Abstract
Background
The number of patients undergoing mastectomy and immediate breast reconstruction with tissue expanders followed by post-mastectomy radiotherapy (PMRT) is exponentially increasing. To reduce the rate of complications, in 2011, the senior author of this manuscript described the use of protective lipofilling in patients undergoing unplanned PMRT to the expander with a specific protocol aiming to decrease the rate of complications.
Objectives
A study was performed to evaluate the thickness of the breast irradiated tissue to create a standard pattern of “protective” lipofilling infiltration on limited key areas that could re-establish a thickness similar to non-radiotreated tissues.
Methods
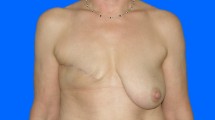
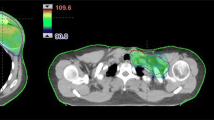
We studied 15 patients who had modified radical mastectomy (MRM) with immediate breast reconstruction with tissue expanders and PMRT (Group 1) before expansion (Time1), before PMRT (Time2), after PMRT (Time3), 3 months after “protective” lipofilling (Time4), and 6 months after “protective” lipofilling (Time5). As a control group, we studied 15 patients who had MRM and immediate breast reconstruction with tissue expanders that would not undergo PMRT (Group 2) at the same time points of GROUP 1 (Time1,2,3). Tissue thickness was studied in specific areas using ultrasounds (US) and magnetic resonance imaging (MRI).
Results
US and MRI measurements obtained 6 weeks after PMRT and 3 months after lipofilling showed an initial decrease and then an average increase in tissue thickness reaching values even higher than the non-radiotreated control group.
Conclusions
This preliminary report shows how a one-step “fat belt” surgical pattern of lipofilling delivered to central “selected” areas of the breast can achieve adequate tissue thickness in patients who underwent breast reconstruction with PMRT reaching a thickness similar (and in most cases higher) to non-radiotreated tissues. Further follow-up studies are needed to analyze long-term complications of tissue thinning such as ulceration and implant exposure, in comparison with the “fat capsule” pattern.
Level of Evidence IV
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.









Similar content being viewed by others
References
Ragaz J, Olivotto IA, Spinelli JJ, Phillips N, Jackson SM, Wilson KS, Knowling MA, Coppin CM, Weir L, Gelmon K, Le N, Durand R, Coldman AJ, Manji M (2005) Locoregional radiation therapy in patients with high-risk breast cancer receiving adjuvant chemotherapy: 20-year results of the British Columbia randomized trial. J Natl Cancer Inst 97:116–126
Overgaard M, Nielsen HM, Overgaard J (2007) Is the benefit of postmastectomy irradiation limited to patients with four or more positive nodes, as recommended in international consensus reports? A subgroup analysis of the DBCG 82 b&c randomized trials. Radiother Oncol 82:247–253
NATIONAL COMPREHENSIVE CANCER NETWORK (NCCN) (2008) Clinical practice guidelines in oncology: breast cancer ver. 1.2009. NCCN, Fort Washington
SUPREMO, an MRC Phase III randomised trial to assess the role of adjuvant chest wall irradiationin“intermediate risk” operable breast cancer following mastectomy. http://www.controlled-trials.com/ISRCTN61145589. Accessed 4–11 Jan 2009
Katz A, Strom EA, Buchholz TA, Theriault R, Singletary SE, Mcneese MD (2001) The influence of pathologic tumor characteristics on locoregional recurrence rates following mastectomy. Int J Radiat Oncol Biol Phys 50:735–742
Baildam A, Bishop H, Boland G, Dalglish M, Davies L, Fatah F, Gooch H, Harcourt D, Martin L, Rainsbury D, Rayter Z, Sheppard C, Smith J (2007) Weiler-Mithoff EEe, Winstanley J, Church J. Association of breast surgery at Baso, association of breast surgery at Bapras, training interface group in breast surgery, oncoplastic breast surgery—a guide to good practice. Eur J Surg Oncol 33(Suppl 1):S1–S23
Overgaard M, Jensen MB, Overgaard J et al (1999) Postoperative radiotherapy in high-risk postmenopausal breast-cancer patients given adjuvant tamoxifen: Danish Breast Cancer Cooperative Group DBCG 82c randomised trial. Lancet 353:1641–1648
Whelan TJ, Olivotto I, Ackerman I et al (2011) NCIG-CTG MA- 20: an intergroup trial of regional nodal irradiation in breast Cancer. J Clin Oncol. Abstract presented at the 2011 ASCO annual meeting
Frasier LL, Holden S, Holden T, Schumacher JR, Leverson G, Anderson B, Greenberg CC, Neuman HB (2016) Temporal trends in postmastectomy radiation therapy and breast reconstruction associated with changes in national comprehensive cancer network guidelines. JAMA Oncol 2(1):95–101
Meattini I, Cecchini S, Muntoni C, Scotti V, De Luca Cardillo C, Mangoni M, Bonomo P, Nori J, Casella D, Simoncini R, Orzalesi L, Bianchi S, Livi L (2014) Cutaneous and cardiac toxicity of concurrent trastuzumab and adjuvant breast radiotherapy: a single institution series. Med Oncol 31(4):891
Lam TC, Hsieh F, Boyages J (2013) The effects of postmastectomy adjuvant radiotherapy on immediate two-stage prosthetic breast reconstruction: a systematic review. Plast Reconstr Surg 132(3):511–518
Anker CJ, Hymas RV, Ahluwalia R, Kokeny KE, Avizonis V, Boucher KM, Neumayer LA, Agarwal JP (2015) The effect of radiation on complication rates and patient satisfaction in breast reconstruction using temporary tissue expanders and permanent implants. Breast J 21(3):233–240
El-Sabawi B, Carey JN, Hagopian TM, Sbitany H, Patel KM (2016) Radiation and breast reconstruction: algorithmic approach and evidence-based outcomes. J Surg Oncol. https://doi.org/10.1002/jso.24143
Voineskos SH, Frank SG, Cordeiro PG (2015) Breast reconstruction following conservative mastectomies: predictors of complications and outcomes. Gland Surg 4(6):484–496
Ribuffo D, Atzeni M, Serratore F, Guerra M, Bucher S (2011) Cagliari University Hospital (CUH) protocol for immediate alloplastic breast reconstruction and unplanned radiotherapy. A preliminary report. Eur Rev Med Pharmacol Sci 15:840–844
Ribuffo D, Atzeni M, Guerra M et al (2013) Treatment of irradiated expanders: protective lipofilling allows immediate prosthetic breast reconstruction in the setting of postoperative radiotherapy. Aesthetic Plast Surg 37:1146–1152
Lo Torto F, Vaia N, Casella D, Marcasciano M, Cigna E, Ribuffo D (2017) Delaying implant-based mammary reconstruction after radiotherapy does not decrease capsular contracture: an in vitro study. J Plast Reconstr Aesthet Surg 70:1210–1217
Lo Torto F, Vaia N, Casella D, Marcasciano M, Cigna E, Ribuffo D (2018) Delaying implant-based mammary reconstruction after radiotherapy does not decrease capsular contracture: an in vitro study. J Plast Reconstr Aesthet Surg 71:28–29
Lo Torto F, Vaia N, Ribuffo D (2017) Postmastectomy radiation therapy and two-stage implant-based breast reconstruction: is there a better time to irradiate? Plast Reconstr Surg 139(6):1364e–1365e
Ribuffo D, Vaia N, Petrianni GM (2016) Comparison of delayed and immediate tissue expander breast reconstruction in the setting of postmastectomy radiation therapy. Ann Plast Surg 76(6):743–744
Bonomi S, Misani M, Settembrini F (2012) Radiotherapy and implant-based, two-stage breast reconstruction: how to minimize complications and maximize aesthetic outcomes. Plast Reconstr Surg 130:745e–748e
Maione L, Forcellini D, Vinci V, Lisa A, Caviggioli A, Klinger F (2012) The effects of postmastectomy adjuvant radiotherapy on immediate two-stage prosthetic breast reconstruction: a systematic review. Plast Reconstr Surg 133:729e–730e
La Radioterapia dei Tumori della Mammella Indicazioni e Criteri Guida—AIRO 2013 guidelines
Dessy LA, Marcasciano M, Rossi A, Mazzocchi M (2015) Response to “comments on a simple device for syringe-to-syringe transfer during lipofilling”. Aesthet Surg J 35(7):NP242-3
Dessy LA, Marcasciano M, Pacitti F, Rossi A, Mazzocchi M (2015) A simple device for syringe-to-syringe transfer during lipofilling. Aesthet Surg J 35(1):91–93
Cordeiro PG (2012) Discussion. In: Kronowitz SJ (ed) Current status of implant-based breast reconstruction in patients receiving postmastectomy radiation therapy. Plast Reconstr Surg 130: 513e
Kane WJ, McCaffrey TV, Wang TD et al (1992) The effect of tissue expansion on previously irradiated skin. Arch Otolaryngol Head Neck Surg 118:419–426
Fajardo LF, Berthrong M (1988) Vascular lesions following radiation. Pathol Annu 23:297–330
Goodman CM, Miller R, Patrick CW Jr et al (2002) Radiotherapy: effects on expanded skin. Plast Reconstr Surg 110:1080–1083
Lo Torto F, Cigna E, Kaciulyte J, Casella D, Marcasciano M, Ribuffo D (2017) National breast reconstruction utilization in the setting of postmastectomy radiotherapy: two-stage implant-based breast reconstruction. J Reconstr Microsurg. https://doi.org/10.1055/s-0037-1604389
Pallua N, Pulsfort AK, Suschek C, Wolter TP (2009) Content of the growth factors bFGF, IGF-1, VEGF, and PDGF-BB in freshly harvested lipoaspirate after centrifugation and incubation. Plast Reconstr Surg 123:826e33
Yamaguchi M, Matsumoto F, Bujo H et al (2005) Revascularization determines volume retention and gene expression by fat grafts in mice. Exp Biol Med (Maywood) 230:742e8
Pallua N, Baroncini A, Alharbi Z, Stromps JP (2014) Improvement of facial scar appearance and microcirculation by autologous lipofilling. J Plast Reconstr Aesthet Surg 67(8):1033–1037
Acknowledgements
The authors certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Vaia, N., Lo Torto, F., Marcasciano, M. et al. From the “Fat Capsule” to the “Fat Belt”: Limiting Protective Lipofilling on Irradiated Expanders for Breast Reconstruction to Selective Key Areas. Aesth Plast Surg 42, 986–994 (2018). https://doi.org/10.1007/s00266-018-1120-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-018-1120-3