telomere length was significantly shorter in the SE-positive RA group than in the SE-negative RA group (SMD = −0.415, 95 % CI = −0.699 to −0.131, p = 0.004).
Conclusions
Our meta-analysis demonstrated that the telomere length was significantly shorter in patients with RA, and was significantly more so in the SE-positive group than in the SE-negative group.
Zusammenfassung
Ziel
Ziel dieser Studie war es, die Beziehung zwischen der Telomerlänge und rheumatoider Arthritis (RA) zu beurteilen.
Methoden
Es wurde eine Metaanalyse von Studien durchgeführt, in denen die Telomerlänge bei RA-Patienten und einer gesunden Kontrollgruppe verglichen wurde. Darüber hinaus erfolgte eine Subgruppenanalyse basierend auf Ethnizität, altersgematchem Status, Studienqualität, Probentyp, Assay-Methode, Patientenzahl und Shared-epitome(SE)-Status.
Ergebnisse
Neun Studien aus 7 Artikeln mit 388 RA-Patienten und 362 Kontrollpersonen wurden eingeschlossen. Die Metaanalyse zeigte, dass die Telomerlänge bei allen Patienten der RA-Gruppe signifikant kürzer war als in der Kontrollgruppe (SMD = −0,833; 95 % CI = −1,332 bis −0,334; p = 0,001). Die Stratifikation nach Ethnizität zeigte eine signifikant verkürzte Telomerlänge sowohl in der gemischten als auch in der altersgematchten kaukasischen Population mit RA (SMD = −1,415; 95 % CI = −1,709 bis −1,120, p < 1,0 × 10−8; SMD = −0,658; 95 % CI = −1,187 bis −0,128; p = 0,015). Die Telomerlänge war in der RA-Gruppe signifikant kürzer als in der altersgematchten Kontrollgruppe, jedoch war dies in der nicht altersgematchen RA-Gruppe nicht der Fall (SMD = −1,070; 95 % CI = −1,489 bis −0,650; p = 5,7 × 10−7; SMD = 0,155; 95 % CI = −0,119 bis 0,429; p = 0,267). Die Stratifikation nach SE-Status zeigte eine signifikant verkürzte Telomerlänge in der SE-positiven Gruppe, jedoch nicht in der SE-negativen Gruppe (SMD = −1,033; 95 % CI = −1,398 bis −0,768; p < 1,0 × 10−8; SMD = −0,967; 95 % CI = −2,382 bis 0,449; p = 0,181). Zudem war die Telomerlänge in der SE-positiven RA-Gruppe signifikant kürzer als in der SE-negativen RA-Gruppe (SMD = −0,415; 95 % CI = −0,699 bis −0,131; p = 0,004).
Schlussfolgerung
Die Metaanalyse zeigte, dass die Telomerlänge bei Patienten mit RA signifikant kürzer war, wobei dies in der SE-positiven Gruppe noch deutlicher war als in der SE-negativen Gruppe.



Similar content being viewed by others
References
Harris ED Jr. (1990) Rheumatoid arthritis. Pathophysiology and implications for therapy. N Engl J Med 322(18):1277–1289
Choi SJ, Rho YH, Ji JD, Song GG, Lee YH (2006) Genome scan meta-analysis of rheumatoid arthritis. Rheumatology (Oxford) 45(2):166–170
Blackburn EH (1991) Structure and function of telomeres. Nature 350(6319):569–573
Kipling D (2001) Telomeres, replicative senescence and human ageing. Maturitas 38(1):25–37
Collado M, Blasco MA, Serrano M (2007) Cellular senescence in cancer and aging. Cell 130(2):223–233
Correia-Melo C, Hewitt G, Passos JF (2014) Telomeres, oxidative stress and inflammatory factors: partners in cellular senescence? Longev Healthspan 3(1):1
Schonland SO, Lopez C, Widmann T, Zimmer J, Bryl E, Goronzy JJ et al (2003) Premature telomeric loss in rheumatoid arthritis is genetically determined and involves both myeloid and lymphoid cell lineages. Proc Natl Acad Sci U S A 100(23):13471–13476
Blinova EA, Zinnatova EV, Barkovskaya M, Borisov VI, Sizikov AE, Kozhevnikov VS et al (2016) Telomere length of individual chromosomes in patients with rheumatoid arthritis. Bull Exp Biol Med 160(6):779–782
Antoniou KM, Margaritopoulos GA, Proklou A, Karagiannis K, Lasithiotaki I, Soufla G et al (2012) Investigation of telomerase/telomeres system in bone marrow mesenchymal stem cells derived from IPF and RA-UIP. J Inflamm (Lond) 9(1):27
Tamayo M, Mosquera A, Rego JI, Fernandez-Sueiro JL, Blanco FJ, Fernandez JL (2010) Differing patterns of peripheral blood leukocyte telomere length in rheumatologic diseases. Mutat Res 683(1–2):68–73
Colmegna I, Diaz-Borjon A, Fujii H, Schaefer L, Goronzy JJ, Weyand CM (2008) Defective proliferative capacity and accelerated telomeric loss of hematopoietic progenitor cells in rheumatoid arthritis. Arthritis Rheum 58(4):990–1000
Koetz K, Bryl E, Spickschen K, O’Fallon WM, Goronzy JJ, Weyand CM (2000) T cell homeostasis in patients with rheumatoid arthritis. Proc Natl Acad Sci U S A 97(16):9203–9208
Steer SE, Williams FM, Kato B, Gardner JP, Norman PJ, Hall MA et al (2007) Reduced telomere length in rheumatoid arthritis is independent of disease activity and duration. Ann Rheum Dis 66(4):476–480
Costenbader KH, Prescott J, Zee RY, De Vivo I (2011) Immunosenescence and rheumatoid arthritis: does telomere shortening predict impending disease? Autoimmun Rev 10(9):569–573
Prelog M (2006) Aging of the immune system: a risk factor for autoimmunity? Autoimmun Rev 5(2):136–139
Hoffecker BM, Raffield LM, Kamen DL, Nowling TK (2013) Systemic lupus erythematosus and vitamin D deficiency are associated with shorter telomere length among African Americans: a case-control study. PLOS ONE 8(5):e63725
Haque S, Rakieh C, Marriage F, Ho P, Gorodkin R, Teh LS et al (2013) Shortened telomere length in patients with systemic lupus erythematosus. Arthritis Rheum 65(5):1319–1323
Skamra C, Romero-Diaz J, Sandhu A, Huang Q, Lee J, Pearce W et al (2013) Telomere length in patients with systemic lupus erythematosus and its associations with carotid plaque. Rheumatology (Oxford) 52(6):1101–1108
Beier F, Balabanov S, Amberger CC, Hartmann U, Manger K, Dietz K et al (2007) Telomere length analysis in monocytes and lymphocytes from patients with systemic lupus erythematosus using multi-color flow-FISH. Lupus 16(12):955–962
Wu CH, Hsieh SC, Li KJ, Lu MC, Yu CL (2007) Premature telomere shortening in polymorphonuclear neutrophils from patients with systemic lupus erythematosus is related to the lupus disease activity. Lupus 16(4):265–272
Kurosaka D, Yasuda J, Yoshida K, Yoneda A, Yasuda C, Kingetsu I et al (2006) Abnormal telomerase activity and telomere length in T and B cells from patients with systemic lupus erythematosus. J Rheumatol 33(6):1102–1107
Lin J, Xie J, Qian WB (2005) Telomerase activity and telomere length in CD4+, CD8+ and CD19+ lymphocytes from patients with systemic lupus erythematosus. Zhejiang Da Xue Xue Bao Yi Xue Ban 34(6):534–537
Honda M, Mengesha E, Albano S, Nichols WS, Wallace DJ, Metzger A et al (2001) Telomere shortening and decreased replicative potential, contrasted by continued proliferation of telomerase-positive CD8+CD28(lo) T cells in patients with systemic lupus erythematosus. Clin Immunol 99(2):211–221
Lee YH, Rho YH, Choi SJ, Ji JD, Song GG (2007) PADI4 polymorphisms and rheumatoid arthritis susceptibility: a meta-analysis. Rheumatol Int 27(9):827–833
Lee YH, Bae SC, Choi SJ, Ji JD, Song GG (2011) Associations between vitamin D receptor polymorphisms and susceptibility to rheumatoid arthritis and systemic lupus erythematosus: a meta-analysis. Mol Biol Rep 38(6):3643–3651
Lee YH, Woo JH, Choi SJ, Ji JD, Song GG (2010) Associations between osteoprotegerin polymorphisms and bone mineral density: a meta-analysis. Mol Biol Rep 37(1):227–234
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13
Ridout KK, Ridout SJ, Price LH, Sen S, Tyrka AR (2016) Depression and telomere length: A meta-analysis. J Affect Disord 191:237–247
Wells G, Shea B, O’connell D, Peterson J, Welch V, Losos M et al (2000) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses
Cohen J (1988) Statistical power analysis for the behavioral sciences, 2nd edn. L. Erlbaum, Hillsdale
Egger M, Smith GD, Phillips AN (1997) Meta-analysis: principles and procedures. BMJ 315(7121):1533–1537
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Zhu X, Han W, Xue W, Zou Y, Xie C, Du J et al (2016) The association between telomere length and cancer risk in population studies. Sci Rep 6:22243
Hohensinner PJ, Goronzy JJ, Weyand CM (2011) Telomere dysfunction, autoimmunity and aging. Aging Dis 2(6):524–537
Lin PY, Huang YC, Hung CF (2016) Shortened telomere length in patients with depression: A meta-analytic study. J Psychiatr Res 76:84–93
Willeit P, Raschenberger J, Heydon EE, Tsimikas S, Haun M, Mayr A et al (2014) Leucocyte telomere length and risk of type 2 diabetes mellitus: new prospective cohort study and literature-based meta-analysis. PLOS ONE 9(11):e112483
Dehbi AZ, Radstake TR, Broen JC (2013) Accelerated telomere shortening in rheumatic diseases: cause or consequence? Expert Rev Clin Immunol 9(12):1193–1204
Starkweather AR, Alhaeeri AA, Montpetit A, Brumelle J, Filler K, Montpetit M et al (2014) An integrative review of factors associated with telomere length and implications for biobehavioral research. Nurs Res 63(1):36–50
Honda M, Mengesha E, Albano S, Nichols WS, Wallace DJ, Metzger A et al (2001) Telomere shortening and decreased replicative potential, contrasted by continued proliferation of telomerase-positive CD8+CD28(lo) T cells in patients with systemic lupus erythematosus. Clin Immunol 99(2):211–221
Mirabello L, Yu K, Kraft P, De Vivo I, Hunter DJ, Prescott J et al (2010) The association of telomere length and genetic variation in telomere biology genes. Hum Mutat 31(9):1050–1058
Bax M, Huizinga TW, Toes RE (2014) The pathogenic potential of autoreactive antibodies in rheumatoid arthritis. Semin Immunopathol 36(3):313–325
Montpetit AJ, Alhareeri AA, Montpetit M, Starkweather AR, Elmore LW, Filler K et al (2014) Telomere length: a review of methods for measurement. Nurs Res 63(4):289–299
Acknowledgements
This study was supported in part by a grant of the Korea Healthcare technology R&D Project, Ministry for Health and Welfare, Republic of Korea (HI15C2958).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Y. H. Lee and S.-C. Bae state that they have no competing interest.
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Editorial board
U. Müller-Ladner, Bad Nauheim
U. Lange, Bad Nauheim
Rights and permissions
About this article
Cite this article
Lee, Y.H., Bae, SC. Association between shortened telomere length and rheumatoid arthritis. Z Rheumatol 77, 160–167 (2018). https://doi.org/10.1007/s00393-016-0209-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00393-016-0209-9