Abstract
Objectives
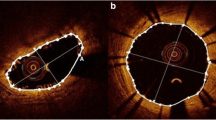
The objective was to investigate the acute mechanical effects of post-dilatation on bioresorbable scaffolds (BRS) as determined by optical coherence tomography (OCT).
Background
Post-dilatation with high-pressure balloons is regarded as a key component of BRS implantation for treatment of coronary artery stenoses. However, the impact of post-dilatation on BRS in vivo has not been thoroughly investigated.
Methods
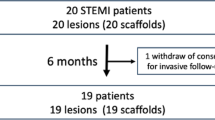
OCT was performed after the implantation procedure of 51 everolimus-eluting or novolimus-eluting polylactic acid-based BRS with (n = 27) or without non-compliant balloon post-dilatation (n = 24). The number of malapposed struts, strut fractures, edge dissections, residual in-scaffold area stenosis, and incomplete scaffold apposition area was analyzed over the complete length of each BRS with a spacing of 1 mm.
Results
OCT revealed a significantly lower incomplete scaffold apposition area if post-dilatation was performed (0.16 ± 0.49 mm2 with post-dilatation vs. 2.65 ± 2.78 mm2 without post-dilatation, p < 0.001), as well as a significantly lower absolute number of malapposed struts (1 ± 2 with post-dilatation vs. 13 ± 13 without post-dilatation, p < 0.001). No significant differences regarding residual in-scaffold area stenosis, strut fracture, edge dissection, symmetry index, or eccentricity index were observed in patients with vs. without post-dilatation.
Conclusion
Post-dilatation of BRS with non-compliant balloons significantly reduces the number of malapposed struts and incomplete scaffold apposition area without inducing higher rates of edge dissection or strut fracture.


Similar content being viewed by others
References
Iqbal J, Onuma Y, Ormiston J, Abizaid A, Waksman R, Serruys P (2014) Bioresorbable scaffolds: rationale, current status, challenges, and future. Eur Heart J 35:765–776
Simsek C, Karanasos A, Magro M, Garcia-Garcia HM, Onuma Y, Regar E, Boersma E, Serruys PW, van Geuns RJ (2016) Long-term invasive follow-up of the everolimus-eluting bioresorbable vascular scaffold: five-year results of multiple invasive imaging modalities. EuroIntervention 11:996–1003
Everaert B, Felix C, Koolen J, den Heijer P, Henriques J, Wykrzykowska J, van der Schaaf R, de Smet B, Hofma S, Diletti R, Van Mieghem N, Regar E, Smits P, van Geuns RJ (2015) Appropriate use of bioresorbable vascular scaffolds in percutaneous coronary interventions: a recommendation from experienced users. A position statement on the use of bioresorbable vascular scaffolds in the Netherlands. Neth Heart J 23:161–165
Tamburino C, Latib A, van Geuns RJ, Sabate M, Mehilli J, Gori T, Achenbach S, Alvarez MP, Nef H, Lesiak M, Di Mario C, Colombo A, Naber CK, Caramanno G, Capranzano P, Brugaletta S, Geraci S, Araszkiewicz A, Mattesini A, Pyxaras SA, Rzeszutko L, Depukat R, Diletti R, Boone E, Capodanno D, Dudek D (2015) Contemporary practice and technical aspects in coronary intervention with bioresorbable scaffolds: a European perspective. EuroIntervention 11:45–52
Cuculi F, Puricel S, Jamshidi P, Valentin J, Kallinikou Z, Toggweiler S, Weissner M, Münzel T, Cook S, Gori T (2015) Optical coherence tomography findings in bioresorbable vascular scaffolds thrombosis. Circ Cardiovasc Interv 8(10):e002518. doi:10.1161/CIRCINTERVENTIONS.114.002518 (Epub ahead of print)
Taniwaki M, Radu MD, Zaugg S, Amabile N, Garcia-Garcia HM, Yamaji K, Jørgensen E, Kelbæk H, Pilgrim T, Caussin C, Zanchin T, Veugeois A, Abildgaard U, Jüni P, Cook S, Koskinas KC, Windecker S, Räber L (2016) Mechanisms of very late drug-eluting stent thrombosis assessed by optical coherence tomography. Circulation. doi:10.1161/CIRCULATIONAHA.115.019071 (Epub ahead of print)
Souteyrand G, Amabile N, Mangin L, Chabin X, Meneveau N, Cayla G, Vanzetto G, Barnay P, Trouillet C, Rioufol G, Rangé G, Teiger E, Delaunay R, Dubreuil O, Lhermusier T, Mulliez A, Levesque S, Belle L, Caussin C, Motreff P; PESTO Investigators (2016) Mechanisms of stent thrombosis analysed by optical coherence tomography: insights from the national PESTO French registry. Eur Heart J. doi:10.1093/eurheartj/ehv711 (Epub ahead of print)
Prati F, Kodama T, Romagnoli E, Gatto L, Di Vito L, Ramazzotti V, Chisari A, Marco V, Cremonesi A, Parodi G, Albertucci M, Alfonso F (2015) Suboptimal stent deployment is associated with subacute stent thrombosis: optical coherence tomography insights from a multicenter matched study. From the CLI Foundation investigators: the CLI-THRO study. Am Heart J 169:249–256
Guagliumi G, Sirbu V, Musumeci G, Gerber R, Biondi-Zoccai G, Ikejima H, Ladich E, Lortkipanidze N, Matiashvili A, Valsecchi O, Virmani R, Stone GW (2012) Examination of the in vivo mechanisms of late drug-eluting stent thrombosis: findings from optical coherence tomography and intravascular ultrasound imaging. J Am Coll Cardiol Interv 5:12–20
Alfonso F, Dutary J, Paulo M, Gonzalo N, Pérez-Vizcayno MJ, Jiménez-Quevedo P, Escaned J, Bañuelos C, Hernández R, Macaya C (2012) Combined use of optical coherence tomography and intravascular ultrasound imaging in patients undergoing coronary interventions for stent thrombosis. Heart 98:1213–1220
Prati F, Regar E, Mintz GS, Arbustini E, Di Mario C, Jang IK, Akasaka T, Costa M, Guagliumi G, Grube E, Ozaki Y, Pinto F, Serruys PW (2010) Expert review document on methodology, terminology, and clinical applications of optical coherence tomography: physical principles, methodology of image acquisition, and clinical application for assessment of coronary arteries and atherosclerosis. Eur Heart J 31:401–415
Serruys PW, Onuma Y, Ormiston JA, de Bruyne B, Regar E, Dudek D, Thuesen L, Smits PC, Chevalier B, McClean D, Koolen J, Windecker S, Whitbourn R, Meredith I, Dorange C, Veldhof S, Miquel-Hebert K, Rapoza R, García-García HM (2010) Evaluation of the second generation of a bioresorbable everolimus drug-eluting vascular scaffold for treatment of de novo coronary artery stenosis: six-month clinical and imaging outcomes. Circulation 122:2301–2312
Mattesini A, Boeder N, Löblich K, Valente S, Foin N, Caiazzo G, Ghione M, Gensini GF, Italo P, Di Mario C, Nef H (2015) TCT-514 Absorb vs DESolve: an optical coherence tomography comparison of acute mechanical performances. J Am Coll Cardiol 66(15_S). doi:10.1016/j.jacc.2015.08.531 (Epub ahead of print)
Mattesini A, Secco GG, Dall’Ara G, Ghione M, Rama-Merchan JC, Lupi A, Viceconte N, Lindsay AC, De Silva R, Foin N, Naganuma T, Valente S, Colombo A, Di Mario C (2014) ABSORB biodegradable stents versus second-generation metal stents: a comparison study of 100 complex lesions treated under OCT guidance. J Am Coll Cardiol Interv 7:741–750
Kimura T, Morimoto T, Kozuma K, Honda Y, Kume T, Aizawa T, Mitsudo K, Miyazaki S, Yamaguchi T, Hiyoshi E, Nishimura E, Isshiki T, RESTART Investigators (2010) Comparisons of baseline demographics, clinical presentation, and long-term outcome among patients with early, late, and very late stent thrombosis of sirolimus-eluting stents. Circulation 122:52–61
van Werkum JW, Heestermans AA, de Korte FI, Kelder JC, Suttorp MJ, Rensing BJ, Zwart B, Brueren BR, Koolen JJ, Dambrink JH, van’t Hof AW, Verheugt FW, ten Berg JM (2009) Long-term clinical outcome after a first angiographically confirmed coronary stent thrombosis: an analysis of 431 cases. Circulation 119:828–834
Gutiérrez-Chico JL, Gijsen F, Regar E, Wentzel J, de Bruyne B, Thuesen L, Ormiston J, McClean DR, Windecker S, Chevalier B, Dudek D, Whitbourn R, Brugaletta S, Onuma Y, Serruys PW (2012) Differences in neointimal thickness between the adluminal and the abluminal sides of malapposed and side-branch struts in a polylactide bioresorbable scaffold: evidence in vivo about the abluminal healing process. J Am Coll Cardiol Interv 5:428–435
Karanasos A, Van Mieghem N, van Ditzhuijzen N, Felix C, Daemen J, Autar A, Onuma Y, Kurata M, Diletti R, Valgimigli M, Kauer F, van Beusekom H, de Jaegere P, Zijlstra F, van Geuns RJ, Regar E (2015) Angiographic and optical coherence tomography insights into bioresorbable scaffold thrombosis: single-center experience. Circ Cardiovasc Interv 8(5). doi:10.1161/CIRCINTERVENTIONS.114.002369
Tearney GJ, Regar E, Akasaka T, Adriaenssens T, Barlis P, Bezerra HG, Bouma B, Bruining N, Cho JM, Chowdhary S, Costa MA, de Silva R, Dijkstra J, Di Mario C, Dudek D, Falk E, Feldman MD, Fitzgerald P, Garcia-Garcia HM, Gonzalo N, Granada JF, Guagliumi G, Holm NR, Honda Y, Ikeno F, Kawasaki M, Kochman J, Koltowski L, Kubo T, Kume T, Kyono H, Lam CC, Lamouche G, Lee DP, Leon MB, Maehara A, Manfrini O, Mintz GS, Mizuno K, Morel MA, Nadkarni S, Okura H, Otake H, Pietrasik A, Prati F, Räber L, Radu MD, Rieber J, Riga M, Rollins A, Rosenberg M, Sirbu V, Serruys PW, Shimada K, Shinke T, Shite J, Siegel E, Sonoda S, Suter M, Takarada S, Tanaka A, Terashima M, Thim T, Uemura S, Ughi GJ, van Beusekom HM, van der Steen AF, van Es GA, van Soest G, Virmani R, Waxman S, Weissman NJ, Weisz G; International Working Group for Intravascular Optical Coherence Tomography (IWG-IVOCT) (2012) Consensus standards for acquisition, measurement, and reporting of intravascular optical coherence tomography studies: a report from the International Working Group for Intravascular Optical Coherence Tomography Standardization and Validation. J Am Coll Cardiol 59:1058–1072
Uren NG, Schwarzacher SP, Metz JA, Lee DP, Honda Y, Yeung AC, Fitzgerald PJ, Yock PG, POST Registry Investigators (2002) Predictors and outcomes of stent thrombosis: an intravascular ultrasound registry. Eur Heart J 23:124–132
Gomez-Lara J, Diletti R, Brugaletta S, Onuma Y, Farooq V, Thuesen L, McClean D, Koolen J, Ormiston JA, Windecker S, Whitbourn R, Dudek D, Dorange C, Veldhof S, Rapoza R, Regar E, Garcia-Garcia HM, Serruys PW (2012) Angiographic maximal luminal diameter and appropriate deployment of the everolimus-eluting bioresorbable vascular scaffold as assessed by optical coherence tomography: an ABSORB cohort B trial sub-study. EuroIntervention 8:214–224
Sonoda S, Morino Y, Ako J, Terashima M, Hassan AH, Bonneau HN, Leon MB, Moses JW, Yock PG, Honda Y, Kuntz RE, Fitzgerald PJ, SIRIUS Investigators (2004) Impact of final stent dimensions on long-term results following sirolimus-eluting stent implantation: serial intravascular ultrasound analysis from the sirius trial. J Am Coll Cardiol 43:1959–1963
Costa MA, Angiolillo DJ, Tannenbaum M, Driesman M, Chu A, Patterson J, Kuehl W, Battaglia J, Dabbons S, Shamoon F, Flieshman B, Niederman A, Bass TA, STLLR Investigators (2008) Impact of stent deployment procedural factors on long-term effectiveness and safety of sirolimus-eluting stents (final results of the multicenter prospective STLLR trial). Am J Cardiol 101:1704–1711
Doi H, Maehara A, Mintz GS, Yu A, Wang H, Mandinov L, Popma JJ, Ellis SG, Grube E, Dawkins KD, Weissman NJ, Turco MA, Ormiston JA, Stone GW (2009) Impact of post-intervention minimal stent area on 9-month follow-up patency of paclitaxel-eluting stents: an integrated intravascular ultrasound analysis from the TAXUS IV, V, and VI and TAXUS ATLAS Workhorse, Long Lesion, and Direct Stent Trials. J Am Coll Cardiol Interv 2:1269–1275
De Ribamar Costa Jr J, Abizaid A, Bartorelli AL, Whitbourn R, van Geuns RJ, Chevalier B, Perin M, Seth A, Botelho R, Serruys PW; ABSORB EXTEND Investigators (2015) Impact of post-dilation on the acute and one-year clinical outcomes of a large cohort of patients treated solely with the Absorb bioresorbable vascular scaffold. EuroIntervention 11:141–148
Ormiston JA, Webber B, Ubod B, Darremont O, Webster MW (2015) An independent bench comparison of two bioresorbable drug-eluting coronary scaffolds (Absorb and DESolve) with a durable metallic drug-eluting stent (ML8/Xpedition). EuroIntervention 11(1):60–67
Suwannasom P, Sotomi Y, Ishibashi Y, Cavalcante R, Albuquerque FN, Macaya C, Ormiston JA, Hill J, Lang IM, Egred M, Fajadet J, Lesiak M, Tijssen JG, Wykrzykowska JJ, de Winter RJ, Chevalier B, Serruys PW, Onuma Y (2016) The impact of post-procedural asymmetry, expansion, and eccentricity of bioresorbable everolimus-eluting scaffold and metallic everolimus-eluting stent on clinical outcomes in the ABSORB II Trial. J Am Coll Cardiol Interv 9(12):1231–1242
Rivero F, Bastante T, Cuesta J, Benedicto A, Restrepo JA, Alfonso F (2015) Treatment of in-stent restenosis with bioresorbable vascular scaffolds: optical coherence tomography insights. Can J Cardiol 31(3):255–259
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards
All patients gave written informed consent for the evaluation of clinical, angiographic, procedural, and OCT data. The study was performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. The Ethics Committee of the Justus Liebig University Hospital (Giessen, Germany) approved the study protocol (reference number 203/14).
Conflict of interest
Christian Hamm and Holger Nef received speaking honoraria from Abbott Vascular. Stephan Achenbach and Holger Nef have received research grants (to institution) from Abbott Vascular. Holger Nef also received a research grant (to institution) from Elixir Medical. All the other authors have no potential conflict of interest.
Additional information
F. Blachutzik and N. Boeder contributed equally.
Rights and permissions
About this article
Cite this article
Blachutzik, F., Boeder, N., Wiebe, J. et al. Post-dilatation after implantation of bioresorbable everolimus- and novolimus-eluting scaffolds: an observational optical coherence tomography study of acute mechanical effects. Clin Res Cardiol 106, 271–279 (2017). https://doi.org/10.1007/s00392-016-1048-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-016-1048-z