Abstract
Background
Amnion-derived multipotent progenitor (AMP) cells, unlike most stem cells, have been demonstrated to be nontumorigenic and nonimmunogenic. Amnion-derived cellular cytokine solution (ACCS), a secreted product of AMP cells, is a cocktail of cytokines existing at physiological levels and has been used to accelerate epithelialization of experimental partial-thickness burns.
Methods
Using modifications of Zawacki’s guinea pig partial-thickness scald burn model, a total of 65 animals were treated with ACCS, ACCS + AMP cells, unconditioned medium (UCM) + AMP cells, or either UCM alone or saline as controls. Dosage times ranged from every other day to once a week. Percent epithelialization was serially determined from acetate wound tracings. Histology was performed on wound biopsies.
Results
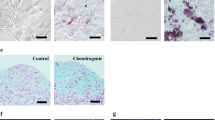
ACCS, UCM + AMP cells, and ACCS + AMP cells improved epithelialization compared with the two control groups (P < 0.05). When ACCS was delivered more frequently, statistically significant more rapid epithelialization occurred (P < 0.05). By day 7, all groups treated with ACCS had reached at least 90% epithelialization, whereas control groups were only 20–40% epithelialized (P < 0.05). Histology showed excellent regeneration of the epidermis with rete ridge formation. Hair growth occurred in ACCS-treated animals but not in the control group.
Conclusions
Amnion-derived cellular cytokine solution accelerates the healing of experimental partial-thickness burns. Based on these findings, a multicenter clinical trial is underway.





Similar content being viewed by others
References
Xing L, Franz MG, Marcelo CL et al (2007) Amnion-derived multipotent progenitor cells increase gain of incisional breaking strength and decrease incidence and severity of acute wound failure. J Burns Wounds 7:39–52
Franz MG, Payne WG, Xing L et al (2008) The use of amnion-derived cellular cytokine solution to improve healing in acute and chronic wound models. ePlasty 8:188–199
Uberti MG, Ko F, Pierpont YN et al (2009) The use of amnion-derived cellular cytokine solution (ACCS) in accelerating closure of interstices in explanted meshed human skin grafts. ePlasty 9:113–119
Banas RA, Trumpower C, Bentlejewski C et al (2008) Immunogenicity and immunomodulatory effects of amnion-derived multipotent progenitor cells. Hum Immunol 69:321–328
Steed DL, Trumpower C, Duffy D et al (2008) Amnion-derived cellular cytokine solution: a physiological combination of cytokines for wound healing. ePlasty 8:157–165
Saranto JR, Rubayi S, Zawacki BE (1983) Blisters, cooling, antithromboxanes, and healing in experimental zone-of-stasis burns. J Trauma 23:927–933
Zawacki BE (1974) Reversal of capillary stasis and prevention of necrosis in burns. Ann Surg 180:98–102
DelBeccaro EJ, Robson MC, Heggers JP et al (1980) The use of specific thromboxane inhibitors to preserve the dermal microcirculation after burning. Surgery 87:137–141
Robson MC, DelBeccaro EJ, Heggers JP et al (1980) Increasing dermal perfusion after burning by decreasing thromboxane production. J Trauma 20:722–725
Hammond SA, Tsonis C, Sellins K et al (2000) Transcutaneous immunization of domestic animals: opportunities and challenges. Adv Drug Deliv Rev 43:45–55
Hokanson JA, Hayward PG, Carney DH et al (1992) A mathematical model for the analysis of experimental wound healing data. Wounds 3:213–220
Han SK, Toon TH, Lee DG et al (2005) Potential of human bone marrow stromal cells to accelerate wound healing in vitro. Ann Plast Surg 55:414–419
Dvonch WM, Murphey RJ, Matsuoka J et al (1992) Changes in growth factor levels in human wound fluid. Surgery 112:18–23
Acknowledgments
This material is the result of work supported with resources and the use of facilities at the Bay Pines VA Healthcare System, Bay Pines, Florida. The authors acknowledge the work of Deepak N. Naidu, MD and R. Emerick Salas, MD, who served as postdoctoral research fellows and participated in the conduct of the two experiments, providing surgical care and treatment to the animals. The work was supported in part by a grant from the Department of Defense (USAMRAA 06153010).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Payne, W.G., Wachtel, T.L., Smith, C.A. et al. Effect of Amnion-Derived Cellular Cytokine Solution on Healing of Experimental Partial-Thickness Burns. World J Surg 34, 1663–1668 (2010). https://doi.org/10.1007/s00268-010-0420-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-010-0420-9