Abstract
Background
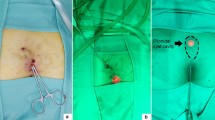
Pilonidal disease (PD) is a common disease of the natal cleft, which can lead to complications including infection and abscess formation. Various operative management options are available, but the ideal technique is still debatable. Recurrent PD after surgical treatment is frequent event for the 25–30% of cases. The present study evaluated endoscopic pilonidal sinus treatment (EPSiT) in recurrent and multi-recurrent PD.
Methods
Of the consecutive prospective patients with recurrent PD, 122 were enrolled in a prospective international multicenter study conducted at a secondary and tertiary colorectal surgery centers. Primary endpoint was to evaluate short- and long-term outcomes: healing rate/time, morbidity rate, re-recurrence rate, and patient’s quality of life (QoL).
Results
Complete wound healing rate was occurred in 95% of the patient, with a mean complete wound healing time of 29 ± 12 days. The incomplete healing rate (5%) was significantly related to the number of external openings (p = 0.008), and recurrence was reported in six cases (5.1%). Normal daily activity was established on the first postoperative day, and the mean duration before patients returned to work was 3 days. QoL significantly increased between the preoperative stage and 30 days after the EPSiT procedure (45.3 vs. 7.9; p < 0.0001).
Conclusions
The EPSiT procedure seems to be a safe and effective technique in treating even complex recurrent PD. It enables excellent short- and long-term outcomes than various other techniques that are more invasive.


Similar content being viewed by others
References
McCallum I, King PM, Bruce J (2007) Healing by primary versus secondary intention after surgical treatment for pilonidal sinus. Cochrane Database Syst Rev (4):CD006213 Review. Update in: Cochrane Database Syst Rev. 2010;(1):CD006213
Iesalnieks I, Deimel S, Schlitt HJ (2013) Karydakis flap for recurrent pilonidal disease. World J Surg 37(5):1115–1120
Bascom J (1980) Pilonidal disease: origin from follicles of hairs and results of follicle removal as treatment. Surgery 87:567–572
Bascom J (1983) Pilonidal disease: long-term results of follicle removal. Dis Colon Rectum 26:800–807
Tejirian T, Lee JJ, Abbas MA (2007) Is wide local excision for pilonidal disease still justified? Am Surg 73(10):1075–1078
Karydakis GE (1973) New approach to the problem of pilonidal sinus. Lancet 2(7843):1414–1415
Gips M, Melki Y, Salem L, Weil R, Sulkes J (2008) Minimal surgery for pilonidal disease using trephines: description of a new technique and long-term outcomes in 1,358 patients. Dis Colon Rectum 51(11):1656–1662
Kepenekci I, Demirkan A, Celasin H, Gecim IE (2010) Unroofing and curettage for the treatment of acute and chronic pilonidal disease. World J Surg 34(1):153–157
Meinero P, Mori L, Gasloli G (2014) Endoscopic pilonidal sinus treatment (E.P.Si.T.). Tech Coloproctol 18(4):389–392
Meinero P, Mori L (2011) Video-assisted anal fistula treatment (VAAFT): a novel sphincter-saving procedure for treating complex anal fistulas. Tech Coloproctol 15:417–422
Steele SR, Perry BW, Mills S, Buie WD (2013) Practice parameters for the management of pilonidal disease. Dis Colon Rectum 56:1021–1027
Karakayali F, Karagulle E, Karabulut Z, Oksuz E, Moray G, Haberal M (2009) Unroofing and marsupialization vs. rhomboid excision and Limberg flap in pilonidal disease: a prospective, randomized, clinical trial. Dis Colon Rectum 52:496–502
Horwood J, Hanratty D, Chandran P, Billings P (2012) Primary closure or rhomboid excision and Limberg flap for the management of primary sacrococcygeal pilonidal disease? A meta-analysis of randomized controlled trials. Color Dis 14(2):143–151
Bali İ, Aziret M, Sözen S, Emir S, Erdem H, Çetinkünar S, İrkörücü O (2015) Effectiveness of Limberg and Karydakis flap in recurrent pilonidal sinus disease. Clinics (Sao Paulo) 70(5):350–355
Nordon IM, Senapati A, Cripps NP (2009) A prospective randomized controlled trial of simple Bascom's technique versus Bascom's cleft closure for the treatment of chronic pilonidal disease. Am J Surg 197(2):189–192
Tien T, Athem R, Arulampalam T (2018) Outcomes of endoscopic pilonidal sinus treatment (EPSiT): a systematic review. Tech Coloproctol 22(5):325–331
Gecim IE, Goktug UU, Celasin H (2017) Endoscopic pilonidal sinus treatment combined with crystalized phenol application may prevent recurrence. Dis Colon Rectum 60(4):405–407
Milone M, Fernandez LMS, Musella M, Milone F (2016) Safety and efficacy of minimally invasive video-assisted ablation of pilonidal sinus. JAMA Surg 151(6):547–553
Chia CLK, Tay VWY, Mantoo SK (2015) Endoscopic pilonidal sinus treatment in the Asian population. Surg Laparosc Endosc Percutan Tech 25(3):e95–e97
Meinero P, Stazi A, Carbone A, Fasolini F, Regusci L, La Torre M (2016) Endoscopic pilonidal sinus treatment: a prospective multicentre trial. Color Dis 18(5):O164–O170
Milone M, Musella M, Di Spiezio Sardo A, Bifulco G, Salvatore G, Sosa Fernandez LM et al (2014) Video-assisted ablation of pilonidal sinus: a new minimally invasive treatment—a pilot study. Surgery 155(3):562–566
Giarratano G, Toscana C, Shalaby M, Buonomo O, Petrella G, Sileri P (2017) Endoscopic pilonidal sinus treatment: long-term results of a prospective series. JSLS J Soc Laparoendosc Surg 21(3):e2017.00043
Emile SH, Elfeki H, Shalaby M, Sakr A (2018 Apr) A systematic review and meta-analysis of the efficacy and safety of video-assisted anal fistula treatment (VAAFT). Surg Endosc 32(4):2084–2093
Author information
Authors and Affiliations
Contributions
Substantial contributions to conception and design, or acquisition of data, or analysis and interpretation of data: PM, GL, AS, AC, FF, LR, MLaT. Drafting the article or revising it critically for important intellectual content: PM, GL, AS, AC, FF, LR, MLaT. Final approval of the version to be published: PM, GL, AS, AC, FF, LR, MLaT.
Corresponding author
Ethics declarations
Conflicts of interest
Professor Piercarlo Meinero declares to receive financial grants from Karl Storz. The remaining authors declare no potential financial conflict of interest related to this study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Meinero, P., La Torre, M., Lisi, G. et al. Endoscopic pilonidal sinus treatment (EPSiT) in recurrent pilonidal disease: a prospective international multicenter study. Int J Colorectal Dis 34, 741–746 (2019). https://doi.org/10.1007/s00384-019-03256-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-019-03256-8