Abstract
Purpose
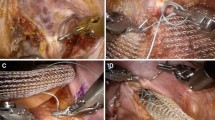
Ventral mesh rectopexy (VMR) is an established, minimally invasive, nerve-sparing procedure for the treatment of various symptomatic morphological changes in the posterior pelvic compartment. We present the short-term functional outcome and patient satisfaction after laparoscopic and robotic VMR with biological mesh.
Methods
We analyzed data from 123 patients who underwent laparoscopic ventral mesh rectopexy (LVMR) or robotic ventral mesh rectopexy (RVMR) from August 2012 to January 2017. Included in these data were patient demographics, intra- and postoperative findings, Cleveland Clinic Constipation Score (CCCS), Obstructed Defecation Score Longo (ODS), Cleveland Clinic Incontinence Score (CCIS), and patient satisfaction as measured by visual analog scale (0–10).
Results
Improvements in CCCS, CCIS, and ODS were statistically significant at 6 and 12 months (p < 0.001). Patient satisfaction was excellent at 6 and 12 months (8.2/10 and 8.3/10, respectively). The overall complication rate was 14%, with a major complication rate of 2%. No mesh-related complications were observed. The need for surgical re-intervention because of relapse, symptom persistence or recurrence, or new symptoms was 3%. Outcome appears to be similar between LVMR and RVMR.
Conclusions
Both LVMR and RVMR with biological mesh are safe and effective in reducing symptoms, as measured by CCCS, CCIS, and ODS, and patient satisfaction is high.

Similar content being viewed by others
References
D'Hoore A, Cadoni R, Penninckx F (2004) Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg 91(11):1500–1505. https://doi.org/10.1002/bjs.4779
Collinson R, Wijffels N, Cunningham C, Lindsey I (2010) Laparoscopic ventral rectopexy for internal rectal prolapse: short-term functional results. Color Dis 12(2):97–104. https://doi.org/10.1111/j.1463-1318.2009.02049.x
Wong M, Meurette G, Abet E, Podevin J, Lehur PA (2011) Safety and efficacy of laparoscopic ventral mesh rectopexy for complex rectocele. Color Dis 13(9):1019–1023. https://doi.org/10.1111/j.1463-1318.2010.02349.x
Samaranayake CB, Luo C, Plank AW, Merrie AE, Plank LD, Bissett IP (2010) Systematic review on ventral rectopexy for rectal prolapse and intussusception. Color Dis 12(6):504–512. https://doi.org/10.1111/j.1463-1318.2009.01934.x
Boons P, Collinson R, Cunningham C, Lindsey I (2010) Laparoscopic ventral rectopexy for external rectal prolapse improves constipation and avoids de novo constipation. Color Dis 12(6):526–532. https://doi.org/10.1111/j.1463-1318.2009.01859.x
Solomon MJ, Young CJ, Eyers AA, Roberts RA (2002) Randomized clinical trial of laparoscopic versus open abdominal rectopexy for rectal prolapse. Br J Surg 89(1):35–39. https://doi.org/10.1046/j.0007-1323.2001.01957.x
Purkayastha S, Tekkis P, Athanasiou T, Aziz O, Paraskevas P, Ziprin P, Darzi A (2005) A comparison of open vs. laparoscopic abdominal rectopexy for full-thickness rectal prolapse: a meta-analysis. Dis Colon Rectum 48(10):1930–1940. https://doi.org/10.1007/s10350-005-0077-x
Powar MP, Ogilvie JW Jr, Stevenson AR (2013) Day-case laparoscopic ventral rectopexy: an achievable reality. Color Dis 15(6):700–706. https://doi.org/10.1111/codi.12110
Smart NJ, Pathak S, Boorman P, Daniels IR (2013) Synthetic or biological mesh use in laparoscopic ventral mesh rectopexy—a systematic review. Color Dis 15(6):650–654. https://doi.org/10.1111/codi.12219
Madiba TE, Baig MK, Wexner SD (2005) Surgical management of rectal prolapse. Arch Surg 140(1):63–73. https://doi.org/10.1001/archsurg.140.1.63
Hurtado EA, Bailey HR, Reeves KO (2007) Rectal erosion of synthetic mesh used in posterior colporrhaphy requiring surgical removal. Int Urogynecol J Pelvic Floor Dysfunct 18(12):1499–1501. https://doi.org/10.1007/s00192-007-0403-z
Alam NN, Narang SK, Köckerling F, Daniels IR, Smart NJ (2015) Rectopexy for rectal prolapse. Front Surg 2:54
Mehmood RK, Parker J, Bhuvimanian L, Qasem E, Mohammed AA, Zeeshan M, Grugel K, Carter P, Ahmed S (2014) Short-term outcome of laparoscopic versus robotic ventral mesh rectopexy for full-thickness rectal prolapse. Is robotic superior? Int J Color Dis 29(9):1113–1118. https://doi.org/10.1007/s00384-014-1937-4
Germain A, Perrenot C, Scherrer ML, Ayav C, Brunaud L, Ayav A, Bresler L (2014) Long-term outcome of robotic-assisted laparoscopic rectopexy for full-thickness rectal prolapse in elderly patients. Color Dis 16(3):198–202. https://doi.org/10.1111/codi.12513
Ramage L, Georgiou P, Tekkis P, Tan E (2015) Is robotic ventral mesh rectopexy better than laparoscopy in the treatment of rectal prolapse and obstructed defecation? A meta-analysis. Tech Coloproctol 19(7):381–389. https://doi.org/10.1007/s10151-015-1320-7
Wahed S, Ahmad M, Mohiuddin K, Katory M, Mercer-Jones M (2012) Short-term results for laparoscopic ventral rectopexy using biological mesh for pelvic organ prolapse. Color Dis 14(10):1242–1247. https://doi.org/10.1111/j.1463-1318.2011.02921.x
Mustain WC (2017) Functional disorders: rectocele. Clin Colon Rectal Surg 30(1):63–75. https://doi.org/10.1055/s-0036-1593425
Sileri P, Franceschilli L, de Luca E, Lazzaro S, Angelucci GP, Fiaschetti V, Pasecenic C, Gaspari AL (2012) Laparoscopic ventral rectopexy for internal rectal prolapse using biological mesh: postoperative and short-term functional results. J Gastrointest Surg 16(3):622–628. https://doi.org/10.1007/s11605-011-1793-2
Sileri P, Capuano I, Franceschilli L, Giorgi F, Gaspari AL (2014) Modified laparoscopic ventral mesh rectopexy. Tech Coloproctol 18(6):591–594. https://doi.org/10.1007/s10151-013-1094-8
Albayati S, Morgan MJ, Turner CE (2017) Laparoscopic ventral rectopexy for rectal prolapse and rectal intussusception using a biological mesh. Color Dis 19(9):857–862. https://doi.org/10.1111/codi.13671
Evans C, Stevenson AR, Sileri P, Mercer-Jones MA, Dixon AR, Cunningham C, Jones OM, Lindsey I (2015) A multicenter collaboration to assess the safety of laparoscopic ventral rectopexy. Dis Colon Rectum 58(8):799–807. https://doi.org/10.1097/DCR.0000000000000402
Balla A, Quaresima S, Smolarek S, Shalaby M, Missori G, Sileri P (2017) Synthetic versus biological mesh-related erosion after laparoscopic ventral mesh rectopexy: a systematic review. Ann Coloproctol 33(2):46–51. https://doi.org/10.3393/ac.2017.33.2.46
Abed H, Rahn DD, Lowenstein L, Balk EM, Clemons JL, Rogers RG, Systematic Review Group of the Society of Gynecologic Surgeons (2011) Incidence and management of graft erosion, wound granulation, and dyspareunia following vaginal prolapse repair with graft materials: a systematic review. Int Urogynecol J 22(7):789–798. https://doi.org/10.1007/s00192-011-1384-5
van Iersel JJ, Paulides TJ, Verheijen PM, Lumley JW, Broeders IA, Consten EC (2016) Current status of laparoscopic and robotic ventral mesh rectopexy for external and internal rectal prolapse. World J Gastroenterol 22(21):4977–4987. https://doi.org/10.3748/wjg.v22.i21.4977
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
K.E. Matzel is medical adviser to Medtronic.
M. Brunner has received an honorarium for lecturing at a Medtronic workshop.
Statement of human rights
For this type of study, formal consent is not required.
Statement on the welfare of animals
This article does not contain any studies with animals performed by any of the authors.
Informed consent
In this study, there is no identifying information of patients.
Rights and permissions
About this article
Cite this article
Brunner, M., Roth, H., Günther, K. et al. Ventral rectopexy with biological mesh: short-term functional results. Int J Colorectal Dis 33, 449–457 (2018). https://doi.org/10.1007/s00384-018-2972-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-018-2972-3