Abstract
Purpose
Because of toxicities, benzodiazepines are not usually recommended in older adults. We therefore sought to describe the trends in benzodiazepine use in long-term care and examine the variation in benzodiazepine use among nursing homes.
Methods
In this retrospective repeated cross-sectional analysis of Medicare Parts A, B, and D claims data linked to the Minimum Data Set from 2013 to 2018, we included long-term residents who stayed in a nursing home for at least one entire quarter of a calendar year in 2013–2018. The outcome was whether residents were prescribed a benzodiazepine drug for at least 30 days during each quarter stay. We use mixed effects logistic regression models to assess the variation in benzodiazepine use among nursing homes, adjusting for patient and nursing home characteristics.
Results
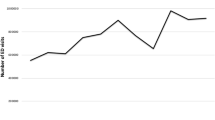
The cohort for the time trend analysis included 270,566 unique residents and 1,843,580 quarter stays for 2013–2018. Prescribing rates for short-acting benzodiazepines were stable over 2013–2016, then declined from 12.1% in 2016 to 10.6% in 2018. The rate of long-acting benzodiazepine use remained relatively steady at around 4% over 2013–2018. During 2017–2018, the variation among nursing homes in benzodiazepine use was 7.2% for short-acting vs. 9.3% for long-acting benzodiazepines, after controlling for resident characteristics.
Conclusion
Prescribing for short-acting benzodiazepines in long-term care declined after 2016, while long-acting benzodiazepine use did not change. The variation in benzodiazepine use among nursing homes is substantial. Identifying factors that explain this variation may help in developing strategies for deprescribing benzodiazepines in nursing home residents.

Similar content being viewed by others
Availability of data and material
The datasets generated during and/or analyzed during the current study are available from the Research Data Assistance Center, The Centers for Medicare and Medicaid Services, https://www.cms.gov/Research-Statistics-Data-and-Systems/Research/ResearchGenInfo/ResearchDataAssistanceCenter.
Change history
16 July 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00228-022-03360-9
References
Woolcott JC, Richardson KJ, Wiens MO et al (2009) Meta-analysis of the impact of 9 medication classes on falls in elderly persons. Arch Intern Med 169:1952–1960. https://doi.org/10.1001/archinternmed.2009.357
Wang PS, Bohn RL, Glynn RJ, Mogun H, Avorn J (2001) Hazardous benzodiazepine regimens in the elderly: effects of half-life, dosage, and duration on risk of hip fracture. Am J Psychiatry 158:892–898. https://doi.org/10.1176/appi.ajp.158.6.892
Tannenbaum C, Paquette A, Hilmer S, Holroyd-Leduc J, Carnahan R (2012) A systematic review of amnestic and non-amnestic mild cognitive impairment induced by anticholinergic, antihistamine, GABAergic and opioid drugs. Drugs Aging 29:639–658. https://doi.org/10.1007/bf03262280
Maust DT, Blow FC, Wiechers IR, Kales HC, Marcus SC (2017) National trends in antidepressant, benzodiazepine, and other sedative-hypnotic treatment of older adults in psychiatric and primary care. J Clin Psychiatry 78:e363–e371. https://doi.org/10.4088/JCP.16m10713
Ray WA (1989) Benzodiazepines of long and short elimination half-life and the risk of hip fracture. JAMA 262(23):3303. https://doi.org/10.1001/jama.1989.03430230088031
Beers MH (1997) Explicit criteria for determining potentially inappropriate medication use by the elderly. Arch Intern Med 157:1531. https://doi.org/10.1001/archinte.1997.00440350031003
Fick DM, Cooper JW, Wade WE, Waller JL, Maclean JR, Beers MH (2003) Updating the Beers Criteria for potentially inappropriate medication use in older adults. Arch Intern Med 163:2716. https://doi.org/10.1001/archinte.163.22.2716
Wagner AK, Zhang F, Soumerai SB et al (2004) Benzodiazepine use and hip fractures in the elderly. Arch Intern Med 164:1567. https://doi.org/10.1001/archinte.164.14.1567
Fick DM, Semla TP, Steinman M et al (2019) American Geriatrics Society 2019 Updated AGS Beers Criteria® for potentially inappropriate medication use in older adults. J Am Geriatr Soc 67:674–694. https://doi.org/10.1111/jgs.15767
Bykov K, He M, Gagne JJ (2020) Trends in utilization of prescribed controlled substances in US commercially insured adults, 2004–2019. JAMA Intern Med 180:1006. https://doi.org/10.1001/jamainternmed.2020.0989
Chen H, Nwangwu A, Aparasu R, Essien E, Sun S, Lee K (2008) The impact of Medicare Part D on psychotropic utilization and financial burden for community-based seniors. Psychiatr Serv 59:1191–1197. https://doi.org/10.1176/ps.2008.59.10.1191
Ong MK, Xu H, Zhang L, Azocar F, Ettner SL (2012) Effect of Medicare Part D benzodiazepine exclusion on psychotropic use in benzodiazepine users. J Am Geriatr Soc 60:1292–1297. https://doi.org/10.1111/j.1532-5415.2012.04031.x
Centers for Medicare & Medicaid Services (CMS) (2012) Transition to Part D coverage of benzodiazepines and barbiturates beginning in 2013. CMS web page. 1927:21244. https://www.cms.gov/Medicare/Prescription-Drug-Coverage/PrescriptionDrugCovContra/Downloads/BenzoandBarbituratesin2013.pdf Access date October 29, 2021.
Agarwal SD, Landon BE (2019) Patterns in outpatient benzodiazepine prescribing in the United States. JAMA Netw Open 2:e187399. https://doi.org/10.1001/jamanetworkopen.2018.7399
Maust DT, Kim HM, Chiang C, Kales HC (2018) Association of the Centers for Medicare & Medicaid Services’ national partnership to improve dementia care with the use of antipsychotics and other psychotropics in long-term care in the United States from 2009 to 2014. JAMA Intern Med 178:640–647. https://doi.org/10.1001/jamainternmed.2018.0379
Vu MQ, Weintraub N, Rubenstein LZ (2006) Falls in the nursing home: are they preventable? J Am Med Dir Assoc 7:53–58. https://doi.org/10.1016/j.jamda.2005.12.016
Cioltan H, Alshehri S, Howe C et al (2017) Variation in use of antipsychotic medications in nursing homes in the United States: a systematic review. BMC Geriatr 17:32. https://doi.org/10.1186/s12877-017-0428-1
Fog AF, Mdala I, Engedal K, Straand J (2020) Variation between nursing homes in drug use and in drug-related problems. BMC Geriatr 20:336. https://doi.org/10.1186/s12877-020-01745-y
Malagaris I, Mehta HB, Li S, Goodwin JS (2020) Decrease of anticholinergic drug use in nursing home residents in the United States, 2009 to 2017. J Am Geriatr Soc 68:2797–2804. https://doi.org/10.1111/jgs.16776
Goodwin JS, Li S, Zhou J, Graham JE, Karmarkar A, Ottenbacher K (2017) Comparison of methods to identify long term care nursing home residence with administrative data. BMC Health Serv Res 17:1–8. https://doi.org/10.1186/s12913-017-2318-9
Downer B, Thomas KS, Mor V, Goodwin JS, Ottenbacher KJ (2017) Cognitive status of older adults on admission to a skilled nursing facility according to a hospital discharge diagnosis of dementia. J Am Med Dir Assoc 18:726–728. https://doi.org/10.1016/j.jamda.2017.04.021
Van Walraven C, Austin PC, Jennings A, Quan H, Forster AJ (2009) A modification of the Elixhauser comorbidity measures into a point system for hospital death using administrative data. Med Care 47:626–633. https://doi.org/10.1097/MLR.0b013e31819432e5
Samuel MJ (2015) American Geriatrics Society 2015 updated beers criteria for potentially inappropriate medication use in older adults. J Am Geriatr Soc 63:2227–2246. https://doi.org/10.1111/jgs.13702
Singh S, Lin Y-L, Kuo Y-F, Nattinger AB, Goodwin JS (2014) Variation in the risk of readmission among hospitals: the relative contribution of patient, hospital and inpatient provider characteristics. J Gen Intern Med 2:572–578. https://doi.org/10.1007/s11606-013-2723-7
Korda RJ, Du W, Day C, Page K, Macdonald PS, Banks E (2017) Variation in readmission and mortality following hospitalisation with a diagnosis of heart failure: prospective cohort study using linked data. BMC Health Serv Res 17:220. https://doi.org/10.1186/s12913-017-2152-0
Hekkert K, Kool RB, Rake E et al (2018) To what degree can variations in readmission rates be explained on the level of the hospital? A multilevel study using a large Dutch database. BMC Health Serv Res 18:999. https://doi.org/10.1186/s12913-018-3761-y
Mattos MK, Sereika SM, Naples JG, Albert SM (2016) Differences in benzodiazepine receptor agonist use in rural and urban older adults. Drugs Real World Outcomes 3(3):289–296. https://doi.org/10.1007/s40801-016-0080-7
Pottie K, Thompson W, Davies S, Grenier J, Sadowski CA, Welch V, Holbrook A, Boyd C, Swenson R, Ma A, Farrell B (2018) Deprescribing benzodiazepine receptor agonists: Evidence-based clinical practice guideline. Can Fam Physician. 64(5):339–351. PMID: 29760253; PMCID: PMC5951648
Funding
This study was funded by The National Institutes of Health (grants number R01 DA039192, 1 K01 AG070329-01, and P30 AG024832).
Author information
Authors and Affiliations
Contributions
Research design and manuscript first draft: all authors. Provision of study materials or patients: James S. Goodwin. Data analysis: Ioannis Malagaris. Final manuscript approval: all authors.
Corresponding author
Ethics declarations
Ethics approval
This research study was conducted retrospectively from de-identified data. The UTMB Institutional Review Board approved this study.
Consent to participate/for publication
N/A. The UTMB Institutional Review Board waived the requirement for consent to participate/consent to publish because the data was de-identified prior to use.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The correct given name of the 1st Author is modified in the original published proof.
Rights and permissions
About this article
Cite this article
Malagaris, I., Mehta, H.B. & Goodwin, J.S. Trends and variation in benzodiazepine use in nursing homes in the USA. Eur J Clin Pharmacol 78, 489–496 (2022). https://doi.org/10.1007/s00228-021-03244-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-021-03244-4