Abstract
Objective
To assess the outcome of low risk prostate cancer (PCa) patients who were candidates for active surveillance (AS) but had undergone robot-assisted radical prostatectomy (RARP).
Method
We reviewed our prospectively collected database of patients operated by RARP between 2006 and 2014. Low D’Amico risk patients were selected. Oncological outcomes were reported based on pathology results and biochemical failure. Functional outcomes on continence and potency were reported at 12 and 24 months. Continence was assessed by the number of pads per day. With respect to potency, it was assessed using the Sexual Health Inventory for Men (SHIM) and Erectile Hardness Scale (EHS).
Results
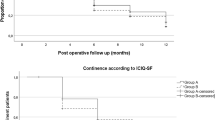
Out of 812 patients, 237 (29.2%) patients were D’Amico low risk and were eligible for analysis. 44 men fit Epstein’s criteria. 134 (56.5%) men had pathological upgrading. Age and clinical stage were predictors of upgrading on multivariate analysis. 220 (92.8%) patients had available follow-up for biochemical recurrence, potency, and continence for 2 years. The mean and median follow-up was 34.8 and 31.4 months, respectively. Only 5 (2.3%) men developed BCR, all of whom had pathological upgrading. Extra capsular extension and positive surgical margins were observed in 14.8 and 19.1%, respectively. 0 pad was achieved in 86.7 and 88.9% at 1 and 2 years, respectively. Proportion of patients with SHIM > 21 at 1 and 2 years was 24.8 and 30.6%, respectively. Moreover, patients having erections adequate for intercourse (EHS ≥ 3) were seen in 69.6 and 83.1% at 1 and 2 years, respectively. Functional outcomes of patients fitting Epstein’s criteria (n = 44) and patients with no upgrading on final pathology (n = 103) were not significantly different compared to the overall low risk study group.
Conclusion
This retrospective study showed that RARP is not without harm even in patients with low risk disease. On the other hand, considerable rate of upgrading was noted.
Similar content being viewed by others
Abbreviations
- AS:
-
Active surveillance
- BCR:
-
Biochemical recurrence
- CI:
-
Confidence interval
- CSS:
-
Cancer specific survival
- EHS:
-
Erectile Hardness Scale
- ECE:
-
Extra capsular extension
- LUTS:
-
Lower urinary tract symptoms
- OR:
-
Odds ratio
- OS:
-
Overall survival
- PCa:
-
Prostate cancer
- PSM:
-
Positive surgical margin
- RARP:
-
Robot-assisted radical prostatectomy
- RP:
-
Radical prostatectomy
- RRP:
-
Retropubic radical prostatectomy
- RT:
-
Radiotherapy
- SHIM:
-
Sexual Health Inventory for Men
References
Bill-Axelson A, Holmberg L, Filén F et al (2008) Radical prostatectomy versus watchful waiting in localized prostate cancer: the Scandinavian prostate cancer group-4 randomized trial. J Natl Cancer Inst 100:1144–1154. https://doi.org/10.1093/jnci/djn255
Andersson S-O, Andrén O, Lyth J et al (2011) Managing localized prostate cancer by radical prostatectomy or watchful waiting: cost analysis of a randomized trial (SPCG-4). Scand J Urol Nephrol 45:177–183. https://doi.org/10.3109/00365599.2010.545075
Wilt TJ, Brawer MK, Jones KM et al (2012) Radical prostatectomy versus observation for localized prostate cancer. N Engl J Med 367:203–213. https://doi.org/10.1056/NEJMoa1113162
Kwon O, Hong S (2014) Active surveillance and surgery in localized prostate cancer. Minerva Urol E Nefrol Ital J Urol Nephrol 66:175–187
D’Amico AV, Whittington R, Malkowicz SB et al (1998) Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA 280:969–974
Lee MC, Dong F, Stephenson AJ et al (2010) The Epstein criteria predict for organ-confined but not insignificant disease and a high likelihood of cure at radical prostatectomy. Eur Urol 58:90–95. https://doi.org/10.1016/j.eururo.2009.10.025
eau 2016 guidelines prostate cancer—Google Search. https://www.google.fr/#q=eau+2016+guidelines+prostate+cancer. Accessed 29 Oct 2016
Musunuru HB, Yamamoto T, Klotz L et al (2016) Active surveillance for intermediate risk prostate cancer: survival outcomes in the Sunnybrook experience. J Urol 196:1651–1658. https://doi.org/10.1016/j.juro.2016.06.102
El Hajj A, Ploussard G, de la Taille A et al (2013) Analysis of outcomes after radical prostatectomy in patients eligible for active surveillance (PRIAS). BJU Int 111:53–59. https://doi.org/10.1111/j.1464-410X.2012.11276.x
Vellekoop A, Loeb S, Folkvaljon Y, Stattin P (2014) Population based study of predictors of adverse pathology among candidates for active surveillance with Gleason 6 prostate cancer. J Urol 191:350–357. https://doi.org/10.1016/j.juro.2013.09.034
Carlsson S, Jäderling F, Wallerstedt A et al (2016) Oncological and functional outcomes 1 year after radical prostatectomy for very-low-risk prostate cancer: results from the prospective LAPPRO trial. BJU Int 118:205–212. https://doi.org/10.1111/bju.13444
Mizuno K, Inoue T, Kinoshita H et al (2016) Evaluation of predictors of unfavorable pathological features in men eligible for active surveillance using radical prostatectomy specimens: a multi-institutional study. Jpn J Clin Oncol 46:1156–1161. https://doi.org/10.1093/jjco/hyw130
Klotz L, Vesprini D, Sethukavalan P et al (2015) Long-term follow-up of a large active surveillance cohort of patients with prostate cancer. J Clin Oncol Off J Am Soc Clin Oncol 33:272–277. https://doi.org/10.1200/JCO.2014.55.1192
Godtman RA, Holmberg E, Khatami A et al (2013) Outcome following active surveillance of men with screen-detected prostate cancer. Results from the Göteborg randomised population-based prostate cancer screening trial. Eur Urol 63:101–107. https://doi.org/10.1016/j.eururo.2012.08.066
Bill-Axelson A, Holmberg L, Garmo H et al (2014) Radical prostatectomy or watchful waiting in early prostate cancer. N Engl J Med 370:932–942. https://doi.org/10.1056/NEJMoa1311593
Hamdy FC, Donovan JL, Lane JA et al (2016) 10-year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N Engl J Med 375:1415–1424. https://doi.org/10.1056/NEJMoa1606220
Druskin SC, Macura KJ (2018) MR imaging for prostate cancer screening and active surveillance. Radiol Clin N Am 56:251–261. https://doi.org/10.1016/j.rcl.2017.10.006
Cuzick J, Berney DM, Fisher G et al (2012) Prognostic value of a cell cycle progression signature for prostate cancer death in a conservatively managed needle biopsy cohort. Br J Cancer 106:1095–1099. https://doi.org/10.1038/bjc.2012.39
Crawford ED, Scholz MC, Kar AJ et al (2014) Cell cycle progression score and treatment decisions in prostate cancer: results from an ongoing registry. Curr Med Res Opin 30:1025–1031. https://doi.org/10.1185/03007995.2014.899208
Klein EA, Cooperberg MR, Magi-Galluzzi C et al (2014) A 17-gene assay to predict prostate cancer aggressiveness in the context of Gleason grade heterogeneity, tumor multifocality, and biopsy undersampling. Eur Urol 66:550–560. https://doi.org/10.1016/j.eururo.2014.05.004
Cullen J, Rosner IL, Brand TC et al (2015) A biopsy-based 17-gene genomic prostate score predicts recurrence after radical prostatectomy and adverse surgical pathology in a racially diverse population of men with clinically low- and intermediate-risk prostate cancer. Eur Urol 68:123–131. https://doi.org/10.1016/j.eururo.2014.11.030
Wilt TJ, Jones KM, Barry MJ et al (2017) Follow-up of prostatectomy versus observation for early prostate cancer. N Engl J Med 377:132–142. https://doi.org/10.1056/NEJMoa1615869
Donovan MJ, Cordon-Cardo C (2014) Genomic analysis in active surveillance: predicting high-risk disease using tissue biomarkers. Curr Opin Urol 24:303–310. https://doi.org/10.1097/MOU.0000000000000051
Donovan JL, Hamdy FC, Lane JA et al (2016) Patient-reported outcomes after monitoring, surgery, or radiotherapy for prostate cancer. N Engl J Med 375:1425–1437. https://doi.org/10.1056/NEJMoa1606221
Ficarra V, Novara G, Rosen RC et al (2012) Systematic review and meta-analysis of studies reporting urinary continence recovery after robot-assisted radical prostatectomy. Eur Urol 62:405–417. https://doi.org/10.1016/j.eururo.2012.05.045
Wallerstedt A, Carlsson S, Steineck G et al (2013) Patient and tumour-related factors for prediction of urinary incontinence after radical prostatectomy. Scand J Urol 47:272–281. https://doi.org/10.3109/00365599.2012.733410
Steineck G, Bjartell A, Hugosson J et al (2015) Degree of preservation of the neurovascular bundles during radical prostatectomy and urinary continence 1 year after surgery. Eur Urol 67:559–568. https://doi.org/10.1016/j.eururo.2014.10.011
Sanda MG, Dunn RL, Michalski J et al (2008) Quality of life and satisfaction with outcome among prostate-cancer survivors. N Engl J Med 358:1250–1261. https://doi.org/10.1056/NEJMoa074311
Bill-Axelson A, Garmo H, Holmberg L et al (2013) Long-term distress after radical prostatectomy versus watchful waiting in prostate cancer: a longitudinal study from the Scandinavian Prostate Cancer Group-4 randomized clinical trial. Eur Urol 64:920–928. https://doi.org/10.1016/j.eururo.2013.02.025
Ficarra V, Novara G, Ahlering TE et al (2012) Systematic review and meta-analysis of studies reporting potency rates after robot-assisted radical prostatectomy. Eur Urol 62:418–430. https://doi.org/10.1016/j.eururo.2012.05.046
Haglind E, Carlsson S, Stranne J et al (2015) Urinary incontinence and erectile dysfunction after robotic versus open radical prostatectomy: a prospective, controlled, nonrandomised trial. Eur Urol 68:216–225. https://doi.org/10.1016/j.eururo.2015.02.029
Van den Bergh RCN, Korfage IJ, Roobol MJ et al (2012) Sexual function with localized prostate cancer: active surveillance vs radical therapy. BJU Int 110:1032–1039. https://doi.org/10.1111/j.1464-410X.2011.10846.x
Mulhall JP (2009) Defining and reporting erectile function outcomes after radical prostatectomy: challenges and misconceptions. J Urol 181:462–471. https://doi.org/10.1016/j.juro.2008.10.047
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zanaty, M., Ajib, K., Zorn, K. et al. Functional outcomes of robot-assisted radical prostatectomy in patients eligible for active surveillance. World J Urol 36, 1391–1397 (2018). https://doi.org/10.1007/s00345-018-2298-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2298-3