Abstract
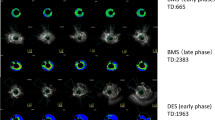
In-stent restenosis (ISR) is a common phenomenon with bare metal stents (BMSs) in the early stage after implantation. However, ISR occurs at a lower rate with long time after BMS implantation. We assessed changes over time in neointimal hyperplasia following BMS implantation using integrated backscatter intravascular ultrasound (IB-IUVS). Thirty-six patients who received target lesion revascularization (TLR) to treat ISR were classified according to the duration of the interval between stent implantation and TLR: the early group (within first year n = 25) and the VL group (very late ISR ≥5 years, n = 11). IB-IUVS was used to evaluate within-stent sites from the proximal to the distal edge of the stent. IB-IVUS color maps were then constructed by tracing the stent struts and vessel lumen. Neointimal tissue was classified as high-IB (IB <−29 dB; a representative cord of calcification), middle-IB (−49 dB ≤ IB < −29 dB; fibrosis), or low-IB (−49 dB ≤ IB; lipid pool). We compared percent (%) volume, average %area of cross-sectional area (CSA), and %area of minimum CSA of each component between the groups. There were no significant differences in %volume, average %area of CSA, or %area of minimum CSA for the high-IB component between groups. The %low-IB components were 20.0 ± 8.8 % for volume, 20.1 ± 8.9 % for mean CSA, and 17.6 ± 8.5 % for minimum CSA in the early group. On the other hand, in the VL group, the %low-IB components were significantly increased to 31.8 ± 7.9 % for volume (p < 0.01 vs. the early group), 31.2 ± 7.6 % for mean CSA (p < 0.01 vs. the early group), and 33.1 ± 12.3 % for minimum CSA (p < 0.01 vs. the early group). By contrast, the %middle-IB component showed a reduction in extended time, with %volume of the middle-IB decreasing from 78.3 ± 8.1 to 66.4 ± 7.1 %, average mean %area of CSA from 78.2 ± 8.2 to 66.9 ± 6.9 %, and % area of minimum CSA from 80.7 ± 7.9 to 65.5 ± 11.4 % (p < 0.01;. the early vs. the VL group). Our results suggest that in-stent neointimal tissues developing over time consist of an increased low-IB component and a decreased middle-IB component and may contribute an increased of lipidemic component and a decreased of fibrotic component.



Similar content being viewed by others
References
Tanaka S, Watanabe S, Matsuo H, Segawa T, Iwama M, Hirose T, Takahashi H, Ono K, Warita S, Kojima T, Minatoguchi S, Fujiwara H (2008) Prospective randomized trial comparing a nitinol self-expanding coronary stent with low-pressure dilatation and a high-pressure balloon expandable bare metal stent. Heart Vessels 23(1):1–8
Pepe M, Napodano M, Tarantini G, Fraccaro C, Cutolo A, Peluso D, Isabella G, Ramondo A, Iliceto S (2011) Percutaneous coronary intervention for unprotected left main disease in very high risk patients: safety of drug-eluting stents. Heart Vessels 26(1):17–24
Bauer T, Möllmann H, Zeymer U, Hochadel M, Nef H, Weidinger F, Zahn R, Hamm CW, Marco J, Gitt AK (2011) Multivessel percutaneous coronary intervention in patients with stable angina: a common approach? Lessons learned from the EHS PCI registry. Heart Vessels. doi:10.1007/s00380-011-0207-4
Grewe PH, Deneke T, Machraoui A, Barmeyer J, Müller KM (2000) Acute and chronic tissue response to coronary stent implantation: pathologic findings in human specimen. J Am Coll Cardiol 35(1):157–163
Wang CH, Hsieh IC, Cherng WJ, Chen CC, Tung TH, Lee JF, Lin SJ, Wang PN (2012) Differentiation profile of peripheral blood-derived vascular progenitor cell predicts intimal hyperplasia after coronary stenting. Heart Vessels 27(1):10–19
Kimura T, Abe K, Shizuta S, Odashiro K, Yoshida Y, Sakai K, Kaitani K, Inoue K, Nakagawa Y, Yokoi H, Iwabuchi M, Hamasaki N, Nosaka H, Nobuyoshi M (2002) Long-term clinical and angiographic follow-up after coronary stent placement in native coronary arteries. Circulation 105(25):2986–2991
Inoue K, Abe K, Ando K, Shirai S, Nishiyama K, Nakanishi M, Yamada T, Sakai K, Nakagawa Y, Hamasaki N, Kimura T, Nobuyoshi M, Miyamoto TA (2004) Pathological analyses of long-term intracoronary Palmaz–Schatz stenting; is its efficacy permanent? Cardiovasc Pathol 13(2):109–115
Nakazawa G, Otsuka F, Nakano M, Vorpahl M, Yazdani SK, Ladich E, Kolodgie FD, Finn AV, Virmani R (2011) The pathology of neoatherosclerosis in human coronary implants bare-metal and drug-eluting stents. J Am Coll Cardiol 57:1314–1322
Nakazawa G, Vorpahl M, Finn AV, Narula J, Virmani R (2009) One step forward and two steps back with drug-eluting-stents: from preventing restenosis to causing late thrombosis and nouveau atherosclerosis. JACC Cardiovasc Imaging 2(5):625–628
Yokoyama S, Takano M, Yamamoto M, Inami S, Sakai S, Okamatsu K, Okuni S, Seimiya K, Murakami D, Ohba T, Uemura R, Seino Y, Hata N, Mizuno K (2009) Extended follow-up by serial angioscopic observation for bare-metal stents in native coronary arteries: from healing response to atherosclerotic transformation of neointima. Circ Cardiovasc Interv 2(3):205–212
Takano M, Yamamoto M, Inami S, Murakami D, Ohba T, Seino Y, Mizuno K (2009) Appearance of lipid-laden intima and neovascularization after implantation of bare-metal stents extended late-phase observation by intracoronary optical coherence tomography. J Am Coll Cardiol 55(1):26–32
Habara M, Terashima M, Nasu K, Kaneda H, Inoue K, Ito T, Kamikawa S, Kurita T, Tanaka N, Kimura M, Kinoshita Y, Tsuchikane E, Matsuo H, Ueno K, Katoh O, Suzuki T (2011) Difference of tissue characteristics between early and very late restenosis lesions after bare-metal stent implantation: an optical coherence tomography study. Circ Cardiovasc Interv 4:232–238
Hou J, Qi H, Zhang M, Ma L, Liu H, Han Z, Meng L, Yang S, Zhang S, Yu B, Jang IK (2010) Development of lipid-rich plaque inside bare metal stent: possible mechanism of late stent thrombosis? An optical coherence tomography study. Heart 96(15):1187–1190
Kawasaki M, Takatsu H, Noda T, Sano K, Ito Y, Hayakawa K, Tsuchiya K, Arai M, Nishigaki K, Takemura G, Minatoguchi S, Fujiwara T, Fujiwara H (2002) In vivo quantitative tissue characterization of human coronary arterial plaques by use of integrated backscatter intravascular ultrasound and comparison with angioscopic findings. Circulation 105(21):2487–2492
Okubo M, Kawasaki M, Ishihara Y, Takeyama U, Kubota T, Yamaki T, Ojio S, Nishigaki K, Takemura G, Saio M, Takami T, Minatoguchi S, Fujiwara H (2008) Development of integrated backscatter intravascular ultrasound for tissue characterization of coronary plaques. Ultrasound Med Biol 34(4):655–663
Okubo M, Kawasaki M, Ishihara Y, Takeyama U, Yasuda S, Kubota T, Tanaka S, Yamaki T, Ojio S, Nishigaki K, Takemura G, Saio M, Takami T, Fujiwara H, Minatoguchi S (2008) Tissue characterization of coronary plaques: comparison of integrated backscatter intravascular ultrasound with virtual histology intravascular ultrasound. Circ J 72(10):1631–1639
Nakayama A, Morita H, Ando J, Fujita H, Ohtsu H, Nagai R (2012) Adverse cardiovascular outcomes associated with concurrent use of clopidogrel or ticlopidine and proton-pump inhibitors in patients undergoing percutaneous coronary intervention. Heart Vessels. doi:10.1007/s00380-012-0248-3
Brott BC (2009) Late vascular healing response to stents: new insights from optical coherence tomography. J Am Coll Cardiol 55(1):33–34
Kang SJ, Mintz GS, Park DW, Lee SW, Kim YH, Lee CW, Han KH, Kim JJ, Park SW, Park SJ (2010) Tissue characterization of in-stent neointima using intravascular ultrasound radiofrequency data analysis. Am J Cardiol 106(11):1561–1565
Wakabayashi K, Mintz G, Delhaye C, Choi YJ, Doh JH, Ben-Dor I, Gaglia M Jr, Pakala R, Suddath W, Satler L, Kent K, Pichard A, Weissman N, Waksman R (2011) In vivo virtual histology intravascular ultrasound comparison of neointimal hyperplasia within drug-eluting- versus bare metal stents. J Invasive Cardiol 23(7):262–268
Komatsu R, Ueda M, Naruko T, Kojima A, Becker AE (1998) Neointimal tissue response at sites of coronary stenting in humans: macroscopic, histological, and immunohistochemical analyses. Circulation 98(3):224–233
Chieffo A, Foglieni C, Nodari RL, Briguori C, Sangiorgi G, Latib A, Montorfano M, Airoldi F, Michev I, Carlino M, Colombo A, Maseri A (2009) Histopathology of clinical coronary restenosis in drug-eluting versus bare metal stents. Am J Cardiol 104:1660–1667
Finn AV, Nakazawa G, Joner M, Kolodgie FD, Mont EK, Gold HK, Virmani R (2007) Vascular responses to drug eluting stents: importance of delayed healing. Arterioscler Thromb Vasc Biol 27(7):1500–1510
Sano K, Kawasaki M, Ishihara Y, Okubo M, Tsuchiya K, Nishigaki K, Zhou X, Minatoguchi S, Fujita H, Fujiwara H (2006) Assessment of vulnerable plaques causing acute coronary syndrome using integrated backscatter intravascular ultrasound. J Am Coll Cardiol 47(4):734–741
Takano M, Mizuno K, Yokoyama S, Seimiya K, Ishibashi F, Okamatsu K, Uemura R (2003) Changes in coronary plaque color and morphology by lipid-lowering therapy with atorvastatin: serial evaluation by coronary angioscopy. J Am Coll Cardiol 42(4):680–686
Serruys PW, de Feyter P, Macaya C, Kokott N, Puel J, Vrolix M, Branzi A, Bertolami MC, Jackson G, Strauss B, Meier B, Lescol Intervention Prevention Study (LIPS) Investigators (2002) Fluvastatin for prevention of cardiac events following successful first percutaneous coronary intervention: a randomized controlled trial. JAMA 287(24):3215–3222
Tanaka S, Yokoyama C, Kawamura I, Takasugi N, Kubota T, Ushikoshi H, Aoyama T, Kawasaki M, Nishigaki K, Takemura G, Minatoguchi S (2008) Conservative medication follow-up for over 20 years of a patient with ischemic heart disease after diagnosis of chronic total occlusion of the 3 main coronary arteries. Circ J. 72(7):1205–1209
Acknowledgments
Reiko Matsuoka, MD, Shintaro Abe, MD, Yoshiaki Goto, MD, Takashi Yoshizane, MD, Takashi Kato MD, Tomoko Hirose, MD, Shunichiro Warita, MD, Tai Kojima, MD, Takeshi Hirose, MD and Koji Ono, MD, participated in data collection for this study. We thank Mr. Kaoru Kawasaki and Mr. Yoshiaki Kodera for their technical support with the experimental equipment.
Conflict of interest
None of the authors has any conflicts of interest pertaining to this manuscript, nor any commercial relationships with the products and devices described.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tanaka, S., Noda, T., Iwama, M. et al. Long-term changes in neointimal hyperplasia following implantation of bare metal stents assessed by integrated backscatter intravascular ultrasound. Heart Vessels 28, 415–423 (2013). https://doi.org/10.1007/s00380-012-0266-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-012-0266-1